Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Mother Had a Cardiac Arrest and is Still in a Coma. Help!
You can check out last week’s question by clicking on the link here.
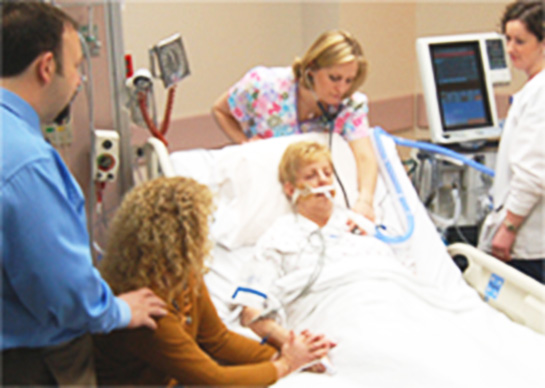
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Stephanie as part of my 1:1 consulting and advocacy service! Stephanie’s mom is a post cardiac arrest patient in the ICU, doing a lot of eye blinking now and she’s asking if it means that her mom is more awake now.
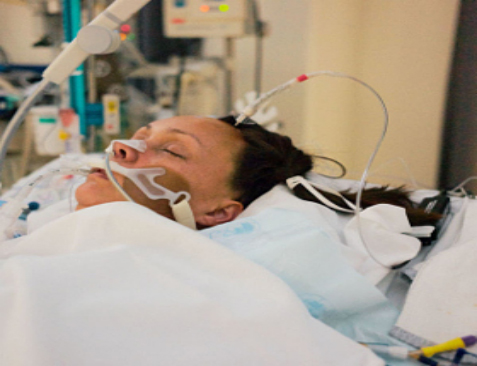
My Mother Had a Cardiac Arrest in the ICU Doing a Lot of Eye Blinking Now. Will She Be More Awake Soon?
Stephanie: Hello?
Patrik: Hi Stephanie. Sorry, before I tried to dial her in, I pressed the wrong button so just give me one second and I’ll try and dial Miranda in.
Stephanie: No problem. Miranda. Okay.
Patrik: Just give me one sec.
Miranda: Hello?
Patrik: Hi Miranda. It’s Patrik here from Intensivecarehotline. How are you?
Miranda: I’m okay.
Patrik: So I’m just bringing…
Miranda: Hello?
Patrik: Hello, bringing Stephanie in. Miranda, can you hear me?
Miranda: I can hear you but my answering phone is old. Something is going on.
Patrik: Right. Stephanie?
Recommended:
Stephanie: I’m right here. Can you hear me? Can you hear me too?
Patrik: Right. I can hear you. Wonderful.
Stephanie: Can you hear me also, Miranda?
Miranda: Yes.
Stephanie: Okay. Good. Everything’s fine.
Patrik: So, it sounds like the meeting…
Stephanie: You want an update on the meeting? He wants an update on the meeting Miranda. And I’m here with you.
Patrik: It sounds like the meeting went fairly well and again I do apologise Miranda that I wasn’t there. I simply didn’t wake up when Stephanie called me. It was 1 am for me. No excuse. It sounds to me like you had it under control. The trach is going to be done. The GCS is higher than when we spoke to them last night. Which is all good.
Stephanie: What is a GCS?
Patrik: GCS. Glasgow Coma Scale. Sorry.
Stephanie: Oh yes, yes, yes.
Patrik: Right. Then the next step is really once you have the trach, you still need to stop them from sending her out to LTAC. Because what could’ve happened Miranda, even though she’s stable now. They were talking about central line. They were talking about A-line. They were talking about vasopressor. That is something they couldn’t do in LTAC. Which means if she had…let’s just run this through in theory. If she had gone to LTAC last week, with a trach, she would’ve bounced back into ICU by now. Right? That is not what Carmen needs. She needs some stable environment. I do believe consistency of care is highly underrated. In a situation like that, such a vulnerable situation, people need consistency of care. They don’t need to go from one room to another. From one facility to another. They don’t need that. That’s added on stress.
Miranda: I mean, I could’ve have it.
Patrik: That’s right. If she has the trach and a week later or ten days later, she’s stable. Maybe let’s explore different options. But, at this point in time, I think it’s almost negligent to even discuss this from them. It’s a sign that they’re just thinking short term and they want to literally kick her out. But, it sounds like you’ve put a spanner in the works and told them, “look we’re not having it.”
Miranda: Yeah.
Recommended:
Patrik: Are you in hospital at the moment, Miranda?
