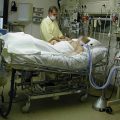
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another “PODCAST“ and in the last Podcast I interviewed Rachel who was able to have her Dad in ICU instead of LTAC and the last episode was
You can check out the last PODCAST by clicking on the link here.
In this week’s episode of “PODCAST“, I interviewed another one of my clients Adam whose father went on a cardiac arrest at home, rushed to the hospital, remained in coma, limited chances of survival as told immediately by the doctors but fought for his chance of living and eventually died in a natural way.
The Doctors asked us to stop treatment, but I gave my father in ICU a chance instead!
You can listen to the Podcast here or read the transcript below.
Patrik: Hello, and welcome to the intensivecarehotline.com podcast. Intensivecarehotline.com helps families of critically ill patients in intensive care to instantly improve their lives so that they can make informed decisions, have more control, more power, and more influence. I’m your host, Patrik Hutzel, founder and editor of intensivecarehotline.com, and as part of our podcast and interview series, today I’ve got a very special guest. I’ve got Adam with me. Hi, Adam. How are you?
Adam: Hi, Patrik. I’m well, thank you. How are you?
Patrik: Very good, thank you. Adam, it’s really great to have you on our podcast. Adam, I know you and your family, you’ve been through a very difficult time in the last few weeks, or even last couple of months. And I really appreciate you taking time out of our day and come on to this interview. Adam, your dad passed away a few weeks back, and I want to pass over to you and let you share your story, but your dad started off in intensive care, very ill, and he’s been through a long journey before he actually passed away. Do you want to share more with our listeners what you and your family have been through?
Adam: Sure. Absolutely, Patrik. My father passed away a few weeks ago. It all started when he had a cardiac arrest at home. He collapsed, and his heart stopped beating completely. I wasn’t there at the time, but it was my wife who found him, and she started to resuscitate him straight away, she called the ambulance and they were on their way. The ambulance had arrived, and they needed defibrillator to regain my dad’s heart, but the downtime, the time he was left without a heartbeat, was 30 minutes.
Patrik: Right.
Adam: He was rushed to the hospital to the Intensive Care Department. My father had remained in a coma after that. His eyes were closed. He wasn’t waking up, but his heart was back to normal again. I arrived straight away, and it was devastating for us. I wasn’t sure what had happened. I wasn’t completely aware of what a cardiac arrest was I’d heard of it and all that and had known that it was like a heart attack. Our whole family was quite devastated. My dad’s just laying there in Intensive Care. The doctors had sedated him, so they should keep him asleep, and straightaway, we were told that, “Your dad’s chances of survival are very slim.”
RECOMMENDED ARTICLES:
It was a hard moment to accept that, and we didn’t quite accept that because I didn’t quite, didn’t want to believe, I believe what was being said, it was only a matter of a few hours, and I’d been told that dad’s chances of survival are very slim. That’s when I got to doing my own research. I think between a lot of friends and family would do that for their loved ones because you, yourself, want to know what’s going on. The doctors can’t give you exactly or give you the exact information from what’s going on because I think they’re quite reserved with what they can say and the time to say it as well. It was a brief two minutes to say that Dad had suffered a cardiac arrest and that his chances of survival were very slim.
I started doing my own research and I could go on the internet, the various search engine just to find out what exactly the cardiac arrest was. What I’d learned from that is that the time that my father had not had his heart beating, there was a very high chance that the oxygen was deprived to his brain, and that, in result, would have caused irreversible brain damage. We went on to, then, wait a few days because we were constantly by his side, and also we were doing our research as much as we could to find out if there had been cases of people that could recover from this sort of injury, because we didn’t want to accept what the commission and the hospitals told us.
RELATED ARTICLES:
What I grew to learn at the time, being in Intensive Care, my father in it, it’s almost based on a really high likeliness of something happening as far as my father was concerned we wanted absolute certainty that this would be the case, before we would accept that my father would not survive at all. And while I was doing my research I was finding cases of people that had had experiences very similar to my father and then went on to survive, come out of it kind of, woken up.
