Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Do We Know If Our Critically Ill Mom in ICU Is Ready To Be Weaned Off ECMO?
You can check out last week’s question by clicking on the link here.
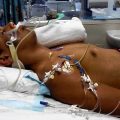
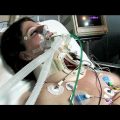
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is on ECMO. Juan is asking if he should trust the ICU team with their medical management for his critically ill mom in the ICU.
Should I Trust the ICU Team with Their Next Steps Whilst My Mom Is Critically ill in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Patrik: Hi Juan. How are you?
Juan: I’m fine. Thank you. How are you, Patrik?
Patrik: I’m very well, thank you.
Juan: Okay. Great. I have Kevin and Mich also with me.
Kevin: Hi Patrik.
Patrik: Hello.
Juan: Hi. Hi. Great. Patrik, I’m going to start with just giving you an update on our talking points from yesterday. And then I’ll go into a status of today.
Patrik: Sure, okay.
RECOMMENDED:
Juan: Okay. Great. On the point about the arrhythmia and the potassium, they agreed, and they’ve actually increased the potassium.
Kevin: And the potassium today was around 4.2.
Patrik: Okay. And that is on dialysis?
Juan: They’ve not actually removed any fluid from the hemofilter today because she’s passing good urine.
Patrik: Okay. But she’s still on the filter?
Juan: It’s there. Yeah.
Kevin: It’s connected to the ECMO.
Juan: I think they turn it on and off.
Kevin: They clamp it every now and then. When they need to draw water from it, then they unclamp it. Otherwise, it’s just kept clamped.
Recommended:
Patrik: Right. Okay. Wonder why that is. The trouble with potassium, it’s a delicate balance. You need to check it almost every four to six hours. And if you’re giving, that’s great. If potassium is low, you need to give potassium. But by the same token, you also need to make sure it’s not going too high because then you’ve got the arrhythmia on the other end as well.
Kevin: Exactly. They’re making sure that it’s not going too high. They’re monitoring it regularly.
Patrik: Okay. Now that’s good. That’s good. That’s all they need to do. They need to monitor regularly.
Kevin: Yeah.
Juan: Right. On the point about pulmonary hypertension, they said that’s not something they’re concerned about anymore. Regarding your recommendation about the dobutamine.
Patrik: Can I just ask why? Why are they saying that pulmonary hypertension is not an issue?
Juan: Kevin, do you remember what the doctor said?
Kevin: No, not exactly.
Patrik: That’s-
Kevin: She just said that it’s not a concern anymore. It’s not an issue. The markers aren’t suggesting it.
Patrik: Right. Now, you’re telling me she’s got pulmonary fibrosis. Is that right?
Kevin: Right.
Patrik: If you Google pulmonary fibrosis, you will find that part of the issue with pulmonary fibrosis is pulmonary hypertension. I don’t-
Juan: We’ll ask again. I think we’ll ask several questions around that then.
Patrik: Sure. Right. I would. I would. It would be new to me that pulmonary fibrosis or cystic fibrosis would not cause any pulmonary hypertension. That’s all.
Juan: Okay.
Patrik: But I probably also agree that at the moment, as long as she’s on the ECMO, it’s still not a priority.
Juan: Yeah. I think maybe that’s the point. I think they’re prioritizing a couple of things right now for them to get the VA ECMO off maybe tomorrow or day after. Maybe that’s why, but yes, we will ask. We’re going to head down to the ICU after we speak so we can bring that up now.
Patrik: Right. Okay.
Recommended:
Juan: Okay. Regarding the Dobutamine and Milrinone, they said that yes, those are tried and tested drugs that they have used and that they do use generally. They said that it can’t be used more than two to three days, so they’re going to save it for when they’re doing the clamping.
Patrik: Really? I have seen … Okay. That’s a new concept to me. I have seen people on ECMO and on dobutamine for days, sometimes weeks.
Patrik: Again, and in all fairness, different hospitals have different protocols and have different approaches. But if you’re weaning someone off ECMO, I would argue that it’s not going to happen with a little bit of Dobutamine or Milrinone.
Patrik: Let me ask you this. What are they predicting as their next steps?
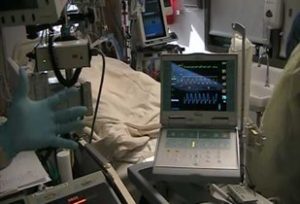
Kevin: They reduced the flows on the ECMO.
Patrik: Yup. I’ve seen that in the pictures.
Kevin: Yes. That has been tolerated well. They also stopped the Atracurium and Midazolam.
Patrik: Great.
Kevin: She’s only on Fentanyl now.
Patrik: Great.
Juan: And she’s tolerated that the whole day as well since the morning. And her BP has held as well.
