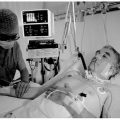
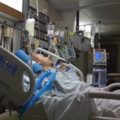
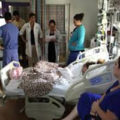
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tara, as part of my 1:1 consulting and advocacy service! Tara’s brother-in-law is with a breathing tube and ventilated in ICU due to ARDS. Tara is asking if his brother-in-law with COVID ARDS survive with the help of ECMO in the ICU.
Will My Loved One with COVID ARDS Survive With the Help of ECMO in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tara here.”
Sandy: Her name is Carmie. And he’s taking care of John.
Patrik: Carmie, is it? That will get us directly to Carmie, this number?
Sandy: It should. If not, they will transfer you to Carmie.
Patrik: Right. I’ll tell you what, I’ll call this number and then once they’re on the call, you do the talking, I guess, to get us in front of Carmie. Just give me a second.
Carmie: Hi, it’s Carmie.
Sandy: Okay. Carmie. Okay. I think we have everybody on now.
RECOMMENDED:
Carmie: Okay. If you don’t mind just tell the name one more time?
Sandy: Yes. My sister Tara, and then our friend Patrik.
Carmie: Okay. And you’re calling for?
Sandy: What’s that?
Carmie: Will you just tell me the patient’s name one more time.
Sandy: Oh yeah. John.
Carmie: Yeah. Perfect. I knew it was you, but just so we’re all on the same page and all that stuff.
Sandy: Okay.
Tara: Okay, yeah. I’m here. I’m Tara. And then Patrik, are you on?
Patrik: Yes. Carmie. How is John doing?
Carmie: What was that?
Patrik: How is John doing?
Tara: How is John?
Carmie: He’s doing about the same. He is maxed out on his ECMO support.
Recommended links:
Patrik: Right.
Carmie: He currently now has the two oxygenators.
Patrik: Yeah.
Carmie: And with that full support, his oxygen is in the 80s right now.
Patrik: Right. His oxygen saturation is in the 80s?
Carmie: Correct.
Patrik: Right. His blood gases would be really poor.
Carmie: They are.
Patrik: What are we talking about in terms of PO2 (partial pressure of oxygen) and CO2 (carbon dioxide)?
Carmie: CO2 have been around 47 and have been fluctuating. His PO2 (partial pressure of oxygen), the last one was 87 on a 100% on ECMO.
Patrik: Right. And is he on vasopressor or is he hemodynamically stable?
Carmie: He’s not.
Patrik: No. Okay.
Carmie: Right now. His blood pressure he’s maintaining himself. He’s just on sedation medication.
Patrik: Okay. And he’s deeply sedated, he’s not arousable?
Carmie: He’s not. Whenever he wakes up, he stops his ECMO circuit.
Patrik: Right.
Carmie: And his oxygen will drop down to 60.
Patrik: Right. I see. And what are you sedating him with? Some versed or fentanyl or…?
Recommended:
Carmie: He is on ketamine and dilaudid.
Patrik: Ketamine and dilaudid. Any opiates?
Carmie: Yeah, he’s on dilaudid.
Carmie: Yeah. And he’s on scheduled oxycodone as well.
Patrik: Right. I see. And all his other blood works like hemoglobin, white cell count, and lactate.
Carmie: So his last lactate was this morning. It was 1.0. And his CBC, his most recent white count is 6.
Patrik: Right.
Carmie: His recent hematocrit is 30.
Patrik: Okay. And he hasn’t had any blood transfusions in recent days?
Tara: He has not, but he’s now bleeding pretty much straight blood out of his foley catheter.
Patrik: Right. Okay. He’s on heparin?
Carmie: He is on heparin for the ECMO.
Patrik: Yeah. And sort of his APTT (activated partial thromboplastin time) is holding?
Carmie: He actually do heparin assays for ECMO heparin and he’s right on goal at 0.5.
Patrik: Right. Okay. And kidneys are working?
Carmie: They are, minus the blood that we are having coming out of it. But his last creatinine was 0.45.
Patrik: Right. And he’s making urine.
Suggested links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Carmie: He is.
Patrik: Okay. And…
Carmie: He is on Lasix with that though.
Patrik: Right. Sure. And sort of with the initial COVID /ARDS, you were treating that with steroids and Remdesivir, I guess that’s sort of what you did initially?
Carmie: He was not here with us when he got admitted.
Patrik: Right.
Carmie: But from what they were saying outside hospital that is what they did.
Patrik: Right.
Carmie: But since being here, no, we have not.
Patrik: Right. I guess your focus was mainly on the ECMO side of things.
Carmie: Correct. And once you’re out of that initial diagnosis we can’t continue that treatment.
Patrik: Yeah. Okay. What do you think are the next steps?
