Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
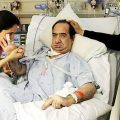
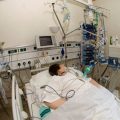
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy service! Marsha’s sister is with a tracheostomy and is on a ventilator in the ICU. Marsha is asking if her sister will ever get off the ventilator in the ICU.
Will My Sister Ever Get Off the Ventilator in the ICU?
Marsha: Hello?
Patrik: Hey, Marsha. It’s Patrik here from Intensive Care Hotline. How are you?
Marsha: All right, Patrik. How are you?
Patrik: I’m very well, thank you. Well, thank you so much for signing up for one of my options. How can I help you?
Marsha: I’d just like to get a consultation with you to go through my sister’s situation and maybe you can guide me
Patrik: Yes, of course.
Marsha: On what’s going to happen and how I should stay ahead of it.
Patrik: Yes, absolutely.
Marsha: Yeah. It’s a very odd thing. I’m having trouble understanding. The doctors and nurses aren’t consistent in the way they say things.
Patrik: Right.
RECOMMENDED:
Marsha: They go by how Noel’s doing. About a week ago, they had her go to a rehab. She was off the ventilator for 10 days, two 16-hour days, and ten 24-hour days straight, and going to a rehab. And now, this week, well, now today, she’s doing a little better, to be honest with you. But the last couple days before this, it’s, “Oh, we don’t know if she’s going to get off the ventilator. Maybe you should have a conversation with her.” So, to me, it’s crazy.
Patrik: Right. So, you were saying she was off the ventilator for 10 days straight.
Marsha: 10 days straight, 6-hour. And so, maybe I should go back a little bit, because the way it happened was funny. She seems to get very anxious at times when she would leave it.
Patrik: Yeah.
Marsha: I’m sorry, somebody texted me. Sorry, but anyhow, so they were getting her pressure down to 16, 14, like that, then they had her on 12 for a couple days. So, I had to go pick up my son from college, I was gone a couple days. When I came back, she was up to 16. I became friendly with some of them. So, I said to the respiratory therapist, “She really should be on 10 by now, the way she was going.” He goes, “I don’t know what happened. I didn’t have her, but she had a couple of rough days.”
Marsha: So, I said, “I don’t know what’s going on.” So, I go in and talk to her, and it seemed like she was all right. So, what had happened is it was almost like, I call it, an act of God. As I’m in there with the respiratory therapist, he puts her down to 14. And then, they came to change her ventilator, because the one she was on needed to be serviced.
Suggested links:
Patrik: Right.
Marsha: So, when they came to change her ventilator, I heard the one therapist say to the other, “Can we put her on a tracheostomy collar while we do this?”. The one that was treating her said, “No, no, no, she can’t go on a tracheostomy collar.” Then, I interjected and said, “Well, she’s been on a tracheostomy collar once before for about two hours.” And she said, “I didn’t know that.” I said, “Yeah, she’s been pretty good, actually.” So, I said, “You can put her on a tracheostomy collar. You’re just going to change out the, “what you may call it.” Because between me and you, Patrik, I always felt like she could get off the ventilator.
Marsha: I felt like something was just uncomfortable for her with the ventilator and with the process. So, when they put her on the tracheostomy collar, they went to switch the ventilators and it took about 15 minutes for them to get the other one out, put the other one in. When they went to plug it in, I asked them not to plug it in. I said, “Look, she’s doing pretty good. Can we let her go a little bit?” So, she went for a couple of hours. At a couple of points, she got very anxious and wanted to get back on the ventilator.
Marsha: One time, I talked her through it. The next time, the respiratory therapist talked her through it, because she actually made me nervous the second time when I said, “Oh, she might not be able to do this.” And she got 6 hours on that bed. The next day, 18 hours. The next day, 18 hours. And then, she told me on those 18 hours, she said, “Marsha, I’m done with the ventilator.” And she went 10 days, but I will let you know, she was on fentanyl. So, she had started fentanyl and that kind of kicked in, and it looked like it took the edge off for her.
Patrik: Yes, I remember you saying that.
Marsha: So now..
Patrik: Yes.
Marsha: Okay. So now, today, I was there, and I go see her every day. I spend a lot of time there, to be honest. I just want to be there, because I think it helps to see what happens, how it works.
Patrik: Of course.
Marsha: And today, she had a different respiratory therapist. She was doing 14, then she went down to 12. And then, the speech therapist came in to put a speaking valve on her, so she did a little bit of the speaking therapy. They took the speaking valve back off and she started to complain to the therapist when she reinflated the cuff, the cuff thingy, because it was very uncomfortable, very uncomfortable. So then, the therapist, for some reason, said, “You know what? Let me try something.”
