Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
The ICU Team Is Negative And Not Transparent With My Mom’s Prognosis. How Do I Deal With It? Help!
You can check out last week’s question by clicking on the link here.
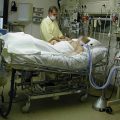
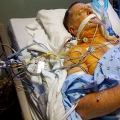
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Cathy as part of my 1:1 consulting and advocacy service! Cathy’s mom is in ICU ventilated and in an induced coma. Cathy is asking if tracheostomy is more comfortable than the breathing tube for her mom.
My Mom is in ICU Ventilated and in an Induced Coma. Is it True that Tracheostomy Is More Comfortable than the Breathing Tube for Her?
Cathy: And so, the only thing that she said was, “Has your family considered that if you take them off the ventilator, that you wait to see if God has them breathe.” And I’m like, “Yes, we’ve considered it and we’ve considered that God has blessed someone to create a ventilator to maintain life and if that breath is still coming in and maintaining the organs, we consider taking them off the ventilator to be killing them. And again, the plan here is not to sit up here with you-all all the time. It is how can we get her to a place where she is back at home, and we’ll go from there.”
Cathy: And she’s like, “Okay, well” She’s like, “I agree with you on the God part of it and all of that. It’ll just be very hard.” And I’m like, that’s life and life is hard. It’s not going to be easy, but we’re going to follow what we think is God’s will on this. So, if her organs are still working, I’m not even, especially I did a little research. I didn’t have a lot of time, but I did a little research on this whole brain-dead concept. It’s like kind of made up.
Patrik: Of course.
RECOMMENDED:
Cathy: There’s no basis in science and I didn’t realize that. I didn’t know that at all. And I was like, you just can’t say what a person’s, you just don’t determine that someone has like their life has meaning based on your qualifications. To me, it is a sign that since her organs are still working that I continue along this path of life. It does not mean that there might not be a complication and God takes her home. I understand that, but my actions now are not going to be, ‘Oh, there’s no hope. Turn everything off.’ I’m just not going to do that.”
Cathy: So, she didn’t pop in there today because I know that she was sent to push me along, but they just can’t argue with the fact that I’m like, you all said all was lost and I come in here, and look at. Because I make them give me her vitals and go through all her blood work every day, and I’m like, again, all her stuff is still working with a few hiccups but I’m just not going to be interested in listening to what you have to say if you can’t explain. There just is no excuse that you just give up on a person when all the rest of the stuff is working.
Cathy: And brain-dead, I think told her, I was like, brain-dead is not dead to me. I don’t even know how you come up with that concept at all. It’s about the breath to me. So, I haven’t heard from her since.
Patrik: And not that I want to digress, but I do know more and more people challenge the brain-dead concept in front of courts, and families are in that situation exactly on that concept. I mean, who are you to determine whether my loved one is dead or not if we can keep them alive.
Cathy: Exactly.
Patrik: So, more and more families are heading that way. And I believe the argument about religion, spirituality, whatever people’s beliefs are, is having more and more weight in the discussion. It has to.
Cathy: Right. Absolutely.
Patrik: And also coming back to palliative care, some families, and we’ve done that as well, Cathy, some families want to have an end of life situation at home. They might be able to accept, “Hey, if I take the ventilator off, my mom, my dad, whatever, is probably going to pass away.” They’re happy to accept that, but they just don’t want to be in ICU. We have taken some people home for three days. And after three days, life support was stopped and they were passing away at home, but that’s what the family wanted.
Cathy: Right. That’s right.
Patrik: These people that have worked in hospitals for too long are so desensitized. They’re just thinking in this one size fits all.
Cathy: And they should all be smarter than that with all of the schooling that they’ve done, but they just don’t have the capacity to do that. I’m just like, “How could you even think that you have a right to determine what someone’s life should look like? You just should focus on whether or not you can keep them alive because the more we go through all of this, the more that we see that you all are wrong about a lot of things. So, just focus on the details and the basics, and don’t come in there with this preconceived notion about what someone should do, which is what they have done to me and my mother this entire time.
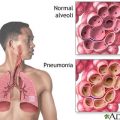
Cathy: So, it’s like there’s no sense of urgency when she came in, which brings me to getting them to tell me what happened. They’re like, “There’s a blood clot in the lung that caused the lung to stop, which caused the heart to stop. And then, well, we can’t be sure that’s what it is, but we know she has a huge clot on her lung.”
Patrik: So, that’s a PE. Have you heard of a PE?
Cathy: No.
Patrik: Basically, what they’re describing is a pulmonary embolism.
Cathy: Okay, got it. Okay, so they did mention that.
Patrik: Right, okay. So, they were able to determine that as a cause of the cardiac arrest?
Cathy: Right. I guess so.
Patrik: Right, and they were able to determine that from the CT scan, I would imagine.
Cathy: Yes. Exactly, yep.
Patrik: That’s why they’ve given the Heparin, okay.
Cathy: Okay, yep. That’s it. So, on the brain scan when it says no reactivity to pain, does that mean that they tried to do something that should cause her pain, that should light up a certain part of her brain?
