Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can I Stop the ICU Team From Pushing Me to “Withdrawal of Treatment” for My Wife?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ricky, as part of my 1:1 consulting and advocacy service! Ricky’s wife is critically ill in ICU with COVID and Ricky is asking why the ICU team can’t wean his wife off the sedation so she can come off the ventilator.
My Wife is Critically Ill in ICU with COVID. Why Can’t The ICU Team Wean My Wife Off the Sedation So She Can Come Off the Ventilator?
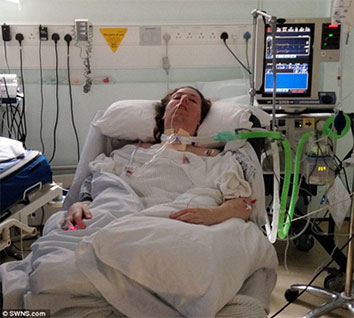
Patrik: Hi, Ricky. Can you hear me?
Ricky: Hello.
Ricky: Yeah, I can hear you. Good morning.
Patrik: That’s wonderful.
Ricky: Hello. Can you hear me?
Patrik: I can hear you fine.
Ricky: Yeah. Let me put my speaker on.
Patrik: I got your email, Ricky. So your wife is in ICU. She’s been in ICU for three weeks?
RECOMMENDED:
Ricky: Yeah.
Patrik: With COVID?
Ricky: Yeah, yeah with COVID, pneumonia.
Patrik: What’s your biggest challenge at the moment?
Ricky: Maybe it’s that I don’t know how long she’s going to stay there because there is no headway about her recovering. They’re just saying that it’s COVID, her body needs to fight it off, and her lungs needs to heal. So that’s why she’s on sedation that she can’t handle the… So it’s just I don’t know how long she’s going to be there.
Patrik: Can you see her? Can you visit her?
Ricky: No. No, no, no. In a normal hospital here, it don’t allow visitors and the ICU is high risk.
Patrik: Of course. Of course. Are you the decision maker while she’s in ICU? Are you the one giving consent for procedures signing off on it?
Ricky: Yes. Yeah.
Recommended links:
Patrik: Okay. And with the COVID, have they had her in prone position? Do you know what I mean by prone position?
Ricky: Yeah, prone position, that is what I didn’t ask them if they call. Or maybe I’ll call them today to ask them about that.
Patrik: But if she’s been in there for three weeks now, she would have probably had it in the early stages, I would think.
Ricky: Yes, exactly, and she’s on tracheostomy.
Patrik: She’s got that already?
Ricky: Yeah. After a week of admission, they did that.
Patrik: Right. How old is your wife?
Ricky: She’s 57.
Patrik: Right. And otherwise, previously fit and healthy previously?
Ricky: Yeah, just high blood pressure.
Patrik: High blood pressure, okay.
Ricky: High blood pressure and an inflamed heart. She has a big heart.
Patrik: That was before COVID?
Ricky: Yeah. Before the COVID, yeah. Yeah. She was born with it anyway. She has this…
Patrik: Right. And in those three weeks, has she been improving?
Ricky: Yeah. They say she’s responding to treatment just that for last week, she had a chest infection. Then, which… because her oxygen requirement has been stable 35 to 40% all the while, so that particular… When they discovered that she had an infection, and before then they tried to reduce the sedation. So they say each time they reduce her sedation, she’s agitated and her blood pressure shoots up, so they have to put her back.
Suggested links:
Ricky: So with the infection of the chest and the infection in her blood, which is sepsis, so her oxygen requirement, that is increased to about 65. Because they were doing daily dialysis to her, so the doctor said since then, since she was responding to treatments and everything, and because she was improving, there is no need for daily dialysis… so they did it every other day to see how it goes.
Ricky: So, I think because they didn’t do the daily dialysis, that caused her having fluid in the lungs. “Maybe it’s because of the drop in the dialysis that led to the fluids in the lungs or all that,” so I said, “Please,” they should start the daily dialysis. They said they were going to put her on antibiotics also to clear the chest and the blood, so they put her on antibiotics for a week and they started dialysis.
