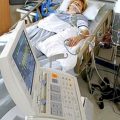
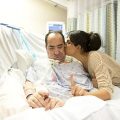
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Megan, as part of my 1:1 consulting and advocacy service! Megan’s brother is critically ill in ICU and Megan is asking if it is true that ICU nurses should act as advocates for her brother.
My Brother is Critically Ill in ICU. Is it True that ICU Nurses Should Act as Advocates for My Brother?
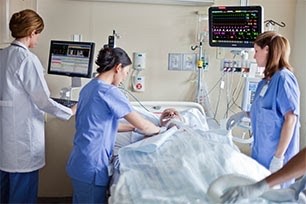
“You can also check out previous 1:1 consulting and advocacy sessions with me and Megan here.”
Megan: Yes. I’m going in the complete opposite direction to them. But in defense of the nurses, I would say that they do … obviously, they have to be very diplomatic. But they do appear to be very, very genuinely very pleased when he does well. They really do seem-
Patrik: Yeah. Because they are there. The doctors just drop in for a few minutes, they look at a piece of paper while the nurses are the ones who know Ryan by now. I would hope.
Megan: They do. Indeed.
Patrik: They hopefully have a bond with him as well.
Megan: I think so.
RECOMMENDED:
Patrik: Right. And they are the real advocates, I believe. And that’s probably another thing if you feel like there are some of the nurses who are a bit more experienced who could take part in your advocacy, that could help too.
Megan: Yes. I mean, I really do think, they ask, the nurses, they ask and the same one, I see them when they’re coming in and they look at me and they say, “I’m hoping I’m going to be looking after Ryan.”
Patrik: Right. That’s good. No, that’s good. I like it.
Megan: Yes. And then the other day there was Analie as well and I said, “You’re looking after Ryan?” She said, “No, but I take a look at him every now and then.” She said.
Patrik: Right.
Megan: That was good. They were almost, both wanting to. And then they said, “Oh, Ryan, he’s got such beautiful eyes. He’s the loveliest man in the ICU.” That’s what they say.
Patrik: Wonderful.
Megan: There is good.
Patrik: Good.
Megan: He is popular with them.
Patrik: Yes. No, that is good. It also would be a shock for them too, if something was to happen.
Megan: Yes. I believe so. Because they genuinely, genuinely seem to want to take care of him and he has the same nurses over and over and over. And they say, “I’m looking after him.” They go like that to me. And I’m sure they don’t make that up.
Patrik: No. No. They don’t make that up.
Megan: No, they don’t. So that is another plus for Ryan, I think. And also if they were doing evil things, the nurses obviously have to do the evil deeds.
RECOMMENDED:
Patrik: Well, this is how I ended up doing what I’m doing. You know? I wasn’t participating in any of those evil things.
Megan: You didn’t want to take part.
Patrik: No. And I told them in no uncertain terms.
Megan: This is how-
Patrik: This is how I ended up doing this and I’m still working, I’m doing two shifts a month and I’m busy with my in-home care nursing but I’m still working in that same ICU, you know? I didn’t burn bridges but I made very clear that if they wanted me to participate in anything that I don’t do, that they can sack me and that I’m happy to leave.
Megan: And that you’re happy to go. Because it’s all very well with the doctors to say, “Oh well we’ll do this and we’ll do that,” but it’s the nurses that have to do it.
Patrik: Well, I asked in some situations. I said, look, you’re asking me to do this, I’m not doing it. If you want to do it, do it yourself.
Megan: Do it yourself. You go and take the vile of things. You go and mix it up and put it in this person’s vein.
Patrik: That’s exactly right.
Megan: When this person can breathe on his own for eight hours. It’s a big ask, isn’t it?
Patrik: It’s a very big ask.
Megan: And it’s very, when you do nursing to help patients, it must be tough. Well, impossible.
Patrik: Well, it’s not only that, it’s overtime you understand the whole politics about beds and money and you don’t understand that from the start of course but with time, after nearly 20 years I just said, oh, hang on a sec. This is all getting … I know way too much.
RECOMMENDED:
Megan: Yes. I know too much.
Patrik: Right.
Megan: I know too much and I don’t like it.
Patrik: That’s right.
Megan: And I don’t like it. It’s against what I started to do this for.
Patrik: Correct.
Megan: Yeah. So in this what you’re doing, with the other things you do plus with this, you’re able to help people.
Patrik: Yes.
Megan: To prevent the evil doers.
Patrik: Yeah. And to navigate the territory. Yeah.
Megan: The territory is very, very rocky. There’s bogs and pitfalls and mountains everywhere.
Patrik: Yeah.
Megan: And wild animals.
Patrik: Yes. Dangerous.
Megan: Very, very, very difficult place to navigate. Patrik, thank you so much. So, I’ll do that email for you now with a little bit of the family thing just so you’ve got it in front of you. And also I will give you the number and everything and the name of the nurse and do you want me … I won’t say anything, I think you just ring.
Patrik: Yes. I will just ring and I will … We’ve got to work it out. Do you have other people ringing?
