Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about how long it takes to wake up after head and brain injuries in intensive care.
Your Questions Answered Live: How Long Does it Take to Wake up After Head and Brain Injuries in Intensive Care?
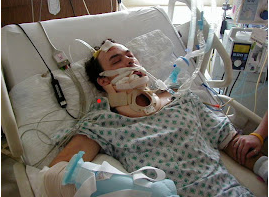
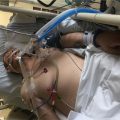
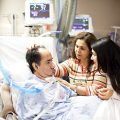
Hi, it’s Patrik Hutzel here from intensivecarehotline.com, and in today’s live stream I want to welcome you, and today’s topic of the live stream is, how long does it take to wake up after head or brain injuries in intensive care. You would have seen me previously talking about how long does it take to wake up after an induced coma? And there are other videos and blog posts on our website, intensivecarehotline.com. There are also videos here on YouTube about this topic about the induced coma and how long does it take to wake up there? Today’s again, a very specific topic, and it’s a very in- depth topic, and also it’s a massive frustration for families in intensive care when they have a loved one in intensive care with a head or brain injury.
To begin with, let’s just start with, what are head and brain injuries in intensive care and can they be classified into different head and brain injuries? And the answer is yes, they can. Let’s just start with one type of head or brain injury which is after traumatic injury, car accident, people falling off roofs, workplace incidents, sport injuries, you name it, when someone falls on their head or gets hit on their head, there’s a big bleed because of the big impact, and patients often need surgery. They need surgery because there’s a bleed and their brain needs to be decompressed. There could be a midline shift, which is basically a shift from the left side of the brain to the right side of the brain or the other way around, which is causing a lot of pressure on the brain and is increasing the intracranial pressure which is basically the pressure in the brain. And if that happens, patients in intensive care often end up with an ICP or an intracranial pressure monitoring also with an EVD (external ventricular drain) to drain excess fluids, excess CSF, or excess blood from the brain. What often also happens is after head or brain injury, depending on the impact on the trauma that’s been caused, patients have a craniectomy, which basically means there’s a partial removal of the skull from the head to relieve the pressure. And then eventually if patients survive their intensive care stay and get better, they have the plastic skull put back on, which is also known as a cranioplasty.
Now, I also want to welcome our viewers of course, and I encourage you to ask the questions in the chat pad. I encourage you to do that. If you have any questions, just type them in the chat pad. If you want to, you can also call me live on this live stream. You can call me if you’re in the US or in Canada, you can call me on 415 915 0090. That’s again, US or Canada, 415 915 0090. If you’re in Australia, you can call me on 041 094 2230. That is again for our Australian viewers, 041 094 2230. And if you are in the UK, you can call me on 0118 324 3018. That is again for our UK viewers, 0118 324 3018.
RECOMMENDED:
Going back to traumatic head or brain injuries, patients then often are induced into a coma as well because the pressure in the brain is so high generally speaking, that the only way to manage that trauma is by putting patients in a deep sleep in an induced coma. Often they’re on propofol, midazolam or Versed, also on opiates such as morphine or fentanyl. As I mentioned, they do have an ICP monitor and an EVD drain. The ICP monitor is showing the intensive care team if the pressure is high in the brain. If it’s high, it needs to be released because otherwise the brain might get permanently damaged. So it’s a fine line managing that ICP. The intracranial pressure needs to be less than 20 mmHg. The CPP, the cranial perfusion pressure which is basically the oxygen or the blood that’s flowing to the brain needs to be above 60 mmHg.
So it’s a very delicate affair really to manage those pressures making sure the brain isn’t get any more damaged. This can be done with medication, it can be done with draining through the EVD, the external ventricular drain, but it needs constant monitoring. It needs constant maintenance. And it can sometimes take many days, sometimes even a couple of weeks or even longer to get those brain pressures under control with medication, with surgery, with EVDs, or with ICPs. And only then can you slowly wake up a patient after the head or brain injury. And if you’ve watched any of my videos or followed any of my blogs, it can take a long time for someone to wake up after an induced coma without a brain injury. So now you’ve got the complexity of a head or brain injury plus the induced coma, and then someone is waking up and that can take ages. And that’s when the intensive care team often comes in and says, “We think your loved one wouldn’t have any quality of life and they’re not waking up and let’s just stop life support and let them just die.” I’ve seen those situations many times, and it’s very tragic. And it can take weeks, sometimes months for people to wake up and they’re not even necessarily waking up in intensive care, they then need to leave intensive care often in a state of coma or semi coma, and then wake up when they’re going to rehab or going on to the hospital floor or hospital ward. It can take time. So that there, I just wanted to highlight briefly traumatic brain injuries.