And then my father’s still not woken up, suffering seizure type activity whenever they lowered the sedation something quite typical of what they do in intensive care unit is to once or twice a day do a sedation drop just to see if that person wakes up, and when they’d done that to my father he’d start suffering seizures. And those seizures from my understanding were myoclonic seizures which are quite typical with someone that’s had a cardiac arrest. So they put the sedation back in because they were quite aggressive seizures and they hadn’t found the right medication to control those seizures yet. Sometimes there are medications that can control those types of seizures but they upped the sedation. So my father was left in almost a coma for two weeks and then after that once the neurologist had come and assessed my dad eventually he’d recommended an anti convulsant drug that would really help my father control his seizures.
RELATED INFORMATION:
During all this time he had not been awake at all, he had been fully sedated. It was only in the second week of him being there once they’d dropped the sedation and the seizures had calmed down a little bit, during this time they dropped the sedation to halfway and then they dropped it fully. For a few days after that, after the sedation was completely off we started to see signs of his eyes opening, and it was at this point that we thought as a family we were making progress, and maybe my father waking up.
At that point the research continued and continued and that’s when we were having several meetings with the clinicians there who would meet us maybe once a week just to update on what’s going on, and in each and every one of those meetings the clinicians would say that, “Your dad’s chances of survival are very very slim, and if he does survive he will be in this state for the rest of his life.”
RELATED ARTICLES:
Patrik: Did they have a name for that state? Did they say that it would be a vegetative state? Did they give that a label?
Adam: They didn’t say a vegetative state. They didn’t classify it just then, but they used the words quality of life a lot that he was gonna have very very poor quality of life. And how do you define quality of life in my opinion might be different to their opinion of quality of life.
Patrik: Absolutely.
Adam: They’d be quite reserved in the type of terminology they used if they couldn’t classify someone as that. So it left us quite confused as well because we’d heard of different cases where people had potentially woken up and it was just time that was needed. For such a devastating event as had occurred to my father, you know, thirty minutes left without oxygen but there were cases of people where people just need that time to recover for their brain to heal. But it just felt like they weren’t giving us the time at all, they were quite pushy they wanted us to make a decision for my father’s life, you know, turning off the machine, and it certainly felt like it was a number thing for them. You know, this person has a low chance of surviving, give our opinion and let the family know what the likelihood is, but for us you know, not being a hundred percent sure which you know clinicians couldn’t, for us that’s not enough. And at that particular time that was certainly not enough.
So they pushed and they pushed and we said, “Look we need time.” But as that time went on the meetings got quite difficult, the clinicians were inviting experts in the field and people who had been doing this for years and years and years and during all this time I felt that I was getting yes an expert opinion but no one could give me 100 percent surety that my father was going to remain like this. We’d certainly read that if someone was in this particular state all of the signs that my father was showing, pointed towards him from my reading his being in a vegetative state. Or he was in a vegetative state, but I think they reserved saying that because if someone is in a vegetative state especially in the UK and they’re there for six months like that, then at that point you classify someone as being permanent.
So I think that, in a way they held back from saying vegetative state because then I could turn around and say, “Well this is not permanent.” Because if it’s going to be permanent one has to be like for six months, so I feel that that’s why they didn’t classify him and they didn’t use that term.
RELATED INFORMATION:
Patrik: Can I just sort of, summarize what’s happened to this point for our listeners, probably just putting a little more terminology around it? So our listeners have sort of a little more clinical insight of what’s happened.
So your dad had a cardiac arrest, he probably had what’s called a quote unquote down time for thirty minutes. Now for our listeners what’s important to understand is that if the brain potentially is without oxygen for more than three minutes, there is often irreversible brain damage and that obviously was a concern in your dads situation. Now, it sounds to me like you’ve experienced a lot of negativity from day one, a strong push towards withdrawing treatment. The term quality of life has been mentioned a number of times and I think it’s really important to understand that, again like you’ve already said Adam, quality of life is a very subjective measure and not up to and outside that to determine what’s acceptable for quality of life for your dad, or for your family member or for yourself.
