Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What Should We Demand from the ICU Team for My Sister to Come Off the Ventilator?
You can check out last week’s question by clicking on the link here.
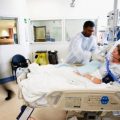
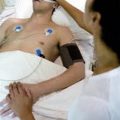
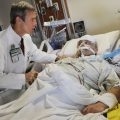
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy service! Marsha’s sister is with a tracheostomy and is on a ventilator in the ICU. Marsha is asking what else they can do to help her sister get off the ventilator in the ICU.
What Else Can We Do to Help My Sister Get Off the Ventilator in the ICU?
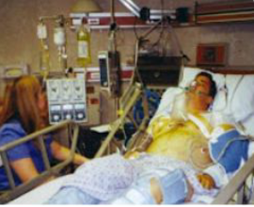
“You can also check out previous 1:1 consulting and advocacy sessions with me and Marsha here.”
Patrik: Yeah. So, I don’t see anything that you’ve described to this point as too unusual, because it is often two steps forward, one step back. I also like simplicity. As much as those situations are complex, I’ll tell you something, Marsha. When someone comes off the ventilator, you start with 5 minutes on the tracheostomy shield. And then, the next day, you might increase to 10 minutes. And then, the day after, you might increase to 15 minutes. And then, maybe you’re working your way up to an hour a day. And then maybe you’re working your way up to 2 hours a day. I believe your sister is heading in the right direction, but it’s just slow.
RECOMMENDED:
Marsha: Right.
Patrik: Right? That’s..
Marsha: So..
Patrik: Unfortunately, reality, that it’s often a slow process and there are setbacks. And I can’t tell you how many patients that I’ve seen over the years that take steps forward, and then they end up with an infection. Nothing that I haven’t seen before. But the challenge is she doesn’t need a second infection, because that could be another setback that she simply doesn’t need.
Marsha: Well, how do I avoid that?
Patrik: Is she in a room by herself?
Marsha: Yes. Oh, that just jogged my memory. So, one of the reasons why I picked this place over the other place was because they guaranteed me a room by herself, one. And two is the visiting hours, because I wanted someone with her a lot. And I wanted to be able to come and go, the visiting was lax. Where the other places, it was two visitors a day and that’s it. And here, I can come for 3-4 hours. Someone else could come. I could leave and then come back at night. There’s no limit as far as..
Patrik: That’s..
Marsha: The only limit is 2 at a time. Now, we only keep it to 5 people. Her 2 kids, her boyfriend, me, and my father, because we don’t want her to get sick.
Patrik: Of course.
Marsha: We keep it to 5 people on our own.
Recommended:
Patrik: Of course, of course. Look, but to come back to your question, how do you avoid an infection? Obviously, the best way to avoid an infection is by going home, because the infection risk at home is so much lower. Part of the infection risk in a hospital is there’s so many sick people around, and the nurses and the doctors might bring in a bug from next door sort of thing. That’s often how people end up with an infection. The problem is, as much as I’m all for home care, it takes time to set it up and you need a team at home. From what I’m hearing, Marsha, your sister is sort of halfway of getting off the ventilator. Is that your impression too or am I just?
Marsha: No, I think yes. I agree. I’m worried about them cutting off the insurance.
Patrik: Right.
Marsha: That’s what I’m worried about. That’s what I’m worried about. I think she can get off, but I think my problem is, (A) not everyone there believes it. So, when I get a non-believer, what I say to a non-believer, like a respiratory therapist, there’s a non-believer. They almost want to make themselves right and they want her to fail, it seems like to me. But when I get a good respiratory therapist and a good nurse, a doctor who’s good, and then I feel like, “Okay, I feel good.”
Marsha: There’s some that say stupid things to her and just keep bringing up her CO2 (carbon dioxide) to me. Which to me, I said, “Listen, it doesn’t matter to me. It’s just a number. If she can breathe on her own, she can breathe on her own.” Okay, CO2 (carbon dioxide) isn’t perfect, but I will tell you this, Patrik. Her CO2 was high when she got put on the ventilator, this is one of the things I told the doctors. I said, “Listen, every time I told the hospital before I was able to see her, I made notes.”
Marsha: So, she was in the hospital for 15 days before she got put on the ventilator. Her x-ray was good, was bad. It got severe and then got better. And then was the same pretty much since then. So, I always said to the doctors, “Listen, if she can breathe for 12 days on that x-ray, because it never got worse from when it got better and she was 12 days not on the ventilator, why can’t she breathe now on those lungs? It’s the same x-ray. Not one of you has ever told me her x-ray got worse.”
