Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Stephanie as part of my 1:1 consulting and advocacy service! Stephanie’s mother is in post- cardiac arrest care in the ICU and she is asking if keeping her Mom sedated might be the cause of her slow recovery.
My Mother had a Cardiac Arrest and is Having Seizures in the ICU. Is the Sedation Helping Her Into Recovery or Not?
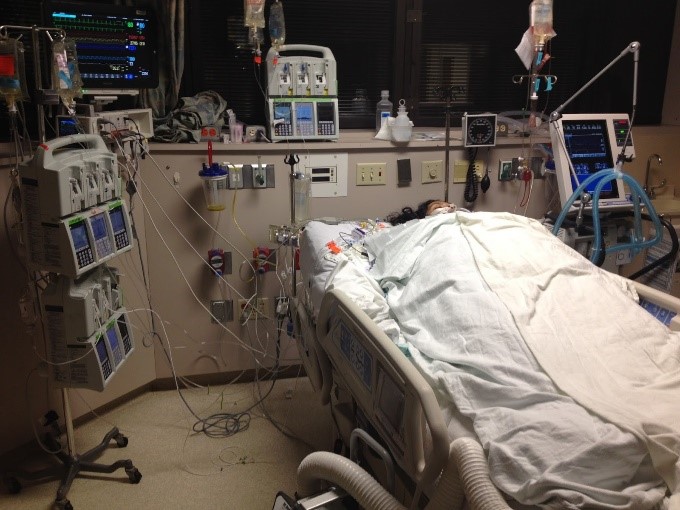
Patrik: It’s a full-on situation. But the other thing … and I’m not sure whether that’s going to help you or not, but I am a big believer that everything in life happens for a reason. I do not know the reason for this situation. By no means, do I claim that I know the reason for this situation. But I do believe things in life happen for a reason. I do not know what the reason is, but maybe there is a reason that you know.
Stephanie: Right. And maybe it will show itself down the line if not now.
Patrik: Correct.
Stephanie: Yeah. That’s what my niece Natalie said at the table. You’re saying that too. I believe everything happens for a reason. But whatever the reason, we walk through the storm.
Patrik: Yes.
Stephanie: So you’re good with that Miranda?
Miranda: I’m sorry, my bad.
Stephanie: You’re going to be all right. Just keep telling yourself, “Stay positive. You’re going to be all right.” I know that you have to step away sometimes from the hospital, then step away. Have somebody else there and just be strategic in it. When you don’t want them and I don’t think you do show them, you don’t want them to see that you’re going down because they can read your body language. Something you were telling me about that Patrik.
Recommended:
Patrik: Yeah.
Stephanie: That something about if you’re staying away to not give them an answer, but be strategic in something, that’s one thing.
Patrik: Yeah.
Stephanie: How do you put it?
Patrik: Yeah. I said something along the lines of-
Miranda: I want to say something, when I had first seen her in that brainstorm, I thought I was going down.
Stephanie: Yeah, she almost fainted.
Miranda: I do not even remember to breathe. I was trying to … They were rushing. They didn’t even look confident. I’m just being honest. Even though they are working there, they didn’t look confident. They’re all panicking and not confident at all. I was looking there and I just was like, “You cannot …” I started thinking to myself thoughts, thinking about breathing. I felt taking my breath, so they couldn’t see me and as soon as it got over, I walked my butt outside because I was like, “I wouldn’t want them to think that if her daughter can’t handle this … ” so they wouldn’t see what I was feeling.
Patrik: Right. Look, I think it’s okay to be vulnerable, that you don’t like what you’re seeing, right? I think that’s okay. I think what’s not okay is to be so vulnerable that they can walk all over you with decision making. Can you see the difference?
Miranda: Yeah, I see.
Stephanie: Say it again Miranda.
Miranda: Actually, I think confident, strong. I know I’m grown, but they can’t say that I’ve been trying to … This is a family thing. I can’t do this without my family. This is serious. And I haven’t been acting like I know everything or I go to them. Stephanie, I come to her, I talk to her. I don’t know. I just … she said I don’t know.
Stephanie: I think what she’s saying was. When it comes to the decision maker, she steps up. Go ahead, Patrik.
Patrik: We don’t know, right? I would never say that I have all the answers, I would never claim that, but I have seen enough to know that it’s not only a cut. And that rushing into a decision now, may cause more damage down the line, than you think-
Stephanie: Your emotions.
Patrik: Yes. Your emotions, your own mental health and so forth.
Stephanie: Right. The one thing I feel … let me just respect myself. One thing I feel is that at least if I feel like I’ve given that person a chance, it won’t be like, “No.” This is from my perspective, not from your perspective Miranda. At least I feel like we try to give her … let her get back to who she was. This is too early over the stage to even have that determination.
