Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
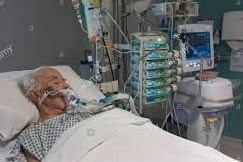
This is another episode of “YOUR QUESTIONS ANSWERED”. And in today’s episode, I want to answer a question from one of our readers, Ken and Ken has his 75 year old dad in ICU after pneumonia and urinary tract infection.
So Ken is asking, “My 75 year old dad is in ICU with pneumonia and urinary tract infection and now he’s on dialysis. He’s been weaned off sedation but he’s not waking up after induced coma. How long does it take?”
My Dad is in ICU and has been Weaned Off Sedation. How Long Does it Take for Him to Wake Up After an Induced Coma?
So Ken writes,
Hi Patrik,
I was trying to research how long it would take for my dad to come out of a medically induced coma and I came across your website. I really appreciate the fact that you’re providing valuable information for families in intensive care. Worried, sick over loved ones in ICU. So thank you very much. That’s why I thought I’ll become one of your clients because it’s such a valuable website and service that you offer.
RECOMMENDED:
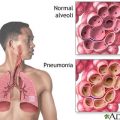
So Ken writes, my father is a 75-year-old male professional who contracted sepsis, a urinary tract infection and pneumonia. We don’t know which came first but all three were present. When my father presented to the hospital and the ICU. The doctors first asked my father for permission to sedate him and put him on a ventilator because of pneumonia. He had difficulties breathing. His chest x-ray was really poorly and we and my father thought that it might be the best option to get him intubated and sedated for a few days.
So my father and my family agreed to authorize the ventilation and intubation for further treatment while he was also becoming more and more unconscious. So we had to take over anyway. It was under sedation for six or seven days during which time they put him on dialysis as well to help the kidneys recover from a kidney infection.
RECOMMENDED:
It was taken off dialysis two or three days later and his and his kidneys were deemed stable enough to remain off dialysis. That seemed like victory number one. Shortly after that, he seemed to be clear of the urinary tract infection and his lungs clear enough that doctors felt he could come off sedation and wean him off the ventilator.
They began reducing the number of sedatives (96) about four or five days ago and he was supposedly entirely free from all sedatives three days ago however, he still hasn’t woken up. From your videos, I take it that he was considered medium-term sedation and both his age and the fact he had kidney involvement may add to the time it takes to wake him up.
RECOMMENDED:
The neurologist reports that his brain activity is normal and doesn’t show any signs of dysfunction, although he doesn’t seem to be waking up still. Our family is massaging his feet and his respiration stopped from 30 to 21 and then to 19 during the massage we assume the foot massage was comforting him although he remained unconscious.
Our question’s probably not unlike most families of ICU patients is how long before he begins the waking up process. We’re trying to be patient, but how long is too long? What’s normal under these circumstances? I suspect you won’t be able to answer any of those questions with certainty, but you’ve undoubtedly seen more than any of the people asking the questions. Thank you very much for all you’re doing to ease the minds of families in intensive care in crisis.
RECOMMENDED:
From Ken.
Well thank you Ken for writing in and thank you Ken for being a client. I really appreciate it. So can the situation that you’re describing with your 75-year-old, that is a situation I’ve seen hundreds of times in ICU. So as a rule of thumb, the older patients are the more, the longer it takes for them to come out of the induced coma and wake up.
Now that’s not to say that the younger patient don’t take that time either. It really depends. But generally speaking, as a rule of thumb, my experience has shown that the older someone is, the longer it takes for them to come out of an induced coma. The added complexity in your dad’s situation is the kidney failure or, or kidney sort of impairment that certainly doesn’t help with waking up because it takes longer for the body to excrete the sedatives and the opiates because in your email you’re only referring to the sedatives.
Now when somebody is in an induced coma, they get sedatives such as propofol or midazolam, also known as Versed. And they also get morphine or fentanyl on top of that, which is basically an opiate and both propofol, midazolam or fentanyl and morphine basically sedate the patients so heavily that it takes time for them to wake up. And again, with the complication, with the added on the complication of kidney impairment, it takes even longer because it takes longer for the body to get rid of the sedatives and the opioids.
