Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Sister is in Intensive Care with Lung Failure and liver failure. Is This a Poor Prognosis? Help!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Arnold as part of my 1:1 consulting and advocacy service! Arnold’s sister has SLE and a severe case of ARDS in ICU, and Arnold is asking if the ICU team is giving positive options or just hindering her treatment.
My Sister has SLE and ARDS in the ICU. Is the ICU Team Doing the Best Treatment for Her or is End of Life Her Only Option?
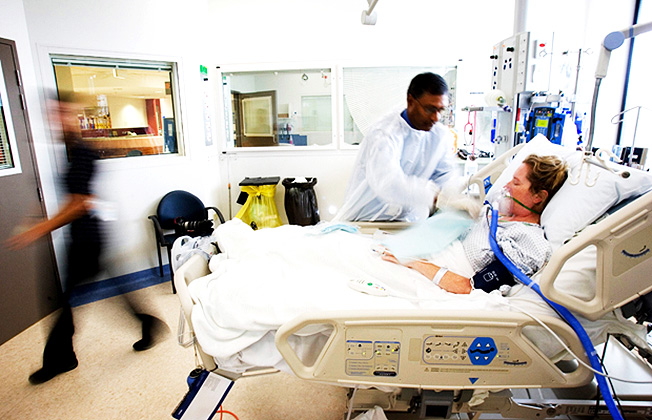
Patrik: Intensive care hotline, Patrik speaking, how can I help?
Arnold: Hi, Patrik this is Arnold.
Patrik: Yes.
Arnold: Good morning.
Patrik: Good morning, how are you?
Arnold: You already know, I don’t have to say how I am.
Recommended:
Patrik: No, that’s okay.
Arnold: Thank you for taking the call. What I’d like to do Patrik, I just spoke with Brian. The husband of Angelica. And of course he has power of attorney. So what I want to do, I just texted him and he said he can talk. So what I first want to do, I do want us to be on like a three way call because my dad is also in the car so I want everybody to be on the speaker phone.
Patrik: Okay. Sure. And do you know what they’ve done in order to get CO2 down to the 90s?
Just got to give me one moment. I’ll just bring up … yeah. And you mentioned in the e-mail yesterday that your brother-in-law Brian… that the ECMO was mentioned as an option yesterday. Is that correct?
Arnold: Yes, ECMO was mentioned as an option.
Patrik: Okay, an option. But then it was never mentioned again basically?
Arnold: Mm-hmm (affirmative) – they did say that ECMO was futile and that it wouldn’t be “in the best interest” of my sister. They said that she would only suffer unnecessarily and that she would die anyway.
Patrik: Ok. I am surprised … yeah … as I mentioned to you yesterday I’m surprised, it sort of was only brought up briefly as an option and when I heard you saying yesterday that your sister is 44. That was a bit of a shock to me. I mean … and then you mentioned she has ARDS two young kids and I just go like, “Ooph.” As I said wouldn’t you try, wouldn’t she go out fighting at least, I mean … but let’s come to that when your brother-in-law is there.
Arnold: That’s how I feel too, however, we feel that Brian has been brainwashed by the doctors in ICU and that he buys into the notion of stopping treatment, limit her suffering and letting her die. That’s why I suggested to him to book a call with you so you can talk more about the options from your experience. I have read on your blog that ICU’s sometimes are not open and transparent and therefore you don’t know what you don’t know and that we need to start asking the right questions.
Patrik: That’s exactly right!
Arnold: I now have Brian on the phone, let’s get him into the call.
Patrik: Absolutely. Yeah, yeah, yeah. Absolutely.
Brian: I’m here. Patrik, how are you?
Patrik: I’m very well Brian. Thank you. How are you?
Brian: I’m alright, exhausted and tired after all these weeks in ICU with my wife!
Patrik: Yeah I can only imagine. You know … so when I was talking to Arnold yesterday. I’ve worked in Intensive Care here for nearly 20 years and especially in the last few years I was looking after a lot of patients on ECMO. Specifically as a bridge to lung transplant and then also often post lung transplant. Right? You know sometimes people get a lung transplant and they do come back on ECMO after a lung transplant. Right? What I was surprised by what Arnold shared with me, was that they’re not even offering that option. I can tell you I have seen over the years some patients go on ECMO and…
Brian: They’re saying that she can’t have ECMO because she’s too weak and because she’s been in ICU for too long. It’s now been four and a half weeks.
Patrik: Yup. Right, right. Yeah, yeah.
Recommended:
Brian: They are saying that the risk of bleeding is too high when going on ECMO and that after all those weeks being ventilated and in the induced coma she has lost too much strength in order to cope with an ECMO.
Patrik: I see.
