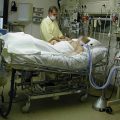
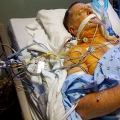
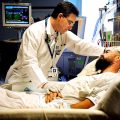
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Can My Brother with COVID in ICU Get Off the Ventilator if He’s in an Induced Coma?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Kenneth, as part of my 1:1 consulting and advocacy service! Kenneth’s brother has COVID in ICU with a breathing tube and on a ventilator. Kenneth is asking how to be in control and advocate for the best medical treatment for his ventilated & critically ill brother in ICU.
How Can I Be In Control and Advocate for the Best Medical Treatment for My Ventilated & Critically Ill Brother in ICU?
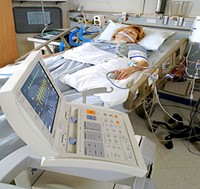
Patrik: Well when you’re ready, my argument there straight away would be, when the hospital is ready, make a referral to a hospital that has ECMO. So they are operating from what they’ve got available there. And I also argue that the smaller hospitals, smaller ICU, I would argue, doesn’t have all expertise in looking at all options. So I believe they’re operating from a mindset of limited resources, limited expertise, whereas, okay, they’re talking about comfort care, how old is your brother?
Kenneth: 36.
Patrik: Oh my goodness, he’s so young. My argument would be, okay you’re talking about comfort care, what about looking at other treatment options in other hospitals?
Kenneth: I try to ask that, but I think even with his doctor from the previous hospital, they wouldn’t do anything differently than what they’re doing, and I don’t know that could be true, that’s why I became interested with your advocacy and consulting services at Intensive Care Hotline.
Patrik: Absolutely.
Kenneth: I wanted to just see, even through this process, I wanted somebody else, a medical professional where we pay and can give updates and help us. I don’t know what services, whether you’re part of seeing with the doctor to just help… The hardest thing is that, now my dad is in the hospital with my brother and just knowing… Then he’s coughing, I’m like, “Please don’t tell me you have COVID.” And whatever happens to my brother, I want to know that we have done what we can do. I don’t trust the hospital, who doesn’t give somebody a COVID test.
RECOMMENDED:
Patrik: Yeah. You can’t, no.
Kenneth: …medical neglect to the extreme, to the extreme. And this man goes to this hospital, they’ve done him wrong because they don’t really know… I don’t want to get into that part, but they’ve done them wrong in the past, I want to know that we’ve exhausted all options, I feel like, why is it opposite? I mean, what if he is a VIP patient and they took him to a prestigious different hospital, what options would they give him, that’s what I want to know.
Patrik: Absolutely. So if they tried proning and proning didn’t work, the next step is ECMO.
Kenneth: So after the new doctor came and he said that eventually he would go into kidney failure and have other failures, and I suspect that that would happen.
Patrik: That risk is there, there is no guarantee that if your brother wants to go on ECMO, there’s no guarantee he would survive, but the chances to buy time and let him rest and recover are there, right? There is the risk that if he’s going on ECMO, that his kidneys fail, anyway, I mean, he’s critically ill after all. So there’s no guarantee that A. ECMO will save his life, and B. he won’t suffer from any other complications, such as potentially kidney failure, a lot of patients on ECMO are on dialysis as well, temporarily. So at the end of the day in a situation like that, we are opening a can of worms, I’m here to help you, but I wouldn’t say that…
Patrik: Just give me a second.
Patrik: I’m here to help you, but I wouldn’t say that things will necessarily get easier, I’m here to present you with options and guide you, but at the end of the day, there’s no guarantee that if your brother wants to go to another hospital, or was to go on ECMO in another hospital, that there are not any other complications arising. But again, going on ECMO would be a very different discussion to have, compared to end of life care, very different discussion.
Suggested links:
Kenneth: What is your services like?
