Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Will My Critically Ill Dad In ICU Be Able To Withstand A Tracheostomy?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ella, as part of my 1:1 consulting and advocacy service! Ella’s father suffered a stroke and is on a ventilator in the ICU. Ella is asking why the ICU team can’t wean her dad off the ventilator before trying a tracheostomy.
Why Can’t the ICU Team Wean My Dad Off the Ventilator Before Rushing Into a Tracheostomy?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ella here.”
Ella: But, I guess, whenever I see the video, I get the confidence and I get the positivity. And that’s how I started to have this interaction and everything. So at least I am a little bit more confident when I am talking to the hospital that I have somebody behind me. There is someone with knowledge behind me, so that I can be more confident and then sounding little bit better than saying yes or nodding to everything, whatever they say. “Okay.” Because he also doesn’t want to be in this situation. Neither me. Or nobody wanted to be in this situation.
Patrik: Nobody wants to be in that situation. No, definitely. No, that’s good. I’m very glad to hear that you gain some confidence from what I’m putting out there. That’s really nice to hear. And as I said, if you decide nothing, just keep watching the videos and gain some confidence. The shortcut is obviously, by talking to me directly.
RECOMMENDED:
Patrik: Hi Ella, can you hear me?
Ella: Yeah, I can hear. How about me? Am I audible?
Patrik: Yes, I can hear you.
Ella: Okay. All right. That’s good.
Patrik: How’s your dad?
Ella: I just checked, just 30 minutes back. He’s doing okay. Like “I’m okay” in the sense, in their terms, they’re saying no significant improvement. But he did yesterday, and today, he did two hours, of Spontaneous Breathing Trial yesterday and today. I think-
Patrik: That’s good.
Ella: Yeah. It was two hours he was able to withstand. And they talked about something. I had a 10-minute conversation with the intensivist in the hospital. He was very down. He was not speaking very corporal or something like that. He was telling, “Is this what your father wants?” Or something like that. I said … He was hinting at tracheostomy and all those things.
Ella: But I kept on saying that it is going to take time. It’s not a fast recovery or wherever, whatever point is, to make him … He sounded a little bit frustrated or something. And then he said, “We are not on the same page,” and all those things you were telling. And I was asking him, “How is his COVID thing?” It is just like 10 days completed and still he’s positive they’re saying about it. So, I don’t know. They said they have a 20-day period when they can certify somebody as COVID-free or something like that. Because the way I’m asking is at least they can move him out of the COVID unit. Right? So I don’t know about that.
Recommended:
Patrik: Okay. Just a couple of things there Ella, on that note. So, basically, what you are describing is the intensivist being very negative.
Ella: Right? He’s kind of yeah.
Patrik: Yeah, okay.
Ella: He’s not having the patience as … It is just six days as past from the ventilator and already he’s talking there is no hope or something like that. He’s talking like that. Maybe I don’t know what kind of pressure they’re undergoing or something. I don’t know.
Patrik: Yeah.
Ella: The thing is keeping in ICU. Even, I don’t want that. If he’s stable, they can move to a non-ICU. What is your suggestion on that, Patrik?
Patrik: Yeah. I’ll tell you my suggestion there. I don’t know how much research you’ve done. I’ve written about this extensively and I’ve done videos about this. The negativity you need to ignore, really. And I’ll tell you why you need to ignore the negativity. They are covering that downside. What is that downside? That downside is them coming to you and saying, “Hey Ella. We’ll treat your dad for two weeks and then he’ll be out of ICU alive.” They would never say that, even though that’s what they’re trying to do, because if it doesn’t happen, you could sue them.
Ella: Okay.
Patrik: So they have to be negative by default. Okay?
Ella: You can say negative or defensive or we can say like that.
Patrik: Both. You can say both, but I would probably more say negative, but yeah, defensive probably as well.
Ella: Yes.
Recommended:
Patrik: What I’m also saying is, at the moment, ICU beds are under pressure outside of COVID times. At the moment, ICU beds are under immense pressure with the COVID. But really what they are managing is their downside, which is you suing them. If they promise you something that doesn’t happen.
Ella: Yes.
Patrik: Okay? So I can’t remember whether I mentioned that to you-
Ella: Yes, I think litigation problem is very much there. Right?
Patrik: Huge. It’s huge. They would never say to you, “Oh yeah, we treat your dad for 10 days.” And then day 10, she leaves ICU alive. They will never say that to you. Never. They will keep your expectations low, so they can withdraw treatment anytime. They think it keeps them in control.