Megan: Yes. But they always push them back to me.
RECOMMENDED:
Patrik: Ah. So you don’t-
Megan: If I’m there, they’ll say, can I give your aunt that? Can I give Auntie Luz, can I give her an update? And I’ll say yes. So they’ll give her an update. But other people that ring are always referred back to me.
Patrik: Okay. So, sorry, I don’t quite … you have people ringing?
Megan: Yes. But they don’t ring so much anymore because they wouldn’t tell them anything. They’ve rather given up.
Patrik: So, would they not tell them anything because … You would have authorized the nurses to tell them things, wouldn’t you?
Megan: I think I should do that with my aunt, yes. Everything was such a rush at the beginning and people were calling and they were just referring them all back to me. But I should give a list, shouldn’t I?
Patrik: You should.
Megan: You can speak to these people.
Patrik: You should. You definitely should. That’s almost removing any ambiguity.
Megan: And it’s removing the barriers.
Patrik: It’s removing ambiguity, it’s removing the barriers, you could go as far as having a code.
Megan: Right.
Patrik: Right. So, for example, you could say we’re using this code, could be a birthday or it could be, I don’t know, anything.
Megan: Whatever.
Patrik: Whatever.
Megan: Yeah.
Patrik: Remove ambiguity if you can.
RECOMMENDED:
Megan: Good idea. So do you think Patrik then it’s better that you don’t phone until I’ve gone in?
Patrik: If your experience is that they’re not giving any information to anybody else, that you’ve authorized, why would they give me information? That’s my question.
Megan: Yes, exactly. Except of course that you are cousin and ICU … married to my cousin and ICU.
Patrik: Yeah. But even so-
Megan: Even so-
Patrik: What usually opens the door is simply either usually a passcode or password or something like that.
Megan: Yes. Yes. Gotcha. I can say to them, Auntie Luz and Patrik and Mary, I authorize you to speak to them and the password is going to be something.
Patrik: Yeah. Let’s do that. Yes.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Megan: And I’ll tell them. I’ll say-
Patrik: In a situation like that, wherever you can remove ambiguity, your life will only get easier.
Megan: Indeed. And I think easier for them as well because they’re very … They’re very funny about what they’ll tell me over the telephone. “Oh, we’ll tell you when you come in.” I say, come on, tell me now. And I push them and they tell me. They are a bit funny about the phone. That’s just too bad. I think if you push them, they’ll tell you.
Patrik: Sure.
Megan: And so what I’ll do Patrik, I’ll do that email to you, when I go in this afternoon, I’ll give your name, and say … They know I’ve been talking about you anyway. And I’ll tell them the code and I’ll say that you will be ringing.
Patrik: Yep. Probably best to give me a call once you’ve done that.
Megan: Yes.
Patrik: Right. So then I know safe to call.
Megan: Lovely. Yes. Now I leave there usually about 7:00 and that’s going to be very late your time though, isn’t it?
Patrik: So 7:00 PM will be 5:00, it’ll be 4:00 AM.
RECOMMENDED:
Megan: Oh. You don’t want to be ringing then.
Patrik: If I called at 10:00 PM your time, is that too late?
Megan: No. You’d have the new night nurse just settling in at that point. That could be good.
Patrik: By 10:00 PM, I’ll be up. It could potentially be even 9:30 PM when I’m calling. I’m usually up at 6:00, 6:30.
Megan: Right.
Patrik: My time, 6:00, 6:30.
Megan: Your time. Yeah. Well, I normally ring them at 10:00 because it’s about 10:00 that I get home and that always seems to be, well it seems to be a reasonable time. I don’t always get to speak to them. Maybe if we said 10:30.
Patrik: Yeah. 10:30 is fine. Yeah.
Megan: I’m just thinking, the last couple of nights, they’ve said, “Oh, she’s on a break. Something, something. Taking a blood or something.” And I said it doesn’t matter. I won’t ring back as long as Ryan is comfortable and that’s it. I would have thought 10:30 would be good. Or any time thereafter. Because they’re there all night.
Patrik: Sure. And they know, you mentioned to them that I’m in Germany so they would know that I might ring at odd hours.
Megan: At odd hours indeed. That’s why I said Germany not Russia. Because of the family connection and I didn’t want them, if any of them knew about your service, I didn’t want them to put two and two together.
RECOMMENDED:
Patrik: No.
Megan: I thought Germany is a bit more crafty.
Patrik: Yeah. No, that’s fine. Sure.
Megan: Lovely. Yes, and I will get that email off to you. And then Patrik, I’ll either email you or call you once it’s all in place.
Patrik: Yes.
Megan: Either email or call.
Patrik: Yeah. Please.
Megan: Fantastic. Thank you, Patrik.
Patrik: You’re very welcome. Thank you.
Megan: Thank you.
Patrik: Okay. Talk soon.
RECOMMENDED:
Megan: Lovely. Thank you Patrik.
Patrik: Thank you, bye, bye.
Megan: Bye for now. Bye, bye.
Patrik: Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!