Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Will My Loved One with COVID ARDS Survive With the Help of ECMO in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tara, as part of my 1:1 consulting and advocacy service! Tara’s brother-in-law is with a breathing tube and ventilated in ICU due to ARDS. Tara is asking if their loved one with ARDS benefit from a lung transplant in the ICU.
Will our Loved One with ARDS Benefit from a Lung Transplant in the ICU?
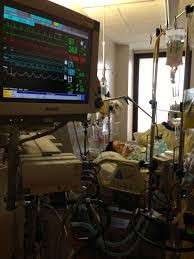
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tara here.”
Carmie: Yeah.
Sandy: You’re very helpful.
Carmie: You’re welcome. You all have a good night.
Patrik: Thank you so much, Carmie.
Tara: Thank you.
Patrik: Bye.
Carmie: You’re welcome.
Patrik: Thank you. Bye. All right. Are you there?
Tara: Okay.
Sandy: Yes.
Patrik: Right. Okay. I guess if I take anything positive from what she’s describing, it’s that from their end, that doesn’t seem to be any talk about fibrosis at this stage.
Sandy: Okay.
Patrik: I mean there will be a formal CT result and maybe there will be something in there, but I am wondering how can they even talk about fibrosis without a formal CT scan result.
Sandy: Right.
Tara: Yeah. I’m wondering the same.
Patrik: Right.
Tara: Yeah.
Patrik: And that’s why I’m sort of…
Sandy: She said that today before they even got the results back, I thought that was strange.
Patrik: Exactly. And you would have an indication even in a chest x-ray whether there is fibrosis or not.
Sandy: Okay.
Patrik: I mean, she sounded very experienced to me. She would know that.
Sandy: I agree.
Patrik: She didn’t struggle for answers for my questions which is good.
Sandy: Right.
Patrik: You know, it sounds to me like she is.
RECOMMENDED:
Tara: Now, what is the thing with the bleeding? Because Sandy had told me that he was really bleeding badly for a couple days. And then she said that some doctor, pediatric doctor or something came in the other day and said, “Oh, I know how to fix this”. And just instantly did something and it quit bleeding. And I thought Sandy, he had been bleeding.
Sandy: I think he made it sound like it was through his urine. Is that right?
Tara: Oh.
Sandy: Or not.
Patrik: Say that again, please. What did they do?
Tara: How was he bleeding? How did she say he was bleeding now?
Patrik: Yeah. So he’s bleeding from his catheter, from his urine, from his urinary catheter.
Tara: Oh.
Sandy: His urine today was rather than normal.
Tara: Okay.
Patrik: But I don’t know. The reason for the bleed could be a couple of reasons, but the most likely reason is probably heparin.
Tara: Right. Because she said he was bleeding from his, what is it called? The cannula or something? The other day, pretty bad.
Sandy: No, no. The other day he was bleeding from where they put like they drop his blood and stuff. And they kept like putting pads on and finally they had this one surgeon come in and he’s like, “Oh I know exactly what to do”. His nose was bleeding a couple times. And that stops too.
Patrik: Right. The risk of bleeding is higher when someone is on ECMO.
Recommended:
Sandy: Right. That what they said. She was like, this is nothing compared to a lot of ECMO patients. I was like, okay.
Patrik: Right.
Tara: Basically, I didn’t understand anything she told you.
Patrik: Right. Yeah. I’ll come to that.
Tara: From what she told you. I mean, do you think 3 weeks on ECMO or for not being crazy to give him a little more time for lungs to heal or…
Patrik: Yeah. Look, the longest I’ve seen people on ECMO is probably sort of 3 weeks at the most. But I can also tell you that at the moment with COVID that has gone out of the window. I do know that at the moment, patients stay on ECMO for longer than 3 weeks because the COVID is posing a new challenge for everyone.
Patrik: The problem is, even if you give him more time to heal. I talked about oxygen levels and I talked about arterial blood gases, and I talked about oxygen saturation levels. And those levels are dangerously low. What that means is even though he’s on maximum support, his oxygen levels are…
Tara: Yes.
