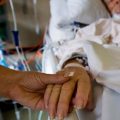
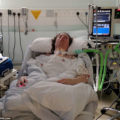
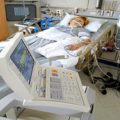
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Until When a Critically Ill Patient on a Ventilator Should Be Given Sedatives in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Richard, as part of my 1:1 consulting and advocacy service! Richard’s dad is with a breathing tube and on a ventilator in the ICU. Richard is asking why his dad is still on sedation and why are they not waking him up in the ICU.
Why Is My Dad Still on Sedation and Why Are They Not Waking Him Up in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Richard here.”
Eunice: All the questions that you’re asking are really good questions. I would write them down, so that way, when his primary doctor gets a hold of you, you get a hold of her, you ask her all these questions. I’m sure she’s going to go over this with you anyways, because she said she had a lot to talk to you about, regarding.
Richard: Yeah, because I definitely wanted to make sure that the ventilator was checked and then make sure that we need to do that or that the flow line and all those items, just in case, because I don’t want to be saying, ” Oh, this is your only last resort.” But we haven’t tried everything.
Eunice: Correct, and his primary doctor is also a pulmonologist and she stopped by and she saw your father, she agree with the ventilator settings are currently going on and she saw all the lines, so I’m sure she has her reasons why he is on those ventilator settings, but like I said, she’s going to discuss those reasons with you.
Richard: Okay.
Eunice: Go on those ventilator settings. I don’t have the answers to that and that’s for her to explain to you her reasoning, instead of me telling you something, then she’s going to tell you something else maybe. I’m the nurse and I’m sure that’s why she wants to get a hold of you.
Richard: Okay, and then the arterial blood gas results, do you have those?
Eunice: Yeah I’ve..
Patrik: Yes Richard, we’ve just gone through that.
RECOMMENDED:
Eunice: Oh, okay.
Patrik: We’ve just gone through that.
Eunice: Oh okay, right, that CO2 (carbon dioxide) and everything. Right.
Richard: So they were done at 6AM.
Eunice: Yeah 6AM.
Richard: Yeah, and then how many times a day do you check all those?
Eunice: The ABG (arterial blood gas)?
Richard: Right. All the labs, are they done twice a day or once a day?
Eunice: So, it’s only once a day. Correct. Arterial blood gas is usually not done daily, but from what I see, the trend here, they’re doing it daily on your father.
Richard: Okay.
Eunice: Yeah.
Richard: Okay. Okay Patrik.
Eunice: I can give you a phone number, you can leave her a message there and she will get back to you.
Richard: Yeah, and if you see her, let know to return my phone calls.
Eunice: She won’t be here. She unfortunately only comes once a day. She has other patients at other hospitals, so she comes in, do her rounds and then she leaves.
Richard: Right, but I’m saying if you see her again, whenever it is, just let her know to return my phone calls.
Eunice: If I see her, I will let her know.
Recommended:
Richard: And then my dad’s post is still full code?
Eunice: Yeah. He is still full code. Correct.
Richard: All right. Anything else? Patrik, anything you want to ask?
Patrik: Just one more question, you mentioned that urea and creatinine are fine and that Lasix was given yesterday, but the kidneys are working?
Eunice: They are, he’s..
Patrik: Just making urine.
Eunice: He’s outputting a lot of urine.
Patrik: Yeah.
Eunice: Yeah. He’s definitely making urine. Today he made 600 mls out and he’s still peeing, so he is making adequate urine.
Patrik: Right, and are you aiming for a negative fluid balance or what are you sort of managing overall?
Eunice: So right now, let me see what’s his intake and all that.
Patrik: Thank you.
Eunice: So his total intake has been 900 and his total output has been 600. He is swollen. He is definitely swollen. The doctor’s aware, but they have been diuresing him, like I said, they gave Lasix yesterday, but they haven’t given any today. They didn’t order any for today.
Patrik: Right, and does he have a lot of secretions on his chest? Do you suction him very often?
Eunice: We suction him every 4 hours. It’s not a lot, very small secretions, yellow thick.
Patrik: Okay, and he didn’t have a gag?
Richard: Did he cough when you suction him?
Eunice: He does have a gag. Yeah. When I suction him.
Patrik: Right, and they haven’t done, as part of the pneumonia, they haven’t done a bronchoscopy in the last few days. Have they?
Eunice: They did do a bronchoscopy a few days ago. Richard is aware of this. Richard, did they ever give you the results on that?
Richard: Yeah. It was just some yeast that they had no idea about, that they had to send out to another hospital or something.
Eunice: Oh, okay. Yeah, because they said they were going to call you to let you know the results, so I was just wondering if they did.
Recommended:
Richard: Yeah. It was kind of like there was no results, so it was just the yeast and so I requested them to get him on some type of yeast medication, and that’s when they added to fluconazole.
Eunice: Yeah.
Richard: 200 mg, I guess once a day, you said right?
Eunice: Yeah. Every 24 hours. Correct.
Richard: Okay.
Eunice: We started him on that yesterday, so today’s the second day.
Richard: Okay.
