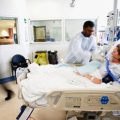
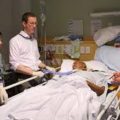
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
The ICU Team Does Not want My Dad to Have Dialysis. Why Are they Limiting their Treatment To My Dad?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Adam, as part of my 1:1 consulting and advocacy service! Adam’s mom is with a breathing tube and is on a ventilator. Adam is asking if there is a chance for his mom to avoid tracheostomy in the ICU.
Is There a Chance for My Mom to Avoid Tracheostomy in the ICU?
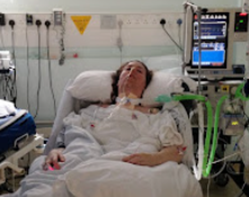
Patrik: Hi Adam.
Adam: Hi there Patrik.
Patrik: So how’s your mom?
Adam: So Patrik, I spoke to the palliative care doctor yesterday and he wants to send us to LTAC. And I told him, because I’ve seen your videos, so I said, “No.” I said, “Unless you can 100% tell me that the nurses and the doctors over there are qualified, like the ICU that they pick specific qualified courses and things like that and the same as ICU.” And he’s like, “Well.” He said he didn’t know, but I think he did. I think he just kind of played it.
Patrik: Yeah, sure.
Adam: Yeah. So he’s like, “I must bring it to the board.” And I know they’re talking about it because, I mean, when we called… Oh, Patrik, they’ve been talking about us for a minute there in the hospital. So he’s like, “I’m going to bring this to the board tomorrow morning and we will see what we can do besides LTAC.” Because I said, “I don’t want to do LTAC,” to hold back.
RECOMMENDED:
Patrik: Yeah. Just remind me, why did your mom go into ICU in the first place? Was that because of COVID?
Adam: Yup, she had COVID pneumonia. She was doing well because they didn’t know that I was giving her H2O2 (hydrogen peroxide). And they’re like, “Oh, okay. She’s probably going to be discharged soon because I’ve got Remdesivir.”
Patrik: Well.
Adam: And so when I stopped Remdesivir and some other stuff that the infectious disease doctor was giving her, I said, “Oh, no. This, this, this, no, no, no.” But she fell asleep, Patrik, and her mask left her face. So her respiratory rate went all the way down to a 30.
Patrik: Got it. How long ago is that?
Adam: She’s been on the ICU now for maybe about since the early of this month.
Patrik: Right.
Adam: So it’s been almost three weeks.
Patrik: Right. And what makes you think they are murdering her?
Adam: Well, when I spoke to the infectious disease doctor, he was giving her medication that he didn’t need. And he didn’t even check to see if she needed them at first. And when I started looking at the side effects of that, that’s murder. That’s not care. That’s just assumption. That’s just assuming.
Adam: So I said, “Okay, so she’s going to have all these side effects, which is going to trickle down to something else. It’s going to affect her body. That’s soft murder.”
Recommendation:
Patrik: Right. Do you know what medications you are referring to here?
Adam: Yeah. So when they first started her… I have them right here. One second. They first started mom in the ICU. She already came in there being a… She is a diabetic, but she didn’t have problems going to the bathroom. So one of the things that they wanted to give her was..Remdesivir was one.. And then the other thing that they gave her was an antibiotic.
Patrik: Okay, an antibiotic. Can I just ask? Is she having a tracheostomy?
Adam: Yeah. I have to approve it today.
Patrik: So not yet?
Adam: Not yet. They’re going to do it on Friday. We’re going to be talking again to a palliative care doctor who I’ll be talking to.
Patrik: How many days has she been on the ventilator now?
Adam: I think about 21 days. 17 depending..
Patrik: 21 days. Okay. Okay. I can give you a quick tip.
Patrik: I’ll give you one tip how you can get her a tracheostomy, but still not go to LTAC. The way to manage this is to not give consent to a PEG tube.
Adam: Oh God.
Patrik: Because she’s not going anywhere without a PEG tube, but she doesn’t need a PEG tube. She can get feeds through an oral gastric or a nasogastric tube. So that’s sort of a bit of a trick of the industry. Don’t, yes, give consent to a trach potentially, but don’t give consent to a PEG tube. That’ll stop them from sending her anywhere, and you get the best of both worlds.
Adam: Wait, you’re saying, once they get back, have they asked if I want to send her? I told them, “I want her home.”
