Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Why is the ICU Team in a Hurry to Transfer My Ventilated Sister with a Tracheostomy to LTAC?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy service! Marsha’s sister is with a tracheostomy and is on a ventilator in the ICU. Marsha is asking if it is safe for her sister with a tracheostomy to transfer from ICU to LTAC.
Is it Safe for My Sister with a Tracheostomy if We Transfer her from ICU to LTAC?
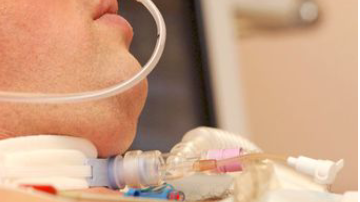
“You can also check out previous 1:1 consulting and advocacy sessions with me and Marsha here.”
Marsha: And then one day, without telling me, they transferred her and then called me up and just called me, “Hey, we transferred her to a step-down unit.” So I didn’t fight them on that. I didn’t think it was a big deal. But then when I got to the unit, I saw that it made her uncomfortable. I was dragging my feet with the LTAC and I was going a good job of doing it, because the insurance doesn’t cover a lot of LTACs where she was going, so I was able to really drag my feet. But then she got frustrated and she said, “Marsha, I want to go to the LTAC.”
Patrik: Right.
RECOMMENDED:
Marsha: So she pushed me, and this is before. And as that all was going on and right after, or right before she was getting transferred, her lifestyle changed. I was like, “Well, I think I don’t like LTACs. Maybe I messed up. I should’ve…” But then it was pretty much too late. I already agreed to it. She already wanted to go. Even if I had told her about it, she would’ve said, “No, I don’t care.” So the step-down unit wasn’t good. The room was very tight. She wasn’t getting weaned off the ventilator, that attachment. They did a worse job than the LTAC weaning her off, but not… The ICU did the best job of weaning her off, but the step-down actually messed the whole thing up.
Patrik: Sure.
Marsha: Set her back a little bit. And basically what they did was, they were telling her too much. And then I told them, “Listen.” I started realizing all of a sudden she was only off the ventilator for like 20 minutes, when she’d be off the ventilator… When she’d be on CPAP, not off the ventilator but on CPAP, for hours when she was in the ICU when I was with her and she wouldn’t even know it. She was only off for 20 minutes.
And I figured it out after a week or two. I’m like, “You guys are telling her?” And they’re like, “Yeah, she’s with it, so we tell her.” I said, “First of all, she doesn’t really understand what you’re telling her. She’s with it, but…” And I said, “You’re making her nervous.” So I told the doctors, “Do me a favor. Don’t tell her. Just do it and lie to her, and when she says, ‘Did you put me on CPAP?’ Tell her, ‘No.'” And that’s what they would do, and she would run for like 7 0r 8 hours. It was like, “Oh, okay.” But they just weren’t good at weaning her off in the step-down unit, where I think in the LTAC they were definitely better at it.
Patrik: Right.
Marsha: And more listening to what I was saying. Now, I was there a lot. I was there all the time, more than probably any other patient’s family. I would be there all day, and so I became friendly with them, and I know how to talk to people. Certain people, there’s certain ways how to interact. Some people want to let you know that they’re the boss and they’re in charge, and that’s fine. It takes time to talk to them. But, basically they would listen to me. The doctor was very good, and she would listen to me.
I even told her at some point, “Listen, she’s never going to get down to 10 because when you guys put her on CPAP she knows it and she feels it. She feels like the tracheostomy collar is way more comfortable.” And so I got them to take her off the ventilator and put her right on the tracheostomy collar when she wasn’t down on 10 at her pressure, she was only at 13 or 15. And it worked. And I just knew from talking to her, she just didn’t like the feeling of the pressure support. And it turned out she didn’t like the cuff, either. So I guess the cuff that they have in her throat, when they put you on the tracheostomy collar they deflate that. So she feels that’s way more comfortable.
Patrik: Yeah, correct.
Recommended:
Marsha: But it took time for me asking her questions, like, “Why? Why? Explain that. Explain that.” And they would put her back on the ventilator, or they would put her back on full support and say, “Well, she was struggling. She was uncomfortable.” But meanwhile, she was trying to say that collar was bothering her. So they didn’t get that part of it right. It’s just so crazy, Patrik, how easy they can just say, “Okay, put her back on the ventilator,” and then walk out of the room like nothing.
Patrik: Oh, yeah. For sure.
Marsha: And I’m just like, “What’s going on?” There’s a lot of people on ventilators out there that don’t have to be on them, I think, that really with some work from the respiratory therapists and the doctors they could really get them off, and from the physical therapists as well.
Patrik: Oh, absolutely.