Recommended:
That’s what we have to get in our minds. We can’t say that this is the end-all-be-all, because this is just the beginning stage. That doesn’t mean that she’s going to be like this. That we have to realise that it is a process and that just because she looks like this now, does not mean that’s how Carmen is going to be. That’s the part.
So if we give her the chance to see who she’s going to be, what her body is going to, let her show us what’s in her. This is what she can do. I feel like until we give her that chance, we don’t know. At least give her a chance to see where she’s going to go with this. It’s not cut and clear and there’s no crystal ball. It’s day-by-day. Today is today. What can we do just to help Carmen at this moment?
Patrik: Yeah. And the other thing-
Stephanie: And Miranda, we’re not going to leave you. You’re not going to be alone. Okay? Go on, Patrik.
Patrik: Miranda, the other thing is when patients die in Intensive Care, I’m almost bound to say they “declare themselves”. What do I mean by that? Patients are in a critical situation and then treatment is maximised, it’s maxed out and patients still don’t survive. Your mother has not shown that, as far as I can see. She has not declared herself.
Stephanie: All right now. Yeah, she’s fighting. That’s what my sister kept saying. “Carmen is fighting.”
Patrik: Right.
Miranda: So that’s done.
Stephanie: Huh?
Miranda: So what is going on?
Stephanie: Wilma, I thought.
Miranda: If for whatever reason tomorrow, she’s, again, God forbid, if she crashes tomorrow and God forbid she’s deteriorating and she may not survive. Well maybe she’s declaring herself. But that to my … look, she’s been as close to death as she has ever been in her entire lifetime. Would you agree with that?
Recommended:
Stephanie: Mm-hmm (affirmative).
Miranda: I would think so.
Patrik: She has been as close to death as she has been in her entire lifetime. She is still with us, right?
Stephanie: Mm-hmm (affirmative).
Patrik: Tomorrow is another day and we have to wait and see what happens tomorrow and then… You know, But-
Stephanie: Exactly. Yeah, I can tell, she’s never been this close to death. Okay? I’ll declare it. She’s never been that close, not that it’s going to be … that’s the end-all-be-all. But she has never been in a state where her brain was without oxygen. You don’t get no closer than that, for two or three days. But that doesn’t mean that that’s the end, that’s for her. That doesn’t mean that that is her destiny. You know what I mean?
Patrik: Yeah.
Miranda: Mm-hmm (affirmative).
Stephanie: No.
Miranda: And it doesn’t mean that it’s your destiny either because that is part of your concern and that’s a valid concern, but it doesn’t happen. It’s too early.
Stephanie: Too early. Yap. So we take it one day at a time.
Miranda: So, Dr. Patrik is going to talk me down.
Stephanie: He’s a Nurse.
Patrik: I’m a Nurse.
Recommended:
Stephanie: Nurse.
Miranda: Okay. Nurse Patrik is going to talk down.
Patrik: Yes, absolutely. I’m also happy if you want me to do that and if it’s practically possible, I’m also happy to talk to them prior to the meeting, if that can be arranged. I would be very happy to do that. But I feel confident that within the time that is available to talk to the doctor so that I get all the information that’s needed. I’m positive.
Stephanie: I see.
Patrik: I’m positive that it can be in…within that period of time. I’ll be guided by you.
Stephanie: That sounds even better because it sounds like it’d be more productive if you spoke to them prior to speaking in the room.
Patrik: Yeah.
Stephanie: They won’t feel antagonised either.
Miranda: You already said that he’s a Nurse.
Stephanie: No.
Patrik: No. But when I start asking questions, they would probably … my questions will be very precise.
Stephanie: Mm-hmm (affirmative). I’d rather say he’s a consultant.
Patrik: Yeah. It doesn’t matter. You could even say I’m your friend or your cousin with an Intensive Care nursing background. It doesn’t matter.
Stephanie: Okay. Got It. And you are, because I feel we all are brothers. I think we’re absolutely all related.
Recommended:
Patrik: Absolutely.
Stephanie: Yes.
Patrik: I leave that up to you in terms of how you want to introduce me. It’s up to you.
Stephanie: Okay. We’ll work that out.
Patrik: Because I can … Yeah, you work that out.
Stephanie: Go ahead. Say last thing.
Patrik: No, you work that out. I’m confident that within the half an hour with the doctor so that we get all the information that we need, if it can be arranged…
Stephanie: Okay. He will speak to whom? The Intensive Care Nurse? Dr. Philipps? Because he’s the one throwing her out.
Patrik: I tell you what would be probably the less … the most, if I can talk to the bedside nurse, that would be not confrontational, right? And I can get-
Stephanie: Yeah. So which nurse … I’m sorry, which nurse?
Patrik: The nurse who’s looking after … If you’re tell me or call them tomorrow at six o’clock, whatever, and talk to the nurse who’s looking after Carmen, that would be good. And it would be not confrontational, because I’m just talking to him.