Recommended:
Let’s just now focus on anoxic brain injury or hypoxic brain injuries. Now, whilst an anoxic or hypoxic brain injury can happen after a traumatic brain injury as well. Many anoxic or hypoxic brain injuries are caused, for example, after a cardiac arrest. Because when people get resuscitated, there may be a prolonged period where there is no oxygen flowing to the brain. Anoxic brain injuries or hypoxic brain injuries can also happen after a stroke. Whether that’s a hemorrhagic stroke or a hypoxic stroke, ischemic stroke, where there’s a clot that stops the oxygen and blood flow to the brain, and that’s causing an anoxic or hypoxic brain injury. As a rule of thumb, if the brain is without any oxygen supply or blood supply for more than 3 minutes, chances are that the brain might be irreversibly damaged.
Let’s just take a cardiac arrest patient. I mean, we have been working with many cardiac arrest clients here at Intensive Care Hotline. Let’s just say someone comes into ICU and I can illustrate that, we’re currently working with a client. So, a 58-year old client is in ICU at the moment after cardiac arrest, had what’s being referred to as downtime for more than 3 minutes while they were resuscitating him. They were able to restart his heart, but most likely his brain hasn’t had enough oxygen supply for more than 3 minutes. It’s unknown for how long he hasn’t had any oxygen supply to the brain, but it’s clear that it was more than 3minutes. So they stabilized him in ICU. They intubated him, ventilated him and took him off sedation pretty quickly and there was no sign of waking up. It’s often being measured. The waking up process is often being measured by a neurological assessment tool such as the Glasgow Coma Scale. And if the Glasgow Coma Scale is less than 8 points, and you might want to familiarize yourself with the Glasgow Coma Score, you can Google that, but I think if you have a loved one in intensive care that’s not waking up after an induced coma or after a head and brain injury, you should definitely familiarize yourself with the Glasgow Coma Scale and you should be Googling that. And it’s almost self-explanatory.
And coming back to this 58-year old man that’s currently in ICU, after an hypoxic brain injury and cardiac arrest, he’s not waking up even now after a couple of weeks. And his Glasgow Coma Score is still less than 6. And he’s opening his eyes slowly, but there doesn’t seem to be any meaningful movement. There doesn’t seem to be any purposeful movement. The family’s saying he’s making eye contact, but it’s very infrequent and it’s just not where they want him to be. But in any case, they’re very hopeful that despite the intensive care team saying that he has no chance of recovery and that his brain is so severely damaged, that he will never wake up, the family is hopeful that he will wake up in his own time. And they’ve asked the intensive care team to do a tracheostomy so that he can have more time to wake up. And that’s what the intensive care team has done.
Also, with our advocacy of course, most families in intensive care are simply lost if they don’t have any advocacy and consulting that’s helping them. The biggest challenge for families in intensive care, simply that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights, and they don’t know how to manage doctors and nurses in intensive care. Most families would have given in and they would have said, “Yep, there’s all hopeless.” And the intensive care team would have stopped treatment, would have taken the breathing machine away and they would have let him die. That’s what most ICUs do. Especially if they’re pushed for beds, especially now with COVID, ICU beds are still in high demand. And again, that’s where our advocacy’s coming in. Understanding intensive care inside out and helping families to steer through that very rocky territory that is intensive care.
Suggested links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
So the bottom line is this, that with any head or brain injury, whether it’s being caused by a traumatic brain injury, whether it’s being caused by a hypoxic/anoxic brain injury, it takes time for people to wake up. And they may never recover to the extent. They might never be able to live the life that they’ve had before by the same token, what is acceptable for you and your family. What is acceptable for your loved one? And that’s not for me to answer, and that’s not for me to judge on either. All I’m here for is to help you make the best possible decision for your situation.
And it’s also not for the intensive care team to judge what is right or wrong for you and your loved one and for your family. You will need to make that decision by yourself. I don’t know your religious beliefs, spiritual beliefs, cultural beliefs, that’s not for anyone to judge. That’s only, that the only person that can answer that question what you want going forward is for you and your family to answer. Especially if there is no advanced care plan.
In the ideal world, patients have an advanced care plan basically documenting their wishes if a tragic situation like that ever happens. It would be good to have it documented where you can put on a piece of paper or in a word document in this day and age, “I want to have everything done in intensive care, irrespective of the outcome, irrespective of my quality of life.” That’s different for different people.
So, the more clear you can be about that upfront, the better it is. But in the absence of an advanced care plan, in the absence of your loved one having documented an advanced care plan and you being put in that position where you need to make a decision, you should be making a decision on what you want going forward. And are you prepared to potentially put up with a disability that your loved one can live with.