The other question that I think is quite important in this, and though we’ve spoken a number of times Adam, I wasn’t quite aware that your dad was in an induced coma for almost two weeks and every time they woke him up he had seizures. It sounds to me like it took a while to get a neurologist involved is that correct, and if that’s correct do you know why it took so long?
RELATED ARTICLES:
Adam: No, you’re absolutely right. A neurologist was involved quite later on down the line, and it was to start with just over the phone. It was the clinicians in intensive care that had spoken to a neurologist over the phone and described what had gone on, and the neurologist had advised on certain anti-epileptic medication to help control those, and only on the point where the epileptic drugs weren’t working. That a neurologist came to see my father for probably less than a few minutes.
At that point I’d requested that I was there during that time to sit down with the neurologist and ask him questions, and ask him what his view was. So you’re right in saying that a neurologist was only later on involved, for me at the time this was all new to me so I didn’t whether this was actual procedure, but I feel that a neurologist maybe should have got involved at an earlier stage because this was certainly from what I read and what I’ve been told this was a match for brain damage and it was the type of brain damage, it was hypoxic brain damage and my father should have been maybe assessed more regularly by a neurologist just to check the progression. So they were really relying on what the clinicians and the intensive nurses had seen. The reality is a lot of times the intensive care nurses are not focused on one patient, or that they may not see small changes a lot of the time it was us giving them feedback on what we had observed and these were the changes we had seen in my father.
RELATED POINTS:
That all happened after he started waking up, what I mean by waking up is his eyes open, it wasn’t consciousness, eyes opening and some signs of movement. But yeah, the neurologist wasn’t there as often as I think it really should have been.
Patrik: Right and did you have to push for a neurologist? Or is that something you asked for? Why do you think a neurologist wasn’t involved earlier? Just from my professional experience whenever there is brain damage or query brain damage a neurologist needs to be involved from the start to assess CT scans, cat scans, EEG’s, potentially MRI’s. Do you know why that didn’t happen from day 1?
Adam: I really don’t know. I mean, I know that particular hospital where my father was there wasn’t a neurologist on site. It was part of a trust and there were three or four other hospitals and a neurologist from in that trust from another hospital had to come see my father, so that may have been one of the reasons why. Or it may have been the case that clinicians don’t think that the ICU clinicians see day in day out and maybe there was no need for one but I certainly felt that there was a need for one. Because it was a matter of brain damage and a matter of the brain and the seizure activity that had been appearing, the myoclonic, that that should have been looked at by someone that’s mixed up into the brain.
RELATED INFORMATION:
Patrik: Yup.
Patrik: Hi, Adam. We got disconnected. That’s okay. We’re back on track.
Adam: Okay.
Patrik: You can just continue. We were talking about the neurologist and their level of involvement. We were also, I do remember when you first contacted me, I was also surprised at that stage, your dad might have been in ICU for about four weeks I believe when you first contacted me. One of the first questions that I had for you was why does he not have a tracheostomy or a trache. Can you say more about what was discussed then with the ICU team in terms of tracheostomy. What I would also like to share with our listeners really is … best practice normally for tracheostomies after about 10 days to 14 days of ventilation with a breathing tube if somebody can’t come off the ventilator, then a tracheostomy should be performed to ease the burden of ventilation.
As I said, I do believe when you first contacted me, your dad had already been in ICU for about three or four week. Can you share more about what discussions you’ve had with the ICU about tracheostomy and what your point of view was at the time?
RELATED POINTS:
Adam: Sure. From what I read in my own research, a tracheostomy is a more comfortable breathing tube and it’s something that should have been done quite straight away. There was a reason that they couldn’t do one for my father is because they said he had a short neck. My father’s anatomy is maybe you could say slightly higher or bigger than the average person. In doing so, this may have been a complicated procedure. From my understanding, this was not done because it was something that just couldn’t be done in the ICU ward. It would have been done under surgery.
