Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
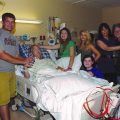
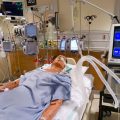
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Arnold as part of my 1:1 consulting and advocacy service! Arnold’s sister had a severe case of ARDS and in the ICU, and now Arnold is asking if there is any way to prolong her life while waiting for a transplant.
My Sister is in Intensive Care with Lung Failure and liver failure. Is This a Poor Prognosis? Help!
Arnold: Yes, hello?
Patrik: Hi, is that Arnold?
Arnold: Oh yes, hello.
Patrik: Yes, Patrik here from Intensivecarehotline.com, how are you?
Arnold: Hi, hi Patrik. So glad that you’re calling. Thank you so much.
Patrik: You’re very welcome. So your sister is not in a good situation is she?
Recommended:
Arnold: Yeah, they said that her CO2 levels have risen to like over 100 and they keep going up and what is it?-
Patrik: Why? Do you know? Tell me, we’ve got about-
Arnold: Well she had lung failure. So she was originally at Blue Hospital to try to get a lung transplant but unfortunately she didn’t get a match and now just recently they said that to keep her alive they have to put her on an induced coma. That was about eight days ago and now today they’re saying that pretty much there’s no more hope, that the CO2 levels are too high and they’re only gonna go higher and higher and cause toxicity for the liver and the kidneys.
Patrik: Yeah. No, I understand. We’ve got about 15 minutes because, you know, I always have 15 minutes, I’m afraid. But that’s okay.
Arnold: Sure.
Patrik: So, is your sister still on the lung transplant list? They have not taken her off because of the issues have they?
Arnold: They have taken her off. They have taken her off. They said that her body would not be able to withstand the transplant.
Patrik: Okay.
Arnold: Even if she got new lungs.
Patrik: How old is your sister?
Arnold: 44.
Patrik: Okay. Have you heard of ECMO Therapy?
Arnold: What kind of therapy?
Patrik: ECMO. E-C-M-O. Have you heard of that?
Arnold: Let me write it down. No, I’ve never heard of it. Can you say it one more time?
Patrik: Yeah so it is E for Emma.
Arnold: Yeah.
Patrik: C for Cynthia.
Arnold: Okay.
Patrik: M for mother.
Arnold: Yes.
Patrik: And O for oxygen. I will send you some information when we come off this call.
Arnold: Okay.
Recommended:
Patrik: So I’ll give you the short version. I’ll give you the very short version.
Arnold: Yeah.
Patrik: When somebody is in severe lung failure … And let me ask you this, why? What’s the primary diagnosis for your sister in terms of lung failure? Is it CF? Is it? Do you know the primary underlying reason?
Arnold: It was like really severe scarring of the lungs. She was hyper sensitized to something that … I can’t remember the medical term but she was only … Her right lung was done, her left lung was on 20% and then she was using the machines, the oxygen machines to breathe.
Patrik: At home.
Arnold: But not the ventilator. No, not at home, at the Blue Hospital because-
Patrik: Right, right, right, right. How long has she been hospitalised for now?
Arnold: So about two months.
Patrik: Two months. And how much of that time has she spent in Intensive Care?
Arnold: Eight days.
Patrik: Eight days. So Intensive Care is fairly recent?
Arnold: Yes. It is.
Patrik: Okay. Okay so I’ll give you … So ECMO is really important.
Arnold: Okay.
Recommended:
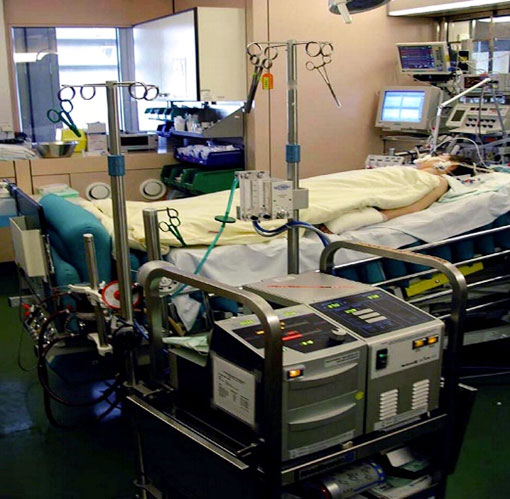
Patrik: So, when patients go into lung failure, right? When patients go into lung failure and the lungs completely shutdown, which it sounds it happened in your sister’s situation, right? You can put them on ECMO. Now, what does ECMO mean and what does it do? ECMO in essence is a by-pass machine. It’s basically bypassing the lungs, taking over the function of the lungs for a period of time, right?