So, she deflated the cuff, took her off the respirator but didn’t tell her, put her on the tracheostomy collar. And I said, “Don’t…” And she asked me, “What pressure am I on?” I said, “14.” And the therapist looked at me and I kicked her a little bit, just gave her a look, because I’m friendly with the lady. I kicked her and shook my head and told her, “Don’t tell her.” That was at about 1:00, 2:00. I left around 4:00 and my dad came after that, and now her boyfriend’s there.
Recommended:
Marsha: She’s still on the tracheostomy collar for the whole time, she’s doing pretty good. And she just texted me a copy of the monitor, and her oxygen saturation is 98, her pulse is 100. Her respiration’s around 13 and her blood pressure’s been high the last couple days, 149 over 98, her blood pressure. And she’s been on that. She’s been weaning since 8:00 this morning on 14 and then 12, and then she’s on tracheostomy collar since about 1:00 and with 40% oxygen.
Patrik: Right.
Marsha: I just don’t know. So, the doctor talked to me today. He said, “Well, maybe we’ll give her a little fentanyl to help her wean.” I don’t know exactly what I’m going to do. I told the doctor before I spoke to you. I told him, I said, “Doc,” I said, “I’m not saying don’t give her fentanyl, but…” So just to backtrack a little bit, my sister has a very low tolerance for drugs. So, when they gave her that fentanyl, they had her at 12, then at 25. Well, they put her at 37, she started to hallucinate. I probably should’ve said something to the doctor then. But, of course, her weaning was going so good, and it was harmless hallucinations. I didn’t say anything. But a couple days later, the hallucinations became where she was trying to get out of the bed and really not harmless hallucinations anymore.
Patrik: How long ago was that?
Marsha: I took all the medications off. What’s that?
Patrik: How long ago were those hallucinations?
Marsha: That was about the 11th, 12th, 13th, and 14th, and she still remains on the tracheostomy collar. She got progressively worse, and I told the doctor, “You got to take her medication. This is what happens when she’s on medication for a long time.” She doesn’t tolerate medications well. She never took drugs. She has a very low tolerance to drugs and alcohol. When she was sedated when she was on the ventilator the 3rd and 4th week, when the doctor finally took the sedation off, it took her 10 days to wake up.
Patrik: Right. I remember you saying last week that your sister has been living a very healthy lifestyle prior to this.
Marsha: Right. So now, she has no drugs. She just gets morphine through the PEG-tube (Percutaneous endoscopic gastrostomy). I guess they call it through the G, whatever, through the stomach, but she needs it every 4 hours. It was 3 mg. Now, today, they upped it to 5.
Patrik: That’s..
Marsha: She does have a big bedsore and it can be painful for her.
Patrik: Right. So that’s morphine she’s getting there?
Marsha: Yeah, morphine just through her stomach.
Patrik: 3x a day
Marsha: Morphine.
Patrik: 3x a day, how much?
Marsha: No. It was 3 mg. Now, they upped it to 5 and it’s every 4 hours when she asks for it. They don’t give it automatically. Just when she asks for it.
Patrik: Right. And how big is the dose? Do you know?
Marsha: I think it’s 3 mg, that sound right?
Patrik: Yeah. No, it sounds right. Yeah, okay, but she’s not getting fentanyl on top of that, is she?
Suggested links:
Marsha: No but the doctor just told me today. I said, “Look, Doc, I’m not telling you what to do because I don’t want to act like I’m the doctor”, I said. “But I’m telling you, if you do decide to give her medication, it’s just got to be a low dose. She’ll be fine with it if you don’t overdo it, but you can’t overdo it”. I told her, “She’s just not one of those guys.” She will never have some pain medication if she’s not in pain. I had to talk her into taking it in the beginning.
Patrik: Yeah, okay. But when you left today, she was off the ventilator still?
Marsha: Yes, on the tracheostomy collar.
Patrik: Right. And how many days between today and when was the other tracheostomy collar last time before today?
Marsha: The 13th, the 14th, the 15th. So, the 14th night, she went back on the ventilator, 14th night. Between 14th and 15th overnight. It was like 11:00 on the 14th.
Patrik: Okay. So basically, what you’re saying is today’s the 20th. So basically, what you’re saying, this is the first time she’s back on the tracheostomy collar since the 14th or 15th.