Patrik: … she said, it’s in the 80s, which means it’s sort of ranging between 80 and 90%. A healthy oxygen level should be above 95%. He’s at a critical level. He’s at a critical level there. You may have heard me ask when I said, “What happens when they turn him”.
Tara: Right.
Patrik: When they turn him on his side and she basically confirmed that they can barely turn him on his side because then his oxygen levels drop to the 60s.
Patrik: And if oxygen level drop too low, you are running the risk that someone goes into cardiac arrest.
Tara: Right.
Patrik: Right. They’re achieving low levels of oxygen by not moving him. And when they do move him, they’re running the risk that they’re triggering a cardiac arrest.
Recommended:
Tara: Yeah.
Patrik: The other risk that’s happening with sort of low oxygen levels you might think, “Oh, 80%. That’s not bad”. But the reality is that if you and I check our oxygen levels, they’re probably above 95%. If it goes…
Tara: Yeah it was around 86%.
Patrik: Right. And that’s dangerous. And it’s not only dangerous I mentioned when you turn him, but it also could cause permanent brain damage if there’s not enough oxygen going to the brain.
Tara: Okay.
Patrik: Right. There’s a number…
Tara: Basically the question I had is obviously, he seemed like he was doing well before the ECMO. I know while they put him on it. But I don’t know what his oxygen levels he was maintaining before the ECMO. But he was surviving on it for 6 days. Basically, I mean, are they saying his lung have gotten worse? So if they took him off the ECMO now he wouldn’t be able to get enough oxygen with a ventilator?
Patrik: Oh, not at all. Not at all. She was saying that he has no tidal volumes going in. What that means is…
Tara: Oh, okay.
Patrik: … the lungs are so stiff that if they took him off ECMO now and they would ventilate him, they wouldn’t be able to get any air in.
Tara: I see.
Patrik: She was referring to a low tidal volume, tidal volumes of 30. John with his sort of height and weight should probably get tidal volumes of around 1000 mls. And she’s saying, he’s getting 30 mls. You could then start the theory of, if he’s getting 30 mls of tidal volumes with a ventilator, it might be an indication that there is fibrosis. Because of the scar tissue, the lungs are no longer elastic to put any volume in or that’s something that the CT scan might bring to light. But it could also be the infection. It could also be the infection. It could be lung fibrosis, but it could also be the infection that…
Tara: Still not cleared out.
Patrik: That’s right. That’s right.
Tara: I see.
Sandy: I feel like it’s hard for him to clear stuff out when he coughs.
Patrik: Yeah.
Tara: He is coughing a lot when they left in his sedation.
Suggested links:
Sandy: Yeah. It’s possible he still has fluid or stuff in there. I guess
Patrik: I should have asked it, do you know, have they done a bronchoscopy?
Sandy: Not that I know of.
Patrik: Right. Something I should have asked, but we can find out on our next call.
Sandy: Okay.
Patrik: I can…
Sandy: I can call her right now if you just get right back on with you guys.
Patrik: Yeah. We can, but it’s not a make or break situation, whether they’ve done a bronchoscopy or not. It’s certainly something that’s useful to know.
Sandy: Okay.
Patrik: But it’s not a make break question either that the CT…
Tara: What is the bronchoscopy? What does that mean?
Patrik: Yeah. The bronchoscopy means they are inserting a video camera into the lungs, through the breathing tube to…
Tara: Oh okay.
Patrik: Clear out mucus.
Sandy: yeah.
Patrik: And also to have a look in the lungs. Both to clear out and also they have…
Sandy: I don’t think they’ve done that.
Patrik: Right. Yeah. I would be surprised if they did. It’s sort of quite invasive if you only do it sort of as a last resort.
Sandy: Okay.
Patrik: But, to sort of determine the current situation, if they’re ventilating him with what they’re doing, plus the ECMO and he’s saturating 80, 85, 86, whatever. They don’t have any room.
