Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
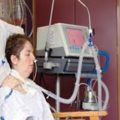
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy service! Marsha’s sister is with a tracheostomy and is on a ventilator in the ICU. Marsha is asking why it is important that she can access her sister’s medical records in ICU.
Why is it Important that I Can Access My Sister’s Medical Records in ICU?
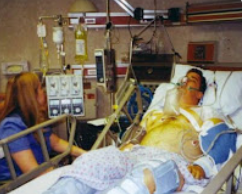
“You can also check out previous 1:1 consulting and advocacy sessions with me and Marsha here.”
Marsha: He said, “Well, she’s in pain. There’s nothing we can do. This is what they do.”
Marsha: I said, “Could you make a note that I’m requesting that? Can you call the doctor and call me back?”
Marsha: They don’t call me back, doctors don’t call me back.
RECOMMENDED:
Patrik: No.
Marsha: That’s why I feel like sending the social worker on that, saying, “Hey, I’ve been telling the doctor and the nurses they got to back up on her medication. Could you please handle?”
Marsha: But nothing happens. I don’t know how.
Patrik: Right.
Marsha: I have no idea. When I used to be there most of the day, I was always with her. We almost had it arranged where someone was with her all the time.
Patrik: Yeah, that’s not a bad thing.
Marsha: Yeah.
Patrik: If you can pull that off, that would be great.
Marsha: Yeah, but not now.
Patrik: Yeah.
Marsha: Now, I can’t do it because of COVID, they won’t let them in. They only let you in for an hour.
Patrik: Yeah, that’s bad.
Marsha: That is bad. It’s crazy. Patrik, it’s crazy.
Patrik: It’s crazy.
Marsha: It’s illegal. How do you do that?
Patrik: It’s crazy. Hospitals were difficult before COVID and now it’s gone completely.
Marsha: And they love it that way. No one’s around to bother them.
Patrik: Yeah. No, and that is why I think it’s even more important that you get access to the medical records.
Marsha: Right.
Patrik: Even more important.
Recommended:
Marsha: Okay, here’s my issue if the doctors don’t call me back, what do I do?
Patrik: Yeah, good question. I think you should escalate that to hospital executive. You could send an email to a hospital executive, like the general manager or CEO, or whoever is running the place.
Marsha: Right.
Patrik: That’s what I think you should be doing.
Marsha: Now, if I go in there tomorrow and ask the nurse, “Did you write down a list of medications?”
Marsha: He probably won’t do it.
Patrik: He might do it. He might do it straight away for you.
Marsha: Wow. It bothers me now, but I don’t know what to do.
Patrik: Look, Marsha.
Marsha: I’m going to text you again tomorrow.
Patrik: Look, I totally get how stressful this is and I agree with you, Dilaudid and the Roxycontin, that’s highly, highly addictive stuff. Highly addictive.
Marsha: Right.
Patrik: Highly addictive stuff and she needs to get off it. But by you getting access to the medical records, you’re telling them, “Hey, I’m not putting up with it.”
Patrik: And it won’t be an overnight process, but by you asking for the medical records, you get the process started.
Marsha: All right. So, I should just ask for a copy of the medical records?
Patrik: Absolutely. I’ll send you a link in a minute about your right to have access to medical records.
Suggested links:
Marsha: Yeah, but my thing was, if I could just simply ask without going through all that, and get a list of the medications, is that sufficient? Or do you want me to do the whole…
Patrik: No, look, if you get access to the medical records, it might take a few days, whereas if you ask just for a list of medications, you might have that quickly.
Marsha: Right. Would that be sufficient for you? You want to see the medications, that’s it?
Patrik: Look, it would be a starting point.
Marsha: Okay.
Patrik: It would be a starting point.
Marsha: Yeah, and they just got her on a pain blocker, starting with an L. That’s the only couple things I noted.
Patrik: Right. Does your sister recognize you?
Marsha: Yeah.
Patrik: Good.
Suggested links:
Marsha: Her eyes, her pupils are dilated, or constricted rather. It’s almost like a mother-daughter relationship because I scold her now.
Marsha: She’ll just be like, “Oh, I know I shouldn’t have done that. I got to stop the pain medication.”
Marsha: The funny thing is, if they get her on the other side of her pain medication, she won’t ask for it.
