Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
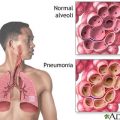
My Dad is Admitted in ICU Due to Pneumonia and Sepsis. How Do We Move Forward with my Dad’s Care?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Anna as part of my 1:1 consulting and advocacy service! Anna is frustrated about the ICU team’s negativity and vagueness about her dad’s condition and Anna is asking about the right approach so that her dad would have a positive outcome.
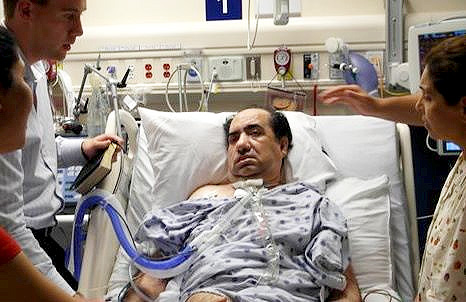
The ICU Team is Thinking Negative About my Dad’s Condition. How Do We Deal with it?
Hello Patrik,
Many thanks Patrik. I’ll request a copy of the CT brain scan report today and will then be in touch re: booking a convenient time to talk. I’ll just need to arrange for my 1 year old to be looked after so that we can talk in peace!
The ICU team have continually asked us do we think Dad would find life post illness acceptable. They said it would be an institutional life in a hospital setting, on permanent oxygen support. That he would likely be in a wheelchair and not be able to walk far. That he would need personal care.
Our response to that was that we felt Dad would accept an altered life as long as he had cognitive function – if he could read, watch films, see his partner, children and grandchildren, have visitors etc. He is psychologically a very strong person and we felt he would choose life over the alternative. In other words, we felt he could live with lung failure, but would not want to live with brain failure.
They said ok.
In recent weeks they have put the question again, saying, we don’t think your Dad will be able to eat or drink if he survives this (risk of aspiration?) and may not be able to have a speaking valve on his tracheostomy. This has worried all of us, but particularly my Stepmom.
The consultant said yesterday “so we only have one facility in the county that could house your dad or he would have to stay in ICU. That means an institutional existence for him and we don’t think that’s in his best interests”
RECOMMENDED:
I’ll be in touch as soon as I have the CT scan report.
Best wishes,
Anna
RECOMMENDED:
Hi Anna,
Thank you for sending this through.
I’m very sorry to hear that the meeting didn’t go quite as planned.
It’s disappointing the consultant doesn’t know what GCS your Dad is currently. I have attached a GCS score so you can have a look for yourself.
It’s a “typical” ICU situation, I have seen this hundreds of times and it will all come down to positioning.
As a next step let’s focus on a couple of things:
1) Let me know when you want to talk.
2) We will then focus on how you can remove the DNR.
3) We will also focus on how you can stop them from removing treatment.
4) Get the CT brain report.
5) We can talk about why your Dad isn’t “waking up”.
Also please have a look at the following two EBooks and videos here:
Let me know when you are ready to talk. You can book a time below or just let me know when it’s convenient for you. Ideally we’ll speak before 1pm UK time today but I can be flexible.
Kind regards,
Patrik
Hi Patrik,
Thanks so much again for speaking to me this morning.
So I’ve just arrived home from a rather frustrating meeting with one of the ICU consultants, Dr. Joeffrey.
My sister, brother and Stepmom all met with him.
He said he doesn’t feel Dad has made any improvements neurologically this last week. He says they don’t know why he isn’t waking up, and describes Dad as neurologically disabled. Conversely, my stepmom, sister and brother all said that they had noticed improvements this week, including:
- Squeezing their hand
- Following their conversation
- Smiling
- Laughing at family “in jokes” (as much as is possible with a tracheostomy!)
- Shaking his head to questions
Dr. Joeffrey said they are just not seeing that in terms of reactions and responses. He said Dad doesn’t respond consistently to commands by the medics and nursing teams, and that they would expect that by now.
I asked what sedatives he was on when he was mechanically ventilated from 27 April – 17 May. Dad’s nurse kindly collated them for me:
- Propofol
- Alfentanil
- Dexmedetomidine
- Remifentanil
He said they still can’t do an MRI as the pacemaker has kicked in a few times on the lower setting (they were hoping to remove it all together and turned it down from 60 beats to 30) and of course the model is not compatible with the MRI machine.
He said they remain massively concerned about his lung function, and the fact that he doesn’t have any ‘reserves’ to draw on. He said they tried to take dad off the ventilator yesterday but that his breathing became labored and that his heart rate went up.
His infection markers have come right down today; he said they would consider the infection gone. My brother pointed out that Dad has always struggled with coming off the ventilator when he’s had an infection; but that once it goes he tolerates it quite well. The doctor conceded that.
RECOMMENDED:
They sat Dad in the chair today for a few hours, but he is very tired and isn’t really responsive.
I asked about where dad scores on the Glasgow coma scale; The consultant said it wasn’t really relevant as Dad can’t give a verbal response. He basically said he couldn’t say.
I asked is it possible that Dad has critical care neuropathy/post Sepsis Syndrome – he said yes, we believe he has the former. I said could that impact on his ability to wake up? He said yes.
I asked what the CT scan showed and would it be possible to have a copy of the report; he said the report would say that it didn’t find any evidence of a major stroke. I will press for a copy of the report if you think it would be useful, Patrik?
I asked why they did a lumbar puncture. He was a bit vague, saying he knew it was discussed but hadn’t realized it had been done. He said it would have been to look at the proteins. (We were later told they were normal.)
My sister asked have they called in a neurologist to assess Dad/give a perspective; he said it isn’t something they would normally do in Dad’s case (?) He said the trouble with neurologists is that they would suggest lots of tests that take weeks and would also push for an MRI.
He said he thought the cardiac arrests Dad had probably caused brain damage. Conversely, two other consultants categorically told me it wouldn’t have – that they responded quickly, it reversed straight away, the quality of CPR was good and that his oxygen levels never dropped. It worries me that we are being given different interpretations.
We asked could we speak to a neurologist to at least put our questions to him/her. We said we need to understand what has happened to Dad, and that as his advocates we must explore everything. He said ok.
RECOMMENDED:
Dr. Joeffrey said it is the consensus among the consultant ICU team that Dad is not going to survive and that it’s not in his best interests to keep supporting him. I think they would like to withdraw treatment.
I asked what the position is re: DNR on his file – Dr. Joeffrey confirmed that he is DNR. We were never asked about that! Or gave agreement! I said we were not comfortable supporting a DNR now that we have seen (albeit small) improvements. It was clear he didn’t agree with us.
We came away with few answers. It was all very vague, and quite frustrating for us. We want to work well with the ICU team, so have always been respectful and appreciative of their time and efforts. However, I think we came away today feeling no better informed, and that we had had to fight for Dad again.
RECOMMENDED:
Looking forward to hearing from you,
Best wishes,
Anna
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!