Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
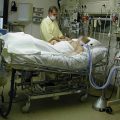
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Stephanie as part of my 1:1 consulting and advocacy service! Stephanie’s mother is in post- cardiac arrest care in the ICU and she is asking if the long-term length of stay in the hospital is a modifier of her prognosis.
My Mother Had a Cardiac Arrest and is on a Ventilator in the ICU. Are We Losing Her?

Patrik: Right. And is she having any seizure?
Mikael: None that I’ve seen so far.
Patrik: And when was the last seizure that you’ve seen or that anybody has seen?
Mikael: She’s getting Keppra, she’s a little bit sedated with anti-epileptics.
Patrik: Right. She’s getting Keppra, she’s getting Dilantin?
Mikael: She’s getting Keppra and she’s getting Phenobarbital.
Patrik: Right. So the thing is Phenobarbital to a degree would keep her sedated depending on the dose.
Mikael: That’s true.
Patrik: But she hasn’t had any seizures?
Mikael: No. Any tonight.
Patrik: Right. Is she hemodynamically stable? Is she on any vasopressor?
Mikael: No, not any. No pressor.
Patrik: No pressors, okay. Is she ventilated, is she triggering any breaths herself or is she in a controlled ventilator?
Mikael: She’s breathing above the vent.
Recommended:
Patrik: Say that again please?
Mikael: She’s breathing above the vent.
Patrik: Right. So she’s triggering some of the breaths herself.
Mikael: Hello?
Patrik: So she’s triggering some of the breaths herself?
Miranda: Hello?
Patrik: I’m here. I’m here.
Stephanie: Mikael? Is he still there? Mikael?
Miranda: No. I hang up.
Stephanie: You sure? Okay. Rebecca’s beating him up. Okay? She says her blood pressure I high. See, Rebecca, she’s not as conventional. She doesn’t time out. She just said it as it is. Even when it’s right or wrong, but he’s like, “No, her pressure is not high. That’s fine.” You can hear on the background.
Patrik: I’m glad we’re getting somewhere.
Stephanie: Yeah. So what you have to do, Miranda … This is what I believe, Miranda, when you call the main hospital number, you call them on extension 7-1. That’s what I think he’s trying to say, Miranda.
Recommended:
Miranda: No, he was saying more, 7-1-4 something, but I’m going to talk to her.
Stephanie: There you go.
Miranda: I’m cool with her.
Stephanie: Okay. Answer … okay.
Miranda: All right.
Stephanie: Okay.
Miranda: Her temperature, when I was up there early, it was like 170 something. I mean, not the temperature, the blood pressure, 170 something. 101-
Stephanie: Okay, go ahead-
Miranda: that’s not high. I mean, 120/80 is high.
Stephanie: Yeah. Plus she’s not on any vasopressor because they took out the arterial line, so how’s she on any vasopressor, right?
Patrik: Yeah. That’s right. If they took out the central … and that’s something I’m going to ask if we do get back to him, whether she’s gotten a central line, whether she’s got an arterial line, all of that. But the other questions that I have is, for example, what are her kidneys doing? It’s not a good sign that she’s got a GCS three but she is sedated. She doesn’t have-
Stephanie: But she’s on … she’s sedated. Whether they want to say or not, she’s sedated.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: That’s right.
Stephanie: Phenobarbital … she’s still sedated. She may not be in a coma, and that Glasgow Coma but she is sedated.
Patrik: That’s right.
Stephanie: She’s on Keppra.
Miranda: One second. Let me call him on my phone number.
Patrik: Yeah. Call him again.
Stephanie: I’ll talk to you while you call him. Go ahead. Whatever you want to do. That was smart. That way is unintimidating.
Patrik: That was very unintimidating. And one thing that I say to people all the time is don’t over complicate. And in this situation, we didn’t over complicate at all. We just found a number.
Stephanie: No, you didn’t. That’s it. Wow. See my sister, she’s like, “Yes, it is.” You heard her on the background. She was confrontational with him. You don’t get anything like that?
Patrik: No. Do you have a family member there every night?
Stephanie: Yes, indeed.
Patrik: Right.