RECOMMENDED:
With the urinary tract infection that you shared, that could have also led to the kidney impairment, cause you don’t say in your email that the kidney impairment was part of the hospital admission. It sounds to me like it came later.
Also, if your dad has developed sepsis, sepsis often does lead to a kidney impairment just simply because the sepsis drops blood pressure significantly and if blood pressure drops significantly and your dad’s kidneys might not have been perfused enough and therefore kidney failure might have followed on from that. And there’s also a very good chance your dad with the sepsis and pneumonia would have been on inotropes or vasopressors for low blood pressure, which is considered life support.
So your father has been on multiple forms of life support, which are the mechanical ventilation and the inotropes or the vasopressors. So with that being said, you know, they would have treated the sepsis with antibiotics. They would have treated pneumonia with antibiotics if it was a bacterial infection. It might’ve been a viral infection, but you didn’t mention that.
So you know, and now you’re saying that your dad that’s infection seems to get better, which is a good sign, of course, you know, and they might have stopped the antibiotics or at least reduce them. So again, probably best if you ask, if you ask those questions to the intensive care team, again, the biggest challenge for families in intensive care is always that they don’t know what they don’t know and they don’t know what questions they need to ask.
RECOMMENDED:
So also with the dialysis, you know, there is a very good chance, again that sepsis with the combination of the dialysis would have dropped blood pressure even further because usually when blood gets extracted from the body through the dialysis, it brings blood pressure down again, making it way more likely that your father would have ended up on inotropes or vasopressors throughout the dialysis.
In the combination with the sepsis, again, it brings blood pressure down. So now you’re saying that the lungs are clear enough so that the doctors feel he could come off sedation. So that’s the first step. They began reducing the amount of sedative about four or five days ago. He was supposedly entirely free from all sedatives three days ago. So, Ken, it’s very important to find out what sedatives and opiates your father has been on.
So for example, propofol is a very common sedative in ICU and it’s short acting. What that means is, you know, get started. Somebody gets propofol, they can be put to sleep very quickly within minutes, and they can also wake up within minutes, right? The longer somebody has propofol, the less likely it is that they wake up quickly, but they could wake up quickly, even if they have propofol for a few days.
What’s often an adding factor for people not waking up is the opiates that I mentioned, such as propofol, such as morphine or fentanyl. Those are heavy opiates. Very powerful. So if somebody gets morphine or fentanyl in high doses it makes them sleepy as well. And again, with the added complexity of kidney failure, you know, the morphine and the fentanyl might make your dad or might’ve made your dad so sleepy that he’s not waking up quickly.
Also, if your dad hasn’t had propofol for the induced coma but he’s had midazolam or also known as versed this is a long-acting sedative, which means it takes much longer for the sedative to get out of the body system. So, therefore, you want to find out, number one, which sedatives your dad has been on. Also, sedative-like midazolam is a benzodiazepine and it is an addictive substance.
So therefore if your dad has been on high doses of midazolam as well as morphine and fentanyl because morphine and fentanyl are addictive substances too, there could be an element of withdrawal going on, which is why your dad needs to be weaned off those sedatives and opiates slowly. They shouldn’t just be switched off because again, your dad could go through some withdrawal there. So, therefore, your next step really is to find out what sedatives and opiates he’s been on and then get back to me.
On the other hand, your dad has just been through a severe critical illness with pneumonia, with a urinary tract infection with the sepsis and the dialysis, which means, you know, on paper your dad should wake up quickly, but the reality is he’s just had a significant critical illness. A critical event in his life is probably as close to that as he’s ever been. So don’t expect your dad to go back to normal quickly. It can take time.
His body might just say, you know, look, you’ve switched off sedatives, but I’m not ready to wake up. Right? He needs the time to recover. His body needs time to recover from pneumonia, from the ventilation, from the induced coma, from the kidney failure. So give your dad the time he needs. Recovery in intensive care is a process, not an event.
RECOMMENDED:
It’s not as simple as, you know, you’re switching off sedation, you’re switching off opiates and your dad is going to wake up like switching on a light. It’s like switching on a light with a dimmer slowly, right? Does it come with risks? Of course it comes with risks. You want your dad to wake up as quickly as possible and I’m with you. But the reality is that’s not happening in many situations, which is why it’s such a big point of kind of contention for families in intensive care.
