Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Tracheostomised Husband Is In ICU. Is Skipping LTACH A Better Option?
You can check out last week’s question by clicking on the link here.
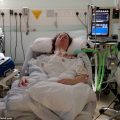
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Kaye as part of my 1:1 consulting and advocacy service! Kaye’s husband had a cardiac bypass surgery and is on tracheostomy in the ICU and Kaye is asking if the insurance plays a role in placing him into a skilled nursing facility.
My Tracheostomized Husband is in the ICU. Is a Skilled Nursing Facility Better for Him?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Kaye here.”
Kaye: No, I don’t think so.
Patrik: The other question I think is quite important, Kaye, you are the medical power of attorney at the moment for your husband?
Kaye: Yeah I do.
Patrik: There’s nobody-
Kaye: No one else, only me. Yeah.
Patrik: Okay. That’s very important. Those are your next steps.
Kaye: What?
Patrik: I said those are your next steps in terms of moving through this. The positives that I can see already are your husband is off the ventilator and your husband is ahead of most other inquires that I’m dealing with from similar situations, right? Your husband is ready to go to LTACH. There is no doubt about that. Other inquires that I’m getting in similar situations are that people are not quite ready to get to LTACH, but your husband is ready.
Kaye: Yeah, yeah, yeah…
Eric: It’s a question of whether it’s an insurance thing or doctor. I’m kind of pretty-
Recommended:
Kaye: Insurance. It’s insurance. She told me straightforward that insurance did not approve him for LTACH because he did not meet criteria. She told me out openly about it. She said that without-
Patrik: We need to find out what the criteria are.
Kaye: I can ask for the old copies of the documents for the medical insurance. I want to see it.
Patrik: That’s probably a very good thing. I think what you should be doing, is you should be requesting the medical records anyway. You have the right to request medical records at any time. You know this is your right and I think you should just to keep the pressure on. Just to communicate to them, “Look we are doing our own research” and take it from there, you know?
What insurance is your husband insured by? Is it Medicare or Medicaid?
Kaye: Both, both. Medicaid and Medicare.
Patrik: Okay. I can tell you that with Medicare, all the clients I have been working with in the past, usually Medicare doesn’t have a problem sending people to LTACH. I don’t think it’s state-dependent. I understand you’re in Ohio, but I don’t think it’s state-dependent. I get inquires from every state really. If there is an issue with Medicare, it’s usually down the track. If people don’t get off the ventilator within, I believe it’s six months in LTACH, then they want to move them on to a skilled nursing. That’s what I’ve certainly learned about Medicare, right?
Eric: So, you are kind of saying our time is not up yet. We’ve got plenty of time.
Patrik: I think you have.
Eric: Yeah.
Patrik: I believe so, right? That’s one thing I definitely have to learn about Medicare is that after about six or twelve months, I can’t remember the time frame is, it’s either six or twelve months in LTACH, and people can’t rehabilitate for whatever reason, then Medicare says, “Okay your time is up, you need to go to skilled nursing or somewhere else.” But that point-
Kaye: Patrik, did you ever hear something like this? Someone told me, and I’m not sure if it’s true or not, they said that Medicare is not like Medicaid. It’s not unlimited. There’s some point in time, when they’ve exceeded their limits and dollars, and we will have to put some deductible. There would ask for some kind of deductible in order for a new, what did they say, for a new-
Eric: Almost like it resets.
Recommended:
Kaye: Reset, yeah. I never heard of anything like that.
Patrik: No, I never heard any of that. Basically, what you are suggesting is that if any patient is using up a certain amount of funds? That they are asking for a return, is that what you’re asking?
Kaye: Like a deductible.
Patrik: Yeah, no, no.
Kaye: Like X amount of dollars.
Eric: You can pay, for example, two thousand dollars and then the limits reset. They made it sound kind of-
Patrik: Oh, that would be new to me, but it wouldn’t surprise me.
Eric: Yeah.
Kaye: Okay.
Patrik: It wouldn’t surprise me if they have clauses like that. It wouldn’t surprise me.
Eric: Okay.
Patrik: I’m not aware of it.
Eric: One thing we can do to move the hand to get him into LTACH if they’re still going to be pretty adamant about it, is you’re saying we’re not going to sign the discharge papers.
Patrik: That’s correct.
Eric: We could also, from what I’ve read, is that possibly, and maybe you know or have some knowledge on this, that we can actually start an appeal process.
Patrik: Oh definitely. Oh absolutely. If you feel like tomorrow you’re having a meeting and this is not going anywhere, you definitely either have to start an appeal process, and the other thing that I would highly, highly recommend if you are going into this meeting tomorrow and you feel like this is not going in the direction that we want, you need to leave. You need to make very clear that you are not agreeing with what is happening.