Miranda: I do not think they have enough information. It’s weird.
Patrik: No. Hang on. I tell you something, Miranda here. I tell you something. One of the biggest challenges for families is you don’t know what questions you need to ask. I will be very clear. I will be very succinct. That person will realise I am somebody who knows the profession.
Stephanie: Exactly. That you’re on the inside.
Patrik: Correct. They will know that within an instant.
Stephanie: Well, do you have a preference of which nurse they speak to, Miranda because … should he talk to somebody tonight? Should he call in the room now? Is Rebecca … nobody’s up there tonight, right?
Recommended:
Patrik: I talked to the charge nurse today and he was informative on any information, and he is free. He was trying to get me to Mikael. Mikael is watching my mother tonight. So that’s the RN that’s working beside her.
Stephanie: Rebecca is up there right now. I can have him call Rebecca and then Rebecca could put him on the phone if he’s there.
Patrik: Yeah. That would be the easiest way to go about … if you had a relative there and they pull out their cell phone, dial my number and say to the nurse, “Oh, can you please talk to my friend?” Or whatever. That would be the easiest way to go about it and then get some information.
Stephanie: Okay. I’ll take care of it, Miranda.
Miranda: One second. Would you gonna act? It’s five o’clock.
Stephanie: Rebecca.
Miranda: One second. Hold on. Don’t stress me though.
Stephanie: Okay. To be for of Wilma to be forewarned, to be forearmed.
Miranda: I’m talking.
Stephanie: Take your time.
Miranda: I’m going to try to give to Becca.
Stephanie: Okay. To make a three-way? Got you.
Patrik: So you have a family member there at the moment. Do you?
Stephanie: Yes. Rebecca.
Patrik: Right.
Stephanie: Rebecca. She was on the call. She’s our rock.
Patrik: Yeah. I get it.
Stephanie: She is the night time. She’s a rock on that end and I’m the rock on another end. We all have a role.
Recommended:
Patrik: Yes.
Mikael: Hey.
Miranda: Mikael?
Mikael: Yes.
Miranda: Hello. This is Miranda, and then Carmen and I’m her daughter.
Mikael: Hi Miranda. How are you?
Miranda: I spoke to you earlier.
Mikael: Yes.
Miranda: I just wanted to speak to you again today, okay?
Mikael: Thank you. How are you doing?
Miranda: Mm-hmm (affirmative).
Mikael: How are you doing this morning?
Miranda: I’m doing my best.
Mikael: Great.
Miranda: I actually have my friend on the phone with me right now and I actually have … we have some questions. Are you able to look at my mother’s charts and giving me some information?
Mikael: Sure.
Miranda: That’s great.
Mikael: Looks like my phone might die soon. Go ahead.
Recommended:
Patrik: I’m Miranda’s friend. Just have a couple of questions. You’re the bedside nurse, are you?
Mikael: Yes.
Patrik: Right. How is she doing? Is she doing okay? She’s stable?
Mikael: I would say she’s stable.
Patrik: Right. What’s her Glasgow Coma Scale at the moment? Is she at Glasgow Coma Scale three?
Rebecca: Good Morning.
Mikael: Good morning Ma’am, how are you?
Rebecca: I’m good. Are you aware that my mother’s blood pressure is high?
Mikael: That’s not high. That’s okay.
Rebecca: What’s not high? 124?
Mikael: Yeah.
Rebecca: That’s not high?
Mikael: Can I finish on the phone, please?
Rebecca: Yeah. Okay.
Mikael: All right.
Stephanie: Yes, my sister is probably concerned.
Rebecca: It’s fine.
Mikael: All right. Go ahead.
Patrik: Yeah, sorry. Is she sedated to the point where she’s got a Glasgow Coma Scale of three or … just trying to find out where she’s at.
Recommended:
Mikael: Sorry. I didn’t hear your question, please.
Patrik: Yeah, sorry. Is she still in an induced coma? So, that her Glasgow Coma scale is three?
Mikael: No, she’s not induced. She’s not been in sedation.
Patrik: Right. Is she waking up?
Mikael: No.
Patrik: Right. So what’s her Glasgow Coma scale then? Is it a three or is it higher than that?
Mikael: Three.
Patrik: Three, right. And her pupils are equal and reactive?
Mikael: Sluggish.
Recommended:
Patrik: Right. And is she having any seizure?
Mikael: None that I’ve seen so far.
Patrik: And when was the last seizure that you’ve seen or that anybody has seen?
Mikael: She’s getting Keppra, she’s a little bit sedated with anti-epileptics.
Patrik: Right. She’s getting Keppra, she’s getting Dilantin?
Mikael: She’s getting Keppra and she’s getting Phenobarbital.
Patrik: Right. So the thing is Phenobarbital to a degree would keep her sedated depending on the dose.
Mikael: That’s true.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!