Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Lara, as part of my 1:1 consulting and advocacy service! Lara’s mother is critically ill in ICU with a hemorrhagic stroke and isn’t waking up. Lara is asking how can she be in control of her mom’s condition and not to be intimidated by the ICU team?
My Mom is Critically ill in ICU with a Brain Injury. How To Be in Control of my Mom’s Condition and Not to Be Intimidated by the ICU Team?
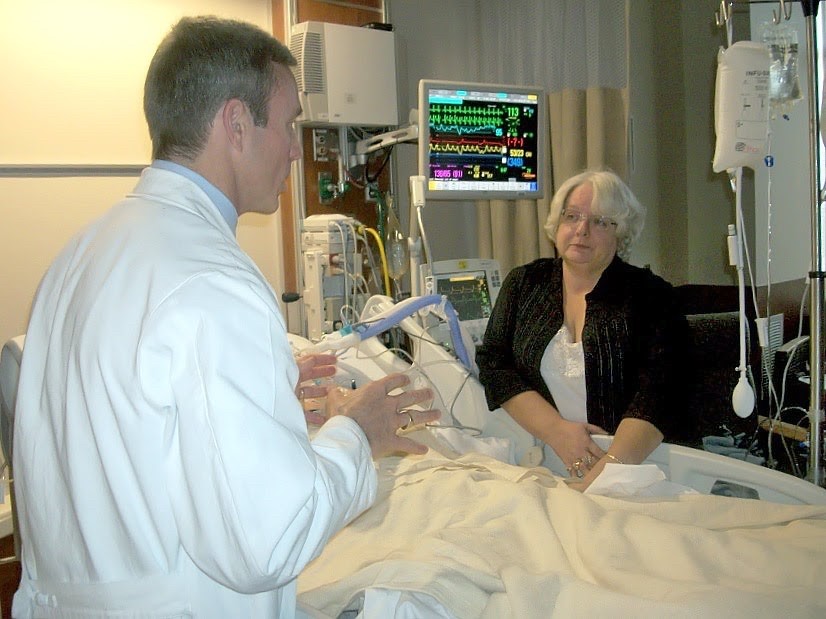
“You can also check out previous 1:1 consulting and advocacy(7) sessions with me and Lara here.”
Patrik: Right. So we can help. And that’s the sort of thing we can help you with. Again, we have removed countless of DNR orders because again, we know, number one, we know where they’re going wrong in terms of how they go about it. And then number two, we know how to ask all the right clinical questions. The reality is that if this DNR order is on your mother’s file at the moment if your mother was to sustain a cardiac arrest if her heart was to stop, there wouldn’t resuscitate her because it’s documented and that document needs to be taken away as quickly as possible.
Lara: Okay.
Patrik: Those are all the things. They’re telling you this is a matter of fact, without giving you an option. They’re always framing things as “in the best interests of your mother,” while the reality is there’s a clear conflict of interest. Your best interest is your mother, their best interests is their beds, their staff, their budget management. That’s their agenda. Right? And they’re not telling you about it, but everything they’re communicating to you is framed around their agenda.
Are you there? Are you there? Hello? Hello?
RECOMMENDED:
Patrik: Intensive care hotline. Patrik speaking. How can I help?
Lara: Okay, Patrik. I think it disconnected.
Patrik: Yes. I don’t know what happened, and sorry, what was your name again?
Lara: It’s Lara.
Patrik: Okay, Lara.
Lara: Yeah, that’s right.
Patrik: Right, right. So you know, those are the type of things, that’s their strategy. It’s all about their framing of, “Oh yeah, this is all hopeless. You know, your mother wouldn’t have any quality of life.” Have they used terms, for example like… and I hate the term and I’m only paraphrasing here. Have they used the term that your mother would be a vegetable, have they used that term?
RECOMMENDED:
Lara: No, they haven’t.
Patrik: Good, good.
Lara: But the thing is, she’s missing her right arm as well.
Patrik: Yeah, yeah, yeah, yeah, yeah.
Lara: I don’t think they have the right to even say that.
Patrik: No, but look, I can’t tell you, the term is being overused and misused, I believe. What has been the biggest roadblocks to this point for you? Number one, what has been the biggest roadblocks at this point for you? And then number two, what’s the ideal outcome you want to get?