Brian: To make matters worse and to complicate the issue, she has Plasmaphereses because of her autoimmune disease. They are therefore saying that ECMO and a lung transplant is contraindicated.
Apparently they tried everything but that’s why we wanted to talk to you to check if they really did try everything?
Patrik: Mm-hmm (affirmative)-
Brian: She’s been on a high PEEP up to 15 and she’s been on 100% oxygen, but we’re not sure if that’s enough?
Patrik: High PEEP. Yup. Yeah no I understand that. Other treatment options for ARDS are things like nitric oxide, Epoprostenol/Prostacyclin nebulisers, Viagra/Sildenafil, prone positioning, hydrocortisone, antibiotics- if the ARDS is bacterial- but also induced coma, sedation, tracheostomy, temporary medical paralysation, pressure control ventilation, potentially high frequency oscillation ventilation etc…
Brian: I believe she’s been on antibiotics and the hydrocortisone. Not sure about any of the other stuff…
Patrik: Okay. Look I understand the situation now and the antibody situation is certainly a factor that seems to complicate things. I’ll tell you my thoughts though.
Many Patients on ECMO have dialysis for kidney failure and even though I haven’t seen plasmapheresis on an ECMO patient myself, because it’s so rare, I can’t see why it should be a contraindication.
The problem is that by now it might be too late.
Recommended:
Brian: Okay, no, no that is certainly … that is certainly concerning!
Patrik: Yup, yup. Most families in Intensive Care completely underestimate the gravity of having a loved one in intensive care. Have you heard of the term plasmapheresis?
Brian: Yes I have and they did that!
Patrik: They did that? Okay. Okay, they did that and with no success?
Brian: Yes, they have and it did work.
Patrik: Right Ok. Right and they’ve done that in the last eight days since she’s been in ICU?
Brian: Yes.
Patrik: Okay.
Brian: They said her blood pressure dropped every time they did it, but it looked like she was holding her own.
Patrik: Ok, I’m not surprised by it. The combination of ARDS, sepsis, ventilation, tracheostomy and then plasmapheresis usually drops blood pressure! Have you heard of inotropes or vasopressors?
Brian: No, I haven’t.
Patrik: When blood pressure drops to such low levels that is life threatening, inotropes and vasopressors can correct that temporarily. It’s considered life support!
Brian: Ok, I didn’t know that. You mentioned something earlier about ECMO and lung transplant with incurable ARDS?
Recommended:
Patrik: Yes, ECMO can be used by giving the lungs a break and giving the lungs time to recover, because oxygenation can take place via the ECMO machine as opposed to the lungs. This also buys time to put patients on a lung transplant list to increase the chances of a lung transplant if ARDS can’t be cured. I would imagine that at your wife’s young age of 44 and having two young kids, they would have considered ECMO and a lung transplant?
Brian: Yes, she was on the transplant list a couple of weeks back, but she has been taken off the transplant list.
Patrik: Right. Do you know why?
Brian: They said that with the plasmapheresis for her lupus and her deteriorating condition she wouldn’t be a candidate!
Patrik: Ok, when your wife went into hospital, and when she went into ICU prior to that she was mobile?
Brian: Yes she was fine. But she was getting weaker and weaker because of her deteriorating lupus condition.
Patrik: Right, she was walking?
Brian: Less and less but she was walking.
Patrik: Right, and she was on home oxygen prior to that?
Brian: Yes, she was on home oxygen.
Patrik: Okay … the antibody situation is certainly a complicating factor. Not being able to walk and being in an induced coma from my perspective and from my experience are not a reason not to put her on a transplant list or to take her off it.
Taking her off the transplant list is inappropriate from my experience. Right? People are in induced coma. When in induced comas when going on ECMO and bridging them to a lung transplant. It takes a long time to recover after an induced coma. Right, and the lung transplant certainly would be a complicating factor in recovery but it’s still, I’ve still seen it being done.
Recommended:
Brian: They have been telling me that she wouldn’t survive ECMO and a lung transplant.
Patrik: Did you ask them why?
Brian: Yes, but they just said that she wouldn’t survive. How would I know?
Patrik: Right, right, okay. No that’s good, so, because that argument as far as I’m concerned is not present. Right? I mean it has to be dismissed from my perspective. Especially at such a young age. You know? So then let’s just run this through, the argument, because she’s not able to walk right? That’s why they’re not putting her on ECMO and that’s why they’re not putting her on a transplant list. That to me is not an argument that would stand as a clinical argument.
Would it make a recovery harder? Yes for sure, but at such a young age they have try everything from my perspective.
Brian: Right, right. They also kept saying that her CO2 is too high, does that make sense?
Patrik: Yup, absolutely it does. I can tell you that if they put her on ECMO, CO2 would come down within a couple of hours.
