Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
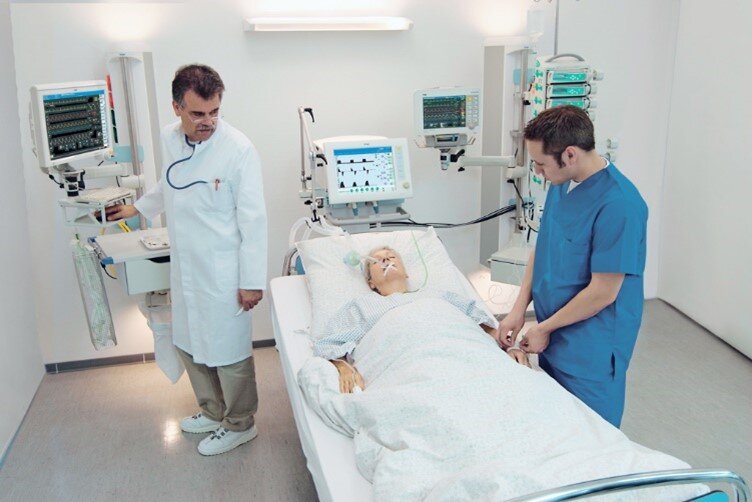
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Richard, as part of my 1:1 consulting and advocacy service! Richard’s dad is with a breathing tube and on a ventilator in the ICU. Richard is asking until when a critically ill patient on a ventilator should be given sedatives in ICU.
Until When a Critically Ill Patient on a Ventilator Should Be Given Sedatives in ICU?

Richard: Hi Patrik. This is Richard.
Patrik: Hi Richard.
Richard: Thank you for getting on to this call with me to talk to the doctors and nurses of my dad.
Richard: I haven’t talked to this doctor yet.
Patrik: Right.
Richard: Hi Nurse Leni, can I speak to the primary nurse for my dad?
Nurse Leni: Yeah, sure.
Richard: You know Patrik, I haven’t spoken to this doctor yet, she’s his primary at the facility. Just been done with the last doctor, actually, they added some fluconazole.
RECOMMENDED:
Patrik: Fluconazole.
Richard: Because they said about the yeast infection. They still need to wait for the results, and I said, “Well, can’t he add something for the yeast?” So they added that, 200 mg IV. They said the arterial blood gas (ABG) is improving, they’re still going to give him more steroids and Lasix. That was last night, and they’re stopping the Meropenem.
Patrik: They’re stopping the Meropenem.
Richard: That’s because he’s got for Fluconazole and Zyvox.
Patrik: Fluconazole and Zyvox.
Richard: Yeah, but I haven’t heard from his primary doctor yet. Last time I texted her I voiced my concern, but she hung up on me, which was very unprofessional.
Patrik: Oh my goodness. Why?
Richard: So now, we decided to call and so I’m assuming it’s to try to give me some type of update on…
Patrik: Yeah and when you spoke to the doctor a moment ago, did they put any pressure on you to make any decisions or?
Richard: No, no, no. That was last night. I haven’t spoke to the doctor, but I’m assuming that’s what his primary doctor is calling about because she never calls when we try to phone call, and so now she’s calling, so I’m kind of like, “Okay.” And yesterday was the end of 13th day, so yeah.
Suggested links:
Patrik: Yeah, she wants..
Richard: She said she left a message about update advice and next steps in treatment.
Patrik: So she wants something from you.
Richard: I think so.
Patrik: That’s what it sounds like to me. When did you last see your dad?
Richard: I’ve seen him on Tuesday.
Patrik: Tuesday. Right, and do you have any Face Time?
Richard: Yeah. I do Face Time every day. I talk and read to him and everything.
Patrik: Okay.
Recommended:
Eunice: This is Eunice. How may I help you?
Richard: Hi, Eunice. It’s Richard, the son of your patient in room 2A.
Eunice: Hi, yes.
Richard: I guess my dad’s primary doctor just called, but I missed her call. How’s my dad doing? How’s the FiO2 (fraction of inspired oxygen) and white cell counts for today and everything?
Eunice: FiO2 right now, it’s at 60%, so we’re trying to titrate him down from the oxygen, which we have, because it was at 75 this morning. You say you wanted to know his lab results?
