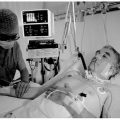
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of YOUR QUESTIONS ANSWERED and in last week’s episode I answered another question from our readers and the question was
Will My Sister Ever Get Off the Ventilator in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy service! Marsha’s sister is in the ICU with a tracheostomy. Marsha is asking what are the things that they should demand from the ICU team for her sister to come off the ventilator.
What Should We Demand from the ICU Team for My Sister to Come Off the Ventilator?
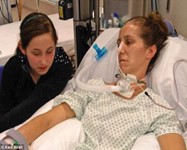
Patrik: Yeah, yeah. I get that, I get that. Look, from my experience, Marsha. Getting in a recliner chair is very good. And I argue that you can’t come off a ventilator without getting mobilized.
Patrik: Yeah, yeah, sure.
Marsha: Sometimes, I’m there all day and they never come back.
Patrik: Yeah, yeah. I get that, I get that. Look, from my experience, Marsha. Getting in a recliner chair is very good. And I argue that you can’t come off a ventilator without getting mobilized.
Marsha: Okay.
Patrik: Right? So, picture this-
Marsha: Make sense.
Patrik: Picture this, you’re lying in bed all day, every day and you’re meant to wean off a ventilator. You’re weakened already, because you’ve spent weeks on the ventilator in an induced coma. Deconditioning is real and it’s quick, and the only way-
Marsha: Oh, Patrik, I’m not meaning to interrupt you, but you’re a smart man and I always want to hear what you have to say. I cannot believe what I witnessed with this deconditioning. It is crazy.
Patrik: Right.
RECOMMENDED:
Marsha: It is crazy how real it is. You’re so right. She is so skinny and so frail. This woman was built not big necessarily but like a rock. It’s just unbelievable and I’m sorry.
Patrik: Yeah, no. No, no. So, you have seen that for yourself. Like you mentioned, I remember when we last spoke. You said your sister was fit, going to the gym, from memory, and all of that. And you can now see how quickly that can turn the other way.
Marsha: Right.
Patrik: Right? So, with that in mind, anybody that’s done any form of exercise in life, knows building up exercise tolerance takes time. It doesn’t happen overnight. If you want to run a marathon, you need to train hard for it. Anyway, the reason I’m saying all of this is, one way to come off a ventilator and off the tracheostomy is to strengthen the upper body. And you’re not strengthening the upper body and your breathing muscles by lying in bed.
Marsha: Okay.
Patrik: Right? So, by sitting in a-
Marsha: Right, right.
Patrik: By sitting in a recliner chair, and I can tell you, even if it’s only for half an hour a day, you got to start somewhere. Because by sitting up, and then by doing breathing exercises and just by having the upper body sitting up, that’s strengthening muscles. It’s strengthening breathing muscles. It increases the chances of her getting off the ventilator. It usually strengthens the cough. The best analogy that I can give to that is you can’t run a marathon without training.
Patrik: It’s the same by weaning off a ventilator. You can’t wean off a ventilator without sitting up, without doing some training, and I agree with you. I’ve seen all of that in my practice. The physiotherapists are coming by, “Oh yeah, she’s weaning. We’re coming back,” and then they never come back. I get all of that. That’s the reality of a hospital, but-
Marsha: Well, can I just stop you there before I forget?
Patrik: Please.
Marsha: So now, how do I handle that? My father, he call them out and being a little mean. I go in a friendly way and try hard to be friendly, so I try to be nice to everyone. I befriend everyone. If someone will talk to me, I’ll talk to them. I’ll learn about them, and their situation. Some people don’t want to talk to me, but yesterday for the first time, I said something to the physical therapist, not yesterday, Thursday. I said something to the PT, I said, “Listen, my sister tells me, yesterday, you came back by the room. You saw she was weaning and then you never came back. She needs to condition herself.” And so, she said, “Okay.” And she came in and did her exercises, but she just did something to just make me shut up. She just went through the exercises to make me shut up. Well, personally, I want to try to get her up myself some days, because they’re not around. And then, you get one shot at them, and they just squeeze by you and go to the next one. So how do I handle that?
Patrik: Yeah, that’s a great question. It probably depends a little bit on the vibe in the place. What’s the vibe you’re getting from the place? Is it a good vibe overall? Is it a negative vibe overall? What’s the vibe?
Marsha: No, I like the doctor a lot, the doctor that’s in charge of her. And I think, overall, it’s a decent environment. Once in a while, I get a person I don’t want to take care of her. Once in a while, I get a respiratory therapist who thinks they’re a nurse or a doctor, and they’re not. And they say things to her that I cringed, and they shouldn’t say to her like, “Oh, your lungs are bad. Your lungs are bad,” stuff like that. And just to me, I’m like, “Man, are you serious?” but I didn’t say anything.