Miranda: Mm-hmm (affirmative).
Patrik: You are?
Miranda: Yes.
Patrik: Right. Does your mother look more awake than she did a couple of days ago?
Miranda: She’s been doing a lot of blinking with her eyes. I guess. What else might…her shoulder’s been doing something.
Patrik: Okay. Would you then say, blinking of the eyes, that wasn’t there a few days ago? That’s new?
Miranda: I can’t say that completely. But, it’s more that I see her moving.
Patrik: Right. Right. Because if she’s blinking with her eyes, that’s something. That is more than probably you’ve ever seen, isn’t it?
Miranda: I’ve seen it a couple of times.
Patrik: Right okay.
Stephanie: Okay.
Patrik: Even last week?
Miranda: Mm-hmm (affirmative).
Patrik: Right.
Miranda: Yeah.
Patrik: So, it’s not brand new?
Recommended:
Miranda: Not completely but I think I haven’t been talking as much neither.
Patrik: Sure, sure.
Stephanie: The more you talk to her, the more she blinks and the more activity you get out of her.
Patrik: Yes, yes. Is she blinking when you’re talking to her? Or is it mainly spontaneously without you even talking to her?
Miranda: Would you say that is why we talk to her…
Patrik: Yeah. Do you feel like she’s blinking with her eyes when you talk to her, when you touch her or is she doing this spontaneously without you?
Miranda: Frankly, we didn’t touch. But, more when I talk to her.
Patrik: Right.
Miranda: When people want to…when the nurses want to…
Patrik: Right, right. Okay, okay. Stephanie was saying they’re talking about fluid build-up in her lungs. She might have too many fluids on her lungs.
Miranda: 75%, mm-hmm (affirmative).
Patrik: Right. You see, the other thing there that I didn’t mention earlier Stephanie, but now that we talk about this. If she has fluids on her lungs, it might change her ventilation.
Stephanie: Right. In what way?
Patrik: She may need more oxygen, for example. Or she may need more pressure. But, we don’t know. I can find out once I talk to someone. If I talk to a nurse, I can find out.
Stephanie: Are they planning to give her more oxygen?
Patrik: No. Not what I am saying. Imagine if you have fluids build-up in your lungs, there’s a very high chance you need more oxygen. There’s a very high chance you’re short of breath.
Recommended:
Stephanie: Yes.
Patrik: Right? So, those are the things you got to keep in mind. I am surprised… that… they’re waiting for the trach until Thursday. That doesn’t make any sense to me. I mean, they’ve been pushing for it all the way along. Why would they all of the sudden-
Stephanie: But, they haven’t taken her… I think… did they take her off of the blood thinners, the other day? When do they plan to do the trach? Did they give us a date, Miranda?
Patrik: No I don’t know the date unless you do. I don’t have any of that right now.
Stephanie: Okay, okay. No problem.
Patrik: Those are my questions. Yes, they’ve got to stop the blood thinners. I agree with all of that. But, that can usually, sometimes they’re stopped 24 hours before the procedure. What could be simply, is that they’re busy and that they’re full and they can’t do it before Thursday. I appreciate that. That could be a valid reason. But, given that they’ve been pushing so hard for it and now, all of the sudden, they’re saying, “well it’s going to be until Thursday.” That to me doesn’t make a lot of sense.
Stephanie: I did ask them what they plan to do to mitigate the… you always think about it later. What they plan to do to mitigate the fluid in her lungs. He says, “Well, we cannot…” at that point in the meeting he said, “We cannot give her Lasix.” But, when he went, he went out of the room. We were still in, having our family meeting. More than an hour later that he came back and says, “Oh her means is…”
Patrik: High.
Stephanie: High enough where we don’t need the arterial line.
Patrik: Yeah, that’s fair enough. Sometimes, if the mean is high, sometimes the kidneys do get more confusion and they produce more urine. But, if she is fluid overloaded in the lungs, you do give Lasix. You really do. Unless, do you know whether your mother is allergic to Lasix, for example. Do you know any of that?
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Stephanie: Not that I know of. What is Lasix? Is it a kind of latex?
Patrik: Yeah. No, no. Latex is, for example, when nurses wear gloves in the hospital, like those rubber gloves they are latex. Latex.
Stephanie: Right, right.
Patrik: One has nothing to do with the other.
Stephanie: Oh. I’m allergic to latex but to my knowledge, she’s not.
Patrik: Right, right.