Brian: Right. They also said that with her autoimmune disease lupus would make it more difficult to recover.
Patrik: Ok, nevertheless is lupus not an absolute contraindication for a lung transplant, there is research out there, I will send you the link when we come of this call.
Recommended:
Brian: Yes, that would be great!
Patrik: Yeah. I totally appreciate that finding a lung donor might be difficult. If however, they did put her on ECMO, you know let’s just say today and you know they took that minimal chance to find a donor. It’s still a minimal chance. I mean if they let her go. You know, I mean it’s not … it’s she’ll be gone you know, I mean that’s … you know those are the odds from my perspective. I tell you another thing and that could be you know, have they-
Are they saying anything about her age in terms of, has that ever been a point of discussion?
Brian: They haven’t brought up her age, however now that I understand more about the issues, I feel that more could be done, for sure.
Patrik: Yeah. So I have seen, sort of the highest age that I’ve seen patients receiving a lung transplant is really sort of sometimes late 60s, like 65, 68 sometimes. I just see your wife Angelica in a … at her young age, two young kids. I just feel like this is … every situation is unique but wouldn’t that be a chance they would have to take. I mean end of life in Intensive Care, that’s a reality don’t get me wrong. That’s a reality but wouldn’t that be that one in I don’t know, have they given you numbers? Is it one in 1000? Is it one in a 1,000,000? Have they given you any numbers in terms of odds?
Brian: They said that her odds to survive are very low, but they didn’t give me any numbers.
Patrik: Ok. Fact is that ECMO would give her a second chance, period. Why would they not take it? It would buy her time to either recover or to go on a transplant list.
Brian: What do you think we should do now?
Patrik: First off, Can they … let’s face it, can they cause more harm? I mean the situation is dire as it is. I mean the situation is incredibly critical. I mean can they, the question is can they cause more harm? Let me ask you another question and I know you might have mentioned it in the beginning. When was the very first time you were made aware of ECMO? When was the very first time?
Brian: Two months ago.
Patrik: And … What was your wife’s view on the worst case scenario? I mean if your wife would be able to make the decision, what do you think she would do?
Brian: I think she would have taken the chance.
Patrik: Right. Sure. That’s important.
And just let me ask you this once again. At what stage did they take your wife off the lung transplant list? At what stage?
Recommended:
Brian: Two weeks ago.
Patrik: And when did she get on the lung transplant list? How long was she on it?
Brian: She was on it for a couple of weeks and then they took her off it.
Patrik: Okay. And with her underlying disease is there also cystic fibrosis or any other medical conditions that are important?
Brian: No not really.
Patrik: Right and how long has she been living with the lupus?
Brian: For about five years. They also mentioned that rejection after a lung transplant could be an issue.
Patrik: Okay. Rejection in lung transplant patients is always an issue, right? With the situation that you are describing, I mean rejection in a lung transplant is a big issue, right? With the antibodies … with the antibody issue it’s certainly complicating the situation. There’s certainly no doubt about that. Right? It sounds to me like also if they did put her on ECMO they wanted to do the trach first. Which makes sense to me and I can tell you why it makes sense. She … Once she is on ECMO she would get some heparin. Are you aware? Have you heard of heparin?
Brian: Is Heparin the blood thinner? They also said that if she went on ECMO that she would need Heparin…
Patrik: Yes of course she would. And she would, yeah, she would get more probably while on ECMO. So they would have to stop the heparin to do the tracheostomy and then put her on ECMO. Right, and then we start the heparin. Right? That’s … those are certainly all fairly high risk components of the situation. Right? There is no doubt about that. Right. At the same time not doing anything or just sort of going along with this current situation will most likely lead to end of life. Putting her on ECMO will buy her time and increase the chances that you might get a set of donor lungs. The … ECMO is a high risk procedure, there is no doubt about that. At the same time not doing, not putting her on ECMO will most likely kill her…
Brian: They also suggested that once a tracheostomy has been done that CO2 levels would come down. But they also said that a tracheostomy would be too risky!
Recommended:
Patrik: Why are they suggesting that once a trach has been done, CO2 level would come down? That doesn’t make a lot of sense to me.
Brian: I’m not sure.
Patrik: Yup, the other thing that I don’t quite understand is that you mentioned that they re-sedated her. Was her CO2 in the 90s or even in the 100s, it’s unlikely that she will wake up. It’s almost like an, you know the higher CO2, the more drowsy a patient and I argue that she wouldn’t wake up anyway unless they get the CO2 down.
Brian: I understand. Last week, she was more rousable after they lessened the sedation. I believe they took off the Propofol for a while but then after a few hours they couldn’t ventilate her because she was too awake. They ended up re-sedating her and then they even had to paralyse her from what I remember.