Patrik: Sure.
Adam: He said, “Well we can’t send her home on a ventilator.’’
Patrik: Yeah, you can send her home on a ventilator, but that’s certainly not an overnight process.
Suggested links:
Adam: Okay. Yeah. How do we get there so that because I want to..
Patrik: Yeah. Look, I’m all for hope here, but what is much better is not to have her… How can I explain this? That the best case scenario is to get her off the ventilator and the trach because then going home is so much easier.
Adam: Yeah. And that’s why I approved it. I was trying to see if she can wean off. But then when I started seeing that her health just kept going down. And I’m seeing that they’re giving her stuff. It’s in her medical records. I was just like, “You know what? This is her medication and I wonder if this man is doing well and the vials and everything, her dialysis the whole time.
Patrik: Yeah. Is she on dialysis?
Adam: Yeah. They put her on dialysis. Sure did.
Patrik: Right. Okay. Look, changing medication every day, there might be method to the madness.
Adam: Okay.
Patrik: That there might be method to what you might think is madness. I don’t have enough information to tell you whether it makes sense or not, but there might be method to the madness.
Adam: Got you. Yeah. And they have her on the… kind of one of your videos. And one thing they had her on is vasopressor. Is it pressor?
Patrik: Pressors. Vasopressors. Yeah. Okay.
Adam: Yeah, yeah.
Patrik: If she is on vasopressors, they can be a lifesaving medication. So I don’t see her on pressors being as negative.
Adam: Okay.
Patrik: Okay. I see it as negative in terms of that she’s on life support, which is a concern, but if they are doing it that means that they’re saving her life.
Adam: Got you. That’s vasopressors.
Patrik: Well, the pressors might go on and off every couple of hours. That’s why I sort of keep saying over and over again, “The biggest challenge for families in intensive care is they don’t know what they don’t know.”
Adam: Exactly, exactly. Yeah.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Pressors is life support and is life-saving most of the time. The question is why is she on pressors? I mean, a lot of patients on… with COVID at the moment would be receiving pressors.
Adam: Okay. All right. And they haven’t gotten rid of her COVID. I looked at her chart. I had no idea my mom’s been in the hospital for 40 days. They still haven’t gotten rid of the COVID.
Patrik: Right.
Patrik: Is she still having the COVID pneumonia?
Adam: Yeah.
Patrik: Right.
Adam: After 40 days.
Patrik: Can you visit your mom?
Adam: My brother and her partner and my mother, they’re all near her. So I’m the farthest among them but I’m her healthcare proxy.
Patrik: Right, I see. So you can’t visit her.
Patrik: So you have not seen your mom?
Adam: I haven’t.
Patrik: Right.
Adam: I’m trying to get everything together here financially and the whole dime because I… And I’m trying to get out there hopefully probably within the next week because I have a huge court date that comes up, and I cannot miss that unfortunately.
Patrik: Right.
Adam: So I’ve got to..
Patrik: Right, sure.
Adam: … and then get there. Yeah.
Recommended:
Patrik: Right. What I would want to know is this. If she hasn’t come off the ventilator for the last 18 days, it sounds to me like she might need a trach. But one question that I still have is what if she stays on the ventilator with a breathing tube for a few more days? Is there a chance she could avoid the trach? I don’t have the answer to that question, but I do believe it’s a question that needs to be answered.
Adam: Yeah. And according to the doctor, they are already talking about the end of life care. Hospice came up, of course LTAC came up, and pulling the cord came up. And they’re also talking to my mom’s boyfriend about pulling the plug. And I’m like, “Why are you guys talking to him when you’re talking to me directly as her healthcare proxy?”
Adam: And then they go into the notes and they say, “Oh, we spoke to families, family.” And I’m just like, “You didn’t speak to family. He’s just her boyfriend. They’re not even married.”
Patrik: Right, right, right.
Adam: So they are noting it like that. Yeah.
Patrik: Right. Look, I mean, as long as you are the power of attorney, you shouldn’t have anything to fear there in terms of you making decisions. How old is your mom and what do you think she would want, if she could make the decisions for herself?
Adam: My mom is 66 years old.