I always suggest to work with people if you can, right? If you think you can’t, and if you think this is not going in a direction that we agree with at all, I would make that very clear to them.
Recommended:
Kaye: And I did, and I was and I told her already. I said, “I’m very unhappy, and I disagree with this.” She right away she told me, “Well, then you need to talk to the nurse practitioner or to your doctor.” She transferred me to the nurse practitioner, the nurse practitioner said to me, “You know, we have to meet some criteria.”
Patrik: Yeah.
Eric: I think you’re going to have better luck with Dr. Daniel tomorrow, the-
Kaye: After talking to him a few times for 15 minutes, eventually the nurse practitioner said, “Well I think the best way for you to approach them will be with the doctor.” I said, “Doctor who?” She said the cardiologist. I said, “Do me a favour, and set me up for tomorrow. I want to see him tomorrow.”
Patrik: Can I ask, he’s got a case manager, and this case manager is a hospital employee, is it an insurance employee? Is that a nurse?
Kaye: Yeah. Hospital, hospital, yeah. It’s a hospital employee.
Eric: Are you sure about that?
Kaye: Yeah.
Patrik: Is it a nurse?
Kaye: I don’t have, oh my God, I don’t have a business card with me.
Patrik: That’s all right.
Kaye: Let me tell you.
Eric: You’re asking me if the case manager is-
Recommended:
Kaye: I don’t think so. I don’t think so. I don’t think so.
Patrik: Is it a social worker?
Kaye: I don’t … Hold on. Dr. Daniel is here by the way. Okay, is she a social worker? Is she a social worker or not? Does she have a medical degree, like nurse or an employee of the hospital?
Patrik: So, she’s not a social worker?
Kaye: No, she just works here. Yeah. I thought maybe she was a social worker or something, you know? Oh, his nurse. I thought maybe she was a social worker or something. Okay, okay.
Patrik: Are you dealing with the social worker as well?
Kaye: No, I never met with them.
Patrik: Okay. The other thing that I can suggest, if you want me to be in the meeting tomorrow with you on the phone, I can certainly do that if you feel that’s of benefit.
Kaye: Okay.
Patrik: I can certainly do that, and I’ll send you some options about that if you feel like you want me to be there. I do believe overall, from a clinical perspective, I do believe your husband could be a lot worse. Obviously, there is a lot of room for improvement, don’t get me wrong, but he has taken a big step already. He’s off the ventilator. That is good, good news.
Kaye: Yeah.
Recommended:
Eric: Yes, yes, we agree. We agree.
Patrik: I know, even though he is, “only” in the chair for two hours a day again, that’s good. They’re doing more than most other ICUs already. They’re supposed to be doing that, but it’s good that it’s happening. I’m very glad that this is happening.
Kaye: Okay, yeah.
Patrik: They’re doing all the right things in that aspect.
Kaye: Yeah.
Eric: Good, good, good.
Kaye: Okay, I want to chat with the doctor. He’s here and might come in.
Eric: I understand. Patrik, she wants to run because the cardiologist is there right now.
Patrik: Yeah, sure.
Eric: She might be able to find out some information right now. Sweetheart, if you want to hang up, I’ll talk to Patrik for just a few minutes, okay?
I’m just going to hang up on her. Give me one second.
Kaye: Patrik, Patrik.
Eric: You can go. Patrik and I are going to talk a little more.
Kaye: Patrik, thank you very much. I’m sorry. I want to talk over here.
Recommended:
Patrik: You’re very welcome. Thank you. Thank you.
Eric: Hopefully, she hangs up because I don’t know how to get off this conference call.
Patrik: Right, right, right.
Eric: Okay. She’s done. By the way, we’ve been talking longer than 15 minutes.
Patrik: It’s okay. It’s okay. It’s fine. It’s fine.
Eric: Just so you know. I don’t know if you caught it. I actually paid for another half-hour too.
Patrik: Yeah, that’s right. I found that. If you want me to call into the meeting tomorrow, I can do that within that half hour if you want to.
Eric: Okay. I just have a feeling she is going to be talking to Daniel right know. That’s really the meeting. She doesn’t even need to make a meeting with the guy. She sees him every morning and sometimes in the evening. She might be getting things straightened out right now.
Patrik: Okay.
Eric: Who knows?
Patrik: Okay.
Eric: I’ll find out. Yeah. We’re fully prepared to play hardball with them. We just need to know how the game is played.
Patrik: That’s right, that’s right. You need to be prepared to play hardball with them. Like I said, I’m always recommending to work with people if you can of course, but if you can’t then you have to look for strategies of course.
Eric: What happens when we refuse to sign the discharge papers?
Patrik: Just wait, just wait.
Eric: They’re going to have to pretty much either do what we want or do they have another option?