Patrik: So when you’re saying last week she was rousable when they reduced the Propofol do you know if CO2 came down?
Brian: I think it did in the beginning but then they had to paralyse her as I said as she was fighting ventilation.
Patrik: Ok, I understand. Yeah, ARDS is tricky, the lungs are completely fibrotic and getting air into the lungs is a big challenge, hence paralysing agents can be used. Once again, ECMO is the better option.
Patrik: Do you know what her baseline CO2 was before going to hospital?
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Brian: I think it was about 55…
Patrik: Right. Okay. Yup. So … but with that in mind, with such a high baseline CO2. If you look at the CO2 of 70 … CO2 of 90, it’s high but for them with a high, if you’re starting with 65. It’s actually not that high. If somebody has a normal CO2 as a baseline and they have a CO2 of 50, that’s double. You know? And…
Brian: Right. I see.
Patrik: Is she septic? Do you know what I mean by that? Is she having a sepsis or is she in septic shock?
Brian: I’m not sure.
Patrik: Chances are that your wife is septic with ARDS. Who is making the decisions? Is it a pulmonologist? Is it an ICU consultant? Is it a combination of those? Who’s making the decisions?
Brian: It’s both, the ICU consultant and the pulmonologist.
Patrik: Yeah, of course absolutely. Can I ask you what might be a little bit of a confrontation or question? Have you 100% ruled out that they don’t have the resources available at the moment to make that happen?
Brian: What do you mean?
Patrik: Okay. Again, after 20 years of ICU, I’ve seen … I claim, I’ve seen everything. I probably haven’t seen everything but I’ve seen enough to ask that question. The worst case scenario for the ICU is to look after a patient indefinitely with an uncertain outcome. Your wife could fit that criteria if on ECMO and vying for a lung transplant. If your wife dies they just prevented their worst case scenario.
Brian: Right.
Patrik: Okay? Just clinical realities.
Brian: Clinical realities. Yeah. Mm-hmm (affirmative). They also said that doing a tracheostomy with a high CO2 it can’t be done.
Recommended:
Patrik: Yup. No I understand and the risk … the risk to do a trach with a CO2 of 90 plus is hi- … it’s huge. Her PEEP would be above 10 I would imagine. That’s a huge risk to do a tracheostomy, no question, but it can be done. But … Yeah, so I understand all of that, that the risk just to do a trach is pretty high. The reality is that to co- … in order to continue treatment. Right? Whether that’s a tracheostomy and then potentially ECMO. The risk is huge there is no doubt about that. The risk is … when people go on ECMO they’re really the sickest patients in an ICU generally speaking. Right?
Brian: Do you think they can take that risk?
Patrik: So the risk is massive, there is no doubt about that. Not doing anything you can expect end of life. Right. Your wife will die by sheer inaction. As you said, “Shooting for the moon.” Would increase a small chance for survival, right. Most patients that I’ve seen in ICU going on ECMO for a bridge to a lung transplant, take a small chance. Right. They really do take a small chance because number one ECMO is high risk and number two nobody knows whether a suitable donor lung will become available. Right. Those are the realities and risks that need to be taken into consideration in a situation like this.
Brian: So you think that she will die because of her not going on ECMO?
Patrik: Yes, correct. Yup and that again usually changes the minute somebody goes on ECMO. Right. So for example somebody might come into a situation like that. They’re not on the transplant list. They do go on ECMO as a last resort and the minute they go on ECMO they are on the transplant list. Right?
Brian: Understood. So do they need to tick certain boxes to get her on the transplant list?
Patrik: Yes they would. Those are all realities and I’m not disputing them. It’s a very difficult situation. And the other thing again don’t get me wrong but I’ve seen it. If they do put her on ECMO for a week. Again, they might think … or even for two weeks. They might think in the back of their minds, “Okay. We put her on ECMO for two weeks. We potentially don’t get a donor lung and we’ll take up an ICU bed for the next two weeks that we could use for somebody else.” Right? So they are certainly considerations they would run in their mind as well, not necessarily sharing them with you.
Also, ICU’s are chronically short staffed and therefore they are thinking twice if they can use the staff for something else, I.e. other patients.
Brian: Yup. Yes. I have seen empty beds though.
Recommended:
Patrik: And most ICU’s are short staffed. So just because you are seeing empty beds doesn’t necessarily mean they can staff for those beds.
Brian: Ok.
Patrik: Yup.
Brian: I do have to go now, because I have to pick up my kids. You’ve thankfully given me enough to think about and I might book some more time with you going forward. I will talk to the team again first.
Patrik: You’re welcome. All the best. All the best Brian for now.
Brian: Thank you. Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!