Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
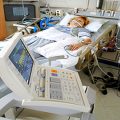
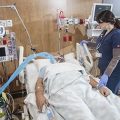
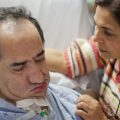
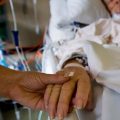
In this week’s episode of ““YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Stephanie as part of my 1:1 consulting and advocacy service! Stephanie’s mother is a post cardiac arrest patient in the ICU and Stephanie is asking if the families with loved ones in ICU have to deal with all of this alone.
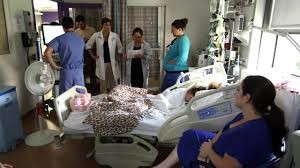
My Mother is in the ICU for Post- Cardiac Arrest Care. Why Is She Having Seizures and isn’t Waking Up. I’m Tired of This Situation. Help!
Stephanie: Yes, okay. Yeah, we gonna’ write all of this down.
Patrik: And also.
Stephanie: And you can ask them too at the meeting.
Patrik: And also, in order to get somebody, you know to get them out of an induced coma, again, you wanna stimulate them. It’s a tricky one with Carmen because you don’t want to stimulate too much because.
Stephanie: Right, because of the heart.
Patrik: Yes, but not so much of the heart, because of the seizure.
Stephanie: Okay, got you.
Patrik: But it’s a tricky one.
Stephanie: Well, we’ll let them do it, we’ll see what they say. We’ll ask them, that’ll be one of our questions on Monday.
Patrik: Absolutely.
Stephanie: Are you giving Carmen any type of physical therapy? Any type of stimulation? What we’re doing, Miranda said, tell them about the songs Miranda, that somebody told you that it’s good to talk to them and give them mental stimulation. At one point when they were on the…hey Miranda, Amy.
Recommended:
Miranda: Yes.
Stephanie: At one point when they were, when she was I think on the sedative or something, they said, “Just let her brain be quiet”. But then Miranda said, Miranda was talking to some friends, says well, “You need to let her hear some songs”, they made us stop playing the music. It was nice and soft music. But they said, “No just let her brain relax”. What is your experience Patrik? That’s what I wanna know.
Patrik: Look, on the one side of things. It’s a tricky one. On the one end you want to have low stimuli because you don’t want to trigger any seizure. On the other hand, I still haven’t seen what she can do. You know it’s a fine line between not triggering any seizures, but also trying to find out can she wake up, what does it look like, you know?
Stephanie: I can understand that because. Miranda, didn’t you tell me that when you were talking to our mother, that’s when she had, when you call her, “Mommy, mommy”, then that’s when she end up havin’ a seizure or the brain storm? Are you there? Did you have to go into the building?
Miranda: No. I’m just looking at something. Stephanie?
Stephanie: Yes.
Miranda: Okay.
Stephanie: Did you hear my question?
Miranda: No Ma’am.
Stephanie: Okay, okay. You have to send a message.
Patrik: So it’s a tricky one.
Miranda: I’m back on the walkie talkie.
Stephanie: Oh okay, on your job.
Somebody’s beeping your walkie talkie?
Miranda: No, not yet. I just want to make sure, at night time they start acting sometimes. Just around the time some of the cars start coming out.
Stephanie: Okay, do that one last thing and we’ll let you go if you can. You just let us know when.
Miranda: I’m ready.
Stephanie: So the questions, I keep forgetting my question. About the mental stimulation when she had the seizures. You said when you started talking, you said when you start talking to her and praying with her or whatever it is, you call her, “Mommy, mommy, I love you” and this that and the other then that kind of stimulates her brain and you said that morning, you were doing something like that, fill me in.
Miranda: I just talked to her and just tell her about everything and don’t worry about.
Recommended:
Stephanie: I don’t think he can hear you Miranda.
Patrik: No, I can’t.
Miranda: What about now?
Stephanie: Yeah, I think a little bit better. Now just a little bit louder.
