Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another frequently asked question our readers and the question in the last episode was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another frequently asked question from our readers and the question this week is
Can a tracheostomy be reversed?
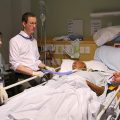
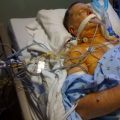
Many mechanically ventilated Patients in Intensive Care in an induced coma require a breathing tube/endotracheal tube to facilitate such mechanical ventilation during critical illness.
The goal should always be to wean mechanical ventilation, get a critically ill Patient out of the induced coma, get them extubated (removal of the breathing tube/endotracheal tube) so that they can breathe spontaneously and unaided so that they can leave Intensive Care and eventually go home.
Related articles/videos:
If for whatever reason, weaning off mechanical ventilation and the breathing tube/endotracheal tube fails, a tracheostomy might be considered as a next step.
When is the right time and right situation to do a tracheostomy?
I’m glad you asked!
Here are articles and videos that will give you all the knowledge you need if your loved one should have a tracheostomy or not
Once a tracheostomy has been done, your loved one can hopefully take the first steps to wean off ventilation and tracheostomy!
Once the ventilator has been weaned, then the next step is to remove the tracheostomy!
Here is a word of warning for our readers in the United States who have a loved one in Intensive Care.
Often, a tracheostomy is being used as a conduit or vehicle to get your loved one out of Intensive Care as quickly as possible and move them to LTAC (long-term acute care facility).
Let me be blunt here. If your loved one was to leave Intensive Care on a ventilator with tracheostomy and go to LTAC it could be the death sentence for your critically ill loved one!
We have families approach us every day, literally begging us to help them get their loved one out of LTAC back to ICU.
Why? Because the only safe place for a ventilated Patient with tracheostomy is either ICU or INTENSIVE CARE AT HOME.
LTAC’s simply don’t have the skills or expertise to wean Patients off ventilation and tracheostomy.
Here is a link to a case study how we helped one of our clients to stay in Intensive Care instead of going to LTAC or long-term acute care after having a tracheostomy. The outcome was successful consulting and advocacy where the client’s Dad was able to be weaned off ventilation and tracheostomy in ICU!
How does ventilation get weaned when having a tracheostomy?
I’m glad you asked!
Here are articles and videos that will explain it for you!
In most cases, a tracheostomy is temporary, providing an alternative breathing route until other medical issues are resolved. If your loved one needs to remain connected to a ventilator indefinitely, the tracheostomy is often the best permanent solution.
The Intensive Care team will help you determine when it’s appropriate to remove the tracheostomy tube. The tracheostomy hole (also known as tracheotomy) may heal or shut on its own, or it can be closed surgically.
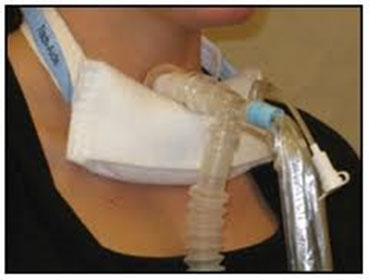
In order to have the tracheostomy removed (decannulation) your loved one needs to be off the ventilator completely and can breathe via trachea mask, trachea hood, trachea collar or trachea shield then it’s time to assess if your loved one can have the tracheostomy removed!
Certain criteria need to be met for tracheostomy decannulation such as
- Good strong cough/gag needs to be present in order to protect the airway
- Swallow reflex needs to be present so that your loved one is not aspirating secretions, sputum, gastric content or food
- Able to obey commands (In the non- neurologically compromised patient)
- Adequate cough and ability to clear secretions effectively and independently.
- Cardiovascular and hemodynamic stability.
- No new lung infiltrates on chest x-ray.
- Tolerates cuff deflation for 24 hours.
- Tolerates speaking valve 12 hours or more (usually during daytime) or decannulation cap for up to four hours (If air flow is present on finger occlusion). In patients following head and neck surgery, the decannulation cap may be left for longer periods at the discretion of the surgeon
I hope this answers all of your questions!
Also, as a quick tip, if your loved one is stuck in ICU, LTAC (god forbid) or even at home with ventilation, tracheostomy or even without ventilation but with tracheostomy, have a look at INTENSIVE CARE AT HOME.
INTENSIVE CARE AT HOME is providing a specialist service, sending highly skilled Intensive Care nurses in the home to either get your loved one out of ICU or put of LTAC and/or keep your loved one at home with ventilation and tracheostomy as a genuine alternative to a long-term stay in Intensive Care/LTAC!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!