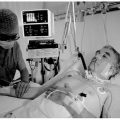
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Do I Take Control and Have Peace in Making Decisions for my Critically Ill Sister in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Joyce, as part of my 1:1 consulting and advocacy service! After a couple of months of fighting with her condition, Joyce’s sister is now off the ventilator but still has a tracheostomy, can’t be weaned, and had developed severe pressure sores. Joyce asks what she will do to keep that fighting spirit, so her critically ill sister has a chance to survive in ICU.
How Can We Keep that Fighting Spirit So our Sister Can Survive in ICU?
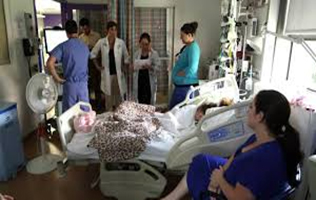
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Joyce: That’s how much she needs … But it’s that minimal. Because I looked at the trach, and barely any air is coming out. You know what I’m saying? That aerosol’s not coming out that much, but it makes such a huge difference. I take that out, she … within minutes.
Patrik: So let’s just run through what you might perceive as the worst case scenario. Let’s just say you go down the track of comfort care, you remove the trach, you stop the feeds, and you do what-
Joyce: I can’t remove the trach, because the trach will be within half an hour. That’s too dramatic.
Patrik: Right, right. But even if you start with removing the feeds, what would you need to do? You need to probably up even the Dilaudid more. You would have to give her a sedative. You could argue-
Joyce: It would have to be in the drip.
RECOMMENDED:
Patrik: Yeah. You could argue, is that supposedly euthanasia? There’s all these questions that I can’t answer for you, but I can obviously open up the discussion around it.
Joyce: So my question is, what do I do?
Patrik: Wait.
Joyce: Do I just cut the feeding, or just wait?
Patrik: No, you can’t cut the feeding. You could potentially starve your sister to death. Would they do that? If I was the nurse-
Joyce: They would. They will do that.
Patrik: You’ve sussed that out?
Joyce: No. Comfort care has gave me that option.
Patrik: Okay, all right.
Joyce: Because they’re saying it’s life support.
Patrik: Well, it is life support. Yeah, for sure.
Recommended:
Joyce: Right, so it’s considered, it’s the same thing as having a VAC. Doing the feeding. But morally…
Patrik: Yeah, morally, ethically, those are the questions. You could keep your sister alive, definitely for longer, if she doesn’t get an infection. But you could also cut it short more or less by withholding the things that we spoke about.
Joyce: It’s just food, really.
Patrik: Food, yeah, but tracheostomy.
Joyce: But the trach is going to happen within … that’s too drastic. That’s within an hour, and-
Patrik: Not necessarily. Yeah, yeah. How do you feel about bringing this up with your sister directly? Do you think that’s too confrontational?
Joyce: She won’t do it.
Patrik: Won’t do it.
Joyce: She won’t do it, because she’s scared to death. I said to her, “You pull it out, it’s up to you… your choice, and do what you want to do.” And ever since I said that, she hasn’t touched it whatsoever. I used to have a binder, I used to fight her over it, and I explained to her, I said, “It’s really bad. It you pull this out, I will not be putting it back in.” And she hasn’t touched it at all. She’s scared. Listen, she is scared. She’s not going … she loves life. My sister loves life.
Patrik: Sure, who doesn’t?
Joyce: She smiles to the nurses. She got used to her situation, but what’s the end game? I mean, is it bad of me? Am I just getting tired and throwing in the thing?
Patrik: Look, look. Okay, so maybe what I haven’t shared with you is this. We have, as you know, we’re running Intensive Care at Home as well here. We have so many clients at home that are on ventilators that are on trachs. I would argue that all of them want to live. Now, they don’t have a nasty wound like your sister does, but I can tell you that I would argue for 90% of our clients, life is worth living. And yes, they’re at home, they’re not in a hospital, but I do believe, your sister is in a situation now … Yes, the situation doesn’t look great, but by the same time, I do believe, even with all the limitations, it sounds to me like life is worth living.