Stephanie: I’m only allergic to it when it gets wet around my mouth at a dentist office.
Patrik: Right, right. Okay, okay. I can’t…it doesn’t make any sense to me that if she is fluid overloaded that they’re not giving her Lasix. That’s almost like, if you’re thirsty, you’re drinking water. If you are…in ICU, if you’re fluid overloaded, you give Lasix.
Stephanie: Yeah, get rid of it.
Patrik: Get rid of it. That’s right.
Miranda: They’re saying things. Hold on.
Stephanie: The nurse, mm-hmm (affirmative). Well, speak to her again. She might’ve.
Miranda: I had actually text you Stephanie. Let me look for the text.
Stephanie: Oh, okay. I heard the text. But, is the nurse in there? Or a doctor we can find out if she’s getting…like you asked what she’s getting antibiotics and I was like, “That should be right on that machine that they’ve given her something.”
Miranda: Diuretics.
Stephanie: Oh, is that like the diuretics?
Recommended:
Patrik: Oh a diuretic, yeah. Lasix is a diuretic, yeah.
Stephanie: Yes, yes it is.
Miranda: Except they can’t do that right now.
Patrik: Can you ask them why? Because that to me does not make any sense. If she’s fluid overloaded, and they can’t give her diuretic like Lasix, there might be something else going on that we don’t know at the moment. Maybe there is something else going on but it would have to be something significant.
Stephanie: We need to know why.
Patrik: I think so. I’ll tell you what that something could be but that’s just speculation. It would be helpful if I could talk to someone. What could happen is, they might be worried that if they give Lasix, she could drop her blood pressure and then they might have to put a central line in and an arterial line. That could be a concern. But, she’s fluid overloaded.
Stephanie: We need it.
Patrik: Absolutely.
Stephanie: Except they need it, they need it. They said they were going to do it. They have said from admission. They said they were going to do it. Then, they said, “oh well she’s high enough where we don’t need to.” Know what I mean?
Patrik: Yeah.
Miranda: I already talked to the nurse…
Stephanie: You talked about Miranda. Say it again.
Patrik: I would like to talk to the nurse, if I can.
Stephanie: I wish we had the nurse that was in earlier today. But, since anyone was in last night, right? But he talked to her and she talked to him nicely.
Recommended:
Patrik: Yeah, she was nice.
Stephanie: Yeah.
Miranda: But at the same token, I don’t want to keep talking to the nurse. I prefer to talk to the doctors because-
Patrik: Yeah, yeah we can.
Miranda: more of the information.
Patrik: Right.
Stephanie: So, who’s the doctor tonight? Or the doctors gone home? Dr. Edwin gone right?
Patrik: There must be a doctor on shift on, all the time.
Stephanie: Yes.
Miranda: I have to find out. Who’s doctor is on shift tonight?
Nurse: Dr. Brendon from Medicine.
Miranda: Are you from the senior?
Nurse: It’s Dr. Brendon.
Miranda: Brendon.
Nurse: They’ll be around…
Miranda: He’s for the whole night? Oh god.
Stephanie: He hasn’t been here yet though, can we speak to him? Can he make his round here?
Miranda: Our whole family would like to speak to the doctor.
Stephanie: Okay. When can we request it? Can we? I don’t want to say when…
Recommended:
Nurse: He has a lot of meeting today so.
Stephanie: That’s a nice way of…
Miranda: No, it’s something I especially want to talk to him about and my sister is… it did have something to do with…
Stephanie: And it’s time sensitive.
Miranda: Alright.
Nurse: Regarding breathing and stuff like that-
Miranda: Yes, yes ma’am.
Nurse: Okay, I’ll let him know.
Miranda: Thank you.
Stephanie: Amen. You’re doing a good job Miranda.
Miranda: Yeah. I’m just like, no, no the doctor that is here tonight, I don’t care for him.
Stephanie: Is that Dr. Stephens?
Miranda: No. It’s one more that’s a little bit, he’s nonchalant.
Stephanie: Oh I’ll tell you, he won’t be nonchalant when he talk to… he can be nonchalant all he wants. Patrik doesn’t care how nonchalant he is as long as he answers his questions. Right, Patrik?
Patrik: Yeah. Look as you’ve seen, we haven’t been confrontational. We have to converse very nice. You don’t want to be…
Miranda: Well, this guy. Listen to me. This guy, when I asked him a question, like two days ago, maybe three. I was like, “what are y’all doing?” He was like, basically gave me the shoulder like, if something we would do, we would do it.