RECOMMENDED:
Patrik: Yes. And also, when you go back, do you remember when I sent you the Glasgow Coma Scale?
Cathy: Yes.
Patrik: Remember, there is a part, and you might have even seen it yourself. Have you seen when they check for the Glasgow Coma Scale? Have you seen that?
Cathy: I saw half of it once before the neurologist stopped coming.
Patrik: Right. So, if you’re mom doesn’t respond, they should actually try to squeeze her shoulder, try to squeeze her hands really hard to find out does she respond to pain.
Cathy: The only thing that, look, one day, the intensivist said that the neurologist came in. He said he didn’t see anything. Then he was saying that he might have seen a little something. Again, it’s just not…
Patrik: Happen.
Cathy: What I think it should be, which would be consistent and then you are tracking what’s going on. Like I track all of her vitals. They’ve just made the decision from the beginning that her life was not worth anything.
Patrik: Sure, sure. Have you heard them talk about Glasgow Coma Scale?
Cathy: No.
Patrik: Okay. When you go there next, ask them what her Glasgow Coma Scale is. I mean, you determined it’s a 3, but get it from them.
Cathy: Okay.
Patrik: Maybe the see something that you may not have seen. They should be checking that Glasgow Coma Scale at least three times a day. The nurse should be doing that.
Cathy: Okay. I think the nurses do it when they come in because they turn her every two hours. It’s not like anyone’s telling me, “Okay, so we did the Glasgow Coma, and this is what we think.”
Patrik: No, they probably wouldn’t, but I think it’s a very relevant question. Also, have you been present when they turned your mother?
Cathy: Not really.
Patrik: Okay.
Cathy: The times that I’ve been there, they told me to step out of the room and then other times, it’s not there, yeah.
Patrik: I would be very curious to know if your mother is opening eyes when they’re turning her. I think, again, that would be a very good question to ask. If she was to open eyes when they turn her, that would up the Glasgow Coma Scale straightaway.
Cathy: Okay, got it.
Patrik: Because she may not open eyes when she’s lying there and she might not even open eyes if people squeeze her hands or maybe squeeze her shoulders or whatever pain stimuli they might try, but she may open eyes when they actually turn her, give her back a wash, change sheets.
Cathy: Okay. I will ask them that tomorrow. So, as far as the tracheostomy and the PEG, do I tell them, “Okay, you can do the tracheostomy but we’re not going to do the PEG right now?” Because, for me, it’s like I can look at the vitals and determine for myself what’s going on. Like her white blood cell count and she’s had the fever that’s high. I’m like, “Well, does she have an infection?” I can do that kind of thing. I just don’t know how to determine because, again, I am not dealing with people who are going through this analytical process that I think you should go through to say, “Okay, she’s strong enough to have the tracheostomy.”
Cathy: The other thing with my mom is she has a huge tumor on her thyroid, and I don’t know if the tracheostomy would affect that. That was one of my questions that I was going to have for him tomorrow.
Patrik: Right. Is it a benign tumor or a malignant tumor?
Cathy: It’s a benign tumor.
Patrik: Benign tumor, okay and she’s been having that for a long time?
Cathy: Twenty years. First time it was diagnosed was 20 years ago.
Patrik: Right. And nothing has been done about it, it’s just sitting there?
Cathy: Yeah. No, she won’t have surgery. She would never consent to have surgery.
Patrik: Right. That could be an issue, but you’d think they would have thought about that already.
Cathy: You would think, but I’m the person, again, they’re trying to get me to sign these forms before the surgeon has even said anything to me. When went in tonight to visit my mom, the nurse was like, “Oh, Dr. Sequio is going to call you tomorrow.” I’m like, “Well, Dr. Sequio should have talked to me earlier because I’m not signing any papers yet.” Well, he’s talking to me because he thinks he’s going to do surgery tomorrow. We haven’t talked about anything.
Patrik: How big is the tumor?
Cathy: I don’t know. It was enough. It was growing to the point that it affected her ability to talk and she would get frustrated and she just stopped talking. It is hereditary. It runs in the family. My great-grandmother died from a goiter. All of her siblings have had to have some type of surgery dealing with that. But just for her, it didn’t really start bothering her until probably in the last year. But she was first diagnosed in the year 2000 with it, but it was benign. It’s benign.
Patrik: Right. Is it visible?
Cathy: Yeah, but not like goiter visible. You have to look. It looks kind of swollen unlike, I guess, if you looked at it enough. The doctor had to say before, “Okay, what am I looking for?” Probably in the last year, it’s gotten pronounced and you can see it.
Patrik: Okay. Look, I guess, you’ve got to wait and see. It’s hard for me say whether they can or they can’t, but now, that we’ve established that then that almost would push her towards a surgical tracheostomy and not a percutaneous tracheostomy. So, remember earlier I said, percutaneous tracheostomies can be done in ICU quick procedure. I would argue that with the thyroid tumor, she’s higher risk and it probably warrants for her to go to the operating room. That, I would say, is a given.