Miranda: I just told her about the dog. Like I talk to her a little normal, but I don’t be having a lot of stuff to say because it’s just really, I’m having a lot of anger. I feel weird now. And thank God! I got my sister supporting me and my family because I just feel very, very weird. I just don’t want to like lose it.
Stephanie: We not gonna’ lose, we not gonna’ let you lose it honey.
Miranda: But it’s just like my thoughts, I can’t think right now.
Patrik: And I understand Miranda. At the moment, you are working night shift is that correct?
Miranda: Well, this my part time job.
Patrik: Right. Because look.
Miranda: And I was just thinking like should I take a leave of absence from work? But of course I would have less if I do that. I was also trying to figure out, which I’m not sure if you know anything about it, but I was going to purchase supplemental insurance for my mother. They saying that supplemental insurance is better than this Medicare aid and BIG.
Patrik: Most likely yes, but I wouldn’t worry at the moment about insurance, I really wouldn’t because if it is an insurance issue, the insurance will contact you.
Miranda: Say that one more time.
Patrik: Yeah, if you think it’s an insurance, it doesn’t look to me like the situation is an insurance issue. If it is, they will contact you. Right?
I wouldn’t worry too much about.
Recommended:
Miranda: See, I would like try to talk to my mother and I would. Don’t you know how somebody eyes just like kind of, she hasn’t done it, but they’re saying that that’s just a part of the brain moving. But I’ve seen in my opinion when I talk to her, her left eye, a tear drop come down.
Stephanie: What? You didn’t tell me that.
Miranda: Well it happened two or three times I think.
Stephanie: Wow.
Patrik: That’s good.
Miranda: But what my cousin was telling me the other day, yesterday which was kind of stressing me out and putting more stress on me and she’s like well you need to be at the hospital more where you can talk to your mother more and your mother may come through because of you. But it’s just, I don’t know about, I don’t think I like looking at the ventilator in her mouth no more, like her tongue hanging out and be like…
Patrik: Yeah and that will change with the trach.
Miranda: Some people say with the tongue hang out that mean that they not there.
Patrik: No, that’s a misconception.
Stephanie: Go ahead, go ahead.
Patrik: That’s the misconception.
Stephanie: Patrik dear.
Patrik: That’s the misconception. It looks terrible, I’ve seen it many times, the tongue hangs out, it doesn’t look nice and I get it. And that’s why a trach would look so much nicer, but just because somebody’s got their tongue hanging out, does not mean they are in a vegetative state or they can’t recover, it’s just Intensive Care treatment.
Stephanie: People making assessments of stuff, but they don’t know what they’re talking about.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: It looks horrible, I know it looks … you know, you’ve got to see, to a degree, I am desensitised because I’ve seen all of this. So to a degree I’m desensitised. It doesn’t look nice, I know that, but it’s just part of what it is.
Stephanie: Part of the process, yup. So whoever that person was that told you that about her tongue hanging out. I mean if you had a thing in your mouth, where the hell I’d say would your tongue be okay?
Patrik: That’s right, that’s right.
Stephanie: You’d rather it be hanging out than back down her throat. I don’t mean to mean gruesome or graphic or anything, but I think I’d rather have it just lying there more so than anywhere else. Because how she gonna’ close her mouth, if can’t close her mouth, where’s the tongue gonna go? That’s just common sense. And I think her tongue was nice and pink. It was darker, it looked like she may have bitten it, but it was nice and pink and looks healthy to me.
Miranda: It’s because I want the family be mindful that I am trying my best to be strong, but it’s just…
Stephanie: Can’t do it.
Miranda: ‘m my mother’s child, I’m ready to run.
Stephanie: Fight or flight, yeah.
Patrik: And you know, the other thing that’s important Miranda is, a situation like that, as you can already see, a situation like that is not black or white. Right? It’s not, you know there are a lot of grey areas and there are a lot of grey areas. You know, it could be life, it could be death, it could be somewhere in between. We have no idea how long the process is going to take. There are so many grey areas, it’s not clear cut and that makes it all the harder.
