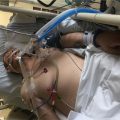
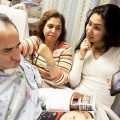
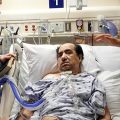
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from Mandy, as part of my 1:1 consulting and advocacy service! And Mandy says, my partner is in ICU with COVID 19 and he was on ECMO. Now he’s off ECMO, but he’s not waking up after an induced coma.
MY PARTNER WITH COVID-19 IS OFF ECMO IN ICU BUT WHY HE’S NOT WAKING UP FROM THE INDUCED COMA?
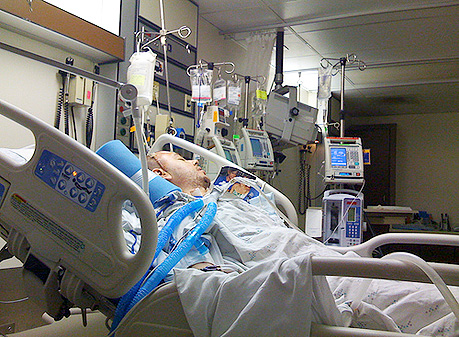
So let’s look at Mandy’s question in detail.
So Mandy writes in,
Hi Patrik,
My partner went into hospital with coronavirus or COVID-19. He was put on a ventilator within 24 hours and he was also receiving dialysis for kidney failure within the first 48 hours. He was then moved to another ICU where they had ECMO available to receive ECMO therapy. He is now off the ECMO after about two weeks on it. And now then he had a tracheostomy and now he’s breathing for himself. That’s at least what the ICU team is telling me but he’s still not waking up and he’s on 25% of oxygen and he’s on dialysis still.
So again, they’re bringing the sedation down at the moment, day by day and bit by bit, they say he’s not waking up and that it could be a number of days before or even weeks before he’s waking up. They’re even saying it could take up to two weeks. I know he’s in the right place and getting the right care, but I’m sitting at home and it’s very hard for me because I can’t visit him because of the COVID-19 situation and I can’t understand how the sedation works or how long it will take him to get over this and out of the induced coma. If you can get back to me, that would be really great.
Thank you.
From Mandy.
RECOMMENDED:
Hi Mandy,
Thank you for writing in. I really appreciate it and I really appreciate you being a client.
So Mandy, I don’t know how closely you have watched what’s happening in the intensive care units at the moment, especially with the COVID-19 pandemic.
So basically a lot of patients that go into ICU with the COVID-19 virus or with the COVID-19 clinical picture, end up on a ventilator, just like your partner and they end up with a breathing tube. They often get either proned which means they are positioned on their tummy for 12 hours a day. Then go back on their back. That is basically to drain fluids out of the lungs and also to help the lungs to expand because you know, when you’re lying on your tummy, the lungs can just better expand and that helps with breathing, helps with oxygenation and so forth.
Now the other option or the alternative option for a prone position is ECMO and that’s what your partner had. So the difference between ECMO and prone positioning is basically that ECMO is more or less taking over the function of the heart and the lung oxygen will be given through the ECMO machine and carbon dioxide will be removed through the ECMO machine.
Now that is very effective. I have seen it many, many times. I’ve looked after many ECMO patients during my time as a nurse in intensive care. And it can be very, very effective, but it also comes with a lot of risks. And one of the risks is bleeding. Most patients on ECMO need to be on heparin, which is a blood thinner. And that’s probably also one of the reasons why your loved one or your partner had the tracheostomy after ECMO, because it would have been too risky to do a tracheostomy while he was on ECMO because of the heparin, heparin is a blood thinner. And again, he’s needed to provide the ECMO therapy. Otherwise the risk for blood clots is just too high by running the blood through the circuits that are going through the ECMO machine. So that’s one of the reasons why your loved one probably had the tracheostomy after ECMO.
So then while he was on ECMO, he would have had the breathing tube still in and he would have needed sedation and the induced coma in order to tolerate the breathing tube or the endotracheal tube.