Richard: Yeah, I apologize. Yes, the labs like his chest x-ray and then what is his latest white cell count result?
Eunice: 18.0
Richard: So it’s gone down, and they’re given him that new fungal Fluconazole, is that correct?
Eunice: Yes. Correct. Yes.
Richard: How much are they giving him on that?
Eunice: Hold on a second. It’s 200 mg bag.
Patrik: And..
Richard: It’s only once a day or twice a day?
Eunice: Every 24 hours.
Richard: Okay, and they’re still giving him the Zyvox, 600 mg twice a day?
Eunice: Yes. Correct. None of his medications have changed. They’re the same from yesterday.
Richard: So steroid and..
Eunice: Yeah.
Richard: What is his propofol and fentanyl at?
Suggested links:
Eunice: Propofol is at 25 mcg and fentanyl is at 70 mcg.
Patrik: Per hour. That’s per hour?
Eunice: Per hour? Yes. 70 mcg per hour.
Richard: That’s Patrik. She’s family, so… And then they’re giving him Lasix as well?
Eunice: Not today. They gave it yesterday.
Richard: Patrik, you were going to say something.
Patrik: And what..
Richard: Oh, they gave Lasix yesterday, not today?
Eunice: Oh, I’m sorry. I was talking to the family side is on the line too.
Richard: Oh, I’m sorry.
Eunice: Can I ask a question?
Patrik: Just a few more, and what ventilator settings is he on at the moment?
Eunice: Is his Zyvox? What was that?
Patrik: No. What ventilator settings is he on? How is he being ventilated at the moment?
Eunice: Oh, hold on second, I’ll get it ready.
Patrik: Thank you.
Eunice: So he’s on AC mode right now with tidal volume of 450, respiratory rate 26, PEEP of 14 and FiO2 of 60%.
Patrik: Right, and that respiratory rate, is he getting that from the ventilator or is he breathing on top of that? What is the set rate from the ventilator?
Eunice: He’s not.
Patrik: He’s not.
Eunice: The rate is 26 and he’s reading is 26.
Patrik: Right. I see, and with the propofol and the fentanyl, what’s his Glasgow coma scale, is he awake? Is he doing anything?
Eunice: Can get the Glasgow down here. It’s a 6.
Patrik: It’s a 6. Okay, and is there any plan to wake him up?
Recommended:
Eunice: Well, that’s what his primary doctor wanted to completely go into details with Richard.
Patrik: Yes.
Eunice: She’s going to discuss all of that with you. Ventilator settings, his status, what’s going to be the continuous care plan for him, all that, so that’s why she was calling you.
Patrik: Right, but what’s..
Patrik: Sure, but you as the bedside nurse, surely you would know why propofol or fentanyl is not being lowered?
Eunice: It is being lowered, but that was 100 and it’s now 70.
Patrik: Okay, and he’s not going above a 6 if you try to wake him up. If you talk to him, is he obeying commands? Is he doing anything if you stimulate him?
Eunice: He is currently being sedated, on purpose, because he’s on life support, so he’s not going to respond to me unless we take that out.
Patrik: Okay, but what stops you from lowering sedation even further? What’s the reason for that?
Eunice: That is something the doctor will discuss with Richard about.
Recommended:
Patrik: Right, so you as the bedside nurse, you’re just carrying out orders without asking, I mean it’s an answer you should have as the bedside nurse.
Eunice: Well, his primary doctor wants to discuss this with Richard, so I would rather her discuss this with him than him hear something from me. She’s the doctor, she’s the pulmonologist, so it’s better for her to answer this and give him these answers.
Patrik: With those ventilator settings, what are his arterial blood gases like? What’s the pH? What’s his CO2? What’s his PO2? What are they like with those ventilator settings?
Eunice: Hold on a second.
Patrik: Okay.
Eunice: I don’t think we do an arterial blood gas today.
Patrik: Right.
Eunice: Okay, so they did an arterial blood gas, but that was at 6 in the morning, this was before they did the ventilator adjustments. I have those results, do you want to know the 6 in the morning results?
Patrik: Yep.
