Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Why is it Vital for My Ventilated Sister to be Mobilized in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy service! Marsha’s sister is with a tracheostomy and is on a ventilator in the ICU. Marsha is asking what will be her sister’s quality of life after she comes off the ventilator.
What will be My Sister’s Quality of Life After she Comes Off the Ventilator in ICU?
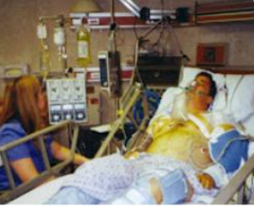
“You can also check out previous 1:1 consulting and advocacy sessions with me and Marsha here.”
Patrik: Sure, sure. How much is the fentanyl patch over 24 hours? Do you know?
Marsha: They have different ones on that. She doesn’t have any now, but I know the doctor talked about maybe putting it back and I think she would start with a 12.5.
RECOMMENDED:
Patrik: 12.5?
Marsha: 25, she said. Yeah.
Patrik: Over 24 hours.
Marsha: I think it’s 3 days. They change it every 3 days.
Patrik: 3 days, 12.5. Just give me..
Marsha: Yeah, it’s 12 1/2. It’s 12.5 every 24 hours for 3 days, yes.
Patrik: Just give me a second.
Marsha: It’s 12.5 over 24 hours, right.
Patrik: 12.5 and that is, I presume, 12.5 mg, I presume.
Marsha: I presume that, yeah.
Patrik: So that would be..
Marsha: That’s correct, right.
Patrik: If it’s 12.5 mg, did you say over 3 days?
Marsha: No, no, that’s 24 hours. But the patch has enough for 3 days in it. They change it every three days.
Patrik: Right, then it must be over 3 days. If they’re changing it every 3 days, it’s 12.5 over 3 days, is basically 96, 48. It’s basically 72 hours. Yeah, that’s 170 mcg per hour. Yeah. I would say that’s a bit too much, but what do you think would happen without morphine and without fentanyl?
Marsha: Well, she’s on with no fentanyl now and she’s on minimum morphine. I think she might be all right, but I’m not sure. And she definitely gets a little pain.
Patrik: Okay.
Marsha: I’m worried about her mobility. She won’t move as much.
Patrik: Exactly.
Marsha: Right.
Patrik: Here’s another thing..
Marsha: She’ll have a little something, but not too much.
Patrik: Yeah. Here is another thing, Marsha. You can quantify pain. And the way to quantify pain is not quantify, qualify pain, is ask her, “On a scale from 0 to 10, zero meaning no pain. What is your pain, and 10 meaning the worst?” She can give it a number, can’t she?
Marsha: Yes, yes. Usually, she’ll say seven when she’s in pain.
Patrik: Oh, is she?
Marsha: Yeah.
Patrik: Okay. So, they’re doing that.
Marsha: I’ve had her say 10. I’ve had her say 10 a couple of times.
Patrik: Right, okay. So, it sounds to me like she needs it then.
Marsha: Yeah, that bedsore’s killing her.
Patrik: Right.
Recommended:
Marsha: Sometimes, I walk in, not lately, but I walk in, “Hey, how you doing?” She goes, “My back is killing me.”
Patrik: Right.
Marsha: And the lady takes pain. And just to simply put in perspective for you, once she got out of the hospital and into this place, they got her off all the pain medication the first time. She didn’t want it at all, she was high constantly. She just didn’t want the pain medication, and then she stopped taking it because she just doesn’t like to take that stuff. But her pain is that bad.
Patrik: Right, I see.
Marsha: So, she does need it. The nurse said today, “Her bedsore’s actually healing and that’s causing her nerves to grow back, and she’s probably going to get a little more pain.” I don’t know if that’s true or not, but he said that that’s true.
Patrik: Right. I see. Yeah. Look, pain medication has its time and its place. I just don’t like it in combination with ventilator weaning. Unfortunately, one often goes with the other.
Marsha: Okay.
Patrik: Unfortunately, one goes with the other, but it..
Marsha: Stay away from it. So, you’re telling me stay away from it if I can.
Patrik: If you can, if you can.
Marsha: It’s not going to help her wean. But to me, it helps her wean, not for her pain, Patrik. It just took the anxiety off where she didn’t care. And she didn’t get nervous, because she didn’t really care what happened. I saw her like a girl who was drinking. I don’t know if you have a couple beers when you go out with your friends, you guys go out. Just she had a couple beers, she doesn’t care anymore. That’s what it seemed like to me, and she cruised. But it backfired in the end because she drank too much. You know what I mean? And she woke up with a hangover the next day. That’s what I’m saying.
Patrik: Yeah, absolutely. Absolutely.
Marsha: You think ease into it, and she’ll be better for it, if I try to keep as little of pain medication as possible.