Stephanie: Rebecca. She’s there. If nobody else, either she or Carmen, her or Rebecca, Wilma has … Listen to me. Her or Miranda, maybe Wilma but mostly Rebecca. Rebecca is retired.
Patrik: Right.
Miranda: He’s not answering the phone.
Stephanie: Why don’t you call my sister Rebecca? I’d just say call Rebecca on the room phone. Yes. I think the room phone will give you a better connection, you don’t have to worry about it dying. He had to tell Rebecca, “Calm down.” Don’t be antagonistic to that guy.
Recommended:
Patrik: No, I don’t think-
Stephanie: You don’t think what now?
Patrik: Do you think I was intimidating to him?
Stephanie: Not you. Rebecca. Not at all. You were wonderful. No, not at all. Rebecca was like, “Yes, it is high.” And he says, “No, it’s not high.” That’s all he had to say. He is on the phone and she’s woofing at him. And he’s trying to tell her, “Can I finish the conversation? Can I finish on the phone, please?”
Patrik: Yes, he did say that.
Stephanie: She wasn’t aware. He didn’t tell her that he was on the phone with Miranda. She wasn’t aware that Miranda was on the phone with him.
Patrik: Right.
Stephanie: Right? Communication. Let me text her while I’m talking … Hopefully I don’t lose the call.
Patrik: If not, I’ll call you back.
Stephanie: Let me just text her while Miranda was on the phone with the nurse. I’m going to tell her Miranda was on the phone with the nurse, so don’t say it … let him let him do his work. Okay.
Miranda: Hello.
Stephanie: Yes.
Miranda: Okay, so Stephanie … Mr. Patrik?
Patrik: Yes.
Miranda: My other sister is on the phone.
Stephanie: Okay got it.
Recommended:
Rebecca: I was just getting ready to call you Stephanie.
Stephanie: Yeah, yeah. We’re on the phone with our cousin Patrik!
Rebecca: Yeah I know, I’m concerned because I was very uptight. Normally I check a lot. She has elevated blood pressure 142/83. I needed to put my pants on and I put my jacket on and I went up there and I spoke to the charge nurse, Nurse Geoffrey. I said, “I’m very concerned about the elevated blood pressure.” I said “you know I never come down here to bother you guys, I said but I want Mikael off of my mother.” He sat in there with those earphones on, and I said not only that, okay is 142/83 and here her pulse was 100, whatever that is, and I’m very concerned.
Stephanie: Is that her pulse oximetry? Is that her oxygen level? What colour is it? Is it green?
Rebecca: Green, yeah
Stephanie: Green. I think that’s her pulse oximetry.
Rebecca: And then the other one is 99, I believe it was 99 and I know for a minute, is 20 between 28 and 29. Now Miranda, the nurse is in here. If you all want to talk to him, I can give him the phone and you all can ask him whatever you want to ask him. I have nothing else to say to him at this time.
Stephanie: Yeah, don’t beat him up ’cause we’re trying to get somewhere!
Rebecca: Wait just one moment Stephanie.
Stephanie: Okay.
Rebecca: Oh here you are … 142/87.
Stephanie: That’s not bad. It’s not.
Recommended:
Patrik: That’s not bad. That’s not bad. I wouldn’t worry about that at all.
Stephanie: Mikael, he’s on the phone.
Miranda: Mr. Mikael, I apologise sir. If you don’t mind this is Miranda again.
Mikael: Hey Miranda, how are you?
Miranda: Can you please, I couldn’t get the extension you were telling me to call you on.
Mikael: I think it’s … hold on let me read it for you again.
Miranda: Take your time, Okay.
Mikael: Hello, are you there?
Miranda: Yes sir.
Mikael: You can send it on 7**** that would be great.
Miranda: So I just dial 4***-***-****.
Mikael: Yes.
Miranda: Okay. Let me try it.
Mikael: Or if you get the operator, you can ask for 7****.
Miranda: Okay, just give me one second. Just stay right there where you at for a second just to see if it rings, and I appreciate your patience.
Mikael: Oh sure! Take your time.
Recommended:
Miranda: Yes sir … one second (pause).
Mikael: Did you call the number?
Stephanie: Miranda? She’s probably calling it now. I don’t know how we’re still connected.
