Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
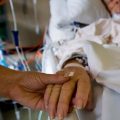
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tim as part of my 1:1 consulting and advocacy service! Tim’s mother had surgery, a history of COPD and is in the ICU for pneumonia and Tim is asking if his mum can still be weaned from the ventilator with a PEEP of 8.
My Mother Had Surgery and is in ICU for Pneumonia. Will My Mum Be Weaned from the Ventilator with A Positive End Expiratory Pressure of 8?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Tim here.”
Patrik: So, right? So, she’s basically triggering every single breath herself, and then flow gets delivered from the machine. But she must initiate that herself, and she’s doing that.
Tim: Okay.
Patrik: Okay, I can see that in the picture. The… there is a couple of things that as a PEEP… what’s important, there are three numbers that are important. There’s a PEEP of 8, which is high still, there’s another number… excuse me…. there’s another number, pressure support of 14, and oxygen is 35%. All those numbers are still too high to get your mother off the ventilator.
Recommended:
Tim: Oh, okay.
Patrik: Okay? So, the PEEP, for example should be down to 5, the pressure support probably be down to 10 or to 8, until she can have the first time off the ventilator. So, can she achieve that? We don’t know at this point in time, right? We’ll probably find out on Monday.
Tim: They’ve done some sprinting this morning, apparently, early this morning.
Patrik: Right, and?
Tim: They said it looked like she was struggling too much, and they put her back… and the oxygen dropped down to 93 or something.
Patrik: Right, right.
Tim: And the nurse said it wasn’t that bad, but-
Patrik: Right.
Tim: She looked uncomfortable so just put her back on it.
Patrik: Right. Does she need… does she need a lot of suctioning, do you know?
Tim: Bit of phlegm, yeah, she’s had a bit of phlegm. But they hadn’t done it until we’d got there this morning, so.
Patrik: Right.
Tim: They said they got little of it.
Patrik: Okay, okay. And then she’s on 35% oxygen, probably should be less than 30%, so just for explanation. Room air, the air that you and I are breathing is 21%, right? So, 35% is still a little bit too high. But look, if the numbers that I spoke about now come down, she could well come off the ventilator. But the next few days will show.
Tim: Because what’s the standard time for a ventilator? 10 days or something?
Patrik: Look, it’s really hard to say. People are so different, Tim, you know.
Tim: Mm-hmm (affirmative)-
Patrik: If your mum… okay, if your mum was on those ventilator settings, and she didn’t have the lung cancer, I would-
Tim: No, not lung cancer, stomach cancer.
Patrik: Stomach cancer, is it?
Tim: Yep.
Recommended:
Patrik: Oh! Why did I think… Okay. Oh, stomach, not lung.
Tim: Yeah. But they cut most of it out, and they-
Patrik: Right.
Tim: stomach there and stuff, and-
Patrik: Right. Is she having chemotherapy?
Tim: Well, not now, they said she’s just too weak, they said if-
Patrik: Right.
Tim: She was supposed… first the professor said it was… he was going to try and cure her, and it started out nice but yeah he sorts of changed that tune to say it’s more palliative surgery-
Patrik: Sure, sure.
Tim: They say one thing and now another thing-
Patrik: Yeah, yeah, yeah, yeah. And is she… does she have any metastasis. Do you know what I mean by that?
Tim: No.
Patrik: The cancer hasn’t spread anywhere else, as far as you’re aware?
Tim: Oh.
Patrik: Metastases.
Tim: That’s it, yes, she did actually but he said he cut the rest of it out.
Patrik: Right, do you know-
Tim: And I know, I know it can spread and come back and….
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Right, right, okay.
Tim: Oh, they removed it.
Patrik: Right.
Tim: This surgeon, he’s a really good surgeon, and he… he sorts of chopped away, he took a lot of stuff out.
Patrik: Sure, sure. And what about… you said your mum has COPD?
Tim: Yes.
Patrik: Right, right, okay. And that could… that certainly doesn’t help to get her off the ventilator. It doesn’t help but it’s not impossible because of COPD, not coming off the ventilator.
Tim: No.
Patrik: It’s not impossible, right.
Tim: No.
Patrik: I think the next step is, on Monday, talk to HCF. Try and be one step ahead of them, because you know if you talk to HCF on Monday, in the ideal world, HCF is open to the idea, right.
Tim: Yeah.
Patrik: And then you could go into the meeting and you could say, “Hey, here is a service, HCF might come to the party, let’s go home.”
Tim: Yeah, I’m sorry. Can’t hear.
