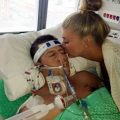
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What are the Risks and Benefits if my Mom Has a Tracheostomy in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Adam, as part of my 1:1 consulting and advocacy service! Adam’s mom is with a breathing tube and is on a ventilator. Adam is asking how his mom can survive COVID in the ICU.
How Can My Mom Survive COVID in the ICU?
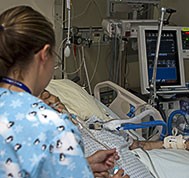
“You can also check out previous 1:1 consulting and advocacy sessions with me and Adam here.”
Patrik: Hi Adam.
Adam: Hello Patrik.
Patrik: So, you have plans of calling the hospital?
Adam: Yup. Maybe it’s a good idea to call them and get a bigger or a better understanding and maybe there’s questions or something that you can ask.
Patrik: Sure.
Adam: Yeah, but I’m livid right now. Do you know what I mean? And I was like, “I don’t even know how much time I have Patrik or whatever.”
Patrik: So, do you want to call them now?
Adam: Yeah. Is that okay with you?
Patrik: It’s fine. If you give me their number, then I can dial them in, or if you want to dial them in. I don’t know how you want to go about it.
Adam: Yeah, I can dial them in. You know what, my brother wanted to be on the call too. But it’s okay, they can hear the recording. I’ll make sure that everything gets recorded or whatever.
Patrik: Okay.
Adam: Let me call them. I’ll call them now.
Patrik: Thank you.
Adam: Hold on one sec.
Patrik: Thank you.
RECOMMENDED:
Adam: Hello. I’m calling to know the status of my mom. She is in Bed2A. Any nurse around?
Receptionist: Okay, hold on one sec.
Adam: I know the nurse has to stay by my mom’s side. That’s what she said.
Patrik: The nurse?
Adam: Yeah. That’s what she said to me because she’s just dropping, dropping, dropping, dropping. And I know, when that happens, your oxygen drops and then the rest of your organs follow.
Patrik: For sure. She probably has every reason to be next to her.
Adam: Yeah. And my mother, I’m not sure if she is already giving out.
Patrik: How old is she?
Adam: She’s 64 Patrik.
Patrik: That’s not very old.
Adam: That’s not old at all. That’s still very young. She’s 64.
Nurse: Hello.
Adam: Hi. Are you the nurse of my mother in bed 2A?
Nurse: Yes.
Adam: Okay. We’re calling to get an update and I also have a family friend on the line. His name is Patrik and he’s a nurse with an ICU background. So, we’re just calling to get an update of my mom to find out exactly what’s happened.
Nurse: Okay. Well, I just came on duty.
Adam: Okay, yeah.
Nurse: And I’m just sitting down to look up all her labs and everything that I have not done yet.
Adam: Okay.
Nurse: But I know the nurse from midnight told me that she had a pretty rough night. I don’t have them written down yet, but her arterial blodo gas ABG‘s were not good, so they want some ventilator changes on them. So, she is now on a pressure control, rate of 20, her FiO2’s (fraction of inspired oxygen) 100% and her PEEP (positive end expiratory pressure] is 10.
Adam: Oh my God.
Nurse: So, none of that is good. That’s not good. It’s going in the wrong direction.
Adam: Yup.
Nurse: So, she had a chest X-ray, it showed just the bilateral infiltrates worsening. Let’s see, because she’s not making any urine at all. I know that she was started on hemodialysis and they did that yesterday. They took 2 liters off. But today, her hemoglobin came back at 5.8 and they just told me that at 7:15, so I have not notified the doctor of that yet.
Nurse: I don’t know if they’re going to want to give them a couple of units of packed red blood cells or not today. They may wait until tomorrow and do it with hemodialysis. And then we have her on medication for her blood pressure.
Recommended:
Adam: Which medication?
Nurse: Levophed. And that is maxed out at 75 mcgs. She’s on vasopressin which is also maxed out. We can’t go any higher on it at 0.04. And she’s on an epinephrine drip at 20 mcg. We’re having trouble keeping her blood sugars up. Her tube feedings are on hold right now because she was vomiting around her tube. They had to put her tube feeding on hold so her sugars keep bottoming out on us. So, they put her on some D10 to try to get her sugars regulated. What else? I’m looking. That’s about all right now. I know she did have a seizure early this month. That was something new. So, she’s on a medication called Keppra for that.
Adam: Right.
Nurse: And what’s she outstanding for? They want to do a TEE on her, which stands for transesophageal echocardiogram. But that is on hold because she’s onto a high dose of Levophed, that’s the medicine to help keep her blood pressure up. And so they can’t do it right now because her blood pressure is so labile. Yeah. And she’s on an antibiotic called Cefazole.
Nurse: And that’s about all the information I have right now.
Patrik: Thank you.
Nurse: Do you have any questions?
Patrik: Is there a septic picture unfolding?
Nurse: I’m sorry, I can barely hear you.
Patrik: I’m sorry. I said is there a septic picture unfolding? Is she in sepsis?
Nurse: Sepsis?
Patrik: Yup.
Nurse: Is that what you said?
Patrik: Yes. Yes.
Nurse: Probably because her blood pressure’s low, her O2 stats are low, she’s not doing very well at all.
Patrik: Yeah. And she’s too labile to prone. If she’s on 100% FiO2 and all these pressors, she’s too labile to be proned I would think.