Suggested links:
Joyce: But not in a subacute.
Patrik: Well-
Joyce: And do you see what? My system is broken. Because if I had your company here, someone that would be able to do 24 hrs … then I’d be like, “Okay, we’ll do this at home. We’ll figure this out,” and it would be a no brainer. But because I can’t do it, and because subacutes are not an option because it’s going to give me half an hour every other day, and she’s going to stare at the wall, there’s no way.
Patrik: I think you should possibly put the onus back to the hospital as well to do something about this wound. And I know that’s probably easier said than done, but I have seen with wounds that there are some people that can be proactive about this, like the surgeons and wound care specialists.
Joyce: Have all of them on team. I have all of them, and I have picked their brain. I said fat transfer and other things. She said, “Honestly, it’s so deep. She has to go through so many layers to build this up, and then we can talk about it, but without the proper nutrition, without being mobile…”
Patrik: What’s led to this? Do you know what led to these wounds?
Joyce: Yes, the other hospital not turning her. The original hospital, they thought she was a goner. Remember? You were there. And they thought she was a goner, and they just did not turn her. And I’m now suing, I’ve got a lawyer. And I’m suing them because the girl said, when my sister went in, she has a clean back. Nothing, not even a scratch. And come three months later, it’s a huge crater. How do you explain that? And I get it, there’s pandemic, it’s COVID-19. Its ventilator, but not to this degree.
Patrik: No. There’s no-
Joyce: Not to this degree, stage two, stage three … But it’s not only stage four, but it’s the worst of stage four that anyone has ever seen.
Patrik: Did she have an air mattress while she was in ICU in the early days?
Joyce: Yes, she did. Yes, she did. And I don’t know how she got this. I mean, she does have diabetes.
Patrik: Yup, that makes her more prone, for sure.
Joyce: But to this horrific?
Patrik: And she did have, from memory, she was on vasopressors? From memory.
Joyce: What is that?
Patrik: She was on epinephrine, norepinephrine?
Joyce: I don’t know what that is.
Patrik: Oh, okay. She would’ve been on life support to maintain blood pressure that’s compatible with life.
Joyce: Maybe, maybe.
Patrik: She would’ve been on that. Now, most likely, at least for periods of time. If she was on that, most likely, and the diabetes, that is a massive risk factor for developing pressure sores. Massive. The combination of that … I’m not saying you’re getting one. With good nursing care, you should still avoid it, but the risk factor is so much higher.
Joyce: And I think to be honest with you, they didn’t think she would survive. They literally did not give her a weekend. In October, they didn’t give her until the weekend. Remember, you and I spoke. And we were fighting, fighting, fighting, and to get to this, it’s a big victory, yet I can’t … And everybody told me, “Quality of life, and quality of life.” And I didn’t really focus until now.
Recommended:
Patrik: But you can now also see, which is what I said in the beginning, what quality of life your sister wants to live?
Joyce: She does, she does.
Patrik: Right, so the whole argument around quality of life is such a subjective topic.
Joyce: But she wants to live, to live in a room and not be able to get out of it is not acceptable.
Patrik: Yeah, sure.
Joyce: To live in subacute is not acceptable, and I can’t bring her home. So what do I do?
Patrik: Yeah, wait. Wait. So do you think that the hospital … the hospital is not saying to you, “You need to be in subacute by next week”?
Joyce: They can’t find one.
Patrik: No, I wouldn’t.
Joyce: They can’t find … Basically, it’s like they basically are going to be knocking at my door, and then if they do, then I can aggressively say, “No, no, no, no. Stop the feeding.
Patrik: I can’t see her going to subacute with that wound also. And I wouldn’t be worried about the subacute. It’s more a case of, okay, where do you go from there? I’ve seen people being in hospital for years, unfortunately. I’ve seen that.
Joyce: I think this is a unique case that they have never experienced, because none of the subacutes have the staffing, nobody wants it. And she has to be isolated, and they don’t want contamination in the center.