Lara: I mean the biggest roadblock was that when she arrived, they said that she has bleeding in three places and they said some of them are quite large. And then the first roadblock was that they couldn’t give her any surgery or drainage because she may not make it out on the surgery. But that’s all they said. They didn’t really explain why and they spoke to the neurologist. And then we did question it. So we had the consultant come up again and then she showed us the results and she said they can’t syringe it because I think because also her age and her size-
Patrik: Her age is-
Lara: … and then they couldn’t…
Patrik: Her age is irrelevant.
Lara: Yeah.
Patrik: Age is irrelevant. Again that is something they are telling you. You’ve got to be prepared to give them something back. You know, my response would have been age is irrelevant.
Lara: Oh no, they didn’t actually say it. She just said that with her condition, the way she is, she wouldn’t make it out. She said that she’s gone to the head neurologist and he said it’s not possible. And then they did hear us complaining. So I think the nurses heard us saying things like, “Oh, they’re just like busy and they can’t be bothered.” So then she did say to us like, “Oh, it’s not just because we’re not bothered and things,” not bothered, she said, “It’s not just because we don’t have the time or we’re too busy or something.” But that’s because I think the nurse repeated what she heard us say.
RECOMMENDED:
Patrik: And what’s the ideal outcome you want to get?
Lara: So the ideal outcome would be that they keep her feet on and then if the antibiotics don’t work for this round, that they should just wait a day or so and then try again. Because it’s not that you just give antibiotics once, you can have a delay of a day or two and let’s try again. Regardless of the fact that you know.
Patrik: Absolutely.
Lara: I mean, what is the protocol for that? Do they have to wait a day or two, or can it just be started immediately?
Patrik: Again, that would be then part of how we can help you, to talk you through that and also talk to them to make that happen.
Lara: Yeah. So I’m going in tomorrow and I’m going to try and get some more information. I think it might be better if I speak to them and get all the information and then call you.
Patrik: Absolutely. So what I’ll do is-
Lara: And then if we go for the one hour option to begin with-
Patrik: Yes, absolutely.
Lara: … I think that will work well just because we just don’t know what could happen.
Patrik: That’s right.
Lara: And actually part of me is a bit scared actually. Because it feels like they’re so adamant with their decision that if we raise our voice too much. I know this sounds terrible, but we just don’t know what they might do overnight, or not do.
RECOMMENDED:
Patrik: Yeah, I wouldn’t be too worried-
Lara: … that can cause her to, you know?
Patrik: I wouldn’t be… yeah, yeah. You see, I wouldn’t be too worried about that because again, once you start working with me, I’ve seen all of that. You should not be intimidated. Never, ever. You should never think that “Oh, what I’m doing could impact on our mother’s care. Because they have a duty of care. And the most important thing is that you start gathering the right information and then go back to them with the right information. That’s the most important part. You should not worry about what you say and what you don’t say. Because as you can see, they’re not worried about what they’re saying or what they don’t say. Look, I’m all for making friends. Don’t get me wrong. I’m not saying, you shouldn’t keep the peace, but at the same time there comes a point where, this is potentially a life or death situation where holding back may not work in your favour, but let’s get more information first.
Now, the other thing that I was going to say is yeah, it’s best if you start with the hour option. Because also if you then want to go on with the four-day or the seven-day options, that amount would be credited towards that.
Lara: Oh, okay, that’s good.
Patrik: Right so you can’t lose out there. And also, for the four-day or for the seven-day option, you can use that at your own pace. Right? So you are in control when you want to use it. So it’s not four consecutive days or seven consecutive days. You are in control when you want to use this.
Lara: I mean I would love to use that option. It’s just that they’ve, from what they said, it could just be any day that something happens or if she suffers another one in the night, we just don’t know. So, I would really appreciate taking your help.
Lara: Okay, that’s fine. So do you think it’s best that I… because I’m going to go in tomorrow, if I speak to them, try and get an update on exactly. Because they told my sister, but I think she was busy so she didn’t question it. So I want to go back and ask them why, and then get that information. And just, I could say on where she is what they think and… And then if I speak to you then, and then maybe if we use the other half an hour for the consultation.