Patrik: No, no, that’s all right. But does that make sense?
Recommended:
Tim: Yes, try… yeah to give them a call first, before the meeting and have a chat to them about you?
Patrik: Yeah, yeah. You can definitely do that, and then go to the meeting. But even if HCF can’t give you an answer on Monday morning, for whatever reason, it’s still timely now to bring it up. And the reason it’s timely is… they will be pushing towards end-of-life.
Tim: Sorry, what was that? Sorry, I missed that.
Patrik: I said even if for whatever reason you can’t speak to a decision maker on Monday morning within HCF, right?
Tim: Yeah.
Patrik: It is still timely to bring up Intensive Care at Home now, right, because… and I tell you why. Their push…. now that they’ve mentioned the term “futility”, from now onwards I expect the worst from them. I expect to push for end-of-life from now on.
Tim: Yep, that what it seems like.
Patrik: Right, right. So, in order to stop them from doing that, you need to make sure you’re going in another direction, which is you want your mum at home. You don’t want her to die in hospital, right?
Tim: Yep.
Patrik: And you know, you’ve got to have an answer to them because, and you have that answer already by suggesting Intensive Care at Home.
Tim: Yes.
Patrik: Right? So, because they will be… knowing Stamford Tim, I tell you I had two clients there, and I mean clients, not for Intensive Care at Home but for my consulting. I tell you Tim, they are butchers there.
Recommended:
Tim: Yeah.
Patrik: They are butchers. When… I’m glad you didn’t have a bad experience with Aaron and I’m not even going there.
Tim: Okay.
Patrik: You know, but there’s the people that I’ve dealt with, and my clients dealt with, at Stamford… and that’s why I’m saying, we need to be prepared. And that’s why, if you had gone in this meeting yesterday, they would have tried and walked all over you. And they will try again.
Tim: Yeah.
Patrik: Right? But now… but we… I know what’s to come. I’ve been in family meetings at Stamford over the phone, right? They are horrible.
Tim: Look, I’m sorry for the noise.
Patrik: Right? So-
Tim: So, what do I say to them? Should I mention that ICU at home?
Patrik: Say again?
Tim: I’ll just mention to them the ICU at home?
Patrik: I think you need to start to plant the seed, you know? You need to start planting the seed saying look, you’re talking to Intensive Care at Home people. We can take her home on a ventilator. You’re talking to HCF. I think you need to start talking about that, especially since they now start talking about futility.
Tim: Yep. Because they’re going to try and-
Patrik: Absolutely, they will be in your ear from now on, every day.
Tim: And they can’t just sort of do it without permission? Or how does that work?
Recommended:
Patrik: That’s a good question. So, obviously you refuse to sign the NFR-
Tim: Yeah.
Patrik: Right? And they didn’t obviously over… they can’t override you, but even though sometimes they’re trying. But it sounds to me like you’ve definitely been standing your ground, they know by now you’re not a pushover.
Tim: Yep.
Patrik: Right? So otherwise they would have said to you, “Oh Tim we don’t really care what you want, we just sign… we just put an NFR form on her file.” They didn’t say that, right? So, you… look, the NFR issue is very grave. What do I mean by that? The New South Wales… there’s a New South Wales policy from the Department of Health that says that, in the ideal situation families need to give consent, right, but that it can be a medical decision only, right?
Tim: Yeah.
Patrik: So, it’s a bit grave, and that’s why it’s so important that you keep saying no for now.
Tim: Definitely, yeah, I understand.
Patrik: Right? And that’s all you’ve got to do for now. I think that’s it for now, really, or do you have any other questions?
Tim: No, I think that’s it, really, yeah.
Patrik: Just… we need to get prepared for Monday. Plant that seed with Intensive Care at Home.
Tim: Okay. Do that today?
Patrik: I think so, I think so. To plant that seed with Intensive Care at Home. Then Monday, talk to HCF. The other thing that I’ve seen with many public hospitals is another strategy to buy time is potentially to get her to Stamford, because for HCF it doesn’t make a difference, all right?
Recommended:
Tim: Okay, yep.
Patrik: But, but for Stamford it will make a difference, because they want the bed.
Tim: Yes, I understand.
Patrik: Right, whereas in the private system your mother is a customer.
Tim: How do we arrange that?
Patrik: Yeah, that would be fairly easy. So, I can tell you that, maybe a year ago, I helped a family to go from Leighton Public to Stamford. It’s pretty much a phone call to the bed manager, right? Because the Private wants to fill their beds.
Tim: Yep.