Ricky: So then, two days later when they called, they said, “Ah, she became stable again.” Her oxygen requirement dropped to 35, which was same as before. So it’s not that the dialysis… They gave her blood also, for two days because she has been anemic. Now, she has anemia.
Patrik: Anemic before COVID?
Ricky: Yeah. Before COVID, yeah. Now and they’re just not that serious. The doctor told her to take vitamin C, folic acid, and all that, so vitamin D.
Patrik: Right. Normally, one of the advantages of a tracheostomy is that you switch off sedation fairly quickly. Do you know why they haven’t stopped sedation when they did the trach? Do you know?
Ricky: Pardon?
Patrik: So, one of the big advantages for doing a tracheostomy, right?
Ricky: Yes.
Patrik: One of the big advantages is that you should be able to stop sedation very quickly. Why are they not…? And I hear that she gets agitated. I heard you saying that, but there must be, there are ways forward. I am wondering why they haven’t-
Ricky: Yes.
Patrik: Why?
Ricky: Yeah, we asked them why are they not taking off the sedation? They said the reason is that they are looking for a sedation that will fit her… I don’t know how they explained to me. Yeah, they’re looking for a particular sedation that would match her. So when they try to take her off, she doesn’t get that agitation and they are controlling her blood pressure. That was what they said.
Patrik: Controlling her… Okay. Do you know whether she’s on any vasopressor or inotropes? Do you know what I mean by that?
Ricky: No.
Recommended:
Patrik: Do you know whether she’s on any medication for her blood pressure?
Ricky: Yes. They are giving her. When they were trying to reduce the sedation, her blood pressure goes up. So they gave her medication for blood pressure.
Patrik: To keep the blood pressure down?
Ricky: Yeah. Down, yeah.
Patrik: What are they saying about the next steps?
Ricky: Yeah because I called yesterday. It was a nurse that picked. She just generalized and she said they are very busy. It’s the doctor that’s supposed to call me. It’s like the doctors, they know more, so she just said she’s so poor, that her lungs, it still needs time to heal. That is why she’s still on heavy sedation. So at least to keep her relaxed for the healing process and the COVID refuse to go, it’s not going away yet.
Ricky: So then I asked her, “What are they giving for the COVID?” They said “They’re giving…” I asked them about the blood, when they gave her blood, is it plasma? That situation when they have to take a sample from a previous COVID patient. So she said no, it’s just the normal blood they gave her. That procedure is not… They are not using that yet, so that they just gave her normal blood, so that she is still very poor, or her lungs still needs to heal. That’s why she’s on heavy sedation. I think I need to speak with the doctor because that was a nurse, a general nurse. She doesn’t even know. I don’t know.
Patrik: How do you get updates? Who’s updating you?
Ricky: It’s the doctors I used to call every day. Yesterday, I was able to talk to the nurse. The last two days, I spoke to the nurse in charge.
Ricky: Yesterday I spoke to another nurse, but not in charge of her. She just gave the general feedback. She said doctor tried to ring me the day before, which I saw the miss call. That’s why I called back, so she said they are not in the same section, that they’ll give me a call back. So yesterday she just said, “If there’s any improvement, they’ll let me know” So I’ve not got a call from the doctor.
Patrik: Right. And dialysis every second day?
Ricky: No. They said now it’s every day. They do it every day.
Suggested links:
Patrik: Every day. And how long has she been on dialysis for?
Ricky: Yeah. She’s been on dialysis since 4th day..
Patrik: Oh, so quite some time?
Ricky: Yeah. Yeah, before now. Before now, she already has problem with her kidney anyway because then doctor used to say, “It’s fluctuating. It goes up and down; goes up and down that she should be careful.”
Patrik: Right. Is she in a big ICU?
Ricky: Yeah. In a big ICU. She used to work there.
Patrik: Right. Oh, so she might’ve…? She caught it at work, did she?
Ricky: Yeah. Since the COVID, I haven’t work there because of the high-risk.
Patrik: Yeah, right.