And also you know, it depends on what sedation your partner had. If he had propofol, which is short term acting he should be able to wake up quicker, but most likely he would have had a benzodiazepine like Midazolam or Versed that kept him sedated and Midazolam or Versed is a long term acting sedative. And it’s also addictive, which means now you’re talking about that, they’re gradually weaning off the sedation because Midazolam is a benzodiazepine and it’s addictive. They need to remove it slowly and by removing it slowly and gradually, so that he doesn’t withdraw from the Midazolam and that’ll delay the whole waking up process.
And the other issue that might come into play here is that your loved one is in kidney failure, meaning he’s on dialysis. And that could delay removing some of the toxins in the body as well. And that could delay him waking up as well. So therefore you need to be patient.
The other thing that comes into play is your loved one, as I said, would have been on propofol but most likely Midazolam. And he would have been an either Fentanyl or Morphine, which is an opioid or a pain medication. And those pain drugs, Morphine, or Fentanyl are so potent. And again, it depends on how much he’s had, but he would have had a fair bit of while he was in the induced coma.
And again, they are accumulating over time. It takes time for the body to metabolize them and get rid of them. And again, that’s delaying waking up and again, the same with Morphine and Fentanyl they are addictive drugs in nature, and therefore they can only reduce them slowly so that your loved one is not going through withdrawal.
By removing drugs like Fentanyl or Morphine too quickly, especially if patients have been on those drugs for quite some time, there is the risk for withdrawal, worst case scenario if somebody is withdrawing could be seizures or other neurological events. And again, you want to try and prevent that.
So, but to come back to your question to how long it takes for your loved one to wake up, for your partner to wake up, that’s really hard to predict, you know, especially after he’s had COVID-19, you probably went into lung failure /ARDS. He’s been in a prolonged induced coma, he’s been on ECMO.
He might have also had some paralyzing agents to keep him paralyzed while he was on ECMO, or maybe even they tried the prone positioning in the beginning. You didn’t mention that, but they might’ve even tried prone positioning. It didn’t work. And again, when patients are being proned, they often need to be paralyzed as well. And sometimes patients need to be paralyzed while they’re in ECMO as well.
So therefore, you know, you can expect a waking up process to be delayed. And, it often is the case in ICU and patients are in an induced coma, very rarely, you know, do you switch sedation and opiates off and patients wake up, it’s not like turning on a light with a switch. It’s more like turning on a light with a dimmer. It’s a gradual process.
And even when your loved one wakes up, he’ll probably be confused. You know, and that is quite normal because, you know, imagine he’s been in a coma now for three weeks and you know, it’s not just like you’re waking up and you’re back to normal. It’s just not how it works. You know, and when you look at the research, what people report from an induced coma, they either don’t remember anything or they have nightmare. So it’s quite a difficult process for patients to come out of an induced coma. And again, it’s not straightforward. So, you know, your number one job at this point in time is really to find out what sedation your loved one has been on and what pain medications he’s been on. And also if he’s still on it, because even small doses can still keep your loved one sedated and in the induced coma.
Next your loved one would have had the tracheostomy after the ECMO. And now you’re saying he’s breathing spontaneously breathing on 25% of oxygen. And that’s good news overall, if he’s breathing spontaneously and once he’s more awake, he might even be able to have time off the ventilator where he can breathe spontaneously with the tracheostomy, with humidified oxygen or humidified air.
RECOMMENDED:
Now with the tracheostomy, please bear in mind, Mandy, your loved one, won’t be able to talk unless they’re starting to use a speaking valve. But again, that might be a little while away still while he’s waking up, you know, he needs to be fully awake to be able to use the speaking valve. And even then he needs some training. You know, the first step really is for your partner to have time off the ventilator. Even if you’re only starting with half an hour a day, that would be a start. You know, maybe the next day he can increase that to two hours a day, four hours a day and so forth.
And then hopefully you can have time off the ventilator during the day, and then he can be ventilated overnight to give him a break. That’s normally how it works to wean somebody off the ventilator with a tracheostomy. And what is also important in those situations is that your loved one is getting mobilized, but again, he probably needs to be off sedation and opiates before he can get out of bed.