They would love their life, wants to wake up quickly. But again, it’s a process and not an event. The biggest risk for your dad not waking up quickly is simply that he can’t come off the ventilator because he needs to be fully alert to come off the ventilator. He needs to be able to breathe by himself. He needs to be able to obey commands.
And I’m glad to see that you are massaging his feet. You know, you’re trying to stimulate him. That’s fantastic. And you know, you should also ask the nurses and the physical therapists and the physiotherapists to keep doing the stimulation, you know, to give him very good nursing care with washers, you know, mouth care, regular pressure area care. So it’s not getting any pressure sores so the skin doesn’t break down. And all of that.
I’m also glad that you got a neurologist involved because if he’s not waking up, he definitely will need a CT scan of the brain to rule out in neurological event to rule out a stroke and things like that. So you are definitely on the right track. But my advice really is that you will need to be patient to carry on, you know, and to be very mindful of your dad if he’s not waking up, he might need a tracheostomy which could lead to long-term ventilation and you certainly want to avoid that.
RECOMMENDED:
Sort of the cut off for removing a breathing tube is sort of 10 to 14 days. And if somebody is not waking up and they still need mechanical ventilation with the breathing tube, again might end up with a tracheostomy that could lead to long-term ventilation. So you don’t want that and you certainly need to keep stimulating your dad and the team that needs to keep stimulating your dad to get him to wake up. Other things you can do is definitely get him out of bed, sit him in a chair, even though he’s ventilated, that will stimulate him. It helps to strengthen his breathing muscles because he will need to strengthen his breathing muscles to be able to be weaned off the ventilator. So those are all very important aspects of the waking up process and the recovery. But again, I can’t stress enough that waking up after an induced coma is not a straightforward event often, especially for older patients.
Other things you need to look at is the chest x-ray. They need to do repeat chest x-rays to make sure that your pneumonia would stay clear so that he is ready for extubation, which is the removal of the breathing tube.
RECOMMENDED:
Please also keep looking for blood results such as hemoglobin levels, which are the red blood cells. Keep looking for white cell count cause the white cell count will tell you whether the infection has really gone and the normal white cell count is between four and 11. Anything above 11 indicates that he might still have an infection. Obviously, ask for your dad’s temperature. Is he feverish? Does he have a temperature? You know, that would also be an indication if he still has an infection or sepsis.
Other things you should be looking for are things like electrolyte levels such as magnesium, potassium. They can often be the range, especially during or after dialysis. And those potassium magnesium levels are quite important. Also, furthermore, if they stopped dialysis, keep looking for urine output. Is your dad now producing your own? Are his kidneys working? Is he off the inotropes that I mentioned earlier? Because if he’s off the inotropes, you know, the only form of life support your dad is on then is the mechanical ventilation.
If the dialysis stays off, because if that’s all normal, then the focus can be 100% on getting your dad to wake up. Other things that are important when your dad will be weaned off the ventilator. Again, I highlighted the importance of the chest x-ray, but also other things that are important. How often does he need suctioning through the breathing tube? Does he have a good strong cough? What are the arterial blood gases showing? Are they physiological? Are they adequate for the level of ventilation he’s getting? Can he breathe by himself?
Before he comes off the ventilator, he will need to breathe spontaneously with minimal support and the arterial blood gases need to be within physiological levels. And your dad needs to be able to obey commands such as poking out his tongue, move his feet on command, squeeze your fingers and you know not or shake his head too simple, yes and no questions.
RECOMMENDED:
So other than that, I have created extra eBooks for when somebody is not waking up after an induced car. For example, I created one ebook, The 10 most frequently asked questions when somebody is not waking up after an induced coma. One ebook with videos and audio recordings. The five biggest mistakes you are making if a loved one is not waking up after an induced coma. And I put some links below this video in the written version of this video blog and another article and video that you can read or watch is how to wean a critically ill patient off the ventilator and the breathing tube. That is also very helpful in your situation.
Well, thank you for watching. I really hope that helps Ken and I hope that helps other families that are in a similar situation.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!