Marsha: But I think the vibe all in all is not, as far as LTACs go, I would think it’s not that bad. I even recommended a couple of people. I went there, my father went there separately. We visited several of them. This was our choice and the social worker in the hospital said that they have a good reputation of getting people off. After she was already on her way to the LTAC is when I read your article and I said, “Man, I wish I would’ve contacted Patrik before she left,” but it is what it is at this point.
Patrik: Of course, of course. Look, to come back to your question, how should you handle this? I’m all for making friends, but there might come a point where, depending on how busy they are, depending on their culture, and all of that, where you might need to change tact. There are many situations that I’m dealing with where it’s gone beyond making friends, where making friends, if anything, is an obstacle.
Marsha: All right.
Patrik: So, if that strategy with being friendly with people, doesn’t work. Then unfortunately, you got to start questioning, and you got to try and hold them accountable. Even that can be done in a friendly way. You seem to have a very good understanding of what needs to happen and even that can be done in a friendly way. But unfortunately, there might come a point in a hospital where the friendly way just doesn’t work anymore, because they’re busy. If you start making a bit more noise, they may not like it, but we will actually see sort of the squeaky wheel, gets the oil sort of thing.
Marsha: Well, Patrik, that’s the scary part. They have a lot of empty beds right now, it’s their slow season. I’m afraid they’re going to get busy now that COVID’s kicking up a little bit. There’s a lot because I look down the halls, I’ve been going here for seven weeks. And I see all the empty beds, not a lot of people, so they’re not that busy. So that’s the scary part. I’m like, “What happens when these guys get busy?”
Patrik: I have something to say about that, Marsha. Empty beds don’t necessarily mean they are not busy, it could simply mean they have no staff.
Marsha: Oh, all right.
Suggested Links:
Patrik: The-
Marsha: Okay.
Patrik: The reason I’m saying that is, especially with the pandemic, there is such a shortage. Nurses are leaving the industry, unfortunately. They’re burned out.
Marsha: Right.
Patrik: Some of them are losing their jobs because they don’t want to get vaccinated because of the mandates that are pretty much rolled out, pretty much everywhere. So, there could be a number of empty beds, it’s not necessarily a sign that they’re not busy. It may be. I don’t know their staffing situation, but I just probably need you to think about that. Whether it’s not-
Marsha: Right. No, I’m glad you said that. I never thought of it that way.
Patrik: Right. Whether it’s not being busy, it may well be the case. But it might just be as simple as not having staff.
Marsha: Okay.
Patrik: Right? So okay, let’s just go back. So, she was off the ventilator for 11 days, then she had an infection that set her back.
Marsha: Right. The infection was a combination of a reaction to the drug where, Patrik, she was wiped for three, four, five days, up for 24 hours. I stayed with her one night in the hospital. I stayed with her awake. She was like a person that was on cocaine for five days, ripping wires out, trying to get up. I hate to say it was actually funny at times, but..
Patrik: Yeah, yeah.
Marsha: I was like, “Why were those fingers pointed at me?”-
Patrik: Yes, yes.
Marsha: Then, violently hit me. She’d get mad when I’d tell her something and she’d point in my face. And I’d tell her, “Scold me, but you can’t talk like that.” You know what she’d say?
Patrik: She-
Marsha: I’m sorry, what?
Patrik: The technical term is she was pleasantly confused.
Marsha: Yeah, yeah, yeah. You know the tank with the oxygen sensor? I kept telling her, “Stop pulling that off.” And I would nod out there next to her. And I’d hear the beeping, and I’d open my eyes and look at her. I’m right next to her and she’s standing there holding the oxygen sensor in her hand, ripped off her finger. And I’m like, “Oh my goodness,” then we put it on her toes, because we convinced her, “Okay, listen. Okay, you want us to put it on your toe?”. She goes, “Yeah.”
Marsha: And I nod out for two minutes. Her sock is off, and she’s got it in her hand. I’m telling you, she was exhausted from being up for four or five days. She got a blood infection, and I didn’t make a big deal about this, Patrik, but they were not giving her IV fluids. She was severely dehydrated.
Patrik: Do they-
Marsha: So, I didn’t make a big deal and I should’ve noticed it. Because between you and I, the night I stayed with her, when she peed, I always tell the nurse, “How much?” Because I just dump it out. I tell him, “How much? How many? What number on that thing?” This way, he doesn’t have to do it. But when she peed, she barely peed to like 50 ml and it was dark. And I-
Patrik: Yeah.