That’s number one, would give a patient’s lungs time to recover. Or number two, gives patients the time to wait for a lung transplant, right? I tell you what I believe is happening in your sister’s situation without knowing the ins and outs. I do believe that ECMO in this hospital is not available. Either that or … Because it’s very specialised. I mean Intensive Care is much specialised but there are not many hospitals who offer ECMO, right?
Arnold: Mm-hmm (affirmative).
Patrik: So, having said that though, if they put her on the lung transplant list in this hospital, there is a chance that ECMO is available, right? I don’t know. What’s the name of the hospital and where is it? What’s the name?
Arnold: They’re one of the best for lungs. Blue Hospital in Arizona.
Patrik: Blue Hospital in Arizona. Just give me one sec because usually they would have advertised on their website.
Arnold: Brenshaw.
Patrik: Brenshaw. Yeah, no, it comes up. Just give me one sec. It’s in Clarke?
Arnold: It is in Clarke, yes.
Patrik: Okay, yeah. I found it. I’ll just quickly have a look on their website.
Arnold: Sure.
Patrik: So, why is it important, Arnold? During my time in Intensive Care I looked after a lot of patients on ECMO, waiting for lung transplant or potentially even sometimes after lung transplant, right? So this for me is standard treatment. Okay?
Arnold: Mm-hmm (affirmative).
Recommended:
Patrik: I don’t know … Especially at your sister’s age, you know, that’s very young. Let me just … Just give me one more moment please. I can find the Blue Hospital but I can’t find … So just give me one sec. Blue Hospital.
Arnold: That’s fine. No problem.
Patrik: Clarke. ECMO. Let me see what comes up. It comes up for paediatrics. It comes up straight away for paediatrics but not for adults. Are you the medical power of attorney for your sister?
Arnold: No. No. I guess it’s my brother-in-law, her husband.
Patrik: Yeah, yeah. And you are not physically present … You are in Georgetown and you are not-
Arnold: At the minute.
Patrik: At the minute.
Arnold: At the minute, yes.
Patrik: Yeah.
Arnold: And it was today we got this information, yes.
Patrik: Right. So, it comes up for ECMO for paediatrics which is for children but it doesn’t come up for adults.
Arnold: Mm-hmm (affirmative).
Patrik: Okay just give me one sec. It’s still … When I’m on their website, I’m on their website and I’m typing in ECMO, the search thing that comes up is paediatrics.
Recommended:
Arnold: Mm-hmm (affirmative).
Patrik: Okay so I can tell you what I … Look, CO2 going up during lung failure is normal, right? That’s one of the effects.
Arnold: But how high can you go and a person still come back and survive?
Patrik: Look I’ve seen up to 120. The other question that I would like to ask, you know, is are they giving steroids? Are they giving nitric oxide? Are they giving flolin inhalers, right? I can email you all of that, you can ask those questions.
Arnold: Yeah, yeah.
Patrik: So my question at the moment is, what are they doing? Are they still proactive? And I agree that if she’s in severe lung failure and they’re not doing anything, she will pass away in the next few days. I probably agree with that, you know, without knowing … You know, I would like to know more but the first thing that stands out to me Roman is where is ECMO? That’s the first thing that comes to my mind.
Having worked in a lung transplant centre for a long time, I have seen those situations. And I know how the Intensive Care Unit could buy time. Is there a guarantee if they put your sister on ECMO that she will get a lung transplant? No, there’s no guarantee but it will buy her time.
Arnold: That’s all we want right now is buy a little time because apparently they’re in the room right now, her and her husband and the two kids and they’re pretty much just spending the last moments with her.
Patrik: Right, right.
Arnold: And I said, “You’re not gonna take her off this.” And they said, “No, we’re not gonna take her off any of the machinery, just her body will give out.”
Patrik: Yeah. The concerning part Arnold to me is that the real concerning part to me is that they haven’t been transparent with you. That’s the concerning part. You know, I mean, if you’re telling me your sister is 44, she’s got a husband, she’s got two young kids and they are not open and transparent with you that ECMO could be a lifesaver potentially. If they don’t have ECMO available fair enough but then please refer her on to an ECMO centre.
Recommended:
Arnold: Okay, no, I didn’t know anything about ECMO. This is the first time I hear about it. Now, there is, brother-in-law’s brother there that he works for the Bishop Lung Department so he’s presently there right now so I don’t … Of course, he probably would know what ECMO is of course.
Patrik: He would. And who is that? Did you say your brother?
Arnold: No so it’s the husband and then it’s the husband’s brother.
Patrik: Oh okay.
Arnold: That works for Bishop Lung. So he’s there right now and so is my … Her husband is there right now.
