Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
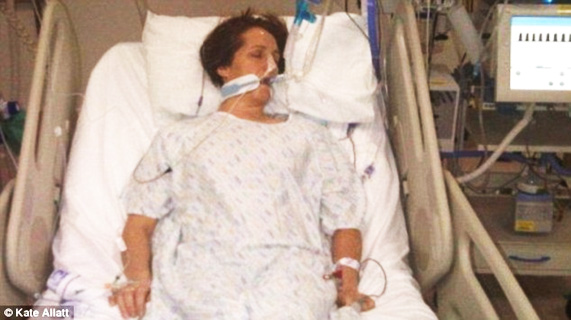
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Stephanie as part of my 1:1 consulting and advocacy service! Stephanie’s mother had a cardiac arrest in public transport and is now in ICU post CPR, and she is asking if Tracheostomy is the only option for her.
My Mother is in the ICU Post Cardiac Arrest. Will She Be Able to Recover and Wake Up?
Patrik: Okay, so now were complete.
Miranda: Yes.
Patrik: Okay, wonderful.
Stephanie: Roll call? You want to take a roll call, Mr.Hutzel.
Patrik: Yes, I can. Can everybody here me?
Stephanie: Yes.
Miranda: Yes.
Tonette: Yes.
Rebecca: Yes.
Recommended:
Patrik: And Stephanie, can I just ask, so the email that you sent to me, with the question, everybody on the call has got the same questions?
Tonette: Yes.
Stephanie: That is correct.
Patrik: Wonderful, wonderful, okay. Okay.
For me to clarify, Stephanie, or for anybody, how long had Carmen been in intensive care for? How many days has it been?
Stephanie: Okay, I’ll let Miranda answer that.
Miranda: Okay, um, she came in last Monday, so…
Patrik: Four days.
Miranda: Nine days.
Patrik: Oh, nine days, so, oh, okay, Monday the tenth, Monday the tenth of September.
Stephanie: Mm-hmm (affirmative)-
Patrik: Okay.
Stephanie: Ten days.
Patrik: Okay, and there’s a couple of other things that I need to clarify before I then go into answering the questions.
You’re talking about massive heart attack, but you’re also talking about that the co-workers started CPR. That to me, indicates that she would have had a cardiac arrest not only heart attack. Do you-
Stephanie: Correct. Myocardial infarction, correct.
Patrik: Okay, but a myocardial infarction is not a cardiac arrest. That’s why I need to-
Stephanie: Oh.
Recommended:
Patrik: That’s why I need to clarify. If CPR was started, she must have had a cardiac arrest.
Stephanie: Correct.
Patrik: Right. So then we can say, I mean it’s, then we can conclude that the heart attack led to a cardiac arrest, and that’s often what happens. I mean if CPR was commenced, she would have had a cardiac arrest.
And just-
Stephanie: Mm-hmm (affirmative)-
Patrik: And the other thing that I need to clarify, is so you think that she had three to four minutes without oxygen, is that correct?
Stephanie: Yes.
Miranda: I’m not sure.
Patrik: Right, right. That’s just what, who guesses that you had three or four minutes without oxygen. Where, who is saying that?
Stephanie: Miranda?
George: That’s based on the timeline of when she walked to her bus.
Patrik: Right.
George: From greeting people and answering the bus driver. So, nobody knows exactly.
Patrik: Right.
George: The timeline.
Patrik: Okay.
Miranda: Actually, I went up there today, and they actually walked me through everything. They walked me through where the bus was, and down, how they got her off the bus, etc. and everything came from, pretty much, quick. What they are saying, that’s all I can say is what they were saying.
Recommended:
Patrik: Okay. Yeah, no that’s fine, that’s fine. And, from then, the paramedics rushed her to hospital, and she went to have the stent placed straight away? Or was that day after, do you know?
Miranda: Well what the people told me, today, was that they were doing the CPR in the ambulance was trying to make sure that she came through, they were waiting, trying to get her pulse. She had a soft pulse, the whole time, from what I hear-
Patrik: Right.
Miranda: And then, they worked on her, and as soon as they was able to get her, I guess, a better pulse, then they bring her to the emergency room and that’s when they did the surgery right away.
Patrik: Okay, okay, no, no, that’s fine. That’s all I needed to clarify then, then I can go into the questions straight away.
Maybe before I go into the questions, I should, you know, you’re talking about, Stephanie, in the email you say she had the following tests: CAT scan, all clear, MRI, nothing definitive, passed breathing test today, has eye reflexes but slow, feet reflexes but when pinched behind the legs, bodily functions are working well.