Marsha: They put her one day before. I said, “Doc, can you skip the weaning process and just put her on the tracheostomy collar? Because she doesn’t like…” because she had told me after she was all clean, after the medication was out. She said, “Marsha, I don’t like the way the ventilator feels. I’d rather do the tracheostomy collar.” So, she says, “I just don’t like when it’s on the pressure point, how it feels. I just really like the tracheostomy collar,” but now I’m figuring out, Patrik. Today, by sitting in the room and listening is, I think what she doesn’t like, I think what she likes better about the tracheostomy collar is they deflate the cuff a little bit. I think she likes that better.
Patrik: Yeah. So, deflating the cuff is a good sign. They don’t necessarily have to deflate the cuff when she’s on the tracheostomy collar, but if they’re doing that, that’s a good sign. I’ll tell you when they deflate the cuff and when they don’t deflate the cuff. If someone can’t swallow for whatever reason or if they’re worried about swallowing. If someone had a stroke, for example, or a neurological condition, you’re not deflating the cuff straightaway, because you need to ensure that people can swallow. Because otherwise, if they can’t swallow and they deflate the cuff, they might end up with an aspiration pneumonia. So, if they’re deflating the cuff, they must feel confident that she, (A) can swallow, (B) can cough up her secretions. Have you seen her coughing up her secretions?
Recommended:
Marsha: Yeah. Well, honestly, I suction them all the time when I’m there. I had to teach myself how to suction them, of course. But I will tell you, she overdoes it sometimes. Where sometimes she gets..
Patrik: She overdoes it? Yeah, sure.
Marsha: Yeah.
Patrik: Sure.
Marsha: Because there’s a lot of things. And she just gets caught up on the one piece of phlegm that she can’t get out. So sometimes, yes, she overdoes it. So yes, she does cough up a lot of blood now, but especially in the beginning. As you know, when you go on the ventilator and go on the cuff, the collar, that she was back at it. She was throwing up in that jar the stuff that was coming out. This is just me being a layperson and watching her, but when I saw the first time she was on the collar, that all that phlegm was coming up. I’m thinking in my head, one, that can’t be good to have that in there.
Marsha: And two is for her to be coughing like that to me, a layperson, it’s waking her lungs up to function again, where the other way, her lungs don’t get the function. So that’s why I was thinking, even though we only made it to down to 16 or 14, I felt, as a layperson looking at this, I felt that, if she was on the cuff, it would speed up her lung recovery. I just felt that. I feel sidelined, but I just felt like, you know.
Patrik: Yeah, okay.
Marsha: So, she does cough up a lot, less now, but still.
Suggested links:
Patrik: Okay. Few questions here, Marsha, and you’re right. The research paper and medical evidence suggests get someone on the tracheostomy collar, if they’re down to a pressure support of 10 or 8, and a PEEP (Positive End Expiratory Pressure) of 5, that’s sort of what the research and practice suggests. But you know your sister and I think it’s a good idea for you to follow your gut there. Here is another question. Is she getting mobilized? Is she getting out of bed?
Marsha: That’s a tough one. See, this is where the drugs affect her sometimes when she’s on it or she gets a little moody. Usually, she’s not herself, obviously. And I try to tell her, “Hey, you have to get up,” because I think I told you my husband’s a nurse, and he tells me, “Laying there is no good.”
Patrik: Exactly.
Marsha: Right, but she has this bedsore, and she can’t stand up straight. And she can’t even sit up straight, she’s not strong enough yet. So, they put her in a recliner, a semi-reclined position, and that really bothers her bedsore. She’s got a bedsore right at the bottom of her coccyx bone, I guess it is.
Patrik: How often?
Marsha: And so, that’s why the..
Patrik: How often is she getting in the recliner?
Marsha: Well, I like to get her in often. On the 16th, her blood pressure dropped. And between me and you, she looked like to me she almost died. I think she was pretty close, actually. I think that was a result of she had an infection that they didn’t know about.
Patrik: Right.
Marsha: To tell you that part.
Patrik: So..
RECOMMENDED:
Marsha: So, I think they were a little reluctant to get her off. So now, I said to them, “Hey, I’d really like you to get her off this. And when the doctor tells us we can get her off, we will,” I said. But they are doing exercises with her.
Patrik: How many days has she been in that recliner chair, and how long, every day, or just a couple of times?
Marsha: No, just I would say when she’s rolling good. It’s every two or three days a week when she’s rolling good. But what I noticed, Patrik, is these Physical therapy people. They stroll by the room, “Oh, she’s weaning? Oh, you’re changing her bandage? Okay, we’ll come back.”
Patrik: Yeah, yeah, sure.
Marsha: Sometimes, I’m there all day and they never come back.
Patrik: Yeah, yeah. I get that, I get that. Look, from my experience, Marsha. Getting in a recliner chair is very good. And I argue that you can’t come off a ventilator without getting mobilized.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!