RECOMMENDED:
Patrik: Coming back to the PEG, I tell you, I’ll give you some examples, so you can, hopefully, make an informed decision there. So, sometimes, people come into ICU and they don’t have brain damage, or they don’t have a cardiac arrest with potentially a hypoxic episode and the brain is damaged, but they come into ICU after car accident. They come into ICU with a pneumonia, with lung failure. They are in an induced coma for many days and then you wake them up, and then they might be a Glasgow Coma Scale of 3 for 10 days. And if you do a CT scan and the CT scan says, “Well, there’s nothing wrong with the brain. People are just not waking up.”
Patrik: Why are they not waking up? Well, they’ve been critically ill. They need time to rest and heal. That’s a reality of critical illness. So, I have seen all of that. Now, in your mom’s situation, there’s a high chance she has sustained some brain damage, but nevertheless, she might still take her time to wake up because she’s been, and she is critically ill.
Patrik: This is what people don’t tell you. Waking up, and I understand your mother didn’t have an induced coma. She wasn’t in an induced coma, I understand that. The examples that I’m referring to are people being in an induced coma, but nevertheless, they still take their time to wake up even though they should wake up once the sedation has been switched off. Waking up after a critical illness is like switching on a light with a dimmer. It’s not like switching on a light and the light is on.
Cathy: Got it, okay.
Patrik: Right? And it’s the same with people after brain injuries. They may or may not wake up. And if they do wake up, nobody knows what it’s going to look like, how long does it take for them to wake up, how gradual is improvement, if any?
Cathy: Right, okay.
Patrik: And that’s where I’m saying like, especially take those examples briefly that I mentioned where people don’t have a brain injury, but they’re still not waking up.
Cathy: Not waking up, right.
Patrik: The ICU would be rushing towards a tracheostomy and a PEG. Where I go especially with people that don’t have brain damage, I would recommendation for families to stay away from a PEG because it makes people complacent.
Cathy: Right, okay. And still just feed her, well, they’d have to switch it and it would go down her nose?
Patrik: Yes, a nasogastric tube.
Cathy: Nasal gastric.
Patrik: It’s a nasogastric tube, right. Again, in your mom’s situation, with everything that you’ve shared, I do believe there is a pretty high chance that there is some brain damage, but again, after 11 days, nobody knows what your mom’s brain function looks like in another 11 days.
Cathy: Right, okay. I mean, is it possible to get her, if they’re so freaked out about her being in ICU, does she get stabilized enough to go up to just like one of the regular rooms?
Patrik: Probably not because they wouldn’t be able to look after her on a ventilator on the regular room.
Cathy: Got it.
Patrik: Do you know whether they’ve got a step-down unit in ICU, like another unit within the ICU? Do they have that?
Cathy: She’s in CCU. So then, there’s an ICU.
Patrik: Okay, so CCU. But CCU stands for Critical Care Unit or for Cardiac Critical Care?
Cathy: I think it’s Critical Care.
Patrik: Critical Care, okay. Critical Care and ICU are interchangeable terms. And this is where a PEG just like a tracheostomy, they all have their time and their place. From my experience, I am opposed to both at the same time for the reasons that I mentioned, but I also understand minimizing the risk. Having two surgeries at two different times is a higher risk than having two surgeries at one time.
Cathy: Right. Again, even with the ventilator, we’re not at the 14-day point. Just explain to me the reason that you want them off of the ventilator where the tube is down their throat is because there might be problems. It’s uncomfortable and there might be problems with the extubation if you leave it in too long?
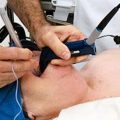
Patrik: Yep. So, most of the time, 9 times out of 10, the reason you want to move to a tracheostomy after about two weeks of ventilation with a breathing tube is because people are in an induced coma to maintain ventilation in the breathing tube because it’s so uncomfortable. So, when you have someone in an induced coma with medication, there are lots and lots of undesirable side effects. So, by doing a tracheostomy, you can pretty much stop the sedation straightaway because the tracheostomy, unlike a breathing tube, is fairly comfortable.
Cathy: Okay, got it.
Patrik: That’s one of the reasons. The other reason is have you seen your mother coughing? Has she got a cough?
Cathy: No. I haven’t seen her cough.
Patrik: Okay. So, a lot of people with a breathing tube, they cough, and the risk is that they cough out the breathing tube, whereas the tracheostomy is much safer.
Cathy: Got it.
Patrik: So, those are the main reasons why you wanted to move to a tracheostomy, but there’s other reasons as well. In your mom’s case, I would argue once somebody has a tracheostomy, I’m almost bound to say they have more time to come off the ventilator, in a time that works for the patient. And also, things like mobilization is so much easier. It’s a much more stable airway compared to a breathing tube.
Cathy: Got it, got it.
Patrik: Much safer.
RECOMMENDED:
Cathy: Okay, so if I, my initial response was, “Is this too much at once?”
Patrik: Yes.
RECOMMENDED:
Cathy: Say yes to the tracheostomy and just tell them to move the feeding tube for now.
Patrik: Yes.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!