Patrik: Absolutely. It’s as I said, Marsha. I like to keep things simple if I can, which is mobilization. Cuff down during day if she can tolerate that. If they can keep downsizing the tracheostomy, that’s great. Find out what size tracheostomy she does have at the moment.
Recommended:
Marsha: I will.
Patrik: And ask them things like, “How often does she need suctioning?” Because I..
Marsha: Okay.
Patrik: If she can cough, if she can cough up her secretions, if she can increase the time off her ventilator, I’d say now that she’s used to the speaking valve?
Marsha: She used the speaking valve a little bit. Her voice wasn’t that good today, but she does use it once in a while.
Patrik: Well, but..
Marsha: She works with her. She’s good.
Patrik: Yeah, but that’s a good sign. And if we can keep using the speaking valve, I think she’s halfway there. She’s halfway there. The setback that happened, those setbacks happen. There’s nothing there that I haven’t seen.
Marsha: But when do I worry about the insurance throwing her out?
Patrik: Great question. Has the insurance contacted you or your sister or anyone within the family?
Marsha: Not that I know of. But they can be calling her phone and I wouldn’t know.
Patrik: Are you the Power of Attorney while she’s in there?
Marsha: Pretty much, yeah. I’m her healthcare proxy, yes.
Patrik: Yeah. You’re her healthcare proxy. I would track you down, Marsha. They would go through the whole spiel, and they would say, “Hey, we need…”. The health insurance is probably the least of my concerns in a situation like that.
Marsha: Okay.
Patrik: Has the hospital come to you and has said, “Hey, the health insurance is knocking on our door”, have they said that?
Marsha: No. Well, the doctor, he said, “I don’t know what health insurance your sister has, but she’s been here a while. I can guarantee you a couple more weeks, but after that, I can’t guarantee you,” she said. She said, “All these companies, I don’t know who she has. I’m just telling you.” In her experience, she said, “Marsha, I’m going to do everything I can to keep her in here to get her off the ventilator, but I’m just letting you know.”
Patrik: Yes. No. That’s a fair call, but my experience is the health insurance is not the major concern in those situations. If you go back to the health insurance and you say, “Hey, my sister needs another couple of weeks here or maybe even another 4 weeks,” they understand. I haven’t found that they are too hard-nosed about this.
Marsha: Okay.
Patrik: If the hospital came to you every day and said, “Hey, you got to talk to the health insurance”. The health insurance is telling us, “She needs to be out of here by Wednesday,” I would be worried. But as long as you haven’t had those.
Marsha: Okay.
Patrik: As long as you haven’t had those conversations with them, I believe you’re not too worried about it.
Marsha: Okay.
Patrik: How many days has she been in there, in this particular place?
Marsha: 7 weeks.
Patrik: 7 weeks. And how long was she in ICU for?
Suggested links:
- My 72 year old Mum’s been in ICU for 6 weeks after stroke,tracheostomy & ventilated,can she go home?
Marsha: Between that and the step-down unit, she was in ICU from August 7th until she got here. So, it was like another..
Patrik: 7 weeks. Yeah.
Marsha: … 7 weeks.
Patrik: And you have not had any conversation, communication, with the health insurance whatsoever?
Marsha: Well, prior to when she got here at the LTAC, I doubled her.
Patrik: Right. And what were the dealings you had with them then?
Marsha: There was no LTAC near her house that..
Patrik: Oh yeah.
Marsha: … accepted her insurance. So, I had to get them, the LTAC and the insurance company, to come to an agreement. Because they were out-of-network, and they did.
Patrik: Right, okay. I see.
Marsha: That’s about it. The lady was pretty good.
Patrik: I see. Okay, all right.
Marsha: … with the insurance company.
Patrik: I’m worried about health insurance if they start calling you. That’s when I get worried about it. Other than that, I wouldn’t lose any sleep over it at the moment.
Marsha: Okay.
Patrik: I really believe you have every reason to be optimistic here. I really believe that, but mobilization is going to be very important.
Marsha: Okay.
Patrik: Sitting up, breathing exercises, strengthening breathing muscles, strengthening upper body. She will need to be able to take deep breaths. She will need to be able to cough.
Marsha: Okay.
Patrik: Right? That is..
Recommended:
- CAN INTENSIVE CARE AT HOME TRAIN FAMILIES TO LOOK AFTER LOVED ONES ON A VENTILATOR and TRACHEOSTOMY?
Marsha: Right.
Patrik: That is so important. Imagine, you’re lying in bed for weeks on ends. You can’t come off the ventilator or it’s much harder.
Marsha: Right.
Patrik: It’s like I always argue that when I used to do the bedside nursing. You sit someone out of bed after weeks in bed. That’s the highlight of their, the last few weeks.
Marsha: Right.
Patrik: And imagine that you can do more of that. There’s a huge psychological aspect there.