Mikael: I can hear a phone ringing outside, I’m in the room. Do you want me to go check? Can you check if that phone is ringing out there?
Stephanie: Um huh, um huh.
Mikael: Go ahead let me go get that one okay?
Stephanie: Um huh. If he gets connected just go ahead and talk to him, Patrik.
Patrik: Sorry. Is he still there? Mr. Mikael?
Stephanie: Yeah if he gets-
Miranda: Hello, hello!
Patrik: Yes, Mr. Mikael can you talk?
Miranda: Okay I can hear you better.
Patrik: Can you talk Mr. Mikael?
Mikael: Yes I can hear you
Patrik: Right, now that’s great. I was just asking a bit earlier before you went off so she’s breathing above the ventilator?
Mikael: Right.
Patrik: That’s great, that’s great. And everything else, kidneys are working?
Mikael: Hmmm, so she’s making urine and let me see, our latest labs are is Crea is 0.7, BUN is 22.
Patrik: Right, Right. Okay so that’s all not too bad. And are there any signs of an infection? Is she having infection? Is her white cell count up?
Mikael: Yeah the white cell count is up.
Recommended:
Patrik: Right, right. And is she getting antibiotics for that?
Mikael: So, let me ask a quick question. Who am I speaking to?
Patrik: Yeah, I’m a family friend, but I also have an Intensive Care nursing background.
Mikael: Do you want me to give you guys to the Intensivist?
Patrik: No, I’m happy with the information that you’re giving me. I’m very happy, very comfortable with what you’re sharing there.
Miranda: We’re just trying to get just the notes from the lab and things from earlier-
Mikael: I mean, I mean I could have given you to the doctors
Patrik: Yeah, well we can, Miranda do you want me to talk to the doctor. Miranda, what do you want?
Miranda: Who’s the doctor on board tonight?
Mikael: Dr. Nancy is here, she’s the intensivist tonight, but there is a resident as well.
Miranda: There’s a resident as well. Who’s the resident? Are you talking about the short lady, Dr. N. something?
Mikael: Dr. Nancy is here tonight. I don’t know who you mean.
Miranda: Is that a young lady?
Mikael: She’s, I would say, middle age.
Miranda: Oh yeah that’s what I mean. I mean like she is a lady and she’s kinda short?
Mikael: Yes.
Miranda: Okay. So you feel more comfortable with us talking to the doctor asking questions?
Recommended:
Mikael: No. You can ask me questions, but I think if you have other needs that any specific plan of care, information that you need-
Miranda: Oh like if her white blood cell is up, why she is not on an antibiotic.
Mikael: Well, those are the things I would give you to the doctor to handle.
Miranda: What do you all want to do? Stephanie, Patrik?
Patrik: Yeah, look. Like I said I’m guided by you Miranda. I’m very comfortable with what Mr. Mikael is sharing there. I’m just trying to find out. I’m very comfortable with the information. It’s really up to you-
Stephanie: ‘Cause we don’t know the lingo Miranda. We don’t know the lingo and Patrik does. He can explain to us.
Miranda: Mikael is asking do we want to speak the doctor, because they can provide more information. Mikael don’t know why she’s not on an antibiotic.
Mikael: I know that his white cell count went up yesterday and we did culture. Why we didn’t start antibiotics at that point I’m not sure but I know we did a culture on her.
Stephanie: I think Mikael is doing just fine giving this information we want. We can explore that at a later date. Do you know what I mean?
Patrik: Mr. Mikael if I just may ask. Probably the biggest problem at the moment is she’s not waking up. That’s probably the biggest problem, she’s a GCS-3 on minimal sedation. That’s probably the biggest concern at the moment.
Recommended:
Mikael: Okay.
Patrik: As far as I can see. Would you agree with that?
Mikael: Once again, she’s been here for since the 10th. Right. I don’t know for how long she was down, and that normally is one of the reasons why someone would take time before they wake up.
Patrik: I understand, but it’s a good sign that she’s not having any more seizures at the moment because I believe that’s been a concern in the beginning. Some of the Keppra and Dilantin seems to work then but on the other hand she’s not waking up.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!