Patrik: Yeah, I agree.
Marsha: It’s just the pain, she won’t ask for it.
Patrik: I agree.
Marsha: Why? Because they don’t listen. Because I’ve seen this. Patrik, I don’t think I’d ever go to a hospital if I thought I really, really need to. It’s crazy.
Patrik: It’s crazy, I agree.
Marsha: It’s like they do what they want.
Patrik: They do what they want, I agree with you. I agree with you.
Marsha: It’s frustrating too. They look at you like, oh, I don’t know.
Patrik: They look at you like you don’t know what you’re talking about. I agree with you.
Marsha: Right. I warned them, the specific thing I told them, “She will stop jumping out of the bed.”
Marsha: And they look at me like I don’t know, “Okay yeah, whatever.”
Marsha: I’m like, “All right.”
Marsha: Tonight, I got there, they all looked and, I said, “I told you just a few days ago, I told you she’s going to jump out of the bed and start seeing little green men. She starts seeing people. She thinks she’s in places, she’s not. And then, she wants to go home and starts getting out of the bed. She doesn’t want to be in the bed anymore, she gets in the car.”
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Right. Look.
Marsha: And the funny thing is, she told me she can’t stop it.
Marsha: She goes, “Well, she’s in here.”
Marsha: I said, “Cut the dope.”
Marsha: I told her in the ER, I said, “When I’m with her and she has the pain medication, I walk out, I walk back in the room, I find her sitting in a hot mess, and she forgets half the time.”
Patrik: Right.
Marsha: So I do it again, but I try to suss it out. But they think, they’re making her nice by giving it to her. Yeah, in the short term, but when she’s jumping out of the bed, it’s on me.
Patrik: Yeah, I hear you.
Marsha: My one concern is, this is my one thing, what are they going to do if she has to get back on the ventilator? Patrik, just tell me, what will they do now?
Patrik: Can you repeat that, please? What will they do, if?
Marsha: This is my biggest thing, this is why I really called; what are they going to do if she needs to get back on the ventilator now?
Patrik: I’ll tell you what they would do, they would put the tracheostomy back in.
Marsha: Oh, I hope you’re right. I hope you’re right.
Patrik: The challenge there is, Marsha, that in the next 48 hours, they can probably easily put the tracheostomy back in. After 48 hours, if she needs it. The tracheostomy hole might be closed and that’s when they may need to intubate her.
Marsha: If they intubate her, Patrik, I don’t think she survives that.
Patrik: What makes you think that?
Marsha: If they intubate her, they’ve got to heavily sedate her, Patrik. I just don’t think she can handle it.
Patrik: Right.
Marsha: Her heart is weakened; her lungs are weakened. When they intubated her, she was 180 pounds of muscle.
Patrik: Yeah.
Recommended:
Marsha: Coming off 170, the other day. You never saw a 54-year-old lady, I’m sorry, she didn’t even have 1% of a 54-year old lady that you ever saw in shape. That is crazy. And now, she’s 115 pounds. She went from 180, you can imagine, like stomach tubes, well-built, strong. No. That’s it, I don’t think she’d survive. I don’t think she’d survive it.
Patrik: Right. Has she been digesting her food?
Marsha: What was that?
Patrik: Has she been digesting her nutrition?
Marsha: Yeah. She gets fluids, so as far as I know. She looks a little good with that, they upped the weight, I noticed that.
Patrik: Right.
Marsha: They want her to gain weight. But she’s never going to gain all that weight back.
Patrik: Right. Look, I totally understand that this is a tricky situation, I totally get it. But again, I see some positives in there. The positive is she’s got the tracheostomy removed. It could be prematurely, it could be, but it could be a blessing in disguise.
Marsha: Yeah. I hope you’re right. So right now, they can’t discharge her, until what?
Patrik: Well, if she stays, if she can maintain the airway without the tracheostomy, she might be going to a hospital floor very soon. She might.
Marsha: Like a regular floor?
Patrik: Yeah.
Marsha: Okay. She’s not outside, she’s going to probably have to share a room, but that’s all right.
Patrik: Say that again.
Marsha: She’s probably going to have to share a room, but that’s all right.
Patrik: Right. I think the next 48 hours will be critical.