Ella: Yes.
Patrik: Right? If they give you hope, you’d be a much more difficult family member.
Ella: But as a medical professional, they should provide a little bit of hope. Right? Even in little ways. But even I was talking to a nurse and then I was just briefly asking. They’re just replaying, like there’s no change in his status or something, which on our side, we cannot accept it. They have to do something more … sometimes, I just ask them, “You do stimulate him?” I just use the word “pinch”. “You do pinch his leg”, or something. Somebody told me a few days back, he was moving both his legs a little bit, to pressure. And then on his own, his left hand, and then his right hand.
Ella: And then that’s what … He’s telling to me that maybe he’s not out there or something. He’s telling that is not, he’s saying it’s cruel or something to pinch somebody or something. We are checking the response. We’re thinking the response to stimulate. That kind of an answer. Sure. They have to also do something when they are in intensive care, also. Right? Because my husband is telling, “In intensive care all they are doing is only monitoring them.” I don’t know.
Patrik: No. Not at all. Look, there’s a few things there, Ella. There’s a few things. Number one, the doctors and the nurses as well are desensitized? What does that mean? Unfortunately, for them, your father is just another patient in a bed. For you, it’s your father.
Ella: Right.
Patrik: For them, he’s just another patient.
Ella: Sorry to interrupt you. Even my husband was telling, “They’re in pressure in terms of COVID bed availability.” I can understand that, but they cannot leave my father in hanging in there or something like that.
Recommended:
Patrik: No. But if you were to give in, they would stop everything.
Ella: Oh, yeah.
Patrik: If you were to give it, they would stop everything, because it frees up a bed. It’s one less hassle. The next patient is waiting.
Ella: Correct.
Patrik: But I’m coming back to the other thing. I can’t remember whether I mentioned that to you yesterday. The research is clearly suggesting that 90% of ICU patients survive.
Ella: Right.
Patrik: So nine out of 10 ICU patients leave intensive care alive. Now, we’re not talking about quality of life. We are talking about a patient leaving intensive care alive. What that looks like is a different story. Okay? But the odds are in a patient’s favor. Now, what is new? What is new is probably in a year’s time, people will say, I don’t know. Eight out of 10 COVID patients leave ICU alive. So that the statistics for COVID is yet to come out.
Ella: Correct.
Recommended:
Patrik: Right? So we don’t know about the COVID survival rate yet.
Ella: One thing is, he started with that COVID test. Identified as a COVID thing. They did some preventive things and everything. Now on the chest x-rays and all those things … He is not having anything, even though his biomarkers is coming down. I think I mentioned to you last time. Right? That inflammation biomarkers?
Patrik: Yes.
Ella: That is coming down, so maybe he’s one week away from totally COVID free or something like that.
Patrik: Could be.
Ella: So having … Yeah, that is what I just want to interject in between your conversation. So …
Patrik: Yeah. No, absolutely. Have they proned him? Do you know what I mean by proning?
Ella: What is proning?
Patrik: They not turning him onto his tummy?
Ella: No, not yet.
Patrik: Okay-
Ella: Is that for COVID? Or for consciousness response?
Patrik: For COVID. Okay. Do you-
Ella: Actually, I think from a code perspective, they don’t sound any alarm.
Patrik: Asymptomatic.
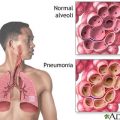
Ella: Yes. He’s not asymptomatic yet. A blood test. The rapid test or whatever the test is showing positive. But his biomarker inflammation is all coming down. He had some slight pneumonia and they treated it for three, four days.
Recommended:
Patrik: Okay. Yeah. The COVID is not the biggest issue.
Ella: Yeah. I think so.
Patrik: Okay. Have I asked you yesterday? Have I asked you about Glasgow Coma Scale?
Ella: Yeah. You asked me, I just saw that just I was watching a video from Glasgow School of Medicine and everything. And they were showing the visual and then a speech and then, I think, touch, I think. Three kind of sensory, I think. Three kinds of things. They’re having, giving the rating based on that. And then here they are mentioning, he’s not opening the eyes all the time, but sometimes when they turn around for cleaning him bowel movement or something that, or stranger touching him or something, it opens and closes it. But most of the time it’s closed.
Patrik: Does your father have an Advanced Care Directive? Do you know what I mean by that?
Ella: No, I don’t.
Patrik: Is there something documented about your father’s wishes in a situation like this?
