Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What Must the ICU Team Do in Order For My Dad to Come Off the Ventilator in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Richard, as part of my 1:1 consulting and advocacy service! Richard’s dad is with a breathing tube and on a ventilator in the ICU. Richard is asking why he should not trust the Intensive Care Team blindly whilst his dad is critically ill in ICU.
Why Should I Not Trust the Intensive Care Team Blindly Whilst My Dad is Critically Ill in ICU?
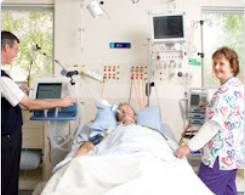
“You can also check out previous 1:1 consulting and advocacy sessions with me and Richard here.”
Patrik: Hi there Richard.
Richard: Hello. Patrik, you know what?
Patrik: Yes?
Richard: So my dad’s doctor is suggesting to do a tracheostomy?
Richard: Are you okay to get on a call with his doctor now?
Patrik: Yeah, sure.
RECOMMENDED:
Richard: Okay.
Richard: Patrik?
Patrik: Yeah.
Dr. Cole: Hello?
Richard: Okay I have Patrik on the line with me.
Dr. Cole: Yes. Hello?
Patrik: Hello?
Richard: Okay. So you’re requesting a trach?
Dr. Cole: Yes. This is Dr. Cole Who am I speaking with again? Hello?
Patrik: Hello?
Richard: Patrik?
Patrik: Yeah. My name is Patrik. I’m a family friend of Richard and his father. So you wanted a tracheostomy for him?
Dr. Cole: Yeah. He’s been in the hospital for more than 2 weeks on a ventilator. And it’s typically between 10 to 14 days, if patients are not expected to come off the ventilator in a day or two, we normally recommend tracheostomy. So now we are beyond that point. And from what I see on the chest x-rays, I don’t see any improvements enough to tell me that he’s going to be able to come off the ventilator in the next few days and to protect his voice box and prevent him from getting any type of sores in his mouth and to allow us to be able to move him a little more easily, I would recommend doing a tracheostomy. We will remove the tube out of the mouth, put it in the neck. He will be connected to the ventilator as he is right now, but this allows us to see if we could start working towards liberating him from the ventilator, because with a tracheostomy, it’s much easier than it is with a tube that he has in his mouth.
Recommended:
Patrik: I do understand when we spoke to the nurse yesterday that he’s currently on a propofol and fentanyl for sedation?
Dr. Cole: Correct.
Patrik: Has that been stopped in the past to see what he’s doing in terms of neurologically?
Dr. Cole: Neurologically he’s at baseline when the sedation is stopped? The only reason that he’s requiring those sedation is because immediately he gets very very tachypneic and he starts high pressuring the ventilator and oxygen count goes down, heart rate goes up. So he’s not suitable to be weaned of sedation under current condition. It’s easier to wean him of sedation with a tracheostomy than it is with a breathing tube.
Patrik: I understand that. Still, has maybe sedation been changed to a different..
Dr. Cole: Yesterday.
Patrik: Okay. What was previous sedation and what has been changed? Can you be more specific?
Dr. Cole: He was on propofol and Versed/midazolam and now he’s getting fentanyl as needed.
Patrik: Right? So propofol is off?
Dr. Cole: It’s not off, sir. He’s not on Versed/midazolam any longer. He’s on propofol and fentanyl as needed right now.
Patrik: Okay. Is he withdrawing from Versed/midazolam and from fentanyl? Is that part of the problem?
Dr. Cole: We cannot get him off the sedation right now because he gets tachypneic, hypoxic and tachycardic.
Patrik: Yeah, I understand. Can you please answer my question? Is he potentially withdrawing from Versed/midazolam or fentanyl? Both are addictive.
Suggested links:
Dr. Cole: No, he’s not.
Patrik: Right. What makes you so certain about that? What makes you so about that if he’s tachypneic?
Dr. Cole: Sir, because I’ve been in practice for 30 years and he has a lot of lung disease at this point that he’s not demonstrating any other signs of withdrawal from the medication.
Patrik: Okay. Has he been..
Dr. Cole: It’s a lung disease that he has.