And also with the dialysis still going, depending on where the dialysis catheter sits, he might not be able to get out of bed. If the dialysis catheter sits on the shoulder or in the neck, there’s a high chance he can get out of bed. But if the dialysis catheter sits in the groin, it’ll be very difficult to get your partner out of bed. Because the catheter will kink and dialysis is no longer working.
So as you can see, the devil really is in the detail when you have a loved one in intensive care, because there are so many things happening simultaneously and all those things are important. And you can see those little things can stop your loved one really from moving forward or not. If he can get out of bed and he’s off sedation, it’s a good chance that he might get off the ventilator quicker.
If he can’t get mobilized, if he can’t get in a chair, chance that weaning off the ventilator will take longer. And it’s all depends on, just as an example, that I’ve just mentioned where this dialysis catheter sits. So the devil really is in the detail in intensive care.
And you know, the biggest challenge for most families in intensive care is simply that they don’t know what they don’t know. They don’t know what to look for, and they don’t know what questions they need to ask. And this is where we can help to break it all down for you.
RELATED ARTICLES:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Other things you should be looking for going forward, especially with your loved one still on dialysis is, what the kidneys are doing? Are they recovering? Are urea, creatinine kidney markers back to normal? What are the BUN levels? Does he have any spontaneous urine output? Is his fluid balance good?
The fluid balance should be probably negative because again, you want to have more fluids out than fluids going in, especially when weaning off a ventilator. You want to have the lungs dry because any fluids on the lungs would be detrimental to wean off the ventilator.
Other things that are important to look for is with the tracheostomy in particular and with the ventilator still, how often does your loved one need suction? So he can’t clear an airway or his lungs while he’s on a tracheostomy. So he needs the nurses to suction any secretions from the lungs and monitoring the frequency of how often he needs suctioning is quite important. Because again, it’ll tell you, can he cough? How far away is he from weaning off the ventilator?
Any excess secretions would really stop or would hinder your loved one coming off the ventilator, the ideal scenario is your loved one can breathe spontaneously, has minimal secretions, and has a good strong cough.
And once he can tolerate being off the ventilator for more than 24 hours, has minimal secretions, if his blood gases are good, arterial blood gases are good. Oxygen levels in the blood are good. Carbon dioxide levels in the blood are good. He’s coughing. He can clear his airways off the ventilator. That’s when you can start thinking about taking off the tracheostomy, but it sounds like he’s a long way away from that at the moment. But just to map out the steps for you, what is around the corner is important for you to know.
Other issues and challenges that might come up again if your loved one is waking up coming out of the induced coma, as I mentioned before, he might be confused, probably will be confused. Can’t quite make sense of what is happening. And, you know, that’s when it’s really important that family members are there to help their loved ones through that challenge when they’re confused.
They’re waking up in a strange environment, doctors and nurses around them they’ve never seen before. So that can be quite a challenge too. And the longer people are in ICU, the higher the likelihood of them ending up with ICU delirium, ICU psychosis, because of a disturbed day and night rhythm.
RECOMMENDED:
ICUs are very busy, noisy places, often 24 hours a day. Patients get very little sleep sometimes, or most of the time, because they’re fully dependent on the nursing care. They get turned every two hours. As I mentioned, they get suctioned. They get their mouths clean, their noses clean, their eyes clean, they get washed. So it’s really almost nonstop. And that’s one of the reasons why patients are confused after the induced coma. They have a disturbed day and night rhythm. And that’s, again, that’s a massive challenge when patients come out of a critical illness.
Other things you should be looking for again is daily blood results. You should be looking for results such as the hemoglobin, white cell count. White cell count will show you whether there’s still an infection. Electrolyte levels such as potassium, magnesium would be quite important to watch, especially on dialysis. Those are really important things to look for. And again you know keep an eye on what’s happening with the ventilator. If your loved one can have time off the ventilator on a day by day basis and if that time can be increased, right?
RECOMMENDED:
So those are probably the next challenges ahead, Mandy. And again, very important that the sooner your loved one can get out of bed and can get mobilized the sooner that’s achievable, the better it is to help him to get off that ventilator.
So thank you again for being a client.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!