Kenneth: So for me, I wanted to see how it works for paying for… Even to talk to my dad, if we pay hourly or how do you do it? The language and the direct, so that we know that we exhausted, I want a consultant that understands… I’m just trying to find somebody that’s…
Patrik: Absolutely, and that’s where I can help you with, I mean, I worked in ICU for 20 years. I am not a doctor, I am a critical care nurse, but I worked in ICU for 20 years. I’m talking to people every day, all over the world in similar situations, and I’m talking to doctors all the time in similar situations with… Obviously I’m talking to doctors with families, I’m not talking to doctors by myself. The next step would be for you, and for me, or for your dad, whoever you want on the call to talk to the doctors there, and find out what is exactly happening, what have they done, what have they not done, what have they told you, what have they not told you? Because I argue that they haven’t even told you half of the story, I haven’t even told you half of the story.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Kenneth: I know his kidneys, I know that that he’s not… Does he still have a little hope when it comes to medication?
Patrik: I wouldn’t know until I’ve spoken to the doctors, because you’re giving me very good information…
Kenneth: I mean, I hope about making it, in terms of him not going totally in coma state with him being in the ventilator. Is it normal for someone to be on the vent for a week?
Patrik: People can be on ventilators for months.
Patrik: That’s what I’m saying, as much as I’ve tried to simplify things for you, it is a very, very complex arena, very, very complex arena. And that’s what I’m saying, you’re probably giving me 10% of the information that is needed in order to guide you with this, and that’s why it’s so important that we were to talk to a doctor and find out, let’s ask a series of questions, what is exactly happening? And let’s ask the other 90% of the questions to get to the bottom of things.
Suggested links:
Kenneth: So assuming that my brother doesn’t drift off in the night or whatnot, can you give me pricing and your availability to maybe set up with the doctor and that you could be present to help me and the family, my siblings, that type of thing.
Patrik: Absolutely. Absolutely. So I have several options, and I can email all of that to you, but I can quickly talk you through it.
Patrik: I have several options, starting where you can work with me over a whole month, you can work with me for a couple of weeks, you can work with me for a week, for a few days, you can work with me for an hour, so there’s several options, different price points, starting $3,000 for a month, going down to sort of $1,700 or $1,800 if you want it over a couple of weeks, all the way down to $199 for an hour. If you started with an hour, and you then wants to continue for a few days or for a week, I will credit the $199 towards any of the other options. I also have an online membership option where you have access to me online, so it comes… I have various options for what works for people.
Kenneth: What’s the fastest that you… Where is your location?
Patrik: I am in Melbourne Australia, but I’m talking 80% of the work that we’re doing is from other countries like US, Canada & UK.
Kenneth: Okay.
Patrik: But don’t worry about that, I will make myself available when you need me.
Kenneth: So when is the fastest that we could do a call or when is your most available time, so I’ll talk to my dad tonight and my step-mom, and let them know that, can we get a meeting with… And hopefully it won’t upset the doctors.
Patrik: No, no. There’s ways to deal with that, so if you are worried about upsetting the doctors if we talked to them, there’s a couple of ways, you don’t necessarily need to be in their face and say, “Hey, I’ve hired a consultant/advocate.” It might get them defensive, it might not, depends on the hospital. The best way to introduce me is to saying, “Hey, I’ve got a cousin, or a family friend that’s a critical care nurse that’s helping me to understand.” That’s all you need to say, that takes the barriers down.
Kenneth: Yeah.
Patrik: That’s my experience.
Suggested links:
Kenneth: Yeah. Because the last doctor did say that, “Okay, we can have more meetings like this to help you guys figure it out.” So I’ll ask my dad to call it a meeting, and then I’ll just say that… So I think you can ask those questions to help us translate it, and then… So how would it work, so we paid for the week, is it an hour each day out the week?