Patrik: What’s-
Adam: … and I already know what my mother wants. My mother would want somebody to fight for her life and she would not want all of these medications in her. She hated the hospital. My mother hated what doctors do. She’s seen what doctors have done to other people and what they tried to do to her as well. So my mother has passed the hospital’s policy. She would want me to find a way to get her out of that hospital as soon as possible. She even said that before that mask came off her face. “Get me out of here. Do what you need to do,” da-da-da-da. That’s why she appointed me her healthcare proxy because I’ve done certain things like this before.
Patrik: Right. For her?
Adam: No, for like my uncle, friends, and myself.
Patrik: Right.
Adam: You know what I mean? But I’ve never had anyone end up in the ICU.
Patrik: Sure.
Adam: Never.
Patrik: Sure. Look, ICU is a different ballgame and a lot of the things that you are seeing don’t necessarily make sense. And you do think that some of the things they’re doing are potentially killing her. I argue that there’s a lot of bad things going on in ICU, generally speaking.
Adam: Right.
Patrik: … in order to get someone out of ICU alive.
Adam: Yeah.
Patrik: Right. So what looks like torture probably is torture.
Adam: Yeah.
Recommended:
Patrik: Right. The question is how far do people want to go? But one thing that I will tell you is 90% of patients in ICU approximately survive. Okay. Now that comes at a cost, and I don’t mean a financial cost. I mean, the psychological cost. It’s burdensome. Telling you anything else wouldn’t be accurate.
Adam: Right. And I do understand that. It’s your health, its lack of sleep, all of that stuff.
Patrik: All of that.
Adam: I have a question. How do you get… Because I tried to give her ozone therapy and a Myers’ Cocktail just before dialysis just to see her. The doctors of course denied it. But that was not put on the record. So after telling the ICU nurse, “I need that on the record,” and she hasn’t put in… No one’s put it on the record.
Patrik: Right. So you are saying that the conversation you’ve had about them, the conversation you had with them about alternative therapy has never been mentioned.
Adam: Yeah. Well I spoke to the nurse and told them about the two therapies that I wanted was the ozone therapy and the Myers’ Cocktail. But I spoke to the head clinical manager of the ICU department and her assistant. After speaking with them and told them, the doctor that I have who is a world renowned doctor. I mean, if I were to give you her credentials, you’ll be like, “Whoa.” Pathologist, scientist, the list goes on.
Adam: And I said, I’m shipping her products, and I would like that stuff given to my mother that does not compromise what you guys are doing, does not interfere with what you guys are doing, but will help the quality of life for my mother to help any other back falls.
Adam: And they said, “Okay, we’re going to call you right back. It’s really interesting,” da-da-da-da because I told them who her doctor was, her credentials, how she turned things around. It’s everywhere. She’s there. And I never did hear from them. So I’m like, “Wow.”
Patrik: Right.
Adam: So the alternative medicine, and it isn’t even medicine. It’s just vitamins and supplements.
Patrik: Sure.
Adam: It’s not even medicine. So they denied.
Patrik: Yeah. No surprises there.
Adam: No surprises.
RECOMMENDED:
Patrik: No surprises there, unfortunately. That’s how ICU operates. Again, what I will say is this. Most ICU patients survive. Of course, people die in ICU, but that’s the minority, not the majority. What’s my view of alternative therapy? Whilst ICU can be very cruel, it does save lives.
Patrik: I guess the other thing that I will say about alternative therapies is this. If you’re working in ICU, doctors, nurses, people are busy? And often the last thing they need is an extra task. And again, that might sometimes look like people are ignorant, or they’re not taking into consideration what other people say.
Patrik: And I’m not saying that the industry is perfect. Far from. I mean, I’m very critical of the industry. However, there’s also a lot of good things happening. And all I can tell you is generally speaking, people are working hard. Not always to the best of their abilities, but certainly working hard to get someone from A to B. But as you know, you know I am very critical of certain aspects of the industry.
Adam: Yeah. And there are some great nurses that I know.
Patrik: Oh, look.
Adam: And I’m like, “Wow. I’m with my mother right now.” I feel blessed to have some good nurses. It’s like they talk to me and they’re like, “Okay, this is what they do.” They take me every step of the way, whatever, even the charge nurse, he did very well. I told him thank you very much. And I was very happy with some of the stuff they were doing.
Patrik: For sure, for sure. When someone is in ICU, they are as close to death as they would probably ever be in their lifetime. Of course, emotions are running wild and things don’t make sense. I get all of that. And you look at it from the outside, and it is difficult to break things down for… to break things down in “layman’s terms”.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!