Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
10 Things About ECMO You Didn’t Know in Intensive Care! (COVID and Non-COVID Related)! Live Stream!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy service! Marsha’s sister is with a tracheostomy and is on a ventilator in the ICU. Marsha is asking why the doctors are pushing her sister to go to a rehabilitation unit.
My Sister is with a Tracheostomy in ICU & Why Are the Doctors Pushing Her Out to a Rehabilitation Unit?
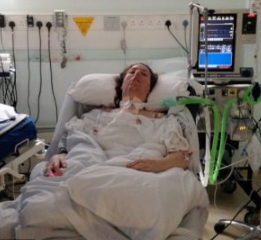
“You can also check out previous 1:1 consulting and advocacy sessions with me and Marsha here.”
Marsha: Hi Patrik!
Patrik: Hi Marsha! How’s your sister doing now? From memory, Marsha, last year she did go somewhere else as well, didn’t she? And then she bounced back to the hospital, from memory?
Marsha: Yeah. So she was in a couple of hospitals, then she went to an LTAC. She was in the LTAC for like a month. And she was off the ventilator for two 16-hour days and then 10 days straight. Her tracheostomy was capped, she was on nasal cannula, and then she had to go back on the ventilator. And what they found out was that she had bleeding in her stomach, she had an infection, she was dehydrated. And so she got transferred from the LTAC to this facility, which is a very good hospital.
RECOMMENDED:
Patrik: Yes. Right.
Marsha: And, but it was awful.
Patrik: Go ahead.
Marsha: There was lots of bleeding. They had to take out her feeding tube, wait 5 days, take out a piece of her stomach, put the feeding tube back in. Then they took her gallbladder out, then they addressed… I think it is her infection, as well.
Patrik: Well.
Recommended:
- My 72 year old Mum’s been in ICU for 6 weeks after stroke,tracheostomy & ventilated,can she go home?
Marsha: She got a couple of procedures on her bedsore, which is pretty bad, and now they’ve put a skin graft on it. So that was the last thing she had, and pretty much she’s stabilized now, she’s doing well. The last couple weeks she was coming off the ventilator during the day for like 14 hours and then going back on at night, and I thought I was going to have to call you when it was time for them to move her back to the LTAC. But they didn’t even tell me that they put in for the insurance company to move her back to the LTAC, and the insurance company denied that. Did me a favour, actually, and said, “No. It looks like she can get off the ventilator. Just wait till she’s off the ventilator there, and then you can transfer her to a rehab.”
So I thought I was going to have to call you for that one, but the funny thing is they never called me. Her insurance, so actually they never called me when they put in for the LTAC, and she got denied from the insurance company, who then said, “Stay there.” Which is what you wanted. You said you wanted her to stay there to wean off. But then they started to do the… So, well, last time I spoke to you I started doing physical therapy with her, the exercises the physical therapist showed me a month ago in the other place.
Patrik: Yeah.
Marsha: I was going and doing the exercises with her, when she was in the mood to do them. I’d try to push her. Sometimes I’d get her to do them, sometimes I wouldn’t. But that physical therapist never even came by her room until the insurance company told them, “Hey, we want her to wean off that.” Then the physical therapist showed up, and the occupational therapist. So the physical therapist comes every other day maybe, and the occupational therapist comes every other day, so between the two of them she probably gets one of them once a day. And she does comply, from what I know, with the exercises. But she’s stronger than she was, but she can’t sit up in the bed. She moves herself in the bed pretty good when she has to, like she grabs onto the side rails and she can move herself. But she can’t stand up, she can’t sit up. She can hold her head a lot better. So I think she really just needs the rehab, and the quicker she gets off the machine the better it’d be.
Patrik: Right.
Marsha: So now, but 48 hours after that then she put in to the rehabs. Now, I did talk to a social worker since I texted you and she said, “Well, the rehab that I put in to didn’t take her insurance, so it may be longer than I thought.” So when I had texted you, they told me she was going to be transferred tomorrow, which was new to me.
Patrik: Right.
Marsha: So now it seems like they have to find someone that takes her insurance.
Patrik: Right. Will she get..
Marsha: But I wanted your input on that.
Patrik: Yes. A few questions there, Marsha. Will she get physical therapy at the subacute?
Marsha: Yes. That’s what it is, rehab, yeah.
Patrik: Right. Have you..
