Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
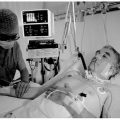
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy service! Marsha’s sister is on a ventilator and with a tracheostomy in the ICU. Marsha is asking why is the ICU team in a hurry to transfer her sister to LTAC.
Why is the ICU Team in a Hurry to Transfer My Ventilated Sister with a Tracheostomy to LTAC?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Marsha here.”
Patrik: Right.
Marsha: And when I go and I ask her, “Hey, did they come in?” And so yesterday… Yesterday they didn’t come in when I was there to see her, but they were in the day before, I think. So, I think it’s like every other day.
Patrik: Right.
Marsha: I mean, I asked her what they do, and she said, “Basically the same thing you do every time.” That’s what she told me.
Patrik: Right, okay. Okay. Look, I do believe every time someone goes from a hospital, or a major hospital to LTAC or to a step-down, there’s a drop in the level of care, okay?
Marsha: Right.
RECOMMENDED:
Patrik: I do believe it’s inevitable for you, or for other family members, to speak to the place that she’s supposed to go, even do a visit if you can, and get a feel for it. I think it’s highly inappropriate for the hospital to say it would send your sister out tomorrow. You have no warning. You haven’t even met anyone there. You don’t know what this place is all about. They haven’t given you two or three options. I think that’s not unreasonable, to give you options, you know?
Marsha: Right. So should I call the doctor or the social worker?
Patrik: Potentially both. And you want to-
Marsha: And I mean, what should I… Well, yeah. I’m sorry.
Patrik: Yeah. You want to find out, is this place getting results or is it… For example, for all I know, you never know. This place where she’s going to could be affiliated with this particular hospital, and there could be three other subacutes that are not affiliated with this particular hospital. You know what I’m saying?
Marsha: Yeah. This one was affiliated. The one that I picked was affiliated.
Patrik: Right. Right, but-
Marsha: But now, I picked it because of the location and what he gave me.
Patrik: Sure, sure. But-
Marsha: I’ll be honest with you, I thought it was going to go the same way that it went with the LTAC. I had a lot of input with the LTAC. I went to visit them. He didn’t give me that option. He didn’t relate it to me. I thought he was just going to put in, and then when they said, “Okay, we’ll take her,” then they would tell me, “These three facilities accepted her.” And then I was going to say, “Okay, I want to go visit them.” But it didn’t seem like it was going to go that way then.
Patrik: Right, right. But I mean, you can see it’s very reasonable to ask these questions. There’s nothing unreasonable in that.
Marsha: Right.
Patrik: I think, and I’m exaggerating a little bit when I’m saying, they’re walking all over people. They’re just making decisions without consulting with families. That’s just inappropriate, as far as I’m concerned.
Marsha: Right. So now, how do I put that? But they didn’t even call. They put in for the LTAC and didn’t even call me, now. They’re supposed to call me. Every other time they used to call me and say, “Listen, this is the next step.” They didn’t do that. I found out from a doctor, that I walked in and said, “Oh, yeah. They denied her from going to the LTAC.” I said, “Good, because I was going to object to that.” They said, “Why?” I said, “I don’t want her going back to an LTAC.”
Patrik: Right. Exactly, exactly. So I really think you’re not asking for anything unreasonable here whatsoever. And if you’re going to object and they are resisting that, you should be asking for their discharge policy. I’m sure, (a), they must have a discharge policy. And, (b), there must be something in the discharge policy, something like that several options need to be given when it comes to external transfers. That families need to be given the opportunity to meet them, and have some lag time. And possibly see that a transfer can’t happen without next of kin or power of attorney consent. So there’s a good chance that if you look at this policy, that they might be breaching it on all levels.
Marsha: Okay.
Patrik: Right? But irrespective of the policy, I do believe everything that you’re asking for is very reasonable.
Marsha: So now, just to tell you, Patrik, I got to see her because I wrote two letters. Because of COVID they stopped visits, and I wrote two letters and a release form with them, and I got in to see her. So I’ve been pretty low-key. I’m afraid they’re going to take away my visitation rights, and if I have no contact with her, then they can do whatever they want. Which sounds crazy, but they can get away with it.
Patrik: Right, right. Well-
Marsha: I mean, think about it. If they tell me that I can’t see my sister because I may have a disease, that I have antibodies against, and that I have a shot… After I got COVID then I got one shot, because I have the antibodies. My antibodies waned, so I got one shot. My antibodies went through the roof, and so I’m not going to get another shot, because I’m going to wait for my antibodies to wane again. But they’re telling me I can’t see my sister because… I mean, they’re telling this to everyone. “You can’t see your loved one or your family member because you may have COVID.” Well, I can prove I don’t have COVID right now.
Patrik: Right.