Marsha: It’s terrible, Patrik. This has just been such an eye-opener for me, that not only does it depress me by the situation my sister’s in, but it depresses me like, what’s going on? I’m 53 years old, I just discovered this? This is crazy. It’s so bad, it’s just so bad. And now, I just learned this, and then I just assume that the social worker and the doctor have my sister’s best interests in mind. And of course I get woken up by you, which you’re right, saying, “Hey.” Because it didn’t seem right to me. It’s like, that’s quick. That’s like… I said, “Hey, that’s quick.” I thought they were going to tell me, “Okay here’s your list. This is the ones we put in for. This is where she got accepted. Tell me which one you want.” And I would say, “Okay, I’m going to go visit them. Give me a couple of days.” And then I was going to call you and say, “Patrik, is this the right move? What should I do now?”
Patrik: Right. Well, I..
Marsha: But I didn’t think they were going to call. I thought they were going to put in, and then it would be a week before they’d even say, “Okay, these people accepted her.” Because that’s what happened with the LTAC. It took like a week or two.
Patrik: Yeah. Okay. Here is another thing, Marsha. So from what I’m hearing, you’re quite comfortable there at the moment overall with what she is getting. Is that fair to say?
Marsha: Yeah. I just think she needs more physical therapy. And she just recovered from bacterial pneumonia, and I see that she gets an infection like every month. So I did want to send her to a place that’s going to give her good rehabilitation and get her moving.
Patrik: Yeah. No. Understood. And once she’s going there, she needs a new team, but you almost need to know who that team is. That’s why I think you need a little bit of time to talk to people.
Marsha: Now, should I be pushing for acute rehab instead of subacute?
Patrik: Say again?
Marsha: Should I be pushing for acute rehab instead of subacute?
Suggested links:
Patrik: Potentially. I think that might be a step above, and again, that’s why I think it’s so important to do all your research and it’s important.
Marsha: Between you and I, I thought it would be too challenging for me. I mean, I was just thinking of physical therapy, it’s going to be too challenging for me. And I was worried about, if I got overwhelmed, that that might push her back onto the ventilator.
Patrik: Yeah, look, I think physical therapy is inevitable. It’s inevitable. You know what I’ll do, Marsha? I’ll send you a link to an interview that I’ve done quite a few years ago. There was a guy and he was in his 80s at the time. He spent about a year in the ICU, and in LTAC. He describes the process of physical therapy quite well in that interview, and it’s a really… If someone can do it who was in their 80s at the time, I’m sure your brother can do it. But it’s a really good interview because this guy really describes the process, how important physical therapy was for him. And without it, he probably wouldn’t have survived and he would still be stuck on a ventilator. He was on a ventilator for 12 months.
Marsha: Oh, no, but I agree with that. But, Patrik, maybe I’m wrong. Isn’t that the concentration when she goes to a rehab? Isn’t that what it is, the physical therapy?
Patrik: Yeah. It is, Marsha. But why am I not jumping on this? I’m not jumping on it because, yes, that’s their sales pitch. That’s their sales pitch, but from what I’m seeing it’s just not happening.
Marsha: Oh, so you’re saying people are going to these subacute rehabs and they’re not getting physical therapy?
Patrik: Correct. That’s the sales pitch to get you out of ICU, or wherever she is now. That’s the sales pitch, but I’m not seeing it in practice.
Marsha: Okay. So, now, if that doesn’t happen, I’m going to go there and raise…
Patrik: But, Marsha, but this is why I’m saying you need to talk to them. You need to talk to those facilities, to make sure that what they’re promising you is what you’re going to get.
Marsha: Okay. Now, what happens if I push for acute rehab but then it’s too much for her? Then what?
Patrik: I don’t think it’s too much. I think it’ll be too little, no more where she goes.
Marsha: Really?
Recommended:
Patrik: Yeah. It’s not what I’m seeing, Marsha. It’s just not what I’m seeing.
Marsha: All right. Anyway, so I should push for an acute rehabilitation?
Patrik: You should, but you should do your research and see where there’s good reviews. Ask them, “Hey, can I talk to a couple of families that you’ve looked after?” And if they deny that, that should be a no-go for you.
Marsha: Okay. So now, this rehabilitation center is well-known. I mean, I think they’re well-known.
Patrik: Right.
Marsha: Have you heard of them?
Patrik: No, I haven’t heard of them.
Marsha: Okay. So it is well known and I actually know two friends that were in terrible shape, and they both went and had their therapy there. One got hit by a bus when she was on a bike and she had like 60 surgeries, and she walks with a limp today. And another guy jumped out of a window, and she had an internal decapitation. When I saw her come out of the hospital, I said, “This lady’s never going to walk again.” But I mean, she did pretty well, and she went to this rehabilitation unit.
