Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can I Be in Control of the ICU Team To Do Everything They Can for My Dad’s Recovery?
You can check out last week’s question by clicking on the link here.
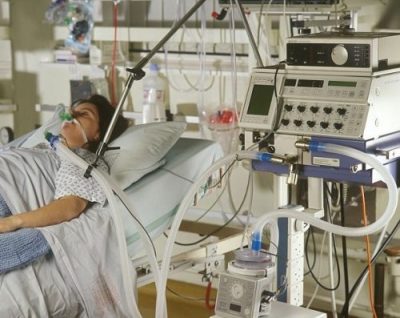
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Rosie, as part of my 1:1 consulting and advocacy service! Rosie’s dad is on a ventilator with COVID Pneumonia in ICU. Rosie asks if her dad will be able to recover when he is on paralytics for a month now.
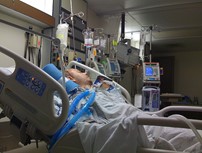
My Dad is on a Ventilator with COVID Pneumonia in ICU & is on Paralytics for a Month Now. Will He Ever Get Up & Recover?
Patrik: Hi Rosie! How are you?
Rosie: Oh well I’m good Patrik, but I’m worried about my dad.
Patrik: Can you share to me what happened to your dad?
Rosie: He had a tracheostomy done last week. They’re trying to wean him off Nimbex, a paralyzing agent, he had some reactions to that. So they… Because he’s been on Nimbex for a good three weeks before the trach. So-
Patrik: And-
Rosie: Go ahead.
Patrik: Why did your dad go into ICU? COVID?
Rosie: COVID, yes.
Patrik: Otherwise previously fit and healthy?
Rosie: Yeah, he had asthma, but other than that, everything was all right.
RECOMMENDED:
Patrik: He had Nimbex probably because he was proned?
Rosie: No, he had Nimbex because they ended up on intubation, and there was a lot of asynchrony with the breathing, so they gave him Nimbex. But they did try versed, propofol all that stuff before the Nimbex. They ended up putting him on Nimbex. Every time they reduced the dose of Nimbex there’s an asynchrony there. After the tracheostomy, they tried to wean him off the Nimbex. His heart rate went really high and he started having reactions to it, so they put him back on the three microgram dose. This last doctor that we had, titrated him. He would reduce the drip and give him a push when he had those reactions, so now he’s down to one microgram of Nimbex. But now-
Patrik: Are you telling me your dad has been on Nimbex for more than a month now?
Rosie: Yes.
Patrik: Oh, my goodness. How much? An hourly dose or a daily dose?
Rosie: All we know is the three microgram. So I’m assuming that-
Patrik: I would argue that’s per hour, I would argue that’s per hour.
Rosie: Okay, they titrated him down to one microgram now. He has a fluid overload, edema like crazy, so they were giving him the diuretic and Lasix, pretty much. So he’s peeing and they stop it, because kidney function goes too high and then they wait off on it until it levels, and they do it again. Now he’s voiding a lot. So, I do want to get your input on that?
Patrik: Yep, are you the medical power of attorney for your dad?
Rosie: Yeah, we are. Me and my brother are.
Patrik: Okay, great, great. Before I can give you some advice, what are they saying? What are they predicting are the next steps?
Rosie: What’s kind of funny is. He has a new doctor every week. With the new doctor every week we get… In the beginning, it’s all negative, and then next thing you know, then it becomes positive during the week.
Patrik: Yep, once they get to know him.
Rosie: Exactly. Right now he said the goal is to titrate him down, get him off the paralytic, get him off the medications. Get him off the fentanyl, and get him off all that stuff. But the kidney function is kind of worrisome, because it was… I think they gave us a 28 or something like that, and that dose of the… Or the result of that 28 is like… 15 is kidney failure. So-
Recommendations:
Patrik: Is he on dialysis?
Rosie: No, he’s not.
Patrik: Okay, when did they first start talking about kidney failure?
Rosie: This was actually pretty recent. Within the last couple of weeks, the nephrologist came to see him, went over his stuff. He said, “Hey, hold off on the Lasix and give it some time.” The doctor yesterday gave him Lasix, so I don’t know.
