Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How To Provide Better Intensive Care For Your Loved One?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Kendra as part of my 1:1 consulting and advocacy service! Kendra’s mom had a stroke and has been on a ventilator for 12 days in the ICU. The ICU team wants to do a tracheostomy on her mom and she’s asking what to do.
My Mother Had A Stroke and Ventilated for 12 Days in ICU. The ICU Team Wants To Do A Tracheostomy. What Should I Do?
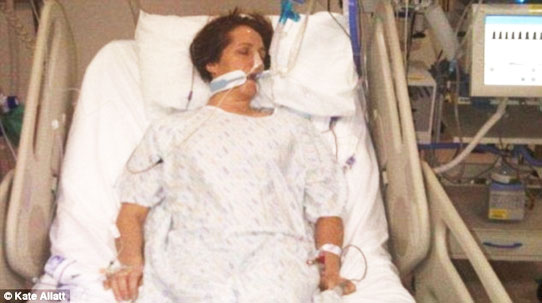
Hi Patrik,
My mother has been in intensive care for 12 days. She had a stroke and she’s been on a ventilator with a breathing tube. They’re trying to wean her off the ventilator. One day, she’s off for four hours and the next day she’s off for six hours, but she can’t go above six hours a day.
RECOMMENDED:
We’re asking the doctors, how did she do? They say, everything looks good. The next day we speak with the doctors and the doctors say that she will need a tracheostomy.
She was put out on the ventilator initially to suck out mucus on her chest. She came to ICU initially with a stroke. I noticed her coughing. So I’m thinking if she’s coughing, wouldn’t she cough out the mucus. She can’t because of the tube. I find this very frustrating on top of that.
My understanding is that her blood pressure is very low and she’s getting medications for that. I also believe they’re still sedating her at times. Even though she seems to be asleep most of the time. Can you please advise whether a tracheostomy is the right thing to do or not?
From Kendra
Hi Kendra,
Thank you so much for writing in and for being a client.
You may have heard me saying this before Kendra, but the biggest challenge for families in intensive care is that you don’t know what you don’t know. I can see you’ve done some of your research, but I can also see, there are a lot of gaps in your knowledge, and I can see that you don’t know what to look for, and you don’t know what questions you really need to ask when someone is in intensive care critically, like your mother is.
There are dozens and I repeat that there are dozens of things happening simultaneously. And unless you have a very good understanding of what those dozens of things that are happening simultaneously mean, you’ll really have no idea what’s happening.
Intensive care is a highly specialized area and unless you can break down the things that are happening into detail, you will never really understand of what’s going on, on a day by day basis. It’s not good enough for me to say, your mother is off the ventilator one day for four hours and except for six hours, we need to know what medications is she on, for example, right?
RECOMMENDATION:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
And if you’re telling me she’s still getting sedation, even though she’s asleep, most of the time she needs to come off the sedation, you know, when someone is having a stroke, like your mother does, there is a very good chance that your mother may need a tracheostomy just simply with a stroke patient often are unable to swallow.
Therefore, they’re at risk of aspiration and they’re at risk of an aspiration pneumonia. So even though your mother might be able to come off the ventilator eventually she may not be able to swallow and she may need airway protection with a tracheostomy.
If your mom was put on a ventilator initially to suck out the mucus, she had a bronchoscopy and that is certainly often very effective, but it may not be enough to get somebody off the ventilator.
You notice that she’s coughing and you think she can’t cough out the mucus because she’s got a breathing tube. That’s not entirely accurate. Patients with a breathing tube can cough. If they’re strong enough to bring up mucus, they can. But in your mother’s situation, the stroke may inhibit some of the coughing.
And also with the coughing, it’s not the tube that’s stopping her. It’s the sedation that’s stopping her. The sedation would stop her from coughing. She may also be on opiates, such as morphine or fentanyl, and the main side effect of morphine fentanyl or any other opiates is simply a respiratory depression. And that’s also inhibiting the cough.
So it’s not so much the tube that’s stopping her from coughing. It’s more like other issues such as the sedation and the induced coma. So where to from here? Your mother needs to be brought out of the induced coma. Your mother needs to have all sedation stopped. She needs to be mobilized, she needs to get in a chair, she needs to have physical therapy or physiotherapy and then hopefully they can strengthen her respiratory muscles, her breathing muscles. Hopefully she can then stay off the ventilator for more than four to six hours and if she can increase the time off the ventilator, she may be able to avoid the tracheostomy.
But again, just because she may be able to come off the ventilator, there’s still the swallowing issues, especially after a stroke. How can you assess that? You can assess that with speech therapy you know, speech therapy assessment needs to be made and they can also do a swallowing test.
RECOMMENDED:
So those would be the steps to find out whether the tracheostomy can be avoided or not. Now those are the next steps in the ideal scenario, she can avoid the tracheostomy, have the breathing tube removed and then move on to a hospital. Or if she’s going to have a tracheostomy, but time in ICU is probably going to be prolonged.
And also, even if she can come off the ventilator and she can go to a hospital ward there may be issues with nursing skills. What do I mean by that? Not every nurse on a hospital ward can look after a tracheostomy because simply that’s a specialist skill in ICU or for ICU nurses in particular.
So it is therefore very important that the assessment, whether your mom needs a tracheostomy or not is accurate and I can’t stress enough that your mother needs to be mobilized. She needs to have good nursing care. She needs to get regular washers every day and she needs to get in a chair, get physical therapy and so forth.
RECOMMENDED:
So that is my advice. I hope that helps Kendra.
Let me know if you have any other questions and go from there.
Thank you so much.
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!