So with that, I would say, that’s it’s very unlikely that there’s any brain damage. It’s unlikely. Can’t be ruled out, but it’s unlikely.
Stephanie: Mm-hmm (affirmative)-
Patrik: Right? And even, you know, even if she may have been from three to four minutes without oxygen, if people were performing CPR, and as long as CPR was effective, you know, that should minimise the risk for causing hypoxic brain injury.
Does everybody know what I mean by a hypoxic brain injury?
Stephanie: Yes.
Tonette: No, I do not.
Recommended:
Patrik: Right, so a hypoxic brain injury’s basically, if the brain can be without oxygen for up to three minutes before irreversible brain damage is caused. Right? So, in a cardiac arrest situation, if CPR isn’t commenced straightaway, the risk for the brain of getting oxygen throughout a cardiac arrest is pretty high.
That’s why it’s so important that people start CPR straight away, because there is that three minutes time window, okay? And if the brain has no oxygen for more than three minutes, that’s when a hypoxic brain injury can be a result of that, right?
But, with everything that you’ve shared, there is no indication at the moment that she has a hypoxic brain injury.
Tonette: Ahm… Who ever wanted to say something-
Stephanie: Go ahead, Miranda-
Miranda: what…. – my concern is that I just don’t know if everything that the employer is saying is 100% correct.
Patrik: Sure, sure.
Miranda: They’re saying that’s what happened, but I don’t know because I wasn’t there.
Patrik: Absolutely-
Tonette: Okay, can I interject right there from what I was told by the owner of the bus company?
Edwin said that he didn’t know how long that the incident happened, but she was on the bus and what happened that somebody came by, the nurse, and started administering CPR. So they don’t know the exact time and I asked him when he called me. So that’s what I wanted to interject.
Recommended:
Patrik: Right, okay, okay. You see, the reality is, we will probably never find out. It’s just really, it’s good to have some timeline to work with. I would be more interested, with all of this, and we’re coming to, with all of this, especially with the CAT scan of the brain as well as the MRI scan of the brain, have you, as a family, have you spoken to a neurologist in all of this?
Miranda: That’s what we have a meeting for tomorrow.
Patrik: Right, so you are going to-
Miranda: I think my family talked to them, I haven’t.
Patrik: Right, and what’s the Neurologist say?
Rebecca: She’s saying that after she watched the video and the EEG scans that she can’t give a definitive answer, because-
Patrik: Right-
Rebecca: Until they do the weaning-
Patrik: Right
Rebecca: So that, she can make the best answer even with us telling her about Carmen’s quality of life previously and her health conditions previously.
Patrik: Okay. So that means an EEG test has been done as well.
Rebecca: Correct.
Stephanie: Yes.
Rebecca: She’s been on video EEG the entire time.
Stephanie: Mm-hmm (affirmative)-
Patrik: Okay.
Stephanie: Yes she has.
Recommended:
Patrik: Okay, wonderful, wonderful. So they’re doing all the right things, that’s good. So then, let’s go, before we go into answering the questions, has any one of you heard of the term GLASGOW coma scale?
Stephanie: No.
Miranda: No.
Patrik: That’s okay, then we won’t go there. That’s okay, then we can bring it up later. That’s okay. Maybe it something-
Tonette: They did mention that, Patrik. They did mention that terminology. GLASGOW coma scale.
Patrik: Yup. Have they-
Tonette: Yes.
Patrik: And that’s attached to a number. And I’ll give you the very brief version. The GLASGOW coma scale is a neurological test. So the numbers range, the lowest score is a three, and the highest score is a 15. So while we’re on this call, we are all at GCS three, uh, GCS 15, sorry.
If a person is fully compos mentis, is walking, talking, oriented, that’s a GCS 15.
A person in a coma, that’s doing nothing at all, is a GCS 3. With the reflexes that you’re sharing in the email has eye reflexes and feet reflexes, right?
That’s a minimum of a GCS of a 5, a minimum. Could be probably, somewhere between 5 and 8 I would think at the moment. That Carmen is at. Right?
When we come off this call to you, I will email you more about the GLASGOW coma scale, because it’s information that you will need for the meeting tomorrow.
Recommended:
Tonette: Amen.
Miranda: Thank you.
Patrik: Right, so then, because it’s quite an important score, you know to also determine how quickly she is waking up, is there any brain damage, quite important to score against that measurement.
So, then, let’s move on to the questions, unless you have any other questions with everything that I’ve mentioned so far.
Miranda: No, I don’t.
Patrik: Okay, everybody following?
Tonette: Yes, you in charge. We don’t have any questions.