Patrik: Great. Is she still on the sodium nitroprusside?
Juan: No.
Patrik: That’s off?
Juan: Yup. That’s off.
Patrik: That’s great.
Suggested links:
Juan: So through the night, she’s without the sodium nitroprusside, and then through the day today, at 10:00 AM … But at 10:00 AM is when they took off the Atracurium, and then a little bit later, they took off the Midazolam as well. They reduced it, and then it was gone completely.
Juan: For most of today in the last six to eight hours, she hasn’t been on either of them, and not on any inotropes as well.
Patrik: That’s great. And last time when they switched off the Atracurium and the Midazolam, she was fighting against the ventilator. Is that right?
Juan: Yeah. Yes.
Patrik: Right.
Juan: Then that is reduced now. She’s more in sync now. They said that there was one time when they, I think… Was it “Fentanyl?” No. Was it Midazolam?
Kevin: The Atracurium.
Juan: Off the Atracurium.” Sorry. When her BP dropped a bit, but then it settled down, so then they just left her as is. She’s fighting less now, and she seems calmer overall.
Patrik: That’s great. That’s great. That’s really positive. The other thing. On the pulmonary hypertension note, when you look at her PA pressures, her pulmonary artery pressures from yesterday, they were around 12, and today they are around 26. Again, I don’t buy for a minute that she doesn’t have pulmonary hypertension.
Juan: I’m not sure. I can’t remember actually if they said that she doesn’t have it or if it’s not a priority right now, but we can bring that up again, definitely.
Patrik: Right. Right. Okay. And what are they saying are the next steps now?
Juan: We asked them about the weaning study. Spoke to the doctor who handles the ECMOs. And we asked them about a weaning study, and I think she said that … Mich, what exactly did she say?
Kevin: She said that because there’s no exact rule book, they have guidelines. At the moment, they’re doing-
Juan: They’re also doing it by intuition and kind of judging her reactions to things.
Recommended:
Kevin: Like, they reduced the ECMO flow today, and it’s been about six to eight hours, and she’s handled it well. They said such like a study, they’re trying things out, and they’re seeing how she’s responding, and accordingly they’re making their adjustments or whatever.
Patrik: Sure. Sure. Okay. And what are they saying … Let’s just say they can take the V-A, ECMO off. What are they saying about the balloon pump?
Juan: I think they said that with her that she would need the balloon pump to support the heart still.
Kevin: And they’re going to see. I mean, it’s all very dynamic because they’re going to see how she responds to once they take the VA off what happens. Then they’ll decide if they can-
Juan: I think the VV will be needed for a little bit more, and they want to keep the balloon pump in, I think, while the VV is still on. I think.
Patrik: I’m still worried about … Great if they can remove the ECMO. If she needs the balloon, I’m almost bound to say it defeats the purpose.
Juan: I mean, they sounded quite sure about that though. We spoke to two or three different people, and all three of them kind of were like VA goes off first. I don’t know why that’s … I mean, it seems like there’s quite a certainty with them.
Kevin: It’s because VA is a larger catheter. And they would like to get that out first and then probably the VV. And as they’re taking the balloon pump, they’ll probably do that with a few inotropes if required. But from what it seems like is that the balloon pump would go out after the ECMOs.
Patrik: Yeah. But when I look at the balloon pump, it’s on one and one. I would argue by introducing some Milrinone and some Dobutamine, I would argue that would aid the process. And maybe they’re not quite introducing it yet. At the moment, they’re probably trying and seeing what is she doing without the Milrinone and Dobutamine. But it’s like, how can I explain this?
Patrik: They started with a balloon pump. The balloon pump wasn’t good enough. Then they went on to ECMO.
Kevin: No. They started with the balloon pump. Then they got off the balloon pump. It was not there for a week.
Patrik: I see.
Kevin: Yeah. For an entire week. And then after an entire week, suddenly there was a deterioration, and things started going downhill really fast. That’s why they added in the VA ECMO.
Recommended:
Juan: The balloon pump did its job in the beginning.
Patrik: I see.
Kevin: It did its job in the beginning. Came off. She was off everything. And then suddenly, there was that deterioration after the transfusion.
Patrik: I see. I see what you mean. Okay. Still, it feels a bit like VA ECMO is a crutch for the heart until it can walk again. Okay? But so is the balloon pump.
Juan: Is it not that because of the VA ECMO is a bigger crutch?
Patrik: It’s a bigger crutch. Yes. It’s a bigger crutch. I agree that it’s a bigger crutch. But there’s still both crutches. And the goal of a crutch is to walk without the crutch eventually. And-
Juan: How do you think we can bring up our concerns about why the balloon pump isn’t coming off first?
