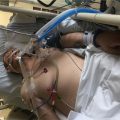
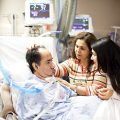
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tara, as part of my 1:1 consulting and advocacy service! Tara’s brother-in-law is with a breathing tube and ventilated in ICU due to ARDS. Tara is asking what could be the reason behind the ICU team not agreeing for a lung transplant for her brother-in-law in the ICU.
What Could Be the Reason Behind the ICU Team Not Agreeing for a Lung Transplant for our Loved One in the ICU?
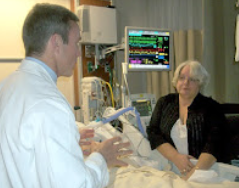
Tara: Yeah. Because she was asking him we’ve read so many stories of people who have been on the ECMO for 4 or 5, 6, even up to 8 weeks.
Patrik: Yeah.
Tara: Or more, and make a full recovery. And so how can you say that his lungs can improve anymore after just over 2 weeks?
Patrik: Yeah.
Tara: Especially when they initially said at least 2 weeks before the ECMO.
Sandy: I said that he said, you need to be very careful what you listen to..
Patrik: Sure. He’s giving… Yeah, absolutely. He’s trying to prepare you for their agenda and their agenda is to stop treatment and…
Sandy: Yeah.
Patrik: Is trying to plant that seed over and over again. Now I think that’s what we need, we need to get down to the more nitty gritty when he says “The lungs are no longer working or something to that extent”. He’s probably referring to that he might develop lung fibrosis. Did he say something like that?
Tara: Yes. He said his lung are fibrous.
RECOMMENDED:
Patrik: Yeah. So when…
Tara: Sorry. Sandy said also, sorry to interrupt. Sandy said also she kind of goes along with this. I’m not sure what this means, but they took him to take and did a full chest x-ray of his lungs.
Patrik: Yes.
Tara: And told her that they would have the results of that tomorrow. We’re not sure why this doctor told her that before they had the results from the X-ray…
Patrik: Right.
Sandy: A scan, they put him down to another room for it.
Patrik: Oh, it would’ve been a scan. Would’ve been a scan.
Sandy: Okay.
Patrik: Okay. Because normally a chest x-ray you have the results within minutes.
Sandy: Yeah. And they do that in the room usually.
Tara: Okay. Well this is a scan.
Patrik: Must be a CT scan. Okay. Tara, I can’t remember. Was it you that told me yesterday, they wouldn’t take him for a CT scan initially?
Tara: No, I just said they did that today, but I’m saying the doctor told her this before they have the results of the scan they did today.
Patrik: Right.
Sandy: It took them 2 days I think a whole body CT scan too. I thought they said they were doing a chest CT scan or something.
Patrik: Okay. I remember Tara, you were telling me yesterday that they did talk about a tracheostomy. Just remind me what were the initial discussions around that?
Recommended:
Tara: The initial discussion last week, they told us that would be the best option for him. Because they said, “Letting you know. Just be realistic”. If they are able to wean him off the ECMO or extracorporeal membrane oxygenation. Once they do that, he could be 2 weeks still on the ventilator after that. And the reason for doing that would be because it’s going to be that long term, it would be more comfortable for him. And also even right now, they thought that they could possibly reduce the sedative, and let him wake up but something was aggravating so much when they tried to wake him up right now.
Patrik: Very much so.
Sandy: Yeah. We tried to call.
Tara: They told us that was the best thing and that’s what we should do. But then this week they decided that it was basically pointless, I guess, or it would change course. That’s how they worded it.
Patrik: Okay. I’ll come back to the tracheostomy in a minute. I have one other question. Has a lung transplant ever been discussed?
Sandy: Yes. They said that was not an option because his BMI was too high.
Patrik: Right. But from what I understand, your husband is very young.
Sandy: Yes.
Patrik: Right. And who did say that? That the lung transplant is not an option? The same doctor that’s talking about lung fibrosis. And that’s talking about tracheostomy. Is that the same person?
Sandy: No. It was a different guy.
Patrik: Right. Do you know who…
Tara: That just a part of frustration too. It’s because you’ve had so many different doctors everything.
Patrik: Yeah.
Tara: And they all tell you something different. So it’s just kind of frustrating.
Suggested links:
Patrik: Right. And if somebody would talk about a lung transplant, it wouldn’t necessarily be the ICU. It would be the transplant team. Right.
Sandy: Okay.
Patrik: But it probably… Look, the reality is this, that if his lungs are developing fibrosis or have developed fibrosis, ECMO can keep him alive, but he’s moving out of the territory where his lungs can be healed. And a lot of patients that end up with lung transplants have what’s called pulmonary fibrosis, which at the end of the day’s fibrosis in the lungs. If the diagnosis of the fibrosis is accurate, ECMO at the moment is keeping him alive. But the goal of the ECMO initially is always to give the lungs a rest and get them to heal.
Tara: Yeah.
Patrik: That is the goal of ECMO. Just as much as it’s the goal of prone position. Now if the lungs have developed fibrosis, again is moving out of the territory where the lungs can be healed. Because there’s too much damage in the lungs now probably through the virus and the only option out of this dilemma, as far as I can see, without having spoken to the doctors and maybe getting more information would be lung transplant. When was the first time lung transplant was mentioned?