Sandy: Right.
Patrik: They don’t have any room to move at the moment.
Tara: Sure.
Patrik: Which means if his lungs are not healing that they don’t have any room to move.
Tara: Correct.
Patrik: The only option going forward would be then, if the lungs are not improving, would be a lung transplant.
Suggested links:
Sandy: Okay. And is that really true, what they said, that can’t get one?
Patrik: I argue that everything in is negotiable. And whilst hospitals and transplant centers have criteria who qualifies for a lung transplant. We can look that up. What that criteria is. What I will argue is that, if John is tall and big, it will be more difficult to find suitable donor lungs for him just simply because of his size.
Sandy: Sure.
Patrik: If you have sort of an average person let’s just say.
Sandy: Okay.
Patrik: Let’s just say someone is sort of the average male with an average weight, it’s much easier…
Sandy: Yeah.
Patrik: … To match a donor.
Sandy: Right.
Patrik: Because there’s not many people out there with a similar sort of BMI.
Sandy: Okay.
Patrik: Right. I’ll take that argument from them. What I don’t take the argument is just his age should make him a candidate.
Sandy: Right. Well, there seems to be a lot of males his size.
Patrik: Right. Sure. Of course there are males of his size, of course. When you match a donor with a recipient, it’s also about it is about blood type. It is about…
Tara: Right.
Patrik: … The testing DNA. It’s not… A, someone has to die let’s call it for what it is. Someone has to die that matches.
Tara: Right.
Patrik: There’s a lot of things that need to fall into place. Now, don’t get me wrong. Those things sometimes do fall into place. I mean, I’ve looked after dozens of lung transplant recipients over the years in ICU it does happen of course.
Sandy: Okay.
Patrik: But there is definitely timing that needs to happen. And that’s all I can say. But the reality is if they’re not considering him in the first place that rules him out for it. The question is what needs to happen so they consider him.
Tara: Right. And you said there’s usually somebody else you talk to besides the doctor there or who…?
Patrik: Oh, if they have ECMO in this hospital, there’s a very good chance there is a transplant unit. Very good chance. Because whenever ECMO is provided as a service, ECMO is often used as a bridge to a lung transplant and sometimes for a heart transplant.
Recommended:
Patrik: Oh by the way, why is he in a children’s hospital?
Sandy: I have no idea.
Patrik: It could well be that at the moment with COVID, the demand for pediatric care is less and they’re using resources for adults. That might be the case. I don’t know.
Sandy: Yes.
Patrik: Right. When you go there, are there adults or children?
Sandy: Adults.
Patrik: Adults.
Sandy: I haven’t seen any children.
Patrik: Right. Yeah. If that’s the case, I wouldn’t be surprised if out of necessity. They’re using pediatric beds for adults because of the whole COVID surge. That would be my interpretation of it.
Sandy: Yeah. It’s such a huge hospital, I think have different wings for everything.
RECOMMENDED:
Patrik: Right. There is reference on the website for lung transplant for children. But not for adults. Having said that, I have worked in ICUs where it was an adult unit, but we actually did also pediatric lung transplants for ECMO. It can go both ways. ECMO is a specialty in and of itself, whether it’s for adults or for children.
Sandy: Right.
Patrik: It’s a specialty in and of itself. And as I said, often, the centers don’t necessarily discriminate between adults and children.
Sandy: Okay.
Patrik: I hope that’s shedding some light on the situation. I tell you what, I’m pretty things sort of, once you have a call with the doctors, or once we have a call with the doctor. Depending on the CT scan result.
Sandy: Yeah.
Patrik: If the CT scan result is talking about fibrosis, they will probably be very pushy for end of life. You got to be prepared for that.
Sandy: Okay.
Patrik: And when I say prepared, I’m not saying that you should be prepared for end of life.
Sandy: Right.
Patrik: What I am saying is we need to be prepared for the discussions around it. And what I mean by that is…
Sandy: Right.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