Miranda: A part that’s difficult for me is if she do come through, when she comes through, will she be herself? And when your parent has already told you that they don’t want something, it scares me.
Stephanie: You have to cross that bridge when you get to it.
Recommended:
Patrik: Yeah, exactly. And the reality is Miranda, there’s a very high chance that if she survives, she won’t be herself at the time when she leaves Intensive Care. There’s a very high chance that she won’t be herself at that point in time. But then, you still have to ask the question, “Does she want to live”? Just because she isn’t herself, doesn’t mean she doesn’t want to live.
Stephanie: Amen.
Miranda: So what is quality of living?
Stephanie: Process. You gotta get there.
Miranda: Well maybe Stephanie you’ll explain more and help me understand more.
Stephanie: No, go head Patrik. You wanna answer that? You wanna say something to that? You wanna speak to that because
Patrik: Say that one more time please Miranda. Can you say that one more time please?
Miranda: I just was saying overall my sister maybe she can help me recap or understand more later.
Stephanie: No, no, no. I want you to tell him what you just told me, not by me helping you recap it for you, but the part about, I just want to know, when she, whatever you were saying about when she get to that point. Say that again Miranda.
Miranda: What I have a fear of is when she do come out, if she not herself, will she be upset at me? You know what I’m saying?
Patrik: Oh I see. I see what you’re saying. I can’t-
Miranda: I know, she said she don’t want to be in that, like if my mother all did written. I mean you can half see and believe the best.
Patrik: I hear you loud and clearly.
Recommended:
Miranda: My mother is not somebody that wanna just be like, sometimes I be like will she even fight if she come out of it. Like if it’ worth it.
Patrik: Look, is recovery after Intensive Care hard work? Sure. It is hard work. I mean as you can already see it’s not an easy situation, right. Will she be angry at you? I can’t really answer that question for you. You know my area of expertise is in Intensive Care. I can tell you that when she wakes up, hopefully she does wake up, when she wakes up, I don’t think that’s the first thing going through her mind is, “Who has made decisions for me while I’m in a coma” or whatever. I don’t think that will be the first questions running through her mind right. That’s not what I’ve experienced.
I mean, will those questions come up down the line? Most likely. Right and it would be good if those questions came up because that’s a sign that your mother actually can think. Right? But getting to the point, is again, too far in the future and I mentioned again in the beginning, living in the future, I think it’s just complicating things.
Stephanie: Yes, too stressful.
Miranda: Yeah, that’s how y’all already know that’s how my brain is, but at the same token I just know that this type of situation takes a toll on the family.
Patrik: Oh totally, totally.
Stephanie: Everybody’s life changes.
Miranda: Everybody cannot be selfish, you know what I’m saying.
Stephanie: Helpful. You be havin’ to handle this all by yourself. I got you.
Miranda: Right. And it’s like-
Stephanie: You gotta work and how you gonna do that and go to work and do this and do that. How you gonna take care of her if you’re the only single child. You know people say they gonna help, they help for a while and they stop.
Patrik: Yeah, absolutely
Stephanie: That’s where she’s getting at. Overwhelmed.
Recommended:
Patrik: And look Miranda, I know you’re on a night shift. I’ve been a registered nurse, I’ve done many years of night shift. I know how draining that is. So you’re not in a good spot, I get it. You know. This situation would be overwhelming for anyone.
Miranda: This is like, “I want to be at the nursing home but … “Sorry, I want to be at the hospital but then it’s difficult to look at … I keep having a lot of anxiety but then I can’t even remember my thoughts. I want to be there, I want to get some sleep. I’m tired. I’ll be tired.
Patrik: Yeah. And you need to get some sleep.
Stephanie: That’s number … that’s one of the critical things that you said in one of your blogs online Patrik.