Patrik: And he is fed through a nasogastric tube and he’s absorbing feeds?
Eunice: Right now he does have a PEG (Percutaneous Endoscopic Gastrostomy) tube in place and he’s getting tube feeding through that PEG tube.
Patrik: Right, and he’s absorbing..
Richard: So the rate is still 45?
Eunice: No, the rate is 40. 40 mls an hour, continuous. With free water flushes, we’re giving him every 6 hours.
Patrik: Right, and he’s absorbing feeds? There’s no residual?
Eunice: No, there’s no residuals. Yeah. He’s tolerating well. No vomiting. Residuals been of 0, so he’s tolerating the tube feedings well.
Patrik: Yeah, and hemodynamically he is stable, he’s in a sinus rhythm. We talk to his doctor and he’s not on any pressors.
Eunice: His heart rate does go a little bit tachycardic, the highest has been 110, but other than that, it’s in the 90’s and it’s sinus rhythm.
Patrik: Sure. Okay. Wonderful.
Eunice: Yeah.
Patrik: I think Richard, I’ve got most information that I think is important for now.
Richard: Okay.
Suggested links:
Eunice: Definitely have… Who is this? A relative?
Richard: Yeah. Yeah.
Eunice: Definitely have this person also with his primary doctor, I think that will be good, because he is asking good questions and I just think overall it’ll be good info for you to know all that stuff from your dad.
Richard: Okay. Great. Anything else Patrik?
Patrik: No, no, I think that’s it. I think that is more than enough to have a chat to his doctor and go from there.
Richard: Okay. Eunice, can you send me a Face Time link?
Eunice: Yeah, let me look for an iPad, and as soon as I get an iPad, you should be getting that invitation. Okay?
Richard: Yeah. Okay. Maybe set it up for 6:30.
Eunice: 6:30, okay. Okay, I’m good.
Richard: All right. Thank you. Okay, bye bye.
Eunice: Bye.
Patrik: Thank you. Thank you. Bye bye.
Patrik: All right.
Richard: Hello?
Patrik: Yeah, I’m here. I didn’t want to push her too far, but there was certainly some things where she just reads out numbers and doesn’t question what she’s reading out. Does your dad have a history of COPD (Chronic Obstructive Pulmonary Disease) or asthma?
Richard: They had listed him before as COPD.
Patrik: They did?
Richard: But he doesn’t really take anything.
Patrik: So the biggest takeaway from this call for me is that his CO2 (carbon dioxide) is 74, and that’s why it’s sort of..
Richard: What is it supposed to be at?
Patrik: 35 to 45? That’s double. It’s almost double to what a physiological level is, and have they ever mentioned anything to you before about CO2?
Richard: No.
Patrik: Right, so then that comes back to the ventilator settings. You might have heard me ask when I said his breathing rate is 26 and he’s not breathing on top of that. A breathing rate of 26 is fairly high, which makes sense to have it high with a high CO2. A high breathing rate, generally speaking, should bring CO2 down, but again, that high CO2, the first question to me is, “Okay, does he have COPD? Does he have asthma? Is there something else going on?”
Patrik: And what I couldn’t work out from him either is let’s just say the CO2 was 74 at 6AM, did they change the breathing rate after that. Was the breathing rate set at 15, for example, before 6AM, then they did the gas, the arterial blood gas, CO2 comes back at 74 and then they increased the breathing rate. That’s the sort of thing she couldn’t answer, and then she was referring back to the respiratory therapist. Well, she needs to know that sort of thing. She needs to know the rationale behind why things are done. The doctors would explain to her the rationale behind why things are done. The respiratory therapist would explain to her why things are done the way they’re done. That’s sort of why I was questioning her. The other thing is, with the propofol and fentanyl still going, why is it still going? Why are they not waking him up?
Richard: I think when they keep trying to wake him up, he starts breathing really fast.
Patrik: Okay, and that’s where I think you had a very good point in your email where you said, should they be trying Dexmedetomidine? And I think they probably should. Is that something they mentioned to you?
Recommended:
Richard: No, I just researched. I do a lot of research over the years with my dad, I’ve done a lot of stuff and I found that, and when I asked Dr. Shu. She’s the one told me about ARDS (Acute Respiratory Distress Syndrome) and I showed her it’s normal and then the other one, she said, “He has fast heart rate.” But I was like, “Well, I’m thinking when you take him off the ventilator, it’s fast heart rate to me.” and then the Dexmedetomidine… I don’t know how you pronounce it, and she said that that wouldn’t work for him because it’s too late?
Patrik: No, I disagree with that. Whilst I said in my voicemail last night, or this morning for you, whilst I said Dexmedetomidine is not working for every patient. In the patient that it’s working, I think it’s working wonderfully. Just my experience is it doesn’t work in many patient, but if he’s sort of at the cusp now of having a tracheostomy or waking up and potentially getting off that ventilator, if it’s either, I think why would they not try?