Marsha: So, if you put me and you on a ventilator, how long would it take for us, healthy guys that can breathe right now with no ventilator? How long would it take us not to breathe, for us not to be able to breathe on our own?
Patrik: Say that again.
Marsha: So, you bring a healthy individual, you did an experiment. Say you did an experiment. Say we agreed to do this. Okay, put us on a ventilator, sedate us. And how long would it take for us not to be able to breathe on our own, with no disease, just a ventilator? So how long does it take? So, in other words, what I’m trying to say is the ventilator causes you to rely on the ventilator.
Patrik: Yeah.
Marsha: That’s crazy, Patrik.
Patrik: Yeah. I’m not..
Marsha: For us, laypeople don’t realize that.
Patrik: Oh no. I do realize just… No, I think..
Marsha: No, no, I’m saying I’m a layperson. You realize it, because you did this for a living, but an individual like me never realized that until now. I’m like, “Hey, most laypeople, us, in the general public have no idea.” We think, “Oh, you put them on the ventilator and when she can breathe, you take her off.”
Patrik: No, no.
Marsha: That’s not how it works.
Patrik: No, that’s not how it works. No, not at all, not at all. I mean, there are some people. They come off the ventilator very quickly. They only need the ventilator for a few hours after surgery. And there’s a lot of those people in hospitals. But anything that’s really critical, like your sister, it’s complicated or it can be complicated.
Marsha: Yeah, it’s very complicated.
Patrik: Yeah.
Marsha: And I want to ask you another question, a personal question. I know there’s a lot of people I run into in the hospital. A doctor told me that she would never be put on a ventilator. How do you feel about the use of the ventilator in general?
Patrik: Oh, I think it saves lives. I think.
Marsha: But you would let yourself be intubated and be put on a ventilator?
Patrik: Oh yeah, for sure. No. For sure.
Marsha: Oh, really? Okay.
Patrik: The problem is that most people that have been on ventilators, especially long-term, unfortunately your sister’s life has changed. And she may never be back to where she was before, but that remains to be seen. The bottom line is ventilators change lives or save lives.
Marsha: Right.
Patrik: The question is, is it the same quality of life after you’ve come off a ventilator than before? But those are questions one can’t really answer before it happens.
Marsha: Right. Well, I think if she gets to where she doesn’t need the ventilator and be able to work to a decent quality of life where she might not be happy with what happened to her, but I think she’ll live a good life. I think she’ll be fine.
Suggested links:
Patrik: I think so, too. I think so, too. People have different philosophies around quality of life, but she’s alive.
Marsha: Right. Well, if she was staying the way she was now, I’d say alive is overrated then. What I see, Patrik, I tell my husband, “I never want to go through that, so don’t hold onto me too long if that happens”. But I’m not sure yet, because I don’t know the full details. To make an honest decision, she would have to recover 100%, and then I need to talk to her and to see what she really knew and what she didn’t know and what she went through.
Patrik: Exactly.
Marsha: Yeah. But, Patrik, I’m going to owe another $50. So, I want you to send me a receipt, okay?
Patrik: Oh no, no. You don’t owe me anything.
Marsha: Oh no, you kidding me? Because I’m pay you for another one. I’m definitely going to see you again, but I..
Patrik: No.
Marsha: … gave me an extra 25% here. That was really nice.
Patrik: Yeah, no, no. Look, if you need anything, just get back to me and we’ll work out what we’ll do next. But I think you have a real reason to be optimistic here.
Marsha: Okay.
Patrik: And keep pushing. Keep pushing.
Marsha: I will.
Patrik: Get her out of bed.
Marsha: I’m going to do that.
Patrik: Please.
Marsha: Patrik, thank you so much. I will definitely be in touch.
Patrik: It’s..
Marsha: Either way, but I probably will need another consultation in a couple days or weeks.
Patrik: Yeah, sure. I’m also happy to talk to them if you want me to. But that’s, of course, up to you.
Marsha: Yeah. Obviously, that’s more complicated. I just wanted to do the first one this way. I was going to sign up for..
Patrik: Yeah, of course.
RECOMMENDED:
Marsha: … 30 days and I’m like, “Let me get the first one.”
Patrik: No, exactly.
Marsha: And let me see how it goes.
Patrik: Exactly.
Marsha: And if it goes well, then I’ll just do it by consultation. I’ll need consultation to get her home. We’ll talk about rehabilitation. So, I’m definitely going to be back. But if it goes bad, then I probably would have to sign up for the 30-day and just say, “All right, Patrik, I’ve signed up for 30-day”
Patrik: Yeah, all good, all good.
Marsha: Thank you very much.
Patrik: It’s a pleasure. Have a good night. Thank you so much, Marsha. Take care.
Marsha: No, the pleasure was all mine. God bless you, Patrik.
Patrik: Same to you. Thank you so much. Bye-bye, bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