Marsha: Matter of fact, I would read to the doctors, “You said on this day a little better, a little better. So, it’s been getting better, but then when you can’t get her off the ventilator, you want to blame her lungs. I don’t believe it.” So finally, when they went through that process and they got her off the ventilator, the doctor said to me, “I don’t see her CO2 (carbon dioxide) going down.” I said, “Give her a couple of days. Her CO2’s going to go down.” She goes, “What makes you so sure?” I said, “I think the ventilator’s keeping her CO2 up, because her CO2 was down before she got ventilators in the 40s.” Sure enough, her CO2 started to go down. It went down to the..
Patrik: Wow.
Marsha: ..upper 60s, but then..
Patrik: Wow.
Marsha: But then, this is when she was on the tracheostomy collar. But then, Patrik, this is what made them put her back on the ventilator. For some reason when she got exhausted, she was dehydrated. I think she was just compensating well because she was in good shape before. But when they did a blood gas, it was up to 100. And that’s what made them put her back on the ventilator.
Suggested links:
Patrik: She was up to 100 CO2 (carbon dioxide)?
Marsha: Yes, from 60.
Patrik: Oh okay, so I..
Marsha: So that’s what made them put her back on the ventilator. But they always bring up to me her CO2 (carbon dioxide) like, “Oh, her CO2’s (carbon dioxide) a problem. I don’t know if she’s even going to be able to get off the ventilator.” And I said, “Why? It’d be fine in the 60s. She’d be able to live with oxygen.” So, they bring that up to me a lot, her CO2 (carbon dioxide), and as a reason for her not being able to get off the ventilator.
Patrik: And I possibly agree with that. One question before we talk more about CO2 (carbon dioxide). Is she having arterial blood gases?
Marsha: Yeah, not all the time. Her last one, she was in the 50s, but she was on the ventilator.
Patrik: Right. How long ago was that?
Marsha: The 16th, the day she had a rough day.
Patrik: Right. When your sister is off the ventilator, would you say she’s getting a little bit drowsy?
Marsha: No, not really. When she’s off the ventilator, well, that time. She was more, if anything, at the end, it would be the opposite.
Patrik: Okay, the reason..
Marsha: A little weird.
Patrik: Okay. The reason I’m asking this, it’s simply that high CO2 (Carbon dioxide) can make people drowsy.
Marsha: Right.
Patrik: It could get them confused. That’s why I’m asking.
Marsha: So, okay, yeah, that’s one of the things they’re worried about and that’s why I said, “No, it’s the drug. It isn’t the CO2 (carbon dioxide),” but the drug.
Patrik: Yeah.
Marsha: I said, “Take her off the drug.”
Patrik: Yeah. It could be a combination. Prior to hospital, your sister was not suffering from sleep apnea.
Marsha: No, not that she knows of.
Patrik: Yeah, okay. No, no. Because I’m wondering, where does her high CO2 (carbon dioxide) come from? Is there something that’s potentially not diagnosed? Or is it a part of her current condition?
Suggested links:
Marsha: So, people who have sleep apnea have high CO2 (carbon dioxide)?
Patrik: Most likely, yes. Yes, most likely.
Marsha: Okay. When you say high, at a range, how high would you put it?
Patrik: Possibly, a normal CO2 (carbon dioxide) is between 35 and 45. So, 60 is in the higher range and I have seen..
Marsha: Right.
Patrik: Unless they’re asthmatic or have sleep apnea, it’s too high. Because people with sleep apnea or asthma or COPD have a higher threshold for CO2 (carbon dioxide). So, for a healthy person, a CO2 of 60 might get them confused. For a person with asthma or COPD or sleep apnea, CO2 of 60 is normal.
Marsha: Okay. Now, there’s a chance she has asthma or COPD, and it’s undiagnosed?
Patrik: Yeah, sure. They would’ve probably diagnosed the asthma as part of this, but they may not have diagnosed the sleep apnea.
Marsha: Okay. That’s what they say a lot of the time. I picked up asthma after October 13th. It doesn’t even affect me. They just picked it up on a breathing test.
Patrik: Sure.
Marsha: So, it doesn’t really affect me. It used to affect me a little bit more when I was on the fire department. When I would breathe in some smoke, you could feel it. But it doesn’t really even affect me, but I do have it. And I never had it before. They picked it up on a, it’s like a breathing test. So, they picked it up, it’s there. I used to use the medication a lot more than I do now. Very rarely do I even use it. I won’t react when I get in smoke or an odor. So, she may have it too, but she just kept herself in such great shape that, honestly, she may not have even noticed it.
Patrik: Yeah.