Patrik: Yes.
Stephanie: One of the biggest mistakes that family do is that they get up there and they stay 24 hours and you just have to, in a sense, to some extent, trust the staff, even though … you know what I mean?
Patrik: Yeah.
Stephanie: If you don’t take care of yourself, you can’t take care of her.
Patrik: That’s right.
Stephanie: You’ve got to get your rest. There are times when-
Miranda: If you look at me, this things stressing me out about how … she thinks I don’t get enough sleep which overall I think I give her the detail of the sleep but it’s difficult. And my brain … I think that maybe a reason why I keep having brain full. I’ve been feeling weird.
Stephanie: That’s stress.
Miranda: Or if I’m driving, I do not know the way I’m driving, I have never gone through this in my life.
Stephanie: Stress, you’ve got to get. Make sure you get some help too. You get to your therapist, talk to them and find something natural that can keep your calm, calm your mind down. You know what I mean? If you have to get any kind of tranquil, whatever you call it, some anxiety medication, then get it.
Recommended:
I know you don’t like that kind of medicine, but if that’s what you need, whether natural or otherwise, do something to feed your mind, to feed your brain, to feed yourself, all of those things, to be able to function because you want to be able to function, not just in regards to mom, but just with these jobs you’re handling and then you’ve got the extra, like you said stress on top of that.
Number one, you take care of yourself and you get on the aeroplane and when the oxygen level starts to fall, this is the first thing you do is put that mask on yourself first before you try to help somebody else. You have to help yourself first, right? You get on aeroplane, and nobody is going to tell you that. Even if it’s for your own child. And so you put that air on yourself.
Patrik: Yes. Correct. That is such a good point of view, Stephanie. Miranda, you are the most important person in all of this. You are the most important person in all of this because you are having a lot of responsibility in this situation. You’ve got to make sure you’re okay and you are well and you are clear in your head. By looking too far ahead, that doesn’t help you with clarity. Tomorrow is the day that’s most important. Once tomorrow’s over, Monday is the day that’s most important.
Stephanie: Remember that.
Patrik: There is no … it just hinders your situation if you’re looking too far ahead.
Stephanie: Very counterproductive. You cannot look too far ahead. And yap. Just one day at a time. That’ll mess anybody up because you go on with what if, what if this and what if that? That’s enough to drive anybody crazy.
Patrik: No.
Stephanie: You just to get to, just one day at a time, and then … I love how you put that, Patrik. Say that again, that tomorrow’s the most important?
Patrik: Yeah. And then Monday is the next most important, right?
Recommended:
Stephanie: And then Monday is the next most important
Patrik: Yeah. Then it’s Tuesday.
Stephanie: When Monday comes-
Patrik: Worry about Monday, and then you can worry about Tuesday. Look, you would’ve heard people saying that. It’s like a phrase, but you would have heard people saying, “Live in the moment to be happy.” I know this is not a happy situation, don’t get me wrong, but there is truth in “Live in the moment.” Confront what’s happening at the moment because that is more than enough to confront, let alone worrying about future.
Stephanie: Yeah. And we are God-fearing people. One of the scriptures says, “Sufficient for one day, one day has its own anxiety.” Something like that. One day has enough anxiety.
Patrik: That’s exactly right.
Stephanie: If you’re thinking about the next day, my goodness.
Recommended:
Patrik: It’s a full-on situation. But the other thing … and I’m not sure whether that’s going to help you or not, but I am a big believer that everything in life happens for a reason. I do not know the reason for this situation. By no means, do I claim that I know the reason for this situation. But I do believe things in life happen for a reason. I do not know what the reason is, but maybe there is a reason that you know.
Stephanie: Right. And maybe it will show itself down the line if not now.
Patrik: Correct.
Stephanie: Yeah. That’s what my niece Natalie said at the table. You’re saying that too. I believe everything happens for a reason. But whatever the reason, we walk through the storm.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!