Eunice: Cool, so the pH was 7.3, Bicarb is 40.6, CO2 is 74.8.
Patrik: CO2 is 74?
Eunice: Yes.
Patrik: pCO2 is 74?
Eunice: Yes.
Patrik: Right, and pO2?
Eunice: pO2 is 94.3.
Patrik: Okay. I mean CO2 is way out of range. Normal CO2 range.
Eunice: Correct.
Patrik: Is that why you’re ventilating him with a rate of 26?
Eunice: Well, I don’t give those orders.
Patrik: But you are an intensive care nurse, are you?
Eunice: I am, yes.
Patrik: Right, right, so you should know if CO2 is 74 that some ventilator settings need to be adjusted, so if CO2 is 74 and they’re bringing up.
Eunice: They’re carrying out those orders.
Patrik: Can I just finish? So if CO2 is 74 and the respiratory rate is 26, my question is, has the respiratory rate been changed after the CO2 was measured at 74?
Eunice: The only ventilator setting that we’ve been doing is titrating down the FiO2 (fraction of inspired oxygen), and that is the RT that does that.
Patrik: Yes so you’re just carrying out orders without really questioning what those orders are or…
Eunice: I don’t carry out the orders. That’s the RT that carries out the orders for the ventilator.
Patrik: How long have you worked in-
Patrik: How long have you worked in intensive care?
Eunice: What was that? 5 years.
Patrik: Okay. What are other blood results? Is his hemoglobin stable? Is he on any inotropes or vasopressors?
Eunice: No, he’s not on any vasopressors at all. His blood pressure is fine.
Patrik: Okay, and hemoglobin? Is hemoglobin stable?
Eunice: Hemoglobin is stable, but like I said, his primary doctor’s going to go over all this with Richard.
Richard: Okay. Well then we should schedule, because I like to have my family involved too, to schedule something with his primary doctor, like a direct time, if you can get with her and in the meantime, strep pneumonia test, has that came back?
Eunice: No, not yet.
Richard: Yes. I don’t know if his primary doctor left you a message with her phone number. Did she leave you a message with a callback number?
Eunice: Yeah, but I thought she might be there because the callback number is just to leave another message, so…
Richard: How were his x-rays today?
Suggested links:
Eunice: Let’s see his results for him. They just did a new x-ray a few hours ago, so it still hasn’t resolved yet. We don’t have to results yet, but they just did one, two hours ago.
Richard: So they didn’t do one early this morning, it was just two hours ago?
Eunice: Let me see. They did one at 5:30AM. You want to know that one? It still says that he has pneumonia. Bilateral infiltrate pneumonia.
Richard: Okay and then his creatinine is still okay?
Eunice: Yes it is. It’s perfectly normal. It’s 0.5. Yeah that’s it. Is there any other questions, I mean we need to really get with the doctor?
Patrik: Yeah, no, no. I don’t have any other questions at the moment. I guess let’s set up a call with his primary doctor and then we’ll go from there.
RECOMMENDED:
Eunice: All the questions that you’re asking are really good questions. I would write them down, so that way, when his primary doctor gets a hold of you, you get a hold of her, you ask her all these questions. I’m sure she’s going to go over this with you anyways, because she said she had a lot to talk to you about, regarding.
Richard: Yeah, because I definitely wanted to make sure that the ventilator was checked and then make sure that we need to do that or that the flow line and all those items, just in case, because I don’t want to be saying, ” Oh, this is your only last resort.” But we haven’t tried everything.
Eunice: Correct, and his primary doctor is also a pulmonologist and she stopped by and she saw your father, she agree with the ventilator settings are currently going on and she saw all the lines, so I’m sure she has her reasons why he is on those ventilator settings, but like I said, she’s going to discuss those reasons with you.
Richard: Okay.
Eunice: Go on those ventilator settings. I don’t have the answers to that and that’s for her to explain to you her reasoning, instead of me telling you something, then she’s going to tell you something else maybe. I’m the nurse and I’m sure that’s why she wants to get a hold of you.
Richard: Okay, and then the arterial blood gas results, do you have those?
Eunice: Yeah I’ve..
Patrik: Yes Richard, we’ve just gone through that.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!