Marsha: So I really had to fight with them. And they were telling me, “Well, she can FaceTime.” I said, “No, she can’t FaceTime. If you read the letter I wrote, she can’t FaceTime because she has a tracheostomy and she can’t even handle her device. So, what am I supposed to do? Look at a picture of her? How am I supposed to…” I mean, she can’t talk. She has a tracheostomy. So I’m afraid that if I start saying, “Wait a minute, we’re not consenting to that,” that they’re going to say, “You know what? We’re going to revoke your visitation.”
Patrik: Look, Marsha, I hear what you’re saying. But I think fear is never a good strategy. And I hear you, loud and clearly, but I think you should be asking for what you want irregardless. Irregardless. As I said, I hear everything that you’re saying. But, look, I do believe everything that I’m observing in the environment, we have so many people coming to us, and they come to us when their loved one has been transferred and they say things like, “Oh, if I had known I would have never agreed to that.” Right?
Suggested Links:
Marsha: Right.
Patrik: Also, I’ll tell you another thing. Yes, I can understand why people are scared of repercussions, and I know hospitals can be very mean. I get that. But I do believe your sister is at a critical point. Would you say she’s developed, would you say she’s come off the ventilator faster than you thought she would? Or, what do you think?
Marsha: That’s a good question. Well, faster like they pushed her, or faster like she did better than I thought?
Patrik: Yeah, probably the latter. So when I just had a look, you and I last spoke on the 30th of March.
Marsha: Correct.
Patrik: So, today it’s the 28th of April, so about a month.
Marsha: Correct.
Patrik: When we last spoke in March, what were you thinking then? How far away were you thinking she is to coming off the ventilator?
Marsha: At this point?
Patrik: Yeah, so-
Marsha: I thought it was probably about the same time. I thought one of her issues was she was starting to come off the ventilator, but after talking to you I thought she had to get in a little bit of better shape. That’s the only thing I don’t like, I wish she was in better… If it was ideal for me, like if I brought her home… Say I had to bring her home. Say she couldn’t get off the ventilator, and she was going to go to an LTAC or come home. I would’ve brought her home, or maybe tried a different LTAC, and keep a close eye on her and prepare to bring her home. So if it was me, I’d want her in better shape. I feel like there’s no room and there’s no therapy here. The first thing that happens to her, she hits a bump in the road, now she’s in a subacute rehab that doesn’t have a ventilator. Now what happens?
Patrik: Right.
Marsha: So, but they’re like, “Oh, 48 hours off, and she’s considered off.” I guess that means, wow, we can consider her off the ventilator.
Patrik: Yup. Look-
Marsha: So I hope that answers your question. I don’t…
Patrik: Yeah. Look, Marsha. Even if you thought this was a good move, it’s still not appropriate to say, “Oh, we’re going in 48 hours,” or, “We’re going in 24 hours.” It’s still not a good move from them, right?
Marsha: Right.
Patrik: I’ll tell you another thing that I’ve learned. I know hospitals are used to getting what they want. They’re used to that, okay?
Marsha: Right.
Patrik: And if you start objecting, they’re not used to it. And yes, they might make things a little bit more difficult, but I’ve also learned if you stand your ground they will eventually give it.
Marsha: Okay. I have no problem… And trust me, Patrik, you’ve got the right guy. I’ve been guilty of that a lot. In this situation, I’m just a little tentative because it’s a hospital, but my personality is just that. I have no problem doing it.
Patrik: I thought so. I thought so.
Marsha: I’m not like that.
Patrik: You don’t strike me-
Marsha: I just want to be confident. Well, I don’t like the feeling when I don’t have the information. That’s where you come in. And when I don’t know the terminology, or what to say? Or what are my grounds? Or what do I really want? I hate to do that when I don’t even know what I really want, you know what I mean? So that’s why I thought I needed to talk to you, because you need to tell me, “This is what you want, this is how you’re going to go about getting it.” And I have no problem doing it.
Patrik: Yeah, yeah. You don’t strike me as someone that gives in easily. And you’ve got to go about it the right way, of course. You don’t want to be rude. But, Marsha, everything that I said in terms of you need some warning, you need to see those other facilities, you need to talk to people. That’s not unreasonable, is it?
Marsha: No, not at all. But I’ll be honest with you, to me it’s amazing. I should have known better after totally being hurt by it. To me they made it seem like, “Oh, it’s just, she’s going to rehab. She’s on her way home, she’s just got to get some work.” So in my head, my thing was I want her close to that hospital if something happens. And they were pretty much all going to be the same in my head.
Recommended:
Marsha: And I noticed that a couple of them were nursing homes and a couple weren’t, and I asked about that. He said, “They’re all considered nursing homes, but this one is not a nursing home.” So I gave that my first choice, because I didn’t want her to be in a nursing home facility. And he said, “Okay.” But then they told my father she was getting transferred. I called the social worker and I said, “My sister’s getting transferred tomorrow?” He goes, “No, who told you that?” I said, “The nurse told my father.” And he goes, “No, the nurse lied to you.” And he said, “Her insurance didn’t get accepted. I have to find a facility that uses her insurance.”