Now, why they couldn’t do it under surgery at the time, I don’t know, but what I was told they didn’t see the point in doing so at the time because they didn’t feel as though my father was going to make a recovery. The UK clinicians, doctors, surgeons cannot carry out anything or treat the patient with anything where they feel as if there’s not going to be a benefit to the situation.
Patrik: Yeah.
Adam: And in this case, in doing so for my father, it could have been no benefit in him having a tracheostomy because as far as they were concerned, my father wasn’t going to recover anymore.
Patrik: Right. How did you feel about that at the time? Was that something you and your family could accept easily? How were you dealing with that level of frustration at the time?
Adam: I was quite disappointed. Not quite, I was very disappointed because as time went on, my research and I had been reading into this quite a bit and I was very disappointed because a tracheostomy would have allowed my father to be moved to a ward where they could have given him the chance the recover. Where they could have potentially set him up to stimulate him a bit more. Under the breathing tube that he came in and they put in which goes down from him mouth into his throat, that doesn’t allow him to do anything.
RECOMMENDED ARTICLES:
That just keeps him in intensive care. So for me, it was very frustrating because they couldn’t do this procedure because their guidelines don’t allow them to carry out a procedure on someone they don’t see the benefits. But as far as I was concerned, it was too soon to say whether he was going to be like this permanently. So I did see the point in doing so. That’s why the battles that we had with them. This is one of the thing that you helped with in terms of the preparation for the meetings.
I done a bit of research myself and from speaking to yourself, it gave me more of a clear understanding on the reasons why a tracheostomy would be beneficial for my father and this really helped me when I went into the meeting with them to discuss this because the doctors, the clinicians, won’t lie, but as much as they would like, they won’t give you scenarios of where someone may have had something like this done and went on to survive. At that point, that’s when talking with yourself, Patrik, really helped me really ask them the right questions (7 days unlimited US 1:1 phone counselling) and having asked those questions, I do believe that the 100 days that my father was in ICU really allowed me and my family some closure and a point of acceptance because in the end, my father remained in a vegetative state. However, it gave us time to accept that this is now … and yeah, there’s not 100% certainty, but this is now as good as it may well get.
In that time, he was seen by various experts that we had requested. That helped us as well. That helped us with giving us closure. Within two weeks, we didn’t accept that my father had his brain damage like this permanently. The brain is such a thing that there is no 100% certainty and there’s cases of people where people have had a cardiac arrest and died straight away. But in my father’s case, we were seeing small signs of changes. Plus, this was heading in the right direction. But eventually it got to a point where we didn’t see any more progress and we’d been there for over three months to give us some closure and give us some more certainty as to what his quality of life would have been in the future. But had it not been for us challenging the intensive care doctors and asking for that extra time, I really feel as if we would have maybe fallen to the pressure of switching the machine off very far too soon, then having to live for the rest of our lives thinking to ourselves, “What if I had done this? Or what if we had said no.”
So this is something that I certainly don’t regret doing. With your help, Patrik, and you really helped us prepare for these meetings and gave us your experience in being in intensive care for many years on what is acceptable and what they can potentially do that they may not have been doing, and that really helped because I really believe that helped us buy time with my father intensive care.
RECOMMENDED:
Patrik: And that was time you and your family really needed as you ended towards, to come to terms with things. I really believe you left no stone unturned. In the end, no matter how hard it is, but in the end I believe you and your family were able to accept that’s the way, and you could accept that your father eventually passed away. Let me ask you a question. Many listeners might ask, or you’ve gone through 100 days in intensive care until your father passed away. And many listeners might think was there a lot of suffering? Would it have been better for your dad to potentially die earlier and limit the suffering? Can you comment on that? Do you think your dad was suffering?
Adam: At the start I didn’t really know. But as time went on and speaking to the doctors, doing my own research, speaking to yourself, I was under the understanding that my father was not aware of himself or his surroundings. If there was suffering, I do believe that he was suffering for the right to live.
Patrik: Yeah.