Patrik: Okay, good.
Marsha: So, they denied my sister last time. They denied her last time, but how do I get them to take her?
Patrik: Ask. You’ve got to start talking to them and give them your sister’s situation. Start talking to them. It’s probably not as simple as, “I’m going to call them up and ask for a placement,” and you’ll get it. It’s probably more of a case of one step by step. But that’s why you need to buy time there, to find the right place.
Marsha: Okay. So the first thing that I’ll do is call the social worker and tell her, “When you find facilities that take my sister’s insurance, I want to have an opportunity to research them and go visit them.”
Recommended:
Patrik: Absolutely.
Marsha: Okay.
Patrik: And, again, there is absolutely nothing unreasonable in that.
Marsha: Right. And then I’m going to tell her I also want to have time after I research them and visit them.
Patrik: Absolutely.
Marsha: And I want to talk to her insurance carrier to make sure that she’s going to have… That that’s going to be covered.
Patrik: Yup, absolutely.
Marsha: Because there might be some insurance issues. I don’t want that, with the insurance issues.
Patrik: Exactly.
Marsha: And I’ll tell them, “I wasn’t given an opportunity to research the LTAC.” Between me and you, that is a lie, which I don’t mind lying to them.
Patrik: They’re lying.
Marsha: But..
Patrik: Yeah. I think they’re probably lying to you, not that I’m saying.
Marsha: Oh, no. I have no problem doing it. Listen, and Patrik, I won’t lie to you, but I have no problem lying to them.
Patrik: Yeah, sure.
Marsha: I didn’t research it for that, and we weren’t happy with the results, so I just want to make sure I don’t make the same mistake.
Patrik: Yeah. No, absolutely. Marsha, I need to..
Marsha: Okay Patrik, and I’ll tell you right now, the social worker, he’s not that… Most of these social workers are not nice, and they’re not too bright. I hate to say it. They’re not the smartest.
Patrik: Right.
Marsha: And they want to act like they’re smarter than they are, so they’re not nice. So, those people I have the hardest time.
Patrik: Right.
Marsha: I have to bite my tongue. One time I did, when I said… Well, actually, I had a fight with one of the social workers, but he clearly didn’t listen. And I told them, I said, “Listen, I’m letting you know right now that LTAC doesn’t take my sister’s insurance. I picked this LTAC. You’re trying to send her to that LTAC. They don’t take my sister’s insurance.” So he says to me, “No, they do. I have it here.” I said, “No.” I said, “That LTAC that you have, I guarantee you, has an address in this place.” She goes, “Yeah.” I said, “The LTAC that she would go to is in another location. The one in the other city. Just call up and ask.” He refused to do it.
Patrik: Right.
Suggested links:
Marsha: So I called the person from the LTAC and she said to me… And I became friendly with her. That’s not where she went. That’s where I would send her now if they forced me. And I said… her name was Chloe. I told her, “Chloe, you know you don’t take the insurance.” So she goes, “Well, Marsha, they’re telling me I do.” I said, “But, you know you don’t. And I just want to let you know.”
Patrik: Right, Marsha? Sorry. Very sorry to interrupt, Marsha. I need to go in 2 minutes. I’m terribly sorry to interrupt you there in your flow, but I need to go in 2 minutes. I’m very happy to call you back in about 45 minutes, but I..
Marsha: No. It’s no problem. I was irrelevant anyway. I was just trying to show you, for you, and with these LTACs so you could see what goes on. And that was a story that, to me, was just they’re being disingenuous. She knew she didn’t take the coverage, but she was going to let the paperwork all go through and hope that I would just say, “Okay, send her there because the paperwork went through.”
Patrik: Right.
Marsha: But, so that’s what I’ll do. I’ll call him, and then I’ll call the doctor. What should I tell the doctor?
Patrik: Similar. Not any different.
Marsha: Okay.
Patrik: Not any different. Stick with the same approach, and that approach is very reasonable. There is nothing unreasonable in that approach.
Marsha: Okay, perfect. You should get back to me, Patrik.
Patrik: All right.
RECOMMENDED:
Marsha: So when I get a chance today about what I should be expecting, and what’s the next step. Because I don’t want to keep her here, because the physical therapy is not good. So I don’t know if I should keep it active, because the physical therapy is not good.
Patrik: Yeah. No, I get that. Marsha, I’m so sorry, I really need to go now. Happy to call you back in about 45 minutes.
Marsha: Okay. No.. I’ll just get back to you.
Patrik: Yeah, please.
Marsha: No, problem. I’ll just get back to you.
Patrik: Thank you. Thank you. Bye.
Marsha: Thanks.
Patrik: Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







