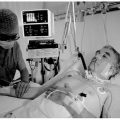
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Is There a Chance for My Mom to Avoid Tracheostomy in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Adam, as part of my 1:1 consulting and advocacy service! Adam’s mom is with a breathing tube and is on a ventilator. Adam is asking what are the risks and benefits if his mom has a tracheostomy in the ICU.
What are the Risks and Benefits if my Mom Has a Tracheostomy in the ICU?
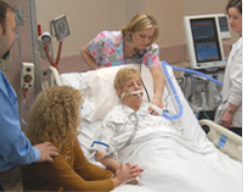
Patrik: No surprises there, unfortunately. That’s how ICU operates. Again, what I will say is this. Most ICU patients survive. Of course, people die in ICU, but that’s the minority, not the majority. What’s my view of alternative therapy? Whilst ICU can be very cruel, it does save lives.
Patrik: I guess the other thing that I will say about alternative therapies is this. If you’re working in ICU, doctors, nurses, people are busy? And often the last thing they need is an extra task. And again, that might sometimes look like people are ignorant, or they’re not taking into consideration what other people say.
Patrik: And I’m not saying that the industry is perfect. Far from. I mean, I’m very critical of the industry. However, there’s also a lot of good things happening. And all I can tell you is generally speaking, people are working hard. Not always to the best of their abilities, but certainly working hard to get someone from A to B. But as you know, you know I am very critical of certain aspects of the industry.
Adam: Yeah. And there are some great nurses that I know.
Patrik: Oh, look.
Adam: And I’m like, “Wow. I’m with my mother right now.” I feel blessed to have some good nurses. It’s like they talk to me and they’re like, “Okay, this is what they do.” They take me every step of the way, whatever, even the charge nurse, he did very well. I told him thank you very much. And I was very happy with some of the stuff they were doing.
Patrik: For sure, for sure. When someone is in ICU, they are as close to death as they would probably ever be in their lifetime. Of course, emotions are running wild and things don’t make sense. I get all of that. And you look at it from the outside, and it is difficult to break things down for… to break things down in “layman’s terms”.
RECOMMENDED:
Adam: Yeah.
Patrik: So I probably agree with you that, look, if they want to get into LTAC, I agree with you that they potentially could kill her there. Absolutely. Absolutely yes. I do believe one of the most important questions at the moment, Adam, is to find out, is there any way she can avoid the tracheostomy?
Adam: The trach.
Patrik: Yeah. Because if she can avoid the trach, everybody’s life will be so much easier.
Adam: Yeah. And that’s why I waited so long to even put her on the trach. Just to see if she can be without it.
Patrik: Yeah.
Adam: And if she can’t…
Patrik: There’s pros and cons for a trach, like with anything in life. There’s pros and cons.
Adam: Are there any other options besides the trach?
Recommended:
Patrik: Yeah. The option might be to wean her off sedation, assuming she’s still on sedation and take the breathing tube out. That is the best option as a matter of fact.
Adam: They did say that, and they said, “But if you do that, it looks like she’s just going to fall.”
Patrik: Yeah. Again, that might be the case. That might be the case. That’s what I’m saying. A trach might be the best thing for her or it might not. I don’t have enough information at the moment to tell you what might be best for you.
Adam: How can I give you that information so that I can know what might be best?
Patrik: Yeah. So the best thing might be for you and for me to get on a call to them.
Adam: Yeah.
Patrik: Or you give me access to the medical records. But I do believe the shortcut might be for you and for me to talk to them.
Adam: Yeah. What are we looking at for that?
Patrik: Nothing. So we can call them now, if you like. I know it’s very early in the morning, but it’s..
Adam: Of course.
Patrik: We can call.
Adam: I move. Yeah. And I also have access to her… I secured by that as soon as I got off the phone with you, I went and got access to the medical chart.
Patrik: Right.
Adam: So I have that. Well, I can call the ICU right now. Yeah.
Patrik: I think that might be a good thing to do. Who do you normally talk to when you call them?
Adam: Most of the time the nurses. They always have something to say. And I’m very kind, but I did challenge and question, and they just kind of avoided.
Patrik: Of course, of course.
Adam: I normally just speak to the nurses that are there. They give me a rundown of her stats, her FIO2 (fraction of inspired oxygen), her dialysis, all of that.
Suggested links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Okay. So you are finding them helpful.
Adam: They are helpful to a certain extent. Yeah. Some of them, depending on the nurse because some nurses are just better at their job.
Patrik: Of course.
Adam: There’s 2 individual nurses that just nailed it every time, and 3, including the charge nurse.
Patrik: Okay. And they are not avoiding your questions?
Adam: They do not avoid my questions. When they don’t have the answers, they will send it for, but I never hear from the doctors. I am the healthcare proxy. I never hear from them. Only a few times.
Patrik: Right. Okay.
Adam: Yeah. You know what? Right now, that’s exactly what they’re doing. Exactly. That is what they’re doing, Patrik.
Patrik: So in order to save you time, if you want to, we can stop here now and then use the time to call them maybe later in the day. But what do you think?
Adam: I think that’s great. But I would want to ask you a question, Patrik.
Patrik: Oh please.
Adam: Who do you think we should talk to? Because I know the palliative care doctor will be calling me today.
Patrik: Yup, okay.
Adam: Right. He’s going to be calling me because he’s like, “Well, as far as the trach and the whole dime.” But who do you think we should talk to?”
Patrik: Great question. Yeah. I think we should talk to anyone that can give us information. And I can get information from a doctor, I can get information from a nurse because I know what questions to ask.