Patrik: Well, right. Well, that is exactly the question. And you’ve got to be blunt there. And … Very-
Kevin: What I-
Patrik: Go on. Go on.
Kevin: What I feel why they want to take the ECMO off first is because the VA has been on now for over two weeks.
Patrik: Yeah, I get that. I get that.
Kevin: Whereas the balloon pump has just been there four days now. I think they want to get that out as soon as possible.
Juan: Because that’s also affecting the hemoglobin and kind of it has a whole bunch of other issues.
Patrik: No. No. No.
Juan: Actually-
Patrik: No doubt about that. No doubt about that.
Juan: Sorry. There was one more point, Patrik, which came up today. They noticed that her right leg is a little bit more swollen than the rest of her body, which seems to have shrunk in size as the fluid has come out. And they believe that’s probably because of … I’ll just tell you what was it called. Venous insufficiency, I think that’s what it’s called.
Patrik: Yeah. Sure.
Juan: Venous insufficiency.
Patrik: Sure. Sure.
Juan: They did do dopplers. I think they did one in the morning yesterday and then one at night. And just to make sure that there weren’t any big clots. And those came out clear, but I think they found a small vein that has a clot. They did change one small catheter somewhere. And they’re just keeping an eye on that. They did mention to us that that’s something they’re monitoring closely, and if needed, once they remove the arterial cannula, then if needed, if that doesn’t settle down, then they remove the venous cannula to the arterial cannula so that the other leg can settle down.
Juan: I think I explained that correctly.
Patrik: Okay. I have not seen ECMO being weaned onto a balloon pump. I just haven’t. That doesn’t mean it has never happened just because you haven’t seen it. It just almost defeats the purpose, especially the absence of Milrinone or Dobutamine.
Juan: I think maybe this goes back to what they said earlier when they said that they put in the balloon pump, and then they realized that she’s actually doing better without the balloon pump or that she’s quite good without it. They sort of think that she doesn’t really need the pump. But they’d rather get the ECMO off and then pump, I think. Because she’s performed well even without the pump. It’s just that they put it in prophylactically, and then they realized that she’s actually doing okay, which I think surprised them. Maybe that’s the reason.
Patrik: Yeah. Look. Look. I mean, if you can come off balloon and ECMO without Dobutamine and Milrinone that would be the best case scenario. But I argue that with an ejection fraction of … Did you say 30 or 35%?
Juan: 30-35. Yeah. 32 to 35. I think they’re going to stop the ECMO tomorrow.
Patrik: Okay. I argue that with an ejection of fraction, let’s just say for simplicity 30%, plus Milrinone or Dobutamine, you get both the balloon and the ECMO off. You don’t need to be going from one crutch to another. The reason why I think the Dobutamine or Milrinone would be so important is getting rid of VA, ECMO as well as balloon … Again, we talked about infection risk yesterday.
Juan: Yes. Yes. Yes.
Patrik: The Milrinone or Dobutamine, the infection risk is much lower. There’s still an infection risk because it’s an infusion. But I still say I don’t quite understand why they’re not doing that.
Recommended:
Juan: I think we can bring this up with the ECMO specialist. I think we’ll do that.
Patrik: I think so. I think so. I think-
Juan: Because it’s not that they were averse to the Milrinone and Dobutamine. They were like, “Yeah. Those are great medications. We do use them.” And this was the opinion of one doctor. We can bring it up with the ECMO specialist and see what she has to say.
Patrik: I would. I would. I really would.
Juan: Okay. And you’re saying that it can be used for more than a couple of days?
Patrik: Weeks. Weeks.
Kevin: The reason she said they can’t be used, she said that the body develops a-
Juan: A resistance to it.
Kevin: A resistance to it quite quickly.
Patrik: Right. That’s new to me. And I’ll tell you why. I’ll tell you why. You remember yesterday we talked about the Impella?
Juan: Yes. Yes.
RECOMMENDED:
Patrik: Okay. The Impella is often being used for a bridge to a heart transplant. Now, that Impella can sometimes be in for months. And patients actually here, where I am, in one of the ICUs that I worked at, patients get the Impella. They are put on a transplant list, and they go home with the Impella plus either Dobutamine or Milrinone infusion. And that-
Juan: Okay.
Patrik: If you are on the Impella and a Milrinone or Dobutamine infusion, and you’re on a heart transplant list, you have no idea how long you are on the heart transplant list.
Patrik: It just doesn’t make sense from my experience.
Juan: Sure. Sure. No, that’s good to know. We can definitely discuss that then. I think we can push for it. Yeah.
Patrik: I’ll show you another thing. I will send you an ECMO weaning protocol. Just give me a second. I will send that to you now. It’s from one of the ICUs that I worked at. You can have a look at that later.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!