Marsha: Okay. So today is Friday, so Sunday night, Monday morning, if she’s still going, do you feel like, okay?
Patrik: If she’s still going and they can remove the Dilaudid and the Roxycontin, this might not be a bad thing, but we wouldn’t know at the moment.
Marsha: Right, understood. I don’t think they’re going to remove it. I don’t think they’ll listen to me, they’re going uphill.
Recommended:
Patrik: Right. But by you asking for the medical records, they also know you’re questioning things.
Marsha: Right.
Patrik: Keep questioning. Keep questioning.
Marsha: It’s only because I’m going to send a note to the social worker, so at least I’ve notified someone. I’m going to copy the case manager.
Marsha: I’m going to say, “I mentioned this several times about Chloe, that she’s getting too much of these heavy drugs. I told the nurse and the doctor that she needs to be weaned off them. I need her weaned off the drugs. I need a list of the drugs that she’s taking, or she’s going to get compulsions and jump out of the bed.”
Patrik: Yeah.
Marsha: They don’t listen to that, then I don’t know.
Patrik: Yeah. There is definitely a risk that she will need the tracheostomy back in. There’s definitely that risk there, but I also wouldn’t be surprised if they stopped the feeds for the next 24 to 48 hours, and I’ll tell you why. You don’t want her to aspirate.
Marsha: Right. Oh, my goodness, something else I’ve got to worry about.
Patrik: Yeah, look, it is a tricky situation. It is a tricky situation. No question. There are risks and there are opportunities in this.
Marsha: Yeah, no, I understand that. I just hope the latter is better.
Patrik: Absolutely.
Marsha: I hope the latter is better.
Patrik: The latter would be great. The latter would be great. Marsha, what I’ve done is I have texted you a link to a document where you can see that you have the right to access medical records.
Marsha: Yeah, they probably won’t give me a hard time anyway, so I’m not too worried about it. Should I tell them not to feed, to stop the feeding?
Recommendation:
Marsha: Should I say, “Maybe, you should stop the feeding, so she doesn’t choke?”
Patrik: Yes, I think you may. Again, it shows them you are doing your own research. I would tell them that, absolutely.
Marsha: Okay. I can send that to the social worker too?
Patrik: Oh, no. The social worker wouldn’t have a clue. Wouldn’t have a clue.
Marsha: Then how do I do it? How do I get it back to him? How do I do it, is the question itself?
Patrik: So, when you’re there, you talk to a nurse.
Marsha: Yeah, they’re very good, they’re nice to me. They’re all good.
Patrik: Well, tell the nurse. Tell the nurse.
Marsha: Okay, I’m going to call the one that has the night too.
Patrik: Yeah. Look, I know how frustrating this is, but keep telling them what you want, even though it hasn’t happened yet. Repetition, I believe, helps. Repetition is the mother of all skill, keep doing, keep saying what you’re saying even though it hasn’t happened yet. Don’t give up.
Marsha: No, I won’t give up. Trust me. I complain, but my spouse will tell you, I won’t give up.
Patrik: Yeah.
Marsha: That’s my problem in life. Sometimes, I don’t quit when I’m ahead, that’s the problem. Not in this situation, but trust me, I won’t give up.
Patrik: Good.
Marsha: Tonight, I’ll be bummed out, but tomorrow when I wake up, I’ll be ready to go again.
Patrik: Good. Don’t give up. Keep repeating what you want.
Marsha: I’ll do that. You’re a good man, Patrik. You there?
RECOMMENDED:
Patrik: Yeah, I’m here. No, keep at it. Hopefully, this is what she needed. Hopefully.
Marsha: I know, I know. Hopefully, you’re right. She came out a couple of places the right way, I mean.
Patrik: Yeah, there are risks in this, but we will know in the next 24 to 48 hours.
Marsha: All right. Thank you, Patrik.
Patrik: It’s a pleasure. Please let me know.
Marsha: Okay.
Patrik: Please let me know how I can help, going forward?
Marsha: Thank you, I will. Thank you.
Patrik: Okay, thank you, Marsha.
Marsha: I’ll speak to you soon.
Patrik: Thank you so much, bye. Bye.
Marsha: Thank you.
Patrik: Thank you.
Marsha: Bye-bye.
Patrik: Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!