Adam: Exactly.
Patrik: So I don’t really mind who to talk to. However, I’ll tell you one thing. I would not over complicate things. And by that, I mean, let’s talk to the people who are willing to share information. And the palliative care doctor has a different agenda potentially to an ICU doctor. They sometimes have different agendas.
Adam: Yeah. I see that.
Patrik: Right.
Adam: Trust me, I see that. Yeah.
Recommended:
Patrik: Of course.
Adam: Yep.
Patrik: But at the end of the day, let’s just say we are going to call ICU and you ask for the doctors. The doctors are not there. Then let’s say, “Can I talk to a nurse?” Just get someone on the phone that can help us.
Adam: Okay.
Patrik: Because sometimes, as you know, hospitals are easy and sometimes, as I said, I’m a big believer in keep life simple. And the situation is complicated as it is. Just get someone on the phone, get it from the horse’s mouth. It doesn’t matter whether it’s a doctor, doesn’t matter whether it’s the nurse.
Patrik: I’ll tell you what the best case scenario is from my experience. Talk to the nurse, get information from them and then talk to the doctor. Because by doing that, you’re getting two points of view.
Adam: Okay. I can find out which doctor is doing their rounds today. My sister’s going to be going up there literally within the next hour. I’m going to be going up there in the morning now. So I can find out which doctor is doing the rounds, and I can relay a message that I need to speak with her.
Patrik: Yeah. And..
Adam: Because my sister will be there and she can do it face to face.
Patrik: Right. And also, Adam, it’s important… Well, no, it’s not important. It’s up to you how you want to introduce me. So for example, you could introduce me as an external consultant/advocate.
Adam: Yeah. Nice!
Patrik: Or you could introduce me as a family friend with a critical care nursing background that’s helping you make decisions and helping you maybe understand what’s happening. Now from experience, the latter works better because it’s non-threatening for them.
Adam: What’s better Patrik?
Patrik: If you introduced me as a family friend with an ICU nursing background that’s helping you to make decisions and helping you understand, that’s non-threatening for them.
Adam: Okay.
Patrik: You can introduce me as a consultant. I’ll leave it up to you. But I’m telling you, we want to get information.
Recommended:
Adam: Yeah.
Patrik: If they feel threatened, you’re not getting information.
Adam: Yes, I agree.
Patrik: Right. If we tell them I’m helping you and your family understand and I’m helping you and your family to make decisions, they might actually appreciate that.
Adam: Okay. Let’s do it.
Patrik: Right. We can still advocate. So I’ll keep it very friendly, and I will say what I have to say if I think I need to say something, of course.
Adam: Okay. Let’s do it.
Patrik: Do you want to do that right now because it is handover time there. We can try.
Adam: Yeah. Well, what I find out that I’ll call anytime between 7:00 and 7:15. Well let’s try. We can try.
Patrik: Let’s try.
Adam: What do we have to lose, right?
Patrik: Sure. Yeah.
Adam: Okay. Hold on one second.
Patrik: Thank you.
Suggested links:
Nurse: This is Nurse Fem. How may I help you?
Adam: Hi Fem.
Adam: I need to know which nurse is in charge of my mom today.
Nurse: I actually couldn’t tell you because at this time of the day, they’re just rounding.
Adam: Oh, they’re rounding.
Nurse: They are.
Adam: Oh, okay. So what’s a good time that you think I should call back?
Nurse: In about an hour.
Adam: In about an hour. Okay, got it. Thank you so much for your time.
Nurse: Okay.
Adam: All right. Bye-bye. Okay. So yeah, it’s rounds right now.
Patrik: Yep. That’s okay.
Adam: Yeah.
Patrik: Look, I’m not sure when I’ll be available in an hour and a half. The next time I’ll be available is probably around 5:00 PM.
Adam: And that might just work because, well, that’s the palliative care doctor calling me. Then I would probably get a doctor because you know what? I believe the neurologist is on the call today.
Patrik: Right.
Adam: What I said to the palliative care doctor, or I can even have my sister who is my mother’s ambassador, she can leave a note for the doctor today. And I could tell her that 4:00 PM will be perfect.
Patrik: Okay. Let’s do that.
Adam: Yeah, I can do that today. Okay. So 4:00. And that works out well too. I knew that that could happen. I think that’s the time the palliative care doctor calls.
Patrik: Right. Look, as I said, I’m happy to talk to anyone and I’m happy to talk to the nurse. I can talk to anyone. Doesn’t matter to me.
Adam: Okay. All right.
Patrik: Let’s just say the palliative care doctor is not available at 4:00 PM. We should still talk to the nurse.
Adam: Yeah. And the medical records. What do you most need with it?
Patrik: You have had MyChart?
RECOMMENDED:
Adam: Yeah.
Patrik: Right. Yeah, look, within the hour, we probably can’t review the medical records. The easiest would be for you to sign up for the membership, and then we could start looking at the MyChart. I’ve got people who would do that in the background and we would closely communicate.
Adam: Oh perfect. Okay. And that’s the one for the $97.
Patrik: Yes.
Adam: Right. Okay, perfect. What time?
Patrik: This is the strategy there. So what I’ll do is I will call you back and we’ll go from there.
Adam: Patrik, that’s perfect. Thank you so much for your time.
Patrik: It’s a pleasure.
Adam: Yeah. Thank you.
Patrik: Let’s talk later.
Adam: Perfect. All right. Bye.
Patrik: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!