Patrik: What bugs are we talking about? VRE (Vancomycin- Resistant Enterococcus) or MRSA (Methicillin- Resistant Staphylococcus aureus)? What bugs are we talking about?
Joyce: I’m not really sure. I don’t know exactly what bugs she has, but she has some kind of bugs that people are like … She’s susceptible. Because every time I go in there, you have to gown up.
Patrik: Wear gloves as well?
Joyce: Gloves, yeah. We have gloves and gown.
Patrik: Yeah, yeah. Probably VRE.
Joyce: What is that, do you know?
Patrik: Probably VRE.
Joyce: Yeah. Which means what? Sepsis? Or-
Patrik: Vancomycin-resistant enterococcus.
Joyce: She has a lot of antibiotic resistance.
Patrik: Yeah. It’s quite a common bug in hospitals, the VRE. And it’s a bug commonly known for long-term patients.
Joyce: So am I just waiting for something to brew now?
Patrik: I think so. I wish I had an easy answer for you, and I don’t. I don’t have an easy answer for you. What I will say to you is wait. That’s all I can say to you, wait. Because you have no other choice but to wait. Subacute, to a degree, it’s good that it’s not an option because you don’t want to-
Joyce: Oh, they would kill her in two seconds. And I wouldn’t want to put her through the horror. Honestly, as hard as this is, I don’t want her to … she’s too special of a woman to even … and because she’s mentally there, how horrific.
Patrik: Absolutely. If the health insurance came to you and said, “Hey, your entitlements are up. You’ve got to go to subacute next week,” that would be a different story. So as long as the health insurance is not breathing down your neck, I wouldn’t be too worried.
Joyce: Well, they have to find you one. They can’t tell me what to do if they can’t find me a place. It’s not like-
Patrik: Exactly, exactly. So it is-
Recommended:
Patrik: On that aspect, it’s actually a very unique case, because as you know from the past, as soon as you have a trach, they want to send you off to subacute, or to LTAC. The wound is stopping that, stopping her from taking those.
Joyce: That’s the only thing that’s stopping it. Listen, if it wasn’t for the wound, then I would’ve been maybe able to bring her home.
Patrik: Yeah, that would be easier.
Joyce: … that big of a deal. That’s not big of a deal. I can get a caretaker for whatever. You know what I’m saying? And the trach, not too big, I can suction … but then again, anything can go wrong with the trach too, from what I understand.
Patrik: Oh, look. The trach is, definitely for home care, a bit of a risk, which is why companies like us are coming in. But again, this is not available in your area unfortunately.
Patrik: So the biggest problem at the moment is probably the wound. And I wish I had an easy answer for you, and I simply don’t. What I will say to you is, again, quality of life is very subjective. And it looks to me like even living in this room, in this condition, with her family around is something that is worthwhile living, for her.
Joyce: Yeah, but she still wants to get the hell out.
Patrik: Of course, of course.
RECOMMENDED:
Joyce: I mean, she’s like, “I want to get out of here, I want to get out of here.” And I don’t know what to tell her. “Where are you going to go? Can’t come home, and you can’t go there. You’re stuck here.” She’s not going to want to … If I told her, “You’re going to be stuck here for the next X amount of time.” But no one’s really telling her.
Patrik: Right, but she would be asking.
Joyce: What do you mean?
Patrik: Is she asking what are the next steps?
Joyce: No. She just says, “I want to go home.” And I said, “You can’t go home because the wound is very, very bad. It’s severely bad.” And she stopped asking because we kind of gave her the scenario. Said, “If you’re frustrated, I understand. You make a decision. You want to pull off the tube, go ahead, we support you. Whatever you decide.” And ever since that, she has stopped even touching it, which would make it easier for us if she did. How horrible is this? I mean, I feel so..
Patrik: Horrible.
Joyce: … even talking to you about this because-
Patrik: No, I have these discussions all the time, and I am confronted with this-
Joyce: I feel guilty. I feel so guilty. I feel so guilty, because I feel so..
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!