Patrik: Yeah, I understand. Has he been tried to..
Dr. Cole: Very good. I’m glad that you understand, sir.
Patrik: And have you tried anything different like Precedex for example?
Dr. Cole: He’s not fit to come off the ventilator at this point, sir. His lungs are not good enough to come off the ventilator. So switching him from one sedative to another sedative is futile because his lungs are not fit to come off the ventilator at this point.
Patrik: Okay. And what’s his lung disease exactly? What’s happening with the lungs.
Dr. Cole: He has extensive pneumonia in both lungs.
Patrik: Okay. And then once you’ve done the tracheostomy you stop the sedation?
Dr. Cole: We do daily sedation vacation on that time. And then depending on how he does, how he behaves, we will work towards getting him off the ventilator.
Patrik: Okay.
Dr. Cole: We’ll be able to sit him up, have him breathe spontaneously if he’s capable of doing so and make an effort to have him come off the ventilator.
Patrik: Okay. So from what we understand yesterday, he’s in an AC (Assist- control) mode with rate of 60% of FiO2 (fraction of inspired oxygen) and PEEP (Positive End Expiratory Pressure) of 14. It’s a fairly fair amount of support.
Dr. Cole: The pressure readings are so high at this point, that it makes him not a candidate to come off the ventilator at this point.
Patrik: Yeah. No, I understand that. I understand that. Yesterday, from what we understood when talking to the nurse, his CO2 (Carbon dioxide) was very high in the 70s. What’s the reason for that?
Recommended:
Dr. Cole: Correct. Because of severe lung disease, because he has a high dead space, if you understand that terminology?
Patrik: Yes. I do understand that terminology.
Dr. Cole: High dead space in ventilation causes the carbon dioxide to go up.
Patrik: Okay. So since when did he have CO2 in the 70s? Has that been for many days? Is that a new thing?
Dr. Cole: It has been for at least 3 days.
Patrik: Okay. And if you’re increasing..
Dr. Cole: Because of the severe dead lung space.
Patrik: Yep. I do understand by bringing up the respiratory rate to, from what I understand, 26 yesterday, has that improved the CO2? What are his last readings?
Dr. Cole: All right. I’m not sure exactly what your intention are trying to test me on this point. The intention behind this conversation having you on the phone is to see if I can encourage..
Richard: If we can help my dad, make sure… Can I speak for a minute? Help my dad to make sure that we’re doing everything we can before we go to the last step. Okay? So these are things that we need to ask and we just need answers for. My opinion is that he barely two days ago received a medication for the yeast on the lungs and the WBC went from 21 down to 14. So the fact that it actually looks like it’s working, maybe in a couple more days he will be able to get off that ventilator.
Dr. Cole: It’s not a problem. There’s a ..
Richard: Hold on. Can I finish talking so you can understand where I’m coming from please? So when we do that and then he wakes up, he’s been on those medications, they are very strong sedation, he could easily have withdrawals. He had psych issues. Have we provided any psych meds to try to help him get off of that?
Recommended:
Dr. Cole: We cannot give psych medications.
Richard: Those are things that I need to make sure I go through before saying, “Yes, just give him a tracheostomy.” So if I can get these stuff answered, then I can say yes or no, I want to go with that. I can’t just say, “Just go with it.” And I know nothing about why and make sure that we tried everything we can. I know you guys always do everything you can, but as a family we need to ask these questions and get these questions answered. So we can make best informed decisions for my father.
Dr. Cole: Let me call you back.
Richard: He needs some psych stuff.
Dr. Cole: Richard, I’m going to have to call you back because I have a critical patient. Because it looks like I need to talk a little bit more extensively.
Richard: My dad is critical and we’re right here. We have 5 more minutes. Is there any more questions Patrik?
Patrik: There would be a few more questions, I guess. Doctor, a tracheostomy is a small operation. If Richard has all these questions, then it’s not as simple as you’re saying, you’re doing a tracheostomy. We need to find out what are the next steps? Why is CO2 so high? How long has it been? That’s what we’re trying to find out and there’s nothing wrong with that, is there?