Patrik: Right? The only issue that I have… well it’s not an issue, it’s just experience, unfortunately… excuse me. Stamford you’d be dealing with the same doctors. Stamford ICU, same doctors.
Tim: Really?
Patrik: Yeah, yeah. Same doctors. There may be the odd different one, but they’re they… you know, out of, I don’t know, 10 consultants, out of 10 ICU consultants at Stamford Public, there would be 8 at Stamford Private.
Tim: Oh?
Patrik: Right, yeah. But, here is where it gets important, and that’s probably something you want to find out as well. The oncologist, as well as the respiratory physician-
Tim: Mm-hmm (affirmative)-
Patrik: Ask them if they have admitting rights at Stamford Private. And they most likely will.
Tim: If they have the what, sorry?
Recommended:
Patrik: If they have admitting rights.
Tim: Oh, okay.
Patrik: Right, and I’ll tell you why this is important. If your mother was to go to Stamford Private, she needs to be admitted under a doctor who has admitting rights there, okay?
Tim: Oh, okay.
Patrik: There is a very good chance that, either Darren Mc Millan or Aaron have admitting rights at Stamford Private; very high chance.
Tim: Okay.
Patrik: Right.
Tim: I’m not sure the professor does, because my mum wanted to go to the private hospital and he said he doesn’t do any work there.
Patrik: Okay, and when you’re saying the professor, that is the oncologist?
Tim: Yes, Professor Mc Millan, yeah.
Patrik: Right, okay. But she could potentially be admitted under Dr. Ives.
Tim: Oh, that’s true too, yes, definitely.
Patrik: Just give me one sec, just give me one sec. So, the respiratory physician is Anthony Ives, I-V-E-S?
Tim: I think that’s how he spells it, yes. I didn’t… I asked him his name and he told me that the one.
Patrik: Right.
Tim: I can ask again if you want.
Patrik: Right, just give me one sec, just give me one sec. Doesn’t come up on the Stamford Private. That’s okay. Look, you’ve definitely got to ask the question. It’s not impossible for your mum to go to Stamford Private, even if neither doctor, Ives not Mc Millan have admitting rights. It’s just going to be a little bit more difficult. But the bottom line is Stamford Public ICU wants her out.
Tim: Yes.
Recommended:
Patrik: Right? You know, they don’t care whether she’s going to Stamford Private or whether she’s going to die. Sorry to be so frank, but that’s the reality.
Tim: Yep.
Patrik: All right. They don’t really care, all they want is, they want her out, right? So, by suggesting that, in the interim to go to Stamford, they probably will help you even.
Tim: Really?
Patrik: Yeah, they may, they may. Again, it’s a matter of finding out, it’s a matter of suggesting, obviously Intensive Care at Home, but also suggesting to buy time at Stamford Private. Because that could stop them from talking about end-of-life, talking about futility, all of that. Seen all of that, Tim, seen all of that.
Tim: Yep.
Patrik: But the private healthcare system is different, it’s very different because, again, a patient is a customer.
Tim: Not a liability.
Patrik: It’s not a liability, it’s an asset, if you will.
Tim: Mm-hmm (affirmative)-
Patrik: Right? So, it’s a matter of finding out… you know, by you mentioning that, find out what they say.
Tim: Okay, I’ll mention that today, yeah, definitely.
Recommended:
Patrik: Right. So now you can start talking to them, but it’ll be on your terms, you know? You’ve got suggestions.
Tim: Yep. No, I appreciate that.
Patrik: Right. And end-of-life is not a point of discussion for you in hospital. It could be a point of discussion for you at home, but at the moment it’s not a point… you know, if they start that argument, just say, “Look, it’s not a point of discussion”, right? And you can also refer back to Mc Millan, who’s way more positive.
Tim: Yep.
Patrik: Right? You can refer back to what he said. So, have that argument lined up.
Tim: Yes. A hundred percent.
Patrik: Right? So, you’re prepared-
Tim: I really appreciate it.
Patrik: You’re prepared.
Tim: Yep. Oh, thanks very much, thank you.
Patrik: You’re very welcome. We’ll talk on Monday, but if you need anything urgent please get back to me, alright?
Tim: I will, no, I will. I appreciate that, and thanks for taking my call.
Patrik: You’re very welcome.
Tim: I’ll chat to you on Monday sometime-
Patrik: Okay, okay.
Recommended:
Tim: Thank you very much.
Patrik: You’re very welcome.
Tim: I will talk to you soon.
Patrik: All the best, Tim.
Tim: Okay. Cheers, bye-bye.
Patrik: Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!