Richard: Right. Just like with the forum and then that the other doctor said, “That doesn’t show good results. We don’t use it.” but why not try? Because if the last resort is the worst resort, why not try all these things prior to? And I’ve read and I’ve done my research and I found these medicines and that’s where I came up with these medicines, and I found one girl was on a ventilator for 120 days, and she came off of it, and they used the steroids and the Lasix and they use that Dexmedetomidine thing, and you can use that while you’re on the ventilator, so I just always try to look at options for my dad.
Patrik: Absolutely. That’s what it’s all about. So..
Suggested links:
Richard: What else did you get?
Patrik: What I didn’t hear from him, I tell you what I didn’t hear from him, so he was obviously talking about the infiltrates in the chest x-ray and the pneumonia. He wasn’t talking about him being diagnosed with ARDS. He didn’t say that. Not that I’ve asked for it specifically. Has anybody told you that he has been formally diagnosed with ARDS?
Richard: No, not until I was there last week and his doctor made that comment, before that, this whole time, I did not hear anything about that. It was just the pneumonia and sepsis.
Patrik: Right.
Richard: And the Vancomycin, and all the propofol, the fentanyl, take it off, propofol, put versed, take off versed, back to propofol and then pretty much that’s it. Try every day and try to take him off the ventilator. In the beginning when he was on Vancomycin, he was on the ventilator during the day, very low, 35%, 40%, 60%. They have a little chart. The moment they moved the Vancomycin, it went up, the x-ray was looking great, but then the moment they moved the Vancomycin, it went up, they were going to do the bronchoscopy, and then they decided not to, even though two doctors called me and they said not to, because the x-ray looked good, and then the next day all of a sudden they doing a bronchoscopy, so I just thought it’s kind of, I don’t know.
Suggested links:
Patrik: Right.
Richard: So, yeah. That’s just kind of where it’s been at.
Patrik: Right, but just, just by what you shared.
Richard: And now it’s a rare yeast.
Patrik: Yeah, yeah, sure, sure.
Richard: That’s when I was like, ” Well, can’t we just get a yeast medication to get him on.” We don’t know the last doctor, last night, we don’t know what she used to give. Okay, well can’t we just give him some used medication, so that’s why they added that, and I took Meropenem off.
Patrik: Yeah, sure, but I mean, if you’re talking about sepsis, earlier in the week, I would argue that even that he’s hemodynamically stable, that he’s not on any vasopressors. I would almost say he has fought that sepsis for now. Do you know what I mean? When I say..
Richard: What does that mean?
Patrik: Yeah, so when someone is in a septic shock.. Did you say he was in septic shock? Or did you say sepsis earlier? Which one did you say?
Richard: No just sepsis. I said pneumonia and sepsis. Yeah, that’s it with no septic shock.
Patrik: Right, okay, so if someone has sepsis, they often end up on vasopressors, which is considered life support, so what happens during sepsis, blood pressure often plummets to low levels, often incompatible with life, and then vasopressors are started. Vasopressors basically are intravenous medications that increase blood pressure. Again, that’s considered life support and that very often happens during the sepsis and given that he is stable on that level either… And that would also hone in with that they stopped vancomycin, that they stopped the Meropenem, because they must have worked to manage the sepsis. Now his white cell count is still 17.3, from what he said, that’s still a little bit on the high side, but I would argue that he’s past that acute septic phase, given with what the nurse shared. An acute septic phase looks different.
Richard: Yeah. His blood pressure has always been high. It’s never been low in this whole journey.
Patrik: Right. The other thing, it leads me back to the ARDS, so the high CO2 (carbon dioxide) might be a result of your dad having COPD (Chronic obstructive pulmonary disease) or it might be a result of your dad being in ARDS. That’s what I don’t understand at the moment, which one are we dealing with?
RECOMMENDED:
Richard: Well, they calculated my dad with COPD like 5 years ago when he was in ICU, but he hasn’t been taking any medicine. He’s had no medicine in the last four years. He’s had all vitamins through the PEG tube. The only medicine he took was ARVs (antiretroviral) because he ended up with some skin thing on his nose and he got off that, that’s when he had some back rash or something, so I don’t know if that’s what created the whole sepsis thing or not, but he doesn’t take any medication for COPD. When he got out of ICU, he had a little oxygen and he hasn’t been on it.
Patrik: Right.
Richard: Like I said, the only thing he has is a feeding tube for the last 4 years, and that’s it, so I’m not sure if he has it because of the scenario he was in, but he doesn’t take anything for it. He doesn’t have asthma. They don’t give him nothing. In the last 4 years, he’s been fine. He breathes on his own, no issue. He just had some skin issue and that’s it.
Patrik: That was the other thing. Why does he have a PEG tube?
Richard: Because the last time he went to the ICU, four years ago at a different location, he ended up getting sick and they had to intubate him. They restarted his heart and they pushed the PEG tube. I hate the PEG tube. I’ve kind of got accustomed to it, but they pushed the PEG tube, this doctor pushed it, to say, “Well, to feed him, that’s what we needed.” Because it was in his nose too long and for them to push the PEG tube, and that’s when the PEG tube showed up.
Patrik: Right, and he’s been having..
Richard: And he’s been doing the PEG tube at night and during the day he’ll eat.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!