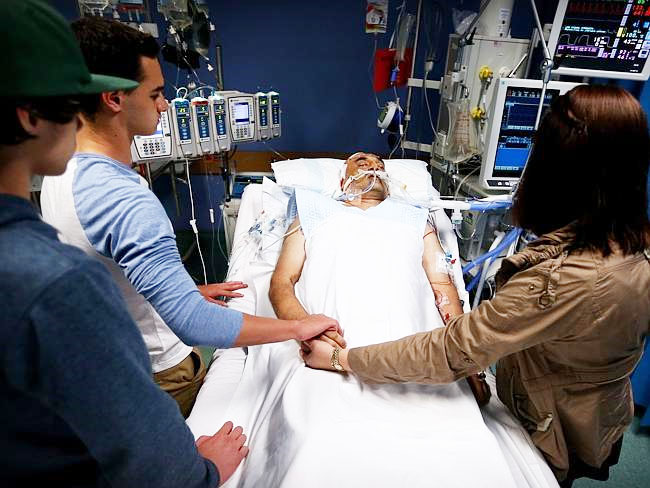
Adam: Because potentially, it was far too soon to say, “Oh my father’s suffering. Let’s switch off the life support.” For me and most certainly in my father’s point of view, that would not have been acceptable.
Patrik: Yeah.
Adam: So it did go through my head that maybe my father is suffering. But in the end, I believed that he may have a chance to live.
Patrik: Absolutely.
Adam: With a little bit of suffering. But when we got to the end, it was my understanding and my belief that he didn’t actually feel anything. He wasn’t suffering. So that almost in a way helped us as well with regards to feeling less regret because this was a very tough decision to make.
Patrik: Absolutely.
Adam: My father, at the end of the 104 days, at the end of that, his eyes were wide open and his eyes were fixed into no particular direction, but he wasn’t aware of what was going on. And that made it harder in a sense to make that decision, but it gave me and my family, it gave us closure and I feel as if we were almost as close to certain as we could be that this is now permanent.
Patrik: Yeah.
Adam: On many occasions, the doctors had said that my father wouldn’t even get to this stage, so as time went on, I was doubting them even more because at one point, the doctor said your father won’t open his eyes. A few weeks later, he opened his eye. So when I saw this progress in my dad and what the doctor said, it made me raise more questions.
Patrik: Yeah.
Adam: Maybe more questions about every single point. And that was every single point in that. We made sure that was looked at and we had various conversations with yourself, Patrik. You helped us in different parts of my dad’s progress. Each time we had that meeting, we could go in there having knowledge and that was probably the best thing because then the doctors had known we had done our research and they knew as well that they could only base it on their experience and say, “Well, we think this and people don’t have a quality of life.” But then, those people that did recover, or were moved on in the state, made me question how many of these intensive care specialists do go on to see that person has lived on and recovered. I’m not sure, so.
RELATED ARTICLES:
Patrik: Yeah. And I’m pretty sure I mentioned that in our conversations that most intensive care doctors and nurses, they know everything about intensive care, but very rarely do they follow up with patients out of intensive care once they leave intensive care alive. They have no idea what the patient’s life looks like six weeks, six months, even six years down the line. There’s very little research there.
There was a final thought that I had and there was a final issue that we spoke about really in the last few days of your dad’s life, and I remember that quite clearly. One of your concerns at the time was the way your dad was approaching his end of life and we discussed the issue of euthanasia therapy because that was very important for you that your dad would die a natural death, which he died a natural death in the end from what I understand. Why was that so important to you? Where I’m going with this is, really a lot of families in intensive care, when it comes to end of life, they actually don’t know that sometimes death is hastened when life support is withdrawn and then medications like morphine or midazolam are given and slow down breathing. And then patients often pass away because they have sedatives on board and they basically stop breathing.
Now that was a really important point at the time for you and your family to have nature take it’s course. Can you elaborate on why that was so important for you?