Just quickly coming back to one other specific form of brain injury. So we talked about traumatic brain injuries. We talked about hypoxic brain injuries after cardiac arrest/stroke. Another brain injury that I want to talk about is for example, a subdural or a subarachnoid hematoma. So what happens there is some people have an aneurysm in the brain, and unfortunately if that bursts they can end up with a subarachnoid or a subdural hematoma. And again, similar to traumatic brain injury, they often need emergency surgery because there’s a bleed happening in the brain. They sometimes, again, can end up with a craniectomy where they have partial skull of their head removed to relieve the pressure. They might end up with an ICP similar to a traumatic brain injury where they need the intracranial pressure and the cranial perfusion pressure measured, making sure the brain is getting enough oxygen and it’s not sustaining any further brain damage.
Recommended:
So those are the types of head and brain injuries that are most common in intensive care. At the end of the day, the treatment is similar. As I mentioned, as for someone with a traumatic brain injury, they often need to be in an induced coma as well, because if they have a traumatic head and brain injury, they might have sustained other injuries as part of a motor vehicle accident, falling off the roof, workplace accident, you name it. So there’s often pain associated with it. And the combination of a traumatic brain injury as well as being in an induced coma with heavy sedatives and heavy opiates, makes it even more prolonged to wake up after the induced coma and then after the head and brain injury. And patients often need to go on to neuro rehab after they can come out of intensive care.
When it comes to hypoxic or anoxic brain injuries caused by cardiac arrest and there are no other injuries, sedation can be switched off much quicker. And then you also get a much quicker assessment of, is your loved one waking up? What does it look like? How much time do they need? Very rarely do they wake up in ICU to the extent where you can be satisfied. Again, that can take weeks and sometimes even take many months as nobody has a crystal ball. I guess your goal should be if that’s what you want, if you want your loved one to live, your goal should be to get your loved one out of intensive care alive. That should be your primary goal if you’re finding yourself in that situation. And then go on to neuro rehab.
Now, we have worked with many clients and I have seen it for myself in ICU that people do survive those head and brain injuries. And then by the time they can leave intensive care that by no means are they awake. They’re still in a comatose state. And then we lose track of what’s happening with those patients down the line. We don’t know what their life looks like 6 months down the line, 6 years down the line. We don’t know what that looks like. And you don’t know either. And neither does the intensive care team. The intensive care team is very good at saving lives. The intensive care team is not very good at predicting what’s happening once patients have left intensive care. So don’t get blinded by a perception where the intensive care team says, “Oh, once your loved one is out of intensive care, if they survive they won’t have any quality of life.” Therefore it is in their “best interest” to stop life support and let them die.
Well, as far as I’m concerned, life is sacred. Life is precious. And I’m sure you feel the same. I don’t think you would be here otherwise if you didn’t feel the same. And that everything should be done to save people’s lives, especially if you don’t know what’s going to come, the reality is this, if you do stop life support and people die, they’re gone. They’re gone for good. There’s no returning back from that. And I can’t tell you how many families come to us where they agree to stop life support in intensive care because they didn’t even know that people like us can advocate for them. They just went with what the intensive care team told them. And then two years later after their loved ones have passed away, they have second thoughts and they come to us and they say, “Oh, I didn’t even realize there is someone that could advocate for us. I didn’t even realize that there is a different point of view. I didn’t even realize people share their experience.” And that’s why it’s so important that you’d be doing your research.
Coming back to sort of other, what I would refer complications of head and brain injuries and that’s similar across the head and brain injuries that I mentioned, which is again, traumatic brain injuries, anoxic/hypoxic brain injuries, as well as a subdural hematoma or a subarachnoid hematoma. What can come out of this as well is often that patients end up with seizures. Seizures can happen as part of brain injuries, and that’s often not a good sign and it needs to be controlled with medication such as phenytoin and Keppra. They are the most common medications that are being used to control seizures in ICU. It’s often a sign that there’s stuff going on in the brain that can be controlled, and it often delays waking up even further.
I’ll come back to that in a second. I just believe there was a question. Question from Helene. Helene you’re asking, can the septic shock cause hypoxic brain injury? Yes, it can. But only if the septic shock is not managed quick enough. I would argue that if someone has a septic shock, they are either in ICU already. If they are in ICU already and have a septic shock, the intensive care team should be able to prevent a hypoxic brain injury because they’ve got all the medications, they’ve got all the training, all the skills to manage that. If someone has a septic shock outside of ICU and they’re at home or wherever they are and it takes time to respond to that septic shock, yes, then it can cause a hypoxic brain injury. Because the septic shock can lead to cardiac arrest, can lead to low blood pressure, and it can lead to the brain not being supplied with enough oxygen. So, I hope that answers your question.