Patrik: No, there’s pretty much no time limit on that, if you work with me for a week, I say, you can reach me unlimited, that sounds great of course, you can… I’m all about getting outcomes for you, I’m all about getting outcomes, I don’t think that outcomes necessarily matter whether you spend an hour with me or three hours, it’s a case of understanding the complexity of the situation, and then taking guidance from there. So what I’ll do is, I will email you the options, and so if you work with me for a week, it’s pretty much you can call me anytime, and there will be times where I can’t pick up the phone, but then I’ll get back to you as quickly as possible of course.
Kenneth: Okay. And what’s the week price?
Recommended:
Patrik: I think the week price is $999, I think the four day price is $799, the 14 day price is $1,799, and the month price is I think, $3,000, and the hour price is $199. I’ll email it all to you. And if you will start with the hour and you wanted to then proceed with the seven days, I will credit those $199 towards the week option.
Kenneth: Yeah. I’m thinking more probably at minimum, the week or four days, but I’ll talk to him, and then you take regular square, or what methods of… Regular PayPal or just regular Visa?
Patrik: PayPal, or credit card, you will see that when I send you this email, you will see some links that I put in the email, you just click on the links and then you’ll get the choice between PayPal or credit card.
Kenneth: My other question is, are you kind of familiar with the medications and all that, that they typically…
Patrik: Very much so, very much so.
Patrik: I mean, it’s almost to me, if they haven’t told you about ECMO and they’re talking about comfort care, I would argue A, they’re either misleading you or B, or not putting all the options on the table.
Kenneth: I felt like, when I went to my dad when I had that, then I was like, it has to be… I just don’t want to… Because I know one of the things, that the steroids they’re giving him, it’s not working out, and I remember his friend saying, “Well, is there different steroids that could help, and wouldn’t upset.” I don’t know the…
Patrik: The challenge with COVID is that, nobody’s found a cure, right? What does help with COVID is obviously treating the symptoms, and treating the symptoms often means resting the lungs, and resting the lungs often means ECMO, so the ECMO can take over the function of the lungs and the lungs can heal. Now, there are cases where COVID is being treated successfully without ECMO, but I do believe from all the statistics that I’m reading, the mortality rate for COVID in ICU, sounds to me it’s almost by 50%, which is very high.
Kenneth: I read higher than that actually.
Patrik: Might be higher even.
Kenneth: Yeah, but the ECMO is a little bit different from the ventilator, because it’s not as intrusive on the body?
Recommended:
Patrik: Oh, it is intrusive, but it’s… They have to put in some cannulas to basically take more blood out, put the blood through an oxygenator, right? And re-infuse it back into the body, but that gives the lungs a rest because the oxygen that the body needs is coming externally.
Kenneth: From the vent?
Patrik: No, not from the vent, from a bypass machine.
Kenneth: So the ECMO is more like a bypass machine?
Patrik: ECMO is a bypass machine.
Kenneth: Would it have enough pressure for him though, if they’re operating the vent at that level, would it be enough?
Patrik: Yeah. Because the lungs are not needed for oxygenation, the lungs are completely out of the picture, it’s all going through the blood, much easier, but also comes…
Kenneth: Would you have to be stable enough to kind of transition that procedure?
RECOMMENDED:
Patrik: He probably would have to be stable enough, but that’s also why timing is critical, I do believe if he’s that sick, they need to move rather swiftly, very swiftly.
Kenneth: I know I got to let you go, we are over 15 and I know that… I’ll see you again, I’ll review the package and then I’ll try to call my dad right away to see if we can get a meeting with the doctor.
Patrik: I think so.
Patrik: What I’ll do Kenneth is, I will email you the options that we just spoke about, I’ll send you that email in the next 10 minutes, and we’ll go from there.
Kenneth: Okay, thank you so much.
Patrik: Pleasure. And try and get some sleep, look after yourself, self-care is very important.
Kenneth: Yeah, it is. Yeah. Thank you so much, Patrik. I will talk to them tonight and get moving.
Patrik: I’ll send you this email in the next 10 minutes, thank you so much.
Kenneth: Thank you.
Patrik: Thank you Kenneth.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!