Patrik: Oh, my.
Recommended:
Miranda: I didn’t like him at all. I didn’t like his response. He did this thing with his eyes. He just like know everything. He’s different.
Patrik: What did he say? Can you repeat that please Miranda?
Miranda: Stephanie can you say it? Because I’m starting to get real tired.
Patrik: Right.
Stephanie: Okay, she said, when she spoke to the doctor, she asked him, “So, what are you doing?” He said, “Whatever needs to be doing.” Now, either you’re gonna talk or I’m gonna talk. Go ahead Miranda.
Miranda: I’m sorry Stephanie. I’m walking back now.
Stephanie: Correct me if I’m wrong but let me try to say what you said. Or you can go tell him yourself because you can get to a place where you can talk louder.
Miranda: No, you tell him.
Stephanie: If I heard her correctly, she said she asked the doctor, basically, “What are you doing for her?” And he said, “Whatever we need to do for her, we’re doing.” Is that almost right?
Patrik: Yeah, sure, sure.
Stephanie: Miranda? Is that almost correct? Yes or no? Can’t hear you.
Miranda: Yes.
Patrik: Yeah. Without going to the details. No, no. That’s almost like an inappropriate response.
Stephanie: That is unacceptable, unacceptable.
Patrik: No, no, no. That’s not acceptable. For sure. Yeah, yeah. No, I hear what you’re saying. Look, you know, you do come across those people of course. That’s why it would be valuable to talk to somebody. So, if somebody had something to me like that, I would’ve sort of said to them, “oh look, can you please be more detailed.” I would’ve probably thrown a clinically question in.
Recommended:
Stephanie: Right.
Patrik: But…
Stephanie: But, you don’t mind talking to him, right?
Patrik: No, no, not at all. Not at all.
Stephanie: Miranda, is she getting the doctor? You’ll let him talk to him?
Miranda: They’re bringing someone over right now. Basically, when I talked to the nurse earlier, she was like, the diuretic, whatever it’s called, can’t be given when you preparing for the tube thing.
Stephanie: The trach.
Miranda: She was saying that they had more concerns than that. They’re not really concerned about her lungs.
Stephanie: How can you not be concerned about…you’re talking about the lungs that are 75 % flooded.
Patrik: I mean, obviously it was a concern for them to bring it up in the meeting. If they’re bringing it up in the meeting…
Miranda: But, that’s what I’ll be trying to tell y’all…oh god, please help me. I need to get some sleep. What I’m trying to say-
Stephanie: Wasn’t it, they say one… you’re doing good.
Patrik: Sure.
Miranda: doctors are say another thing.
Patrik: That’s why it would be helpful…
Miranda: To be honest with you, even if the doctors had said stuff and go back on their word too.
Patrik: Yeah, yeah. That’s why it would be helpful to talk to one of the doctors to find out what’s happening. Why can’t they give Lasix?
Recommended:
Miranda: Thank you.
Patrik: Unbelievable.
Miranda: I have a friend of my aunt on the phone and I want them to talk to the…
Stephanie: Family friend, yeah.
Miranda: Okay. I appreciate that. I didn’t know that she was saying…
Stephanie: Hello?
Miranda: I’m here. I didn’t know that they said they going to do the trach before the Easter come down. Well, Thursday, I agree with y’all. As long as everything is fine, what is stopping them from having a test to do the trach before then because they’re telling me-
Stephanie: All of the sudden, it’s going to be at the next day because she was stable at the time. Yeah.
Patrik: So, are we getting somebody on the phone Miranda? Is that what’s happening? Are we getting somebody on the phone?
Miranda: We’re working on it.
Patrik: Right, right. That is something that I don’t really understand. Last week, the trach couldn’t happen fast enough. Now, it’s going to be Thursday or Friday. That to me does not make any sense.
Recommended:
Miranda: I think, just to let y’all know, even though the doctors down here tonight. Last night, remember, I had to say something to the doctor and now we got a CT scan.
Patrik: Right.
Miranda: If you don’t tell me, then you’re saying that you’re all going to do resuscitate, when you should’ve already done it, in the beginning. I had to keep asking. So, even the night shift is different from the day shift. Even, if they come at night, we need to contact them in the morning time.
Patrik: So, are you saying that they did a CT scan last night of the chest. Is that what you’re saying?
Miranda: Right. But, I’d already been asked them a couple times. Does this fall under my mother’s problem?
Patrik: Right. Did they give you-
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!