Marsha: But how much of the CO2 (carbon dioxide) should I worry about? She’s 54 years old. Honestly, a 54-year-old lady in that shape can honestly be stuck on a ventilator from COVID? I know it could happen, but I don’t see how she wouldn’t get off. I’m not saying she’ll be back to her 100%. Trust me, I thought she was going to die a couple of times. They were arguing with the doctor, but just to see that she went for 12 days like that and see what you said, the conditioning? I felt that, too.
Recommended:
Marsha: I said, “Hey, you have to get yourself into shape. The better shape you’re in, the better you’re going to handle it.” So, I just think there’s so much room for improvement with the conditioning that I just think she’d get off. I just think she needs to avoid infections, no setbacks. She needs the right group of people. And that’s why, after reading your blog, watching your videos, I said, “She really needs to go home. I would rather take it off.” But if she does and they throw her out, I got to bring her home. No matter how much it costs me, I have to do it.
Patrik: Yeah., I know. I get that. I think what you are describing here, there’s nothing out of the ordinary. I am worried about the high CO2 (carbon dioxide).
Marsha: Okay. So now, what should I be looking for in the CO2 (carbon dioxide)? I asked them if they can do a blood test. They said, “We don’t do it all the time. We do it once in a while.” They said there wasn’t a need to do it.
Patrik: Well, it sounds to me like your sister is not confused and she’s not drowsy. That’s what it sounds like to me, so hopefully her CO2 (carbon dioxide) is within a normal range. But again, maybe she’s got a high threshold. We don’t know. The bottom line is this. In the ideal world, they should do a blood gas while she’s on the ventilator, and then they should do a blood gas when she’s on the tracheostomy collar to make a comparison.
Marsha: Right.
Patrik: That would be the ideal scenario, but then it’s also very painful doing a blood gas. Very, very painful.
Recommended:
Marsha: Right, I know.
Patrik: Right. So, there’s..
Marsha: I know.
Patrik: There’s pros and cons to doing a blood gas, but it comes back to mobilization. I also argue that, if she’s getting morphine or fentanyl, that increases the chances of her having a high CO2 (carbon dioxide). Because again morphine, fentanyl, main side effect is respiratory depression.
Marsha: Okay.
Marsha: Okay. Given the option, I should tell them, “No, she should do without,” but she still needs the morphine for pain, because she does have a bad bedsore. That’s part of the problem. She doesn’t move because of that bedsore.
Patrik: Yeah, sure.
Marsha: And so, to me, I’m trying to follow this line where, okay, I don’t want her to be in pain. But I know she’s got to move, so it’s like you walk this tightrope. And also, I have to be honest with you, Patrik, but if it was me, I told my husband, “Make sure you give me all the medication you can give me. I don’t want to remember anything,”. But I know that it’s the best, I just feel terrible.
Marsha: To me, if I was medicated and I had to go through it, it’d be fine. But if I had to go through what she was going through, and I don’t know how much she’s really going to remember. She doesn’t remember a lot from last week. Even last week, she gets confused, but she remembers today and she’s of a sound mind. She understands the situation. She doesn’t understand that she might not be able to get off the ventilator, unless one of those people told her, which I’d never tell her that. I wouldn’t even broach the subject, but I just think give the girl some medication. But now, if it’s going to hamper her from getting off the ventilator, then I don’t want it. So, you tell me what’s best if I’m given the choice.
Patrik: Well, if you can avoid morphine, fentanyl, if she can start mobilizing, I do believe that is the next best step. I think.
Marsha: Okay.
RECOMMENDED:
Patrik: I like simplicity wherever I can, and I do understand that the pressure sore might be an obstacle of her getting mobilized. But if you ask me, in the ideal world, the ideal world is mobilization, stopping morphine, fentanyl, doing breathing exercise, and doing the regular physical therapy. And again, that’s easier said than done, but that’s the recipe from my experience for success.
Marsha: Okay. She’s on pain medication. She’s not getting a lot. And so, what if they give me a choice? “Hey, the fentanyl patch or morphine? What do you think?” Because I’m pretty friendly with the doctor. One thing about this doctor, she doesn’t claim to know. She says, “I don’t know.” She’s like, “Yeah.” She’s pretty honest with me as far as she doesn’t act like she knows everything.
Patrik: Sure, sure. Look..
Marsha: So, what would be my better choice?
Patrik: The better choice, I believe, is a fentanyl patch because it’s sort of getting in slower.
Marsha: Okay.
Patrik: If you ask your sister is she in pain, you will get a yes?
Marsha: Yes. She will say the ventilator today was killing her. So then, yesterday, they cleaned it out, but that’s it. If she doesn’t have medication, when you ask her, “Dear, you’re in pain?” she just says, “My back.”. And then, she means the sore there. She means the sore on her back. Yeah, she’s a tough lady, trust me. I saw the picture. Patrik, I’m sure you saw this thing.
Patrik: Oh yeah.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!