Ella: No. He used to tell me out of frustration. You know all the people try and they said, like, “I don’t want to live. Pick me. I want to go with my mother and my sister.” Actually, basically, that is a common thing. Out of anguish and helplessness, they say that a lot of times. I just comfort him and then say that it is okay. The thing is, it will be better, but he will be sometimes in a crying kind of stage, he will be there. And then when he sees me, he said, “I just come back from crying or helpless stage. After seeing you feel better,” he is telling. “But you’re going away,” he’s going to say.
Ella: I used to go and visit him for the lunchtime and for the dinner time, every day, to make him like psychologically more stable and everything, because he’s in a new country and he was on assisted living. And there, the care was horrible. They were not able to understand, because had too many people and all those things. So, for that reason, I used to go and see him and visit him and then comfort him. He even, for one day, if I don’t come, he would really get upset. He started yelling or something like that. I said, “Pacify him.” I also told him that, “I’m just here only. Anyway, if you call, I’m going to come. I’m not gone anywhere else. Just be comfortable.” I’m just telling that way I was doing that. But other than that, there is no written or anything like that.
Recommended:
Patrik: Okay. Coming back to the ventilator. So he’s on the Spontaneous Breathing Trials?
Ella: Correct. They’ve been doing from … I think if I’m not wrong, I think once they removed the sedation after a couple of days … That is on a weekend they started the spontaneous, I think. Last Saturday or Sunday. So this is the fifth or sixth day. So yesterday and today it’s been two hours off … he was able to withstand. I think that is a little bit of progress, at least from my side, I can see. Better than what he was before.
Ella: And the one thing they were telling, the intensivist was telling that the secretions, he’s saying, that he will not be able to handle and all those things. And then he’s telling he has to be with the tracheostomy and ventilator, going forward, also for long. Or something like that.
Ella: He sounded, I cannot cross him much beyond that point. I know this is a fact, but the … What do you call us? The quality of life or the way they are better off with the tracheostomy, I know. But I was telling even my husband that, “Don’t rush for anything.” They don’t take the time. My husband was also telling … He doesn’t understand all those things he is telling. “You have to listen to medical professionals.” I said, “I’m ready to listen to medical professionals, but they also have to listen my concern and everything.” And he was also telling, “Is this what your father wants?”I said to, “Yes.” You were saying just some time back. Right? If you yield to them, they’re going to go in that direction. You think? I think.
Patrik: So, looking at quality of life … And that’s why I said earlier. When patients survive intensive care, you don’t know what the quality of life looks like in six months’ time. Right? So you really got to break your goals down into steps. I guess, at the moment, the goal is to get your father out of intensive care alive. We don’t know what that looks like. We don’t know, does he need a tracheostomy to get out of intensive care alive? Nobody knows at this particular point in time.
Patrik: If he has a tracheostomy, it will buy your father time to come off the ventilator. Whether he can come off the ventilator, if he ends up with a tracheostomy, nobody knows at the moment. The easiest way would be to get him off the ventilator without a tracheostomy. That should always be the goal.
Recommended:
Ella: Oh, okay. But if they have to do that, maybe I don’t know, I’m just hypothetically saying if that could take even two, three weeks, would they be patient enough to try that before trying tracheostomy?
Patrik: Great question! So, what’ll happen is the following. 10 to 14 days is the mark. If someone can’t come off the ventilator with the breathing tube after 10 to 14 days? Right? Then a tracheostomy needs to be considered. If for whatever reason, either the patient or the family doesn’t want a tracheostomy … Right? Well, you could argue let’s stop treatment, and let’s look at the end-of-life options. Okay? But that is still your decision. It’s not the hospital’s decision.
Ella: Right. He actually briefly asked that. I said, go ahead with tracheostomy. Something I’ve mentioned in that way. But the thing is like, what my concern is, even before waiting for 10, 14 days, they might rush for the tracheostomy ahead of all trying those things. That is my concern. I don’t know when they’re going to, because today when I just had … Because I was telling right from the beginning, they were trying to say about quality of life and then trying to scare me and whatever. And then I was little bit on the resistive side. So I just said, “Okay. We’ll let him do this. And then … “Because I have another question. To be weaned off the ventilator, does he have to be on an ICU?
RECOMMENDED:
Patrik: Yes. Yup. The only difference is, that when someone has a tracheostomy and … Okay-
Ella: No, not a tracheostomy. If he doesn’t get a tracheostomy-
Patrik: Oh, yeah. Definitely. ICU. Definitely ICU. If he has a tracheostomy, he could go somewhere else.
Ella: Okay.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!