Sandy: I asked about a little over a week ago.
Patrik: Right. You asked about it.
Tara: Yeah.
Sandy: Yeah.
Patrik: Yeah.
Recommended:
Sandy: And he claimed he tried his hardest, but his BMI was too high.
Patrik: Right.
Tara: He said the doctor, he tried his hardest to what?
Sandy: To make it work.
Tara: Oh he…
Sandy: He called another hospital and they told him, no.
Tara: I see.
Patrik: Would be very advantageous for you to find out who this doctor was, what their qualifications are.
Sandy: Okay.
Patrik: I would argue strongly that at your husband’s age he would be a candidate. Yes, I hear all about BMI.
Sandy: Yeah.
Patrik: But I would argue just your husband’s age would get him into that category.
Sandy: Okay.
Tara: All the nurses are always positive as far as we know. As far as just his vitals and his they said his, they’re always making comments. “His circulation is so good. It feels so good”. That kind of stuff, what that means. But he…
Patrik: It means that ECMO is working.
Tara: Yeah. Sure. Basically, like I said, I’ve read a lot of, I mean, reports and studies. I’m kind of a researcher.
Patrik: Yeah.
Tara: It’s hard, the lungs can take months to heal and they can…
Patrik: Yup.
Tara: There’s people that are on for 8 to 10 weeks and then their lungs start improving. But are you saying that they don’t think that they could heal still at that point?
Patrik: I would argue if the diagnosis of lung fibrosis is accurate, I would argue that the option that the lungs are going to heal is very diminished. And the simple reason for that is basically fibrosis means there is scar tissue in the lungs.
Tara: Right. I understand that.
Patrik: Yeah. So if you have a virus or a bacteria in the lungs that you can heal with medication with giving the lungs a break. That is the ultimate goal of ECMO or even of proning, that’s the ultimate goal of that in combination with whatever they would’ve done for, COVID probably Remdesivir and probably steroids and all of that.
Tara: Right.
Suggested links:
Patrik: That is the ultimate goal of that. If that, for whatever reason doesn’t succeed, the lungs will unfortunately will develop in into fibrosis and you will have scar tissue as a result of that. And once there’s scar tissue in the lungs, you won’t achieve any gas exchange. Oxygen won’t go into the artery.
Tara: Right.
Patrik: Just that the oxygen CO2 barrier just is blocked. And the only way out of that really is a lung transplant. Now granted you would need to hear that at least a number of times that pulmonary fibrosis has been diagnosed. I wouldn’t just take it for gospel just because you heard…
Tara: After 2 weeks, but…
Sandy: Okay.
Patrik: They’ve been telling you that for the last 2weeks?
Tara: No, I’m saying he’s been on the ECMO for 2 weeks. That just the new thing for today.
Patrik: Yeah. You would need to wait for the CT scan results and somebody confirming that.
Sandy: Okay.
Patrik: But yeah, I would argue over the years, 9 out of 10 lung transplants that I’ve seen in ICU would’ve been for fibrosis. But that might make it difficult, such a tall man to find the right set of lungs. But then again, if they don’t start looking for it… Is there any other premedical history that would potentially exclude him from a lung transplant?
Sandy: No.
Tara: No, no. He was very healthy. He didn’t have any health issues at all.
Patrik: Yeah. Okay. What else is happening that you’re aware of? Are the kidneys working? Is he on dialysis?
Tara: No. His kidneys are functioning, right Sandy?
Sandy: Yeah.
Patrik: Right. Kidneys are working. Do you know if he’s on inotropes or vasopressors? Have you heard of that?
Sandy: Not really.
Patrik: Right. No. That’s OK. We’ll find that out.
Tara: We haven’t really don’t really know any info.
Patrik: Yeah, yeah, no, No. That’s fine.
Tara: … still have to ask.
Patrik: Yeah. No, that’s fine. Look, I would to get all of that information. The next step is for us to talk to the nurse to begin with and it’ll be good.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Tara: Yeah.
Patrik: Yeah. It’ll be good to get as much information from the nurses as possible. And then we are better prepared for the doctors.
Tara: Okay. Do you want me to add her now?
Patrik: I think so. I think the best way to approach it and keep it low key is you can just say, look I got Patrik on the phone. He’s a family friend.
Tara: Yeah. She’s already expecting a call.
Patrik: Oh good. Good.
Sandy: I’ll get her on now. Oh, it wouldn’t work. I told her Patrik would call.
Tara: Okay. Patrik, do you want to give it a try or?
Patrik: Yep, absolutely.
RECOMMENDED:
Sandy: Her name is Carmie. And he’s taking care of John.
Patrik: Carmie, is it? That will get us directly to Carmie, this number?
Sandy: It should. If not, they will transfer you to Carmie.
Patrik: Right. I’ll tell you what, I’ll call this number and then once they’re on the call, you do the talking, I guess, to get us in front of Carmie. Just give me a second.
Carmie: Hi, it’s Carmie.
Sandy: Okay. Carmie. Okay. I think we have everybody on now.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!