Marsha: I think that’s what she gets. I’m assuming that’s..
Patrik: No, not necessarily. That’s why I think it’s valuable to have the discussion. So sometimes when people go to LTAC, and they’re sort of not succeeding at the LTAC, the next step then for them is to go to a subacute. And a subacute is usually a step lower than an LTAC, so that’s why I’m concerned. Have you looked into this subacute facility? Have you gone to the website there, have you spoken to anyone?
Marsha: No. She gave me a list. She gave me a couple of them, and she said… And the one request I did have, I said, “I want her to go to a place that’s near this hospital, because if she has a problem in the subacute rehab I want her to come back here.” Because it actually is a pretty good hospital, especially for the area she’s in. But, so she said, “Okay,” and she gave me some. And the one I picked was the one that wasn’t connected to a nursing home.
Patrik: Yup. Yeah, good point.
Recommended:
- CAN INTENSIVE CARE AT HOME TRAIN FAMILIES TO LOOK AFTER LOVED ONES ON A VENTILATOR and TRACHEOSTOMY?
Marsha: So I did it. Yeah, so I said, “You know what? I’ll take that one.” It was close to the hospital. And she actually… Well, I was saying because it’s not connected to a nursing home. And she agreed with that, but then today she told me otherwise.
Patrik: Right.
Marsha: But I assumed that’s why you go. See, I shouldn’t assume anything. And I assumed that that’s what a subacute rehab is, more concentration on physical therapy, isn’t it?
Patrik: Yeah. That’s what they’re trying to sell you, of course. That’s what they’re trying to sell you, because otherwise you would have second thoughts. Unfortunately, I’m very wary of what they’re trying to tell you so you are agreeable to get her wherever they want her to go.
Marsha: Right.
Patrik: But I believe it’s critical for you to speak to one of those facilities, to more or less get it from the horse’s mouth. Or, I’ll tell you what problem that I have with the timeframes particularly. When did you first find out when she was going?
Marsha: My dad went up to see her today and said, “Hey, the nurse said she’s getting transferred tomorrow to a rehab.”
Patrik: So basically, you’ve only found out in the last 24 hours.
Marsha: Right, and that’s why I said. Well, there’s no… Oh, okay. So a couple days later, she… No, a couple days prior to that when they were starting to wean her off the ventilator, they said to me, “So after 48 hours off the ventilator, we’re going to try to place her in a subacute rehab.”
Patrik: Sure.
Marsha: Isn’t that right? And I said it sounded like to me… I said, “That seems a little quick.” If you observe her for 48 hours it doesn’t mean that they’re going 48 hours. But after she’s off the ventilator, since she’s been off it before, “Once she’s off it for 48 hours that’s it. We’ll start to try to place her.”
Suggested links:
Patrik: As I said, the problem that I have is that it sounds to me like they’ve selected the place for you, and I do believe you need to know where she’s going. And my question would be, do those places get results? Do they have good testimonials? And the list goes on. I believe that giving you 24 hours’ notice for what they… I mean, they do that all the time, we know that. But for you and for your family, this is a big deal.
Marsha: So when they send her to a subacute rehab, I just thought it was physical therapy at least once a day, as opposed to 2 to 3 x a day in acute rehab. And that’s what their job is, to get her back in shape so she can walk, go back to work and all, and move. So what do I have? I mean, the thing is, nothing’s on the level. It’s just a maze to me. So what could happen if she went to one of these places? Tell me what you’re worried about.
Patrik: Yup. Yeah. Well, I’ll tell you what. At the moment, as of today, where is she? Is she still in an ICU, or in a step-down ICU?
Marsha: Actually, she was never in the ICU in this hospital. She hasn’t been in the ICU in a couple months, since before the LTAC. And she’s in a cardiac care unit because they support ventilated patients there. But that one isn’t an ICU, yeah.
Patrik: They support what?
Marsha: Ventilated patients. The patients on the ventilators.
Patrik: Oh, ventilators.
Marsha: In terms of, I mean, it’s mostly a cardiac unit. There are some people on ventilators, but they’re mostly cardiac related. But I would not call it a… it is not an ICU.
Patrik: Yeah, okay. But she doesn’t..
Marsha: Although I think they have..
Patrik: Right. But she doesn’t have a cardiac issue, does she?