Patrik: What’s the prognosis of the COVID, does he have ARDS? Do you know what I mean with ARDS?
Rosie: Yeah, he does have ARDS, the chest x-rays showed both infiltration in the lungs, so that’s there. The last doctor said it’s little bit improving, but it’s still there. And he says, “Honestly, when you look at the patient, that’s how you know they’re getting better versus the chest x-ray, because the chest x-ray takes months to get better.”
Patrik: That’s right, that’s right. How old is your dad?
Rosie: He is now 77.
Patrik: 77, okay. Do you know if he’s on any pressors, or vasopressors? Do you know that?
Rosie: No, he’s not. He’s not right now.
Patrik: He’s not, okay.
Patrik: What else is he on besides the Nimbex? He’s on fentanyl? What else is he getting?
Rosie: He’s on fentanyl, Versed. They’ve given him blood pressure medication, because I know yesterday blood pressure was high. But I think because they did a CT scan, because when they did the trach, he was really… His belly was extended like crazy. They took him for CT scan, they found nothing there. They gave him some medications, some laxative medication, and that helped. Really what it is, is that, with that buildup of fluid, that’s when he has a problem weaning off those medications, when there’s a big fluid. But once they release that fluid, he goes down. It’s like perfectly, the medications start titrating now.
Recommended:
Patrik: Okay. With the blood pressure medications he’s getting, is he getting them intravenously, or through a feeding tube? Do you know?
Rosie: You know what, I think… I want to say it’s through the feeding tube, because they push medications through the feeding tube. I think they’re trying to limit the amount of fluid he’s getting through IV, just because he has a lot of edema.
Patrik: Yeah, sure, but even if they’re giving it through the feeding tube, they would still have to dilute it in water, so he would still be getting fluids. But anyway, okay. With the ARDS, what have they been doing so far? He’s never been proned?
Rosie: He was proned. When he was about 80, 70% oxygen on the vent, he’s been proned. But right now he’s between 40 and 45% on the ventilator.
Suggested links:
Patrik: Okay. How long ago? How long ago was it when he was last proned?
Rosie: He was last proned, I would say about two and a half, three weeks ago.
Patrik: Two and a half, three weeks ago. Okay. I tell you quite frankly, very rarely have I seen patients being on Nimbex for weeks, because that’s what it sounds like.
Rosie: Yep.
Patrik: The Nimbex is like… It’s a last resort drug. It’s like… You can’t ventilate someone, even if you’re sedating them, that’s when you give Nimbex. You’re giving Nimbex if you’re proning. As soon as you stop proning, you stop the Nimbex. As soon as you can start ventilating someone, you stop the Nimbex. Are you aware of any of the side effects of Nimbex?
Rosie: I know there’s a lot of delirium with it.
Patrik: Delirium. But my biggest concern is this, at the end of the day, the Nimbex is a paralyzing agent. My biggest concern with Nimbex is, when someone is in an induced coma, they’re not moving, they’re losing their muscles very quickly. On top of that, you’re using the Nimbex that is a paralyzing agent. I argue that if your dad gets out of this alive, it’ll take him months to just recover.
Rosie: And the doctor said that, yeah.
Patrik: Right, right, right. The Nimbex is not helping that. As I said, very, very rarely have I seen someone on Nimbex for more than a few days, maybe a week at the most. I’m very concerned there, and three milligrams, I argue that would be per hour.
Recommended:
Patrik: What’s your dad’s weight, roughly?
Rosie: He was about a 120 when he went in.
Patrik: So not heavy?
Rosie: No, he’s not heavy.
Patrik: Not overweight?
Rosie: No.
Patrik: None of that?
Rosie: No.
Patrik: That’s… Okay, so what is my take so far? I would really like to get even more information. I would really want to know why they are giving the Nimbex for weeks on end. Have you heard… Have-
Recommended:
Rosie: I got the doctor calling for my dad.
Patrik: I only have 15 minutes. I only have 15 free minutes, I can’t interrupt really. I’m too busy, sorry. I understand.