RECOMMENDED:
Patrik: Yes, absolutely. Absolutely. And I’m not counting minutes. You know, if it takes an hour and a half it’ll be absolutely fine. You know, I’m not counting minutes. And the other thing is, I will be available over the weekend, if you know, it’s… because I know my clients, they need help. It doesn’t matter what day of the week really, you know, so that it’s not like a Monday-to-Friday service at all. It’s really like a 24-hour service.
Patrik: So what I’ll do is I will email you the consulting options, and then you can have a look, and you can also then go through the checkout there. You just click on the link and it’ll talk you through what to do. It’s very simple. And then I’ll wait to hear back from you.
Lara: Oh, brilliant. So I’ll definitely use that. I’m just not sure when, because obviously we need to get hold of the consultant although they’re busy.
Patrik: Say that again please. The last part you’ve dropped out a bit.
Lara: Sorry. So if we do ask to speak to the consultant, they’re obviously busy, so they come to the bay when they have time. So would that be okay for you if I call you?
Patrik: Okay.
Patrik: It would, yeah, absolutely. It would be okay. But you see, I’ll tell you where there’s a bit of an issue and it’s more a mindset issue rather than anything else. You say they are busy and they come when they have time.
The first step for you now is you need to ask them, “Hey, I’m available at,” you know, your time, whatever. And you say, “Look, I’m coming in at four o’clock. Can you please talk to me at four o’clock.” The first thing you need to change, is the way you communicate with them. That’s the first thing. You see, a lot of things in life you can’t control. Focus on what you can control, and you’ll be far more powerful.
You see, all families in ICU don’t ask or don’t tell the consultant, “Hey, I’m available at four o’clock,” or whatever time you are available. “Can you please talk to me?” Right?
RECOMMENDED:
Lara: Yeah.
Patrik: So change the rules and change the rules tomorrow.
Lara: Okay, yeah.
Patrik: Right? They will, again, I hate to say it, and I’m probably exaggerating a little bit here, but they will walk all over you if you let them. Don’t let them. If they are doing what they’re doing 365 days a year, that’s how they manage their ICU. You need to start managing them.
Lara: Yes. Yeah, that makes sense.
Patrik: Change-
Lara: Yeah.
Patrik: Change the way you communicate with them and change it when you’re going in there tomorrow.
Lara: Yeah. No, that makes a lot of sense. So I’m definitely going to use your services. So I’ll send that through, but I just don’t know exactly what time.
Patrik: Yeah. That’s fine.
Lara: So I’ll need to… I mean, I will try and do what you said. I’ll go in and say, can they be available at this time. But you know, I’ve tried that before. They still haven’t done their rounds or I’ve bleeped them, but they’re not answering, you know, that’s the answer they give.
RECOMMENDED:
Patrik: Sure, sure. And you know, the reality is with anything that needs to change, it usually doesn’t happen in the first attempt. Just because you’ve tried and didn’t succeed yet, doesn’t mean it’s not going to happen. You know, you need to be persistent. You know, usually when they realise, “Oh, hang on a sec, this lady is very different from everybody else because number one, she’s saying different things and number two, she’s not giving up,” you know, so…
Lara: Yeah, that’s true. Because then they start worrying that, you know, you’re going to question what they’ve done, later.
Patrik: Exactly. Exactly. So what I’ll do is, I will send you the email. Okay, and then I’ll wait to hear from you.
Lara: Oh brilliant. And I just wanted to ask one question. So the person in charge of a whole unit, that’s the registrar. Is that correct?
Patrik: Say that again, please.
Lara: The person in charge of a unit is the registrar? Is that correct?
Patrik: No, no. It would be the consultant, it would be the consultant.
Lara: Oh, it is the consultant?
Patrik: Yep.
Lara: No, that’s fine.
Patrik: Yep, yeah.
Lara: And if you wanted to complain about the consultant,
Patrik: That would probably best be on a hospital level, like on an executive level. Like probably director of nursing or even a CEO level.
Lara: Right, I understand.
RECOMMENDED:
Patrik: Okay. Look, I’ll let you go. I’ve got another call coming in. I’m so sorry. I will then email you the consulting options. Okay?
Lara: Okay, Sure.
Patrik: And I’ll wait to hear from you then.
Lara: Thank you so much.
Patrik: Thank you. All the best for now. Bye bye.
Lara: Thanks. Thank you.
Patrik: Bye. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!