What I haven’t talked about is, when someone comes into ICU with either a traumatic brain injury or a hypoxic brain injury, one of the first diagnostics that is happening in those situations is a CT scan of the brain. Sometimes an MRI scan of the brain to diagnose what’s going on. Is there a significant brain damage? Is the brain damage irreversible? So you get lots of answers there. Other things that often happen is, and patients end up with an EEG (electroencephalogram), where they get hooked up to electrodes to the brain and the brain activity is being recorded, is there any brain activity? So that’s what’s happening on that level?
My other suggestion is this, that if you do have a loved one in intensive care with head or brain injury, to speak to the neurologist, to speak to the neurosurgeon. If your loved one had brain surgery, you definitely want to talk to the neurosurgeon. If your loved one had an anoxic or hypoxic brain injury, you definitely do want to speak to the neurologist. Because they are the experts on dealing with the brain. So, you definitely would want to do that.
The intensive care team are definitely the experts on dealing with critical illness, but they’re not the experts on dealing with neurological harm long term. That’s the neurologist’s area of expertise. Get the specialists involved, talk to the specialists. The other issue that happens with anoxic or with traumatic and anoxic brain injuries in general, especially if people are not waking up and they’re on the ventilator is simply that they often can’t be weaned off the ventilator. Even if they can be weaned off the ventilator, they often need a tracheostomy. Even if they can be weaned off the ventilator, the reason they need a tracheostomy often is simply that they can’t swallow. They can’t cough. And if you can’t swallow and if you can’t cough, you can’t protect your airway. And therefore, you can’t be protecting your airway and you need a tracheostomy. That’s often a side effect of a neurological condition and a head or brain injury.
Recommended:
But it’s also a tracheostomy, especially if your loved one can’t breathe, it’s also a vehicle that will buy your loved one time, the device that will buy your loved one time, they can then swallow, cough, they can be suctioned. It’s just a device that will buy your loved one time. And you should be asking for it if you think that’s what you want to prolong your loved one’s life.
Helene you’re asking, my mom also suffered iatrogenic induced injury that caused septic shock from BiPAP machine. The ICU team concealed the septic shock from me. Sure. I would be curious to know why a septic shock was induced from the BiPAP machine. Now, if you feel like the ICU team concealed the septic shock from you and your family, my advice there is to look for the medical records, ask for the medical records, and we can help you with reviewing them. We can find out, was the septic shock really induced from the BiPAP machine? Was the septic shock concealed by the intensive care team? We can find that out by looking through the medical records.
The only correlation I can see with the BiPAP machine causing a septic shock is maybe BiPAP caused vomiting. Maybe vomiting then cause an aspiration pneumonia. And an aspiration pneumonia caused the septic shock. Or other causes might be that the BiPAP machine caused a pneumothorax, and maybe that caused the pneumonia and that caused the septic shock. Maybe you can share more there, but the answers to your questions will come from a medical record review. And again, we can help you with that. My team of intensive care professionals and myself, we can help you with that.
Recommended:
Just coming back to the head and brain injuries then, and I’ve talked about seizures. Seizures can often delay waking up even further. Seizures may also be resulting in the permanent seizures unfortunately. And that also leads me to other head and brain injuries that I should have mentioned earlier is a stroke. That’s also a head and brain injury caused by hypoxia. But at the end of the day, whether it’s traumatic brain injury, whether it’s hypoxic brain injury, nobody knows how long it takes to wake up. And the ICU team will be very quick in trying to tell you that everything is hopeless and that your loved one will never wake up, that they will not have any quality of life. And they will tell you that three weeks in ICU is a very long time and that we can’t wait any longer and we should stop everything.
Time is relative. Three weeks in ICU, probably a bit longer than the average patient, but then there’s patients in ICU that stay there for 3 months. It really all depends on your preferences. It depends on what you want. It depends on your beliefs and how much time do you want. And again, you’ve got to look at it in advance and also in retrospect. You’ve got to look ahead and think about, okay, if you agree to take off life support today and your loved one is dying because the ICU team is telling you, “Oh, they’ll never wake up after this head or brain injury.” In two years’ time, you will have second thoughts because you think, “Oh, what if we had not agreed to removing life support?” The “what ifs”. But if your loved one is dying because you agree to a withdrawal of life support, it’s too late, they’re gone. They’re gone for good. So therefore you need to do as much research, get as much help as you can, get as many opinions as you can. And we can help you with a second opinion here at intensivecarehotline.com.