Marsha: I was thinking in my head, “Man, she looks dehydrated.” And sure enough, her blood pressure drops the next day. I mean, listen, the doctor told me, “Marsha, she almost died today.” I was in the room. I thought she was going to die. In my head, I was thinking, “Oh, she’s dying soon.” But she got through it, but I didn’t make a big deal about it. One of the nurses, who I became friendly with, he told me, “Marsha, I don’t know who stopped her IV fluids. She hasn’t had these in days.” So, she was-
Patrik: Yeah, I see.
Recommended:
Marsha: – dehydrated.
Patrik: I see.
Marsha: Yeah.
Patrik: Okay. And then, she is over that infection now?
Marsha: Well, no. She’s been treated for a couple of days now, so I forgot how many days. I want to say they started her on the IV antibiotic on the 14th. So, I think they got to run it 7 days or 10 days. So now, they’re texting me, “Hey, she’s getting better. She’s getting back to herself.” I don’t know what she really means, if she’s talking about the infection or just, in general, she’s getting back to her normal level, so I think she’s doing pretty good. So, I don’t think that’s an issue anymore, because I think she might not have technically finished the antibiotics. But I don’t think she still has an active infection. And I’m just worried about how do I handle the anxiety, too. I don’t know how to-
Patrik: Yeah.
Marsha: – handle it.
Patrik: Right.
Marsha: So-
Patrik: Do you know what medications she’s on at the moment?
Marsha: Very few, but Zoloft is the only drug she’s on. They had her on Seroquel at one time. She had a bad reaction to that where she became terrified. It probably worked for a little while and she would tell me, “Marsha, don’t leave me.” I couldn’t leave her, but she used the word terrified. This woman never gets scared over anything, and she used the word terrified, so my husband looked it up in the drug book. He’s like, “Marsha, just ask them to give her something else because of all that.” And they gave her BuSpar, which seemed better.
Patrik: BuSpar?
Marsha: And then when she was going crazy. Yeah, BuSpar, B-U-S-P-A-R. It’s like an antianxiety medication.
Patrik: Yeah, okay. I’m aware of Zoloft, and Seroquel. I’ve never heard of BuSpar, but I need to look it up. Maybe it’s under a different name.
Marsha: Okay. They said it’s a little minor one, but they took her off that one. She started going crazy. They took her off everything except Zoloft.
Patrik: So, she’s-
Marsha: And morphine. Zoloft and morphine and she was on a blood pressure medication. They took her off that. She might be on a steroid now. I don’t know why. Someone said she might have a little fluid in her lung, but I don’t know what that’s about. So, I couldn’t get a straight answer on that. So, I have to find out about the steroids, but that was just recently added. And then, they took her off the blood pressure medicine after her blood pressure went up.
Patrik: Right, okay. Right. With the morphine, I tell you what I don’t like about the morphine and the fentanyl. Now, it sounds to me like the fentanyl was the right thing for her last week. But again, morphine and fentanyl, part of, or one of the main side effects is simply respiratory depression.
Marsha: Right.
Patrik: Right? And that’s what I don’t like in your sister’s case. But it also sounds to me like, even that today, it was the first day again where she had time off the ventilator. That is very encouraging.
Marsha: Right
Patrik: That is very encouraging. And I do believe that the secret is, there is a secret, it’s really about ongoing mobilization. Also, by the sounds of things, is it fair to say that it’s been two steps forward, one step back? Is that fair to say?
Marsha: Oh, absolutely.
Suggested Links:
Patrik: Okay. So, there’s nothing-
Marsha: And I’m going to interrupt you because I just want you to have all the information. It usually seems like it’s a combination of medication that gets her going in the first direction, and then she goes off the end. So, the first time was Dilaudid and Seroquel that set her back, where she was nice and mellow. She was doing all right. She had Dilaudid, because she had a couple of procedures done on her bedsore. And in the hospital, they use Dilaudid.
Marsha: And when she came to this place, all of a sudden, they call me up in the middle of the night. She has her clothes off. She’s trying to get out of bed. So, I said, “Take her off those medications.” Took her off those medications. Just use morphine as needed, did okay. They added the fentanyl back, did okay. Added more fentanyl, when I was gone, for two days, and upped her dose. I don’t know why. And then, boom. Again, off the deep end. Crazy and then sets her back.
RECOMMENDED:
Patrik: Yeah. So, I don’t see anything that you’ve described to this point as too unusual, because it is often two steps forward, one step back. I also like simplicity. As much as those situations are complex, I’ll tell you something, Marsha. When someone comes off the ventilator, you start with 5 minutes on the tracheostomy shield. And then, the next day, you might increase to 10 minutes. And then, the day after, you might increase to 15 minutes. And then, maybe you’re working your way up to an hour a day. And then maybe you’re working your way up to 2 hours a day. I believe your sister is heading in the right direction, but it’s just slow.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!