Marsha: No. She has some damage from COVID, but she’s not there for that. They just mentioned that. It’s in that workup I mentioned, it listed that she had some… I think they call it myopathy, which I don’t know what that means. I guess a little heart damage.
Suggested links:
Patrik: Oh, she does have cardiomyopathy?
Marsha: Yeah, a little bit. A very little bit.
Patrik: Right. Do you know… Sorry, I don’t want to digress. Do you know her ejection fraction? Have you heard of that?
Marsha: No. No.
Patrik: Might be..
Marsha: Maybe I’m wrong. Maybe I’m wrong about the myopathy. Maybe they suspected myopathy, and they just said that she has a little bit of heart damage. So I don’t know if it was myopathy. What is myopathy?
Patrik: Cardiomyopathy is a weakness of the heart muscle. If you have a weakness of the heart muscle or cardiomyopathy, the heart can’t contract to its full extent, okay? And in order to determine the extent of the weakness, it can be simply done by an ultrasound. I’ll text you a question that you should be asking them. It’s basically have they done an ultrasound of the heart, and what is her ejection fraction? I think that’s a very important question, and if they say, “No, that’s all good,” I think that would be great. But I think I’m a bit wary. Why is she in a cardiac unit?
Marsha: They told me, well, that… But, yeah. No, she was in there from the beginning, and they told me the reason. I asked that. They told me, “No, no, no. Because she’s on a ventilator and she’s really not ICU.”
Patrik: Yeah.
Recommended:
Marsha: So she said, “This is a unit that we have that’ll support a ventilated patient, so that’s where we put our ventilated patients that are not in the ICU.” But they suspected cardiomyopathy, and they did do an echocardiogram. They came in and did that, I think. So, they did. And they didn’t tell me the results, they told her, but they told her he has a little… I think they used the words, “You have a slight heart damage. It’s not a big deal.” And the cardiologist told her, “When you get discharged and you get on your feet, come and see me and I’ll tell you what you need to look out for and whatever.”
Patrik: Right. But coming back to your original question, what’s the next step and should she be going, I’m wary of a few things here. And every time… We’re having so many inquiries where people say, “Look, my family member left for LTAC or they left for a subacute, and it’s just bad,” And what’s the nurse-to-patient ratio at the moment? Is it a one in..
Marsha: I would say if I has to guess, it’s 4:1.
Patrik: 4:1? Okay.
Marsha: That’s what, if I had to guess the patient ratio to the nurses.
Patrik: Yeah, sure.
Marsha: Because it’s been up there, and it looks like she has about 4 patients to 1 nurse.
Patrik: Okay. And do you feel like the nurses are competent?
Marsha: They’re very good.
Patrik: Okay, good. That’s good.
Marsha: This is probably one of the better hospitals she’s been in. Except that ICU, when she was in an ICU before? That was pretty good. The step-down unit there compared to this? I’ll take this.
Patrik: Okay, fair enough. That’s good to know. And how often are they doing physical therapy at the moment?
Marsha: Well, so after speaking to you I started her moving, and exercises. But when I watch… See, I used to do it with her all the time in the LTAC, and I watched her physical therapist doing them and the physical therapist told me, “Hey, I’m going to show you the exercises so you can do them with her.” So I do all those exercises with her, like four upper body ones and four lower body ones. But it’s basic, very basic exercises. And they weren’t..
Patrik: Yeah. Right, but you are doing it.
RECOMMENDED:
Marsha: Yes, they weren’t coming in at all. But when they denied her from leaving the hospital, the insurance company, then suddenly, they wanted to. The physical therapist was contacting me, the hospital was contacting me and saying, “Hey, she’s denied.” It was like one day, the first day she came in, I guess she misunderstood them, or I guess she didn’t feel like doing it and she said, “My sister does the exercises with me.” So, they called me and I said, “No, no, no, no. I’m going to talk to her.” So I went there and I said, “Hey, when they come in make sure you do the exercises with them. I’ll come later, and if they don’t do them, I’ll do them with you.” Then I hung a note in her room basically saying, “She should do the exercises, and if she gives you a problem call me. I’m her sister.” My husband is a nurse. He wrote the note. So I hung it behind her head so she couldn’t even see it.
Patrik: Right.
Marsha: And when I go and I ask her, “Hey, did they come in?” And so yesterday… Yesterday they didn’t come in when I was there to see her, but they were in the day before, I think. So, I think it’s like every other day.
Patrik: Right.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!