Again, there’s no guarantee, maybe you regret prolonging the life of your loved one. Nobody knows. It’s a very difficult question to answer. But I can assure you that 3 or 4 weeks in ICU, it’s not long, in the bigger scheme of things if it takes 4 months for your loved one to wake up and have any meaningful interaction. It all depends on your preferences. But maybe just to illustrate a little bit more with examples. We’ve worked with a client over the last few months and their 78-year old dad ended up in ICU with a stroke and didn’t wake up for quite some time, was in ICU for prolonged periods, eventually went home and he’s now slowly waking up. Very slowly waking up. And again, it takes time and he’s probably never going to have the quality of life that he had before. But he’s alive and they want him alive. And it sounds to me like he wants to be alive. That’s what it comes down to. It comes down to your preferences.
Suggested links:
We’ve reached the half an hour mark. I hope that today’s session was helpful. If you have any questions, please type them in the chat pad now. Helene you’re asking, “How long can an elderly patient be on a BiPAP machine? Mom’s pulmonary team had her on BiPAP 72 hours straight and without food, water and break from the machine. Is this overuse?”
A couple of things there, Helene, if you are aware of people, for example, having sleep apnea, they’re on BiPAP machines at home, they’re not on BiPAP during the day, but they’re on BiPAP overnight for sleep. And there’s many elderly patients that suffer from sleep apnea so they can be on a BiPAP machine for quite some time. Now, if your mom’s pulmonary team had her on BiPAP 72 hours straight and without food, water and break from the machine, is this overuse?
It’s a difficult question to answer and it comes back again to reviewing the medical records, because the question is this, what would have happened if they took her off the BiPAP machine? Would they have needed to intubate her? It’s only overuse, BiPAP is only overused if she could breathe by herself without the BiPAP machine. Well, I don’t know whether that was the case or not. BiPAP for 72 hours straight without food, water, and break from the machine is tough. It’s very tough. But it also keeps people alive. So I don’t know enough about why your mom ended up on BiPAP. I don’t know what setting she was on. I don’t know what did arterial blood gases show? I don’t know what the chest x-rays show. What BiPAP settings was she on.
When you’re saying she was without food, water and break from the machine, was she, for example, on TPN? Was she on intravenous nutrition? So there’s all these unanswered questions that we would need to look at before I can really answer your question. And it all comes back to, families in intensive care don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care.
In your mom’s situation Helene, when someone is critically ill in intensive care, there are dozens of things happening simultaneously. Dozens. And whilst you’re asking a very good question and I would need to know so much more. I would really need to review the medical records. Would really need to talk to a doctor what else was happening at the time. It’s not an easy questions to be answered. You’re saying, “No sleep apnea nor feeding nasal.” What about TPN? Was she on TPN? TPN is total parental nutrition and it’s intravenous nutrition. Did she have any of that while she was on BiPAP, do you know? “No.” Okay. Well then that could be deemed as negligent for sure. Definitely.
RECOMMENDED:
So, okay, conscious of the time, Helene or anybody else, did you have any other questions? So Helene you’re asking, what did I just say? So yes, TPN, in the absence of TPN, Helene, basically if she did not get any nutrition at all for three days, that could be negligent. Having said that, I would argue, again, I haven’t seen the medical records, but I would argue that at least she would have had hydration. She would have been on a normal saline drip or on another drip to give her fluids. I would argue that. I would be very surprised if they at least hadn’t hydrated her. Do you know whether they were hydrating her while she was on BiPAP?
All right. While I wait for your answer, Helene, so conscious of the time, need to move along. Well, thank you so much. Helene, you’re saying, “Excessive fluid overload.” So she might’ve had too much normal saline. Right. Okay. Again, the answers to your questions there Helene will be in a medical record review. I can see the bits and pieces that you’re bringing up, but there is probably a much bigger picture at play and it would need to be broken down to all the nitty gritty and only then could we provide you with answers.
Anyway, look, I’m conscious of the time. I need to move along for now. Thank you so much for coming to this live stream. I really appreciate you. If you have a loved one in intensive care, please go to intensivecarehotline.com and call us on one of the numbers on the top of the website. You can also send me an email to [email protected]. That’s again, [email protected]. If you need, you can also subscribe to my YouTube channel. I really appreciate you as a subscriber. You can comment what questions that you have below the videos and like this video and subscribe to my YouTube channel. And thank you once again wherever you are, and I wish you and your families all the very best. Take care for now.
This is Patrik Hutzel from intensivecarehotline.com and I will talk to you in a few days.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!