Rosie: It’s okay. Can I set up another appointment with you? And I’ll pay for it.
Patrik: My time…Yeah, yeah, definitely. Yeah, you can do that.
Rosie: I’ll do that.
Patrik: I’ll send you a link.
Rosie: Thank you.
Patrik: Thank you.

Patrik: Hi Rosie, can you hear me?
Linda: No..
Rosie: Okay, now I can hear you.
Patrik: Wonderful, wonderful, thank you. Thank you so much for coming on. We’ve got Rosie, and then we’ve got Linda?
Rosie: Yeah, it’s my brother and then I’ve got my sister on there too.
Patrik: Great, Great.
Patrik: So I’ve got three people, okay great. How can I help you?
Rosie: I know we touched base that other day. So, kind of give you a run down, pretty quick synopsis. My dad’s been in the hospital since end of year 2020.
Patrik: Right.
Rosie: He got a trach. He’s been on Nimbex pretty much the whole time that he’s been-
Patrik: Yes.
Rosie: … on there.
Patrik: Yes.
Rosie: The last doctor titrated him down to one by giving him pushes, to be able to get him down to one.
Patrik: Yeah.
Rosie: The doctor last night decided to put him back at 2.8.
Patrik: Per hour? That’s per hour?
Rosie: Yeah.
June: I believe so yeah.
Rosie: Then, essentially the doctor today, he told us he’s going to start a new sedative to wean him off the Nimbex. Giving him more Lasix and so on and so forth to get the fluid out because he’s really fluid overloaded right now.
Patrik: Yeah.
Rosie: So, kind of we want to get your insight, get your inputs since you’ve been around these situations before.
Patrik: Yes. Okay just remind me, so hospital admission did you say end of the year?
Rosie: Okay he was intubated right then.
Patrik: Yeah
June: Yeah, he entered the ICU days after.
Patrik: Right ICU and-
June: He was there maybe three days before on the regular floor.
Patrik: Okay and he does have COVID?
June: By now he did have COVID at that time.
Patrik: He had COVID.
June: I don’t know maybe by now he is probably-
Linda: COVID pneumonia is what they called it.
Suggested links:
Patrik: COVID pneumonia. As of today do you know whether that diagnosis is still present?
June: Pneumonia?
Patrik: Yes.
Rosie: Yes.
Patrik: Yes pneumonia and COVID pneumonia specifically?
June: So his x-ray show a lot of gray matter.
Linda: Infiltration.
Patrik: Yeah.
June: I’m assuming the answer is yes.
Patrik: Okay.
Linda: The doctor today said that 80% of his lung is involved in this.
June: Has infiltrates.
Patrik: Okay, I’m just making some notes. 80% okay. You mentioned COVID pneumonia, has the term COVID A-R-D-S been mentioned? Have you heard of A-R-D-S or ARDS?
June: Yes.
Rosie: Yeah, that’s what he has.
Recommended articles:
Patrik: It probably started with pneumonia and it’s now gone into an ARDS. Okay, Rosie as I mentioned to you on Saturday or Friday when we spoke, A-R-D-S often leads to the inability to ventilate because the lung is not open, the lung is more or less closed by infiltrates. Then you often end up on drugs like Nimbex. But I have not seen that for more than three or four days. But the Nimbex is a last resort drug if you can’t ventilate someone. So, you’re basically telling me he’s been on Nimbex for a whole month?
Rosie: Yes.
June: Yes.
RECOMMENDED:
Patrik: I’ve never seen that, never heard of it. Worked in ICU for 20 years I’ve never, yeah Nimbex sure, a common drug, last resort drug, temporary. Why is it-
Linda: That’s what they told us.
Rosie: He’s been on it for a whole month.
Patrik: Cool. What happens if-
Rosie: He kept on having this synchrony when they would get him off of it and they keep him back on it.
Patrik: Sure.
Rosie: That’s been the whole thing all the way through.
Patrik: Yeah.
June: So they attempted to take it off two weeks ago, two separate occasions. But at that time he was still intubated.
Patrik: What is he now? He’s not intubated?
June: He has a trach.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!