What is acute severe Asthma?
Asthma is a chronic inflammatory disease of the airways characterised by reversible airways obstruction and bronchospasm.
Acute severe Asthma is severe asthma that does not respond well to immediate care and is a life-threatening medical emergency. Ensuing respiratory failure results in hypoxia, carbon dioxide retention and acidosis. The exact mechanism underlying the development of an acute severe asthma attack remains elusive but there appear to be two phenotypes:
- Gradual-onset – in about 80%, severe attacks develop over more than 48 hours. These are associated with eosinophilic infiltration and slow response to therapy.
- Sudden-onset – often in association with significant allergen exposure. Patients tend to be older and to present between midnight and 8 am. This type of attack is associated with neutrophilic inflammation and a swifter response to therapy.
- What does the Respiratory system do?
- Abnormal and or inadequate breathing
- Acute Severe Asthma
- What Happens in Intensive Care?
- How long will my loved one remain in Intensive Care?
What does the Respiratory System do ?
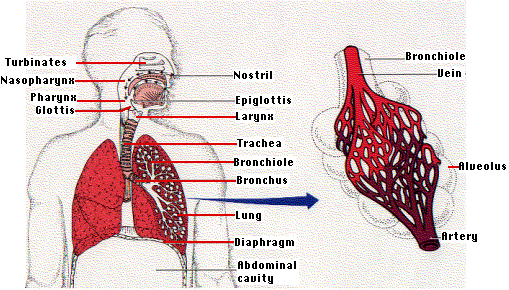
The respiratory system consists of the lungs, airways and blood vessels. The respiratory system inhales oxygen into the body and exchanges oxygen by removing carbon dioxide from the body. A normal breath requires a complex coordination between the nervous system (brain & spinal cord) and the muscles of breathing (including the diaphragm and muscles between the ribs).
Abnormal and or inadequate breathing can occur as a result of:
- An interruption to the nervous system (head injuries or spinal injuries for example)
- Barriers to the absorption of oxygen (eg fluid or secretions in the alveoli);
- Obstruction to the flow of gases through the lungs, both breathing in or out (eg asthma);
- Damage to the rib cage such as rib fractures or flail chest(in motor vehicle trauma for example);
- Pneumothorax(deflation of one part of the lung)
- Haemothorax(infiltration with blood to parts of the lung)
- Pain, which makes taking a normal breath difficult.
A number of respiratory conditions can result in respiratory failure and require Intensive Care or High dependency Unit admission. It is often that respiratory failure results in ventilation support (help with breathing). This support may be through the use of oxygen masks, BIPAP or Non- Invasive Ventilation(NIV) or via a Breathing Tube (endotracheal tube) and Ventilators (Breathing Machines)
Severe Acute Asthma – what happens?
A severe acute asthma attack is an emergency situation requiring prompt airway management. The airway is very sensitive to stimuli (such as smoke, pollens, fumes) and react with severe inflammation and spasm of the airways. The airflow in the lungs is obstructed.
If your loved one is a known asthmatic experiencing an asthma attack, which is not responding to their usual emergency treatment plan and is experiencing worsening symptoms over hours to days and slowly deteriorate to where they require emergency management in Intensive Care.
Sometimes Asthma Patients experience a sudden overwhelming attack where the airways shut down and the Patient deteriorates quickly. Obtaining emergency assistance immediately is imperative in this last group.
What happens in Intensive Care?
- After the diagnosis of the acute asthma attack has been made, efforts will be directed towards treating and reversing the airway obstruction(spasm)
- Initially oxygen and respiratory support might be commenced via na oxygen mask or via Non- Invasive Ventilation(NIV) or BIPAP ventilation
- In Intensive Care your loved one will very likely require a Breathing Tube (endotracheal tube) and mechanical ventilation on Ventilators (Breathing Machines)
- Medications given are nebulisers such as Ventolin(Salbutamol), Atrovent, Pulmicort. Salbutamol may also be given intravenously. Furthermore, steroids/ cortisone and other medications may be given to control the asthma attack.
- Your loved one will be closely monitored using a Bedside Monitors.
- Frequent Chest X-rays and blood tests (Blood& Pathology tests in Intensive Care)especially arterial blood gases (ABGs) will be performed regularly.
How long will your loved one remain in Intensive Care?
Your loved one will usually stay in intensive care for a few days if they have no other complication.
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual patient variation.It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