Adam: Yeah, sure. Just before the removal of the breathing tube for my father, me and my family sat down with the intensive care doctors and discussed at what point they would remove the breathing tube and what’s likely to occur after they remove the breathing tube. We also discussed that if my father was to live on, because he was only, the breathing tube was assisting him in a small way. I can’t remember the technical term, but it was a small percentage. Most of the breathing was done by himself.
Patrik: Right.
Adam: So the doctors in mixed views. Some said that he would die. Some had said that he would live on for perhaps days, weeks, months even. But it was important that if my father did live on, what sort of care would my father be given and what would happen in the case of he had started to show a sign of recovery and wakefulness or consciousness. So all of these things were discussed. After my father’s breathing tube was removed, he continued breathing by himself. Which he then at that point, a couple of days after, he was moved on to a general ward. In that general ward, he was seen by a different team completely.
It was a different care team and there was end of life.
RELATED INFORMATION:
Patrik: Yeah.
Adam: I had a couple of meetings with them as well about what level of care to provide to my father now because it was accepted by all of that, this is my dad’s end of life now. And a few days after removing the tube, his breathing had been quite difficult for him. You could almost hear it.
Patrik: Yeah.
Adam: It was very important to me and my family that if my father was going to pass away, it would be very natural. He would just naturally pass away. So, it was important for us that he was being kept hydrated and he was being kept fed through a feeding tube. For me, that’s not really, in my opinion, certainly it would have been particularly of our family values and certainly my father’s that these are your basic necessities, food and water to be continued up until the end of life.
And we’d all agreed that any other interventions wouldn’t be made. If there were any failure to any particular organ, then that would not be treated, but the withdrawal of food or hydration, that was important that that was not removed and my dad would eventually pass away slowly but in a dignified way as well.
Patrik: Yeah.
Adam: That’s exactly what occurred. But it got to a point where, my father lived on a further week after removal of the tube. It got to a point where, within four days, the doctors wanted to introduce a sedative again because they thought it would make my father more comfortable. In our opinion, I think I only wanted him to be sedated or wanted to … from what I understood from when I read that potentially that would slow his organs down. And for me, that was being very natural. I wanted him to pass away naturally and peacefully.
RELATED INFO:
Patrik: Yeah, yeah.
Adam: On one hand, if he wasn’t aware of himself or his surroundings and on the other hand, they want to make him feel comfortable, so I didn’t quite understand their thought process behind that.
Patrik: Right. You mean one might argue and it’s certainly my experience, you felt under pressure from the start to withdraw treatment. Even in the end then, you felt under pressure they wanted to introduce a sedative. One thing that I always argue is they want to limit the resources. They want to free up their beds. It’s very sad, but I’m really pleased knowing your story that you stood your ground to the end and you basically had as much of an end of life situation on your terms as possible, as much as the situation allowed. Can I just ask, it’s always hard to … I don’t even want to use the word success. It’s not a term that fits the situation. I can’t come up with a better term at the moment, but it has been very important for you and your family to leave no stone unturned and give your dad the best chance of survival.
And you’ve done all of that and I would assume it has given you and your family some peace of mind to know that you’ve done everything within your power to give him the best chance. Can you look back at least and can you say we’ve got some peace of mind around this situation?
RELATED ARTICLE:
Adam: Yeah, I’d say, Patrik, I can because me and my family, when we sat down and talked about this on a daily basis, we wanted to make sure that the decision regarding the end of my father’s life is made by what my father would have wanted and we were representing my father’s wishes. It wasn’t made, or it wasn’t pressured by anyone else, the doctors. And that, as you said, that gave me a little bit, quite a little bit peace of mind me and my family knowing that we had not left any stone unturned.
And we had explored every single avenue up to the point where the experts’ opinion that eventually come in was someone that is of the highest degree of that particular field. The expert in that field or the other disorder of the consciousness. That gave us peace knowing that we had explored everything. We’d done it on our terms. And we gave my father the fighting chance because right now, it’s devastating what’s happened. In the end, my family we take a little confident in knowing that it wasn’t, the fact that it happened obviously is out of our hands. But, the whole process throughout, we were very, very involved with every single decision. It gave us a bit of comfort knowing that we’d made those decisions and that was the best and only, the best decision for my father. No other agenda. And like you said, it wasn’t about bed space for us. It wasn’t about probability of survival for us. It was pure, this is what’s best for my father. This is what we think is the best for him in terms of giving him a chance and that’s what we wanted.