Ricky: Last week, I was planning to work, to book a shift there, so I can see her, but the manager… I called the manager if she can put me in because there’s always shifts on where I am a bank worker, so there’s always shifts on that ward: ICU. So I saw a shift; I wanted to book it. I said, “Let me speak with her.” I spoke with the manager. The manager said I can’t walk there since I’m a family member. My wife is there, that they don’t allow it.
Patrik: Don’t allow that. Fair enough. Fair enough. What I can certainly do for you is I can certainly help you talking to the doctors. I think that would be very helpful because you’ve got a good understanding of what’s happening, but there’s probably another 10 things that are happening that we need to ask to really find out, what are her blood result, chest X-ray results? What are her ventilator settings, in particular? Is there any chance for her to get off the ventilator soon? What sedation is she on? There’s a whole series of questions I would like to ask.
Patrik: If you want me to get on the phone with you with the doctors, I do charge a fee for that, and I think we’ve emailed that to you. You can have a look and decide from there.
Ricky: How much is it?
Patrik: It depends what you want. We have several options. I have several options. You can start with one hour. You can take me up for four days, for seven days, for 14 days. You could just start with an hour. I also offer some email consulting where you have access to me via email. That’s obviously a lot cheaper. I emailed that to you, but the prices are roughly… I think its £119 just for an hour. I have to look it up. Hang on. I’ll bring it up. Just give me one second and then I can tell you exactly how much it is. Just give me one second, please.
Ricky: Is it online? Is it not on the site?
Patrik: It’s on the site-
Ricky: But the price is not on the-
Patrik: It’s on the site, but we email… No, no. It’s on the site, but most of the prices on the site are in US dollars.
Patrik: So it’s £119 for an hour. It’s £459 for four days; £599 for seven days and for 14 days, it’s £999. If you start with the hour, it can be credited towards the four day or the seven day option. If you wanted to continue beyond the hour. It’s all in the email. It’s all in the email that we sent you, but I can send it to you again.
Ricky: Yeah. What I want to ask, the one hour, because you can’t be on the phone with the doctors for one hour, can it be spread?
Patrik: Absolutely. Absolutely can be spread.
Ricky: Okay, yeah. So, the questions, you said that about the questions I need to ask, what sedation she is on.
Patrik: No, that’s just one of the questions. What sedations is she on? What ventilator settings is she on? What medications?
Recommended:
Ricky: What ventilator?
Patrik: Ventilator settings. But then, they will give you the ventilator settings, which probably won’t make a lot of sense for you. Right?
Ricky: Okay. Yeah.
Patrik: That’s where I’m coming in. What medications is she on? What are chest x-ray results? What are arterial blood gas results? As you can see, it’s such a very specialized area and, yes, you will get answers with my questions, but then you’ve got to ask the next question. It’s a complex area. You’ve got the most important questions, but once you’ve got the answers, I would have more questions for them, depending on their answers. You know?
Ricky: Yeah.
Patrik: Do you know what ventilator settings she’s on? Have you got any idea?
Ricky: Ventilator settings? No. They just said she’s on 70%, then 70%.
Patrik: Right. There’s are other numbers we need to know for someone on a ventilator. That’s why I’m saying it’s a very complex situation. And I would also want to know what sedation is on to find out how likely is it for her to come off the ventilator soon. You know?
Suggested links:
Ricky: Yeah. They told me that. Ahhh. I’ll ask again. I’ll just call them to ask them this additional-
Patrik: Right. Right.
Ricky: They do tell me all the drugs. They do tell me, but just because the names are so difficult, so I just…
Patrik: Yes, exactly. I understand and that’s why you need someone like me that can help you with this.
Ricky: Yeah. Yeah.
Patrik: So, I’m sure it’s a very tough ride for you. Three weeks of not seeing her, it’s a very tough time.
Ricky: Yeah. Yeah.
Patrik: Ricky, I need to leave. I only have 15 minutes of my free time. I do need to leave in a second. I will email you those options again, and then you can go from there. Please, note I do work on a first come first serve basis.
RECOMMENDED:
Ricky: Yes. Okay, thank you very much.
Patrik: Okay, thank you so much, Ricky. All the best for now. Thank you.
Ricky: Bless you.
Patrik: Bye-bye. Thank you. Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