Dr. Cole: Not a problem, sir. I’ll call you back in about half hour because I have a patient in front me that I need to address right away. I’ll give you a call back in about half hour. All right?
Richard: Okay.
Dr. Cole: Thank you.
Suggested links:
Richard: Hello?
Patrik: Yep. All right. Well, he was getting a bit short and he might have to attend to patient. I hear this over and over again when the doctors are telling me, “Oh yeah, I’ve been in practice for 30 years.” I respect that, but that doesn’t stop you from asking questions and getting answers.
Richard: Right, based off of his levels and what they have done and what they haven’t done.
Patrik: Yeah.
Richard: Why can’t we try different medicine?
Patrik: Exactly.
Richard: Why can’t we try these different things than just put a hole in his throat?
Patrik: Exactly.
Richard: You know my dad has psych issues, he’s been on psych medicine, so I know coming off these medicines, of course, he’s going to have side effects.
Patrik: Absolutely.
Richard: Who wouldn’t have a side effect coming off this stuff?
Patrik: Exactly. I want to know from him, why now? Why not 5 days ago? Why is his CO2 going through the roof? And him saying, “I’ve been in practice for 30 years.” That doesn’t cut it. Doesn’t cut it. What we might do Richard, call me back when he calls you back okay?
Richard: Okay.
Patrik: Thank you.
Richard: Thank you, bye.
Patrik: Thank you, bye.
Recommended:
Hi Richard,
It’s Patrik here from Intensive Care Hotline.
Richard, just quickly summarizing my thoughts from the call we had with the doctor. Look, obviously the questions that I asked I thought were all very relevant. He was not coming to the point and was trying to avoid the answers to the questions that I had, which might have been one of the reasons why he cut the conversation short. I would’ve had a lot more questions, including what is his approach going forward?
For example, he did say, well, they will try and start lower the sedation. Now, most of the time when someone is having a tracheostomy, they should be able to stop sedation straight away. If they can’t stop sedation straight away, again, it does come back to potentially withdrawing from medications. Because if you were to stop sedation, especially with fentanyl still going, if he starts withdrawing, he could be having all sorts of symptoms/side effects.
So therefore, I really believe the approach with sedation actually matters going forward. The whole purpose of a tracheostomy is to avoid/stop sedation straight away. The other question that I didn’t get answered was for CO2 (carbon dioxide) in the last blood gas, it was 74 or 75. That’s sky high. And he could not answer my question, A) Why? And B) what’s the approach going forward? They did increase the respiratory rate to 26 and they did increase the PEEP to 14, which can help with high CO2. But we don’t know whether this arterial blood gas and this CO2 result was before or after they’ve increased PEEP and the respiratory rate.
I would argue that the CO2 came first, then they would’ve increased the respiratory rate to 26 per minute. They might have increased the PEEP at the same time, and then they would’ve done another blood gas, and we don’t know the result. But again, we have to find that out, whether that was the case or not.
The other question that I would’ve had is around mobilization. Can your dad be mobilized? I have not seen anybody getting off a ventilator successfully without mobilization. And that includes mobilizing when patients are on breathing tubes and not on traches. He claimed that it’s much easier to mobilize your dad once he has the trach. And whilst I agree with that that should not stop them from mobilizing him while he’s having the breathing tube.
We also didn’t know, are they doing physical therapy? Have they done physical therapy? What’s their plan to move him off that ventilator? And again, that includes physical therapy. It includes breathing regimes. It includes breathing exercises. He hasn’t really talked about that.
RECOMMENDED:
What I also don’t know is what size tracheostomy does he have? Would also be important to know if they’re planning or what size tracheostomy he would be getting. It would also be important whether they might start with a size 7 or size 8, and whether then the plan would be to downsize that slowly and gradually.
So there are a lot of unanswered questions. And obviously, as you would’ve also seen, he said, “Oh, do you want to test me?” Well, it’s not about testing people. It’s about being transparent so that you understand the process. And that they understand we are questioning, and there’s nothing wrong with that. So I think the next step, really, is to try again and get on a call with the doctor again and get all the questions answered.
Take care for now.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