Patrik: Yeah. Well, that’s another good point, Marsha. Talk to your insurance or to her insurance, right?
Marsha: Right.
Patrik: Make sure, (a), it’s all covered, right? Look, you can just go back to the hospital and say, “Hey, there might be some insurance issues. I need to talk to them.” That’s all you need. They wouldn’t know.
Marsha: Right.
Patrik: Talk to them. I think everything we’re looking at, there’s absolutely nothing unreasonable, I think from what you’re asking for. Nothing unreasonable whatsoever.
Marsha: Okay. So now, from a medical standpoint, if I’m going to call the doctor in charge of the rehab, well, should I say, “Listen, I think it’s too early to discharge her. I don’t think they should be discharging her already”?
Patrik: Yeah, I think-
Marsha: Or should I just play the angle of that, okay, I’ve got to research these places and dirty my feet a little bit?
Patrik: I think so. I think so. I think that you should play the angle of researching the places. I think so.
Marsha: And then don’t say anything about me objecting to the things? Act like I’m going along.
Patrik: Correct.
Marsha: Like say, “Yeah, she can go to rehab but I’ve got to research the places”?
Patrik: Correct, correct. You want to make sure that you’re… And you can actually take your last experience as an example, where she was going to LTAC, and then she bounced back. I mean, that in and of itself is not a great experience, and you can say that. You can say, “Hey, we didn’t research the places last time, and it didn’t serve my sister well.”
Marsha: Okay.
Patrik: And if that doesn’t work, then you should play the card of hospital policy about discharge.
Marsha: Okay.
Patrik: How does your sister feel about it?
Marsha: I didn’t get a chance to talk to her, and that’s why. Normally I see her every day.
Patrik: Right. Right.
Marsha: But yesterday I saw her and she was a little down, so I thought it’d be better if my father saw her because he hasn’t seen her yet… She hasn’t seen him. So I said, “You know what?” I told him how to get in, because technically I’m the only one that’s supposed to go and see her. But I just, I said, “Pa, go early, and if they don’t let you in don’t argue with them. I’ll just go see her.” But he got in. They let him in, and then he was getting all this information. So I didn’t see how she felt about it. I don’t know how she felt about it.
Patrik: Right, right. But-
Marsha: She’s saying she wants to go home at this point, but a couple of weeks ago she didn’t want to go home and I said, “Liza.” I thought she was going back to the LTAC and I was just preparing her. I was like, “We’ll just go home after this and we’ll just wean you off at your house, at your own pace.” But, and she was like, “No, I don’t want to go home with the ventilator. I don’t want to go home with the ventilator. I’d rather go to the LTAC, but not that one.” She said, “Send me to another one.”
Marsha: I said, “Hey, I don’t think that’s a good idea. I think you should honestly just think about going home.” But yesterday she actually said to me she wants to go home. She’s like, “I want to go home.” I said, “I understand. You’ve been through a lot.” She was totally upset, and she usually doesn’t get like that. She hasn’t been like that in a month, so I felt bad for her, but I didn’t know what to tell her. I said, “Liza, hopefully, you go to rehab and you just do your exercises. You’ll be able to walk from across the room, be able to go to the bathroom by yourself, and then you can go home.” I told her, “You can just sign yourself out if that’s the case, once you get too frustrated. As long as you know that you’re going to do the work at home, or get your physical therapist to come at home.”
Patrik: Right.
Suggested Links:
Marsha: So I was just telling her that, and I was going to research it with you first. But, you know.
Patrik: Yeah. Now, let me ask you another question. Knowing what you know now, not only with your research but also with the transfer with your sister last year, knowing what you know now would you have agreed for her to go to LTAC last year?
Marsha: The problem with that was… Well, I wouldn’t have done that LTAC, I would’ve tried another one. But the problem with that was that the hospital put her in a step-down unit, and that’s what pushed her. I was saying that she should stay in the ICU as long as possible. I wanted her to stay in the ICU as long as possible, and they knew that. And I became friendly with some of the nurses, and I maybe fit right in a little bit because I was there all the time.
Patrik: I see.
RECOMMENDED:
Marsha: And then one day, without telling me, they transferred her and then called me up and just called me, “Hey, we transferred her to a step-down unit.” So I didn’t fight them on that. I didn’t think it was a big deal. But then when I got to the unit, I saw that it made her uncomfortable. I was dragging my feet with the LTAC and I was going a good job of doing it, because the insurance doesn’t cover a lot of LTACs where she was going, so I was able to really drag my feet. But then she got frustrated and she said, ” Marsha, I want to go to the LTAC.”
Patrik: Right.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!