Patrik: Right. And is your brother-in-law’s brother a medical doctor or …?
Arnold: He’s like the head or manager of the lung department, nurses over there at Bishop Hospital.
Patrik: Well he should know. He should know. However, look, he should know. However, I can tell you, if you worked with patients on ECMO … I looked after I don’t know, thousands of patients on ECMO, right? So if you haven’t had that hands-on experience, you may know about it in theory but if you haven’t had the experience and literally done hands-on work with those patients, you may know what it looks like in theory but if you haven’t had that hands-on exposure, I’m not sure. I think you need to ask the question.
I think you need to ask the question in the next hour.
Arnold: Yeah. Yes about ECMO.
Patrik: What I will do Arnold, I’ll tell you what the next step is. I will email you. So we have information about ECMO on our website. I will email that to you literally when we come off this call, okay? I will also email you a couple of links to some case studies where we worked with people on ECMO, how we helped them. Right?
Arnold: Okay.
Recommended:
Patrik: From my perspective, one of the next steps is to get on the phone again with you and potentially with your brother-in-law and tell you more but the first thing I’ll do is I will send you a link to our ECMO section on our website.
Arnold: Mm-hmm (affirmative).
Patrik: I will send you a couple of case studies.
Arnold: Mm-hmm (affirmative).
Patrik: And the next step really that I can see is to get the ball rolling in there and ask them why are they not transparent? Why are they not even bringing this up as a point of discussion?
Arnold: Yeah. And it could be possible that they have brought it up but I just don’t know about it.
Patrik: Right.
Arnold: So yeah I’m gonna-
Patrik: Sure, sure. So, that would be the next step.
Arnold: Yeah, okay.
Patrik: So if you give me about 10 minutes I will send you some information. If you then want to proceed with some help, for example, what I do then, what I could do. I could get on the phone with you and your brother-in-law, I could also get on the phone with the doctors and ask them some I believe, significant questions, you know?
And if you then wanted that I would charge a fee for that but let’s just start, you can ask the questions and you can, you know, go from there.
Arnold: Sure. Okay that is understandable. My concern right now is that they’re saying that once she feels enough pain, I think the sedation is at 10 right now, they’ve definitely lowered it. But they said that once she feels enough pain they’re gonna sedate her again and they’re not anticipating that she’s gonna wake back up back from that sedation.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Yeah. So, I tend to agree with that, especially if her CO2 is so high. Right? I tend to agree with that. Again, to me, when a patient is in a situation like that, if they started ECMO in the next hour, right? And I’m just saying that. Her CO2 would come down in no time. Her CO2 would come down in an hour, in less than an hour.
Arnold: Okay then yeah.
Patrik: So I can see that they’re pushing towards end of life. I can see that, right? But they haven’t been transparent with you, that’s the problem. You know, you haven’t given ECMO as an option. Or if they did mention ECMO as an option to your brother-in-law, I don’t think they… You know, they might have sort of mentioned it but I don’t think they’ve given him the full story. What-
Arnold: Yeah.
Patrik: Right? That is where the problem is.
Arnold: I see. Okay I understand fully Patrik. Okay please send me that stuff. Time is of the essence right now so I have to-
Patrik: Absolutely.
Arnold: Patrik, would it be okay if I put my brother-in-law on, to see if he would pick up the phone, on the call with us?
Patrik: Yes. Yes. Do that. But please bear in mind, my time is limited and I can really not dedicate a lot more of my free time towards this.
Arnold: Yeah, I understand.
Patrik: But not a problem. Quickly call, talk to your brother-in-law. See what you wanna do next. And please get back to me. Please look out for the email that I’m sending you in the next five minutes. Okay?
Arnold: Okay. And if I do want to talk to the doctors, I mean I don’t have … We’re not immediate family so do I have any rights to do anything or it has to go through my brother-in-law?
Patrik: Yes, probably your brother-in-law would be the medical power of attorney most likely, wouldn’t he?
Recommended:
Arnold: Yeah.
Patrik: Right. Now it’s probably best-
Arnold: And he’s not picking up calls right now.
Patrik: I see. Look I mean, in a situation like that. If you can’t get hold of your brother-in-law, you know, in a situation like that, it’s probably best to try and get on to the doctors. I mean, you know, your brother-in-law is probably so distressed and you can’t blame him for it.
Recommended:
Arnold: Right. Okay. I will definitely reach out. Please send me that email and then I’ll keep you in the loop as far as what’s gonna happen.
Patrik: Please. Yeah, okay.
Arnold: Thank you. Thank you Patrik. Thank you so much.
Patrik: Thank you. Bye.
Arnold: Okay bye.
Patrik: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!