Recommended:
Carmie: What steps would be for you all to have your family meeting. You know, with the team. And as of right now, the doctors that perform the tracheostomy don’t feel that he is stable enough to do so.
Patrik: Right.
Carmie: We’re kind of at a standstill right now.
Patrik: Sure. You are talking about 100% FIO2 (fraction of inspired oxygen). Did you say PEEP (positive end expiratory pressure) of 10?
Carmie: Yes.
Patrik: Right. Okay.
Carmie: And he’s on a 100% on the ECMO, but on the ventilator.
Patrik: Of course.
Carmie: So he’s only on 50 on the vent.
Patrik: Yeah. I understand.
Carmie: But that just says he doesn’t really have much tidal volume. They’re about 30.
Patrik: Yeah.
Carmie: And so it wouldn’t do much.
Patrik: No, wouldn’t do much. I understand. And there has been a CT scan and in the last 24 hours?
Carmie: He did. We went down for a CT chest and abdomen around one o’clock
Patrik: Right. And the results for that are back or…?
Carmie: They are. It showed nothing remarkable.
Patrik: Okay.
Carmie: Then for his test, it’s just bilateral lung consolidation from COVID.
Patrik: Right.
Carmie: But it’s new by any means.
Patrik: Sure. Okay. There is no talk about fibrosis?
Carmie: There’s not, not the CT scan, just from consolidation.
Patrik: Okay.
Carmie: That is the initial read though. The final read probably won’t be back until tomorrow.
Patrik: Yeah. I understand. And other than that, I would assume he’s on nasogastric tube (NGT) feeds and he’s getting feeds and he’s absorbing feeds, opening bowels. There’s no issue there?
Carmie: Yeah. No issue.
Patrik: Okay. I guess it’s a case of probably waiting for the final result of the CT scan and…
Carmie: Right.
Patrik: With the bleeding, what did you see? Is his hemoglobin dropping? Bleeding… Doesn’t sound like it’s under control at the moment. Does it?
Carmie: Yeah. It looks like it drops two points in 12 hours, but we don’t transfuse unless your hematocrit is less than 30% and we’re right at 30.
Patrik: Yeah. Okay. And with the bleed, I guess you’ve got to weigh up the risk. Can you stop heparin whilst being on ECMO which is very unlikely.
Carmie: Right. They have a theory right now that the bleeding is because we’re running at such high flows in order to keep him oxygenated.
Patrik: Right.
Carmie: And so we can’t drop the flow and we can’t stop the heparin, so it’s one of those things where…
Patrik: Yes.
Carmie: … if we were to stop either those, it would be more risky.
Patrik: Yeah. Got to weigh up the pros and cons. I hear you.
Recommended:
Carmie: Right.
Patrik: And when you turn John maybe to give his back a wash, can you do that? Or would he drop his saturation to a dangerously low level?
Carmie: It’s intermittent. Little small movements are okay. But anything like big turns like that he drops pretty low.
Patrik: Yeah. Okay.
Tara: Is he on his back right now? Or is he on his back this whole time?
Sandy: He’s on his back because of the …
Carmie: He’s turned left and right. And supine.
Patrik: Okay. Tara, Sandy, I don’t have any other questions at the moment. I don’t know what…
Tara: Okay.
Patrik: Whether you have any…
Tara: Perfect. Thank you very much.
Sandy: Yeah.
Carmie: You’re welcome.
Patrik: Thank you so much, Carmie. Thank you so much.
Carmie: Yeah. You’re more than welcome.
Patrik: Appreciate it.
Carmie: Y’all have any other questions?
Tara: No, I’m good.
Sandy: Thank you though very much.
RECOMMENDED:
Carmie: Yeah.
Sandy: You’re very helpful.
Carmie: You’re welcome. You all have a good night.
Patrik: Thank you so much, Carmie.
Tara: Thank you.
Patrik: Bye.
Carmie: You’re welcome.
Patrik: Thank you. Bye. All right. Are you there?
Tara: Okay.
Sandy: Yes.
Patrik: Right. Okay. I guess if I take anything positive from what she’s describing, it’s that from their end, that doesn’t seem to be any talk about fibrosis at this stage.
Sandy: Okay.
Patrik: I mean there will be a formal CT result and maybe there will be something in there, but I am wondering how can they even talk about fibrosis without a formal CT scan result.
Sandy: Right.
Tara: Yeah. I’m wondering the same.
Patrik: Right.
Tara: Yeah.
Patrik: And that’s why I’m sort of…
Sandy: She said that today before they even got the results back, I thought that was strange.
Patrik: Exactly. And you would have an indication even in a chest x-ray whether there is fibrosis or not.
Sandy: Okay.
Patrik: I mean, she sounded very experienced to me. She would know that.
Sandy: I agree.
Patrik: She didn’t struggle for answers for my questions which is good.
Sandy: Right.
Patrik: You know, it sounds to me like she is.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!