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: I don’t think they have another option. You see one strategy that I find works is either stop communicating for a while with them or just send one message over and over again. That usually works at least to buy you time, right?
Eric: Right, right.
Patrik: Again, I’m always for working with people, but you also need to be prepared for being a bit stubborn if that’s what it takes.
Eric: Oh, she can be stubborn, don’t worry about that.
Patrik: No, no. It’s good because that’s what sometimes it takes to be stubborn.
Eric: Sure, sure.
Patrik: This is what I always-
Eric: You’re dealing with a Russian and German here. Come on, we’re the most stubborn in the world I think.
Patrik: That’s right. That’s right. Time to get more stubborn. Your surname is German?
Eric: Yes. I was born here in the states, but I have relatives in Germany.
Recommended:
Patrik: I was born in Germany.
Eric: Oh really.
Patrik: Yeah, yeah. I was born in Germany.
Eric: Oh wow, north or south?
Patrik: Sorry?
Eric: North or south Germany.
Patrik: South, southwest, southwest.
Eric: Oh, okay. We’re from near the Stuttgart area.
Patrik: I’m probably an hour and a half northwest of Stuttgart.
Eric: Oh, okay, okay, yeah.
Patrik: Small world.
Eric: Very interesting. Yeah, sure is.
Patrik: Very small world.
Eric: Yep, in fact it’s funny, my sister and her daughter, my niece, are actually flying to Germany tomorrow.
Patrik: Right.
Recommended:
Eric: We don’t go very often, in fact the last time my sister and I went was in 2002 right after 9-11. The funny thing is that my niece is actually a certified, ICU nurse.
Patrik: Right.
Eric: So, we’ve had a lot of conversations with her. I read a lot on your website. She is new into it. You have a lot more years on her than she does. She has a lot of the technical and background stuff, but right away she said it’s probably the insurance. It sounds like an insurance thing.
Patrik: I think so too.
Eric: Yeah, yeah. We are going to just have to fight that.
Patrik: Yeah. As I said to you, Eric, what I can do tomorrow is … What time is the meeting? Do you know?
Eric: I don’t think there is any set time in the meeting. She was just planning on going there at 7 o’clock in the morning because that’s usually what time the cardiologist is there, and they usually always see each in the morning and then they talk. It wasn’t a planned scheduled meeting that she had. I told her, just tell the case manager … because at the time, I was thinking we need to get all the doctors in there or one of the doctors either the cardiologist, the pulmonologist or whichever doctor has made the decision that he doesn’t have to go to LTACH. You know?
We wanted to have a debate with them to see exactly why you are saying that he doesn’t need to go to LTACH because we don’t agree.
Patrik: That’s right. Exactly right.
Eric: That family meeting so far as a scheduled meeting, or even the head of ICU, what do you call him, the-
Patrik: The medical director?
Eric: Yeah, exactly. Even if we need to get him involved, we would do that too. We’re going to fight this.
Patrik: Keep in mind with the ICU, there is one more thing that I think is important to be mentioned. Let’s say, LTACH, for whatever reason doesn’t have a bed, or let’s just say they don’t have the resources to take your dad in now. Let’s just leave it there. Let’s just say the LTACH doesn’t have the resources to take your brother in, ICU needs the bed. There’s no doubt about that. ICU needs the bed.
From an ICU perspective, they want to empty the bed. There is no LTACH bed, but there is a skilled nursing facility bed. Therefore, ICU might say, yeah, we’ll send him to skilled nursing because we need the bed. So you’ve got to look at this from all angles.
Eric: Right. Okay, well she actually talked to the lady from LTACH today.
Patrik: Mm-hmm (affirmative).
Eric: It was on a different matter. This is when we thought we were going there. She’s trying to get that mattress that our cardiac doctor designed. She’s trying to get that mattress over to the LTACH. That’s what she was working on today.
Patrik: Okay. Yep.
Recommended:
Eric: I will have her talk to LTACH tomorrow. The case manager at the hospital didn’t say anything that didn’t have any available beds, she was saying that it was the insurance.
Patrik: Yeah.
Eric: I think it is the insurance, but we’re just going to ask the right questions and see if that is maybe the real issue.
Patrik: Yeah, okay, okay. All right.
Eric: Okay.
Patrik: I hope that helped. Let me know when you need help.
Eric: It did. I will, I will.
Patrik: And we will take it from there.
Eric: Okay, thank you very much Patrik. You’ve been a great help.
Patrik: You’re very welcome.
Eric: Love your website by the way.
Patrik: Thank you, thank you for those kind words. Thank you very much
Thank you very much.
Recommended:
Eric: Thank you, sir.
Patrik: Have a good day.
Eric: Okay, bye-bye.
Patrik: Okay, bye-bye.
Eric: You too.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!