Recommended:
Nurse: Exactly. Right now we kind of have her in a reverse, not a lot, just a little bit. She’s just a little bit low with the blood pressure right now. So, she’s just very labile.
Patrik: Right. And you don’t have the blood gas results but you expect them to be pretty poor.
Nurse: Oh yes. Yes. They were pretty poor 2 times last night from the night nurse. So they planned on putting her on a bicarb drip.
Patrik: Right. I see. Okay.
Nurse: Yeah. She also had an infection in her blood.
Adam: Yeah, yeah, exactly. She did have an infection in her blood. Hold on. If I can remember what that was. I thought I had it here but I don’t. I’m so sorry.
Nurse: I’m not sure. She might have had a blood stream infection. Maybe MRSA.
Adam: No, no, no. They didn’t tell me a thing about MRSA (Methicillin- resistant staphylococcus aureus). They didn’t even tell me about the blood infection. I just went into her records and I saw it.
Nurse: So, I am trying to pull up her chart right now but my computer’s being very slow. So, I know she’s on an antibiotic called Cefazole.
Adam: Right.
Nurse: And I know that they talked about tracheostomy PEG for her.
Adam: Right.
Nurse: Do you know what a trach and a PEG is? Yeah. But I can tell you right now that the plan for that, she’s too unstable to go to OR. She will die on the OR table if they try to do it.
Adam: Yup, yup.
Nurse: Her ventilator settings are at 100% with a high PEEP, which she needs that to sustain life. And her blood pressure without the maximum dose of Levophed, she’s just too unstable to even take to OR.
Patrik: Yeah.
Nurse: So, we are doing everything we can. We have her on epinephrine, D10, bicarbonate.
Patrik: Everything.
Nurse: But she’s heading in the wrong direction.
Recommended:
Adam: It just took off in that direction. I just don’t understand why. Okay. She was doing okay for a second. I mean, she started. She was just neutral to me.
Nurse: Yes.
Adam: And they don’t know why any of this just started to happen.
Nurse: Well, I haven’t had time to prepare any of the notes. And today’s actually my first day back from vacation so I’m just trying to get into the computer now because I’ve been gone for a week. But I can tell you, when patients test positive for COVID, it hits their body very, very hard. And some of this could be ramifications from having the COVID virus.
Adam: Oh, I know what it was. It was MSSA bacteremia.
Nurse: So, she’s on an antibiotic.
Adam: They have a brand of their own.
Nurse: Yeah.
Adam: Oh God.
Nurse: I’m looking to see who’s ordered that. So, she follows her, she looks at her labs and things every day, and she’s the one that orders the appropriate antibiotic for what is going on with her cultures and her blood work and all that.
Adam: Yeah, got it.
Nurse: So, she knows about all that. She looks at the labs every single day and she does have her on Cefazole right now.
Adam: Okay.
Patrik: Just one last question. You mentioned she had a seizure. Any ideas? Because she didn’t have a brain injury as far as we know.
Nurse: She had a what? I missed it. She had a what? I didn’t hear that.
Patrik: Sorry. You mentioned that she had a seizure and that she was started on Keppra.
Nurse: She did have a seizure early this month.
Patrik: Early this month, okay. Quite some time ago.
Nurse: I was told she had a CVA, a stroke before she had seizure.
Patrik: I see.
Suggested links:
Nurse: Yeah. So, that seizure could have been a sign that she’s having a stroke.
Patrik: Sure.
Nurse: So, she also went into respiratory arrest.
Patrik: Right.
Nurse: So, she’s been hit every single organ. This poor lady has just been through the ringer. This COVID has ravaged her body. It has hit everything. Her heart, her lungs, her kidney. She didn’t escape any damage to any of her organs from that. So, she is fighting a good fight. But I think COVID is winning. I’m being honest with you. She’s in really, really poor condition right now.
Adam: Okay.
Patrik: Okay. Thank you so much.
Nurse: And we will keep doing everything we can, keeping her comfortable, and keep the medicines going to keep her going because I understand she’s still a full code, you guys want everything done, correct?
Adam: Yes. Yeah, she’s still full code. Yeah.
Nurse: Okay.
Patrik: You’ve got her on sedation?
Nurse: Oh yeah, she’s on sedation. Wait, sorry. Wrong patient. No, she’s not. She’s not on anything for sedation, no.
Patrik: Right. But she’s pretty much unconscious?
Nurse: Yes.
Patrik: Right. Is she getting anything for pain relief?
Nurse: Well, I was just in there with her and although I haven’t done a complete head to toe neurological exam on her, I was just in there checking everything out real quick on her. She doesn’t appear to be in any pain at all.
RECOMMENDED:
Patrik: Okay.
Nurse: She was very comfortable.
Patrik: Okay.
Nurse: She’s still sleeping.
Patrik: Okay. Thank you so much.
Nurse: Yeah. She’s very comfortable. I don’t want you to be shocked because she’s in poor condition. Any changes, I will be giving you a call.
Adam: Okay, perfect. Thanks.
Patrik: Thank you so much.
Nurse: All right. Bye-bye.
Patrik: All right.
Adam: Okay. Oh my God, Patrik. Oh my goodness.
Patrik: Okay. You are living far from your mom right now?
Adam: Yes, sir.
Patrik: If you want to see her, I would recommend for you to go there because, by all accounts, I don’t think she has time left.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!