We wanted time. We wanted to give him the chance because we’d heard stories about people surviving. We’d read, and they were quite small, but we got to the point where we were absolutely of certainty in our hearts that now … and it gives us a bit of comfort knowing that. And it gave us closure as well knowing that we didn’t leave any stone unturned.
Patrik: Yeah, yeah. What would you recommend … we have so many families coming to us at intensivecarehotline.com who are in a similar situation. They feel under pressure. The feel like, the doctors have asked us to agree to stop treatment. What would your advice be to families, to other families, who are in a similar situation?
Adam: My advice would be not to just be pressured by the doctors or treating team. Not to say that their word is the final word. If it’s a matter of opinion, then an opinion is called an opinion for a reason. Go and look for another opinion. Go and do your own research. Go and question the doctors. It’s quite daunting to go into a meeting room with people that are completely qualified and have done this for many years and when this is something very new to you because you almost feel scared to ask them questions back.
RECOMMENDED ARTICLES:
Where you almost feel, get the impression that their opinion is the final opinion. And trust me, it’s certainly not. There have been doctors in the past that have been, in my reading, not knowing them, but from what I’ve researched, there have been doctors that have been proven wrong and they’ve got it wrong and I just wanted to make sure that my father’s case, he wasn’t one of those cases where the doctors got it wrong. So, don’t feel pressured. Prepare before you go into those meetings. And go fully armed with all the knowledge so that you can’t be intimidated in a way where you’re pressured to make decisions that you may well regret in the future. And that was very important to me.
Patrik: Yeah. It is important because at the end of the day, they are life or death decisions and you can’t afford to get those decisions wrong. They are once in a lifetime situations, once in a lifetime decisions you have to make. And we certainly see it all the time. The minute you start educating yourself, the minute we educate clients about their rights as well, which is very important. You’ve got to be aware of your rights in situations like that. And you’ve certainly exercised all your rights in terms of giving your father the best chance of life.
Patrik: Adam, I’m conscious of your time, obviously and I’m conscious of our listener’s time. Was there anything else you would like to add to the whole situation before we close off this interview?
Adam: No, not really. I think we’ve covered most things. Again, I just want to … I haven’t thanked you enough, Patrik. I’d just like to say thank you as a person that has really helped me and my family. One of the reasons I agreed to go on and help you with this podcast is because I do feel as if you do add true value into something that was very, very, very important to me and my family. And as you said, it’s a matter of life and death. Any decision like this shouldn’t be taken lightly. So I just want to say thank you. I think it’s fantastic what you’re doing in helping people make these decisions. What you can help them do is but just educating them a bit from your experience. But you don’t have any agenda but what’s your experience in an ICU environment for many years.
So you’ve absolutely helped me and my family with closure. So I just want to say, again, thank you very much Patrik.
Patrik: You’re very welcome and I really appreciate you taking time out of your day to come onto our podcast and share your story with our listeners. I can’t thank you enough for that because it has been a very difficult time for you in the last few months. And I really appreciate you taking the time out of your day while you’re probably still going through the grief process. Because we’re really recording this interview just a few weeks after your father passed away. So I do really appreciate you taking time out of your day and then coming onto the podcast. So thank you Adam.
For our listeners, check out our Your Questions Answered Section as well. We also just opened a membership for families in intensive care, intensivecaresupport.org. You can check that out on our website. If you want to get one on one consulting and advocacy, check out the options on our website. Again, thank you Adam for coming onto this podcast. Have a good rest of the day.
RECOMMENDED:
Adam: Okay. Thank you Patrik.
Patrik: Thank you so much. Bye bye. Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s PODCAST and I’ll see you again in another update next week!
Make sure you also check out our “YOUR QUESTIONS ANSWERED” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!