Patrik: Okay, okay, alright. Let’s move on then to the questions.
So how can you be sure that they are weaning your, Carmen off the ventilator instead of just doing the tracheostomy as a first option?
So, that’s one of the most important questions you can ask in all of this, right? And, it’s almost like a make or break question. It’s good that you realise that this is an important questions. So the first thing that you need to understand, the goal for anybody in intensive care on a ventilator with a breathing tube should always be to wean them off the ventilator.
That should always be the goal. No matter what people say, that should always be the goal. Now, a tracheostomy has its time and its place, if weaning efforts, or I should say, if multiple weaning efforts have failed, right?
Tonette: Say that again, if multiple what?
Patrik: If multiple weaning efforts-
Recommended:
Tonette: Yes-
Patrik: Have failed.
Tonette: Amen.
Patrik: Right?
Tonette: Right.
Patrik: So one of the questions you should be asking them is, “Are you trying to wean?” And if so, “Is she passing the weaning tests or not?” Right?
That’s one of the questions. But here is another thing that’s incredibly important, right?
Are you feeling under pressure at the moment that you have to give consent to a trach? Is that how you feel? That’s how they sort of?
Tonette: Yes.
Patrik: Right.
So they’re basically telling you, “You need to make a decision whether she should have a tracheostomy or not.”
Tonette: Yes.
Patrik: Right, okay.
Rebecca: Mm-hmm (affirmative)-
Patrik: Have they given you any timelines?
Miranda: No, no, no, no. When I talked to the doctor, he said that he wanted to just-
Rebecca: What? I’m sorry, I couldn’t hear you.
Recommended:
Miranda: Actually, he said that, let me come out of the room, he said that he wanted to take her off the ventilator.
Patrik: Without doing a trach?
Miranda: Correct.
Rebecca: Oh good.
Miranda: Correct.
Patrik: Okay.
Miranda: He said he wanted that to happen. One second, let me walk to my… I’ll be back, Mom. Okay.
Stephanie: Are you there? Are you there at the hospital, Miranda? Okay.
Miranda: Mm-hmm (affirmative) – and they’re doing their… they’re doing their rounds, too.
Patrik: And, he didn’t, sorry, Miranda, I didn’t hear that 100%. So they were quite happy to take her off the ventilator and they didn’t say that if they took her off the ventilator she wouldn’t survive? They didn’t say that, did they?
Miranda: No, they didn’t-
Rebecca: Yes, they did. I was there. I been there the whole time. They said that.
Stephanie: Let Miranda, let Miranda finish what she has to say, and then you can tell them what you heard, Rebecca.
What did you hear, Miranda?
Miranda: They basically said that her quality of life is how she is, and they said that they wanted to see what would happen. Let nature take itself. That’s the words that they said to me.
Recommended:
Patrik: Okay, okay. Alright. I’ll come to quality of life as well, I think it’s a very important issue in all of this. I’ll come to that as well.
So, here is, let’s just say, and let me ask you another question. If they did a tracheostomy and they did it in the next, let’s just say they do it in the next three days, have they mapped out the next steps from there?
Have they mapped out what’s next for Carmen if they did a tracheostomy?
Rebecca: Yes.
Patrik: So they would send her out to LTAC, would they?
Rebecca: Right.
Patrik: Okay, okay. That’s good, that’s good-
Rebecca: Tell me what that acronym stands for.
Patrik: Long term acute care facility.
Rebecca: Okay. But it would be inside the hospital.
Patrik: Okay, she wouldn’t have to change hospitals?
Rebecca: No, it would be right there, and they have a vent unit.
Patrik: Yeah.
Rebecca: That specializes, supposedly, in a, you know…with the airway.
Patrik: Weaning yeah, yeah. Okay, okay, that’s good- You mentioned that, go on, go on.
Tonette: The neurologist did tell me though that their vent unit is just a transitional unit. It’s not her long-term acute care unit.
Patrik: Right. Okay, okay.
Recommended:
Miranda: So what happened, I missed it. I missed it because the doctor was-
Tonette: Their vent unit is not a long-term care unit. It’s a transitional unit.
Miranda: That’s right.
Patrik: Mm-hmm (affirmative) okay, okay. So what is important to know with the long-term acute care, we see especially in the United States, that a tracheostomy is often illegal to get patients out of ICU to long-term acute care as quickly as possible? Why? ICU beds are in demand, right? From an insurance perspective an LTAC is way more cost-effective. From my perspective and my experience talking to people in a situation like yours every single day, an LTAC, most of the time, is a disaster zone. Right?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!