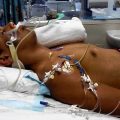
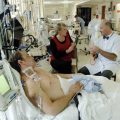
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ronnie, as part of my 1:1 consulting and advocacy service! Ronnie’s mom can’t be weaned off the ventilator & wants to get the treatment at home. Ronnie is asking if his mom will get a good quality of life with the 24/7 ICU nurses at home.
Will Mom Get the Best Quality of Life by Having 24/7 ICU Nurses at Home?
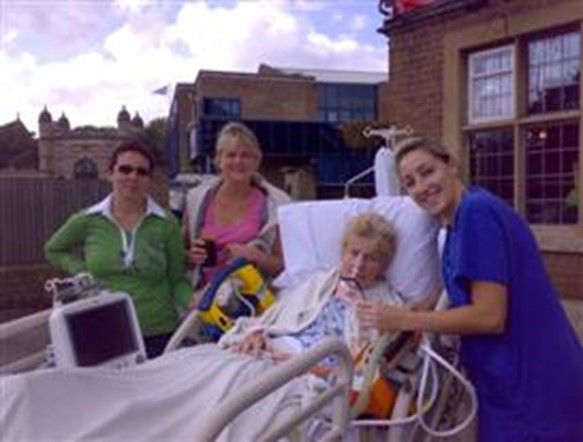
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ronnie here.”
Patrik: Want to keep the peace?
Ronnie: Yeah. Collectively, the siblings are doing everything behind the scenes, but we’re trying to vent, we’re keeping things very, very calm and very just so that we can be by mom.
Patrik: Positive.
Ronnie: Yeah. Be positive for mom and be by mom, because at the end of the day, if she presents herself the way she has, there’s not really much that they can do. So, that’s what we’re holding onto, that hope that having the family around stimulates and motivates her, keeps her positive.
Patrik: Right. And she’s positive still?
Ronnie: Yeah, she is.
Patrik: That’s amazing.
Ronnie: She is, with just even-
Patrik: No, no. Yeah, I hear you. And that’s good information. You want to keep her positive. I hear you. I hear you.
Ronnie: Patrik, can I come back to that medication you were saying?
Patrik: Please, please, please. Yeah.
Ronnie: You know you’ve sent the name. So, did you say it was fine?
Patrik: Yeah. No, it’s fine. It’s fine to use. I have seen it being used every now and then, but not all too often. It’s generally speaking used for other things. Hang on, I’ll just quickly need to go back.
Ronnie: There you’ll find mom’s CO2 (carbon dioxide) from that measurement of her forehead, that it was about in the sevens, the CO2 output.
Patrik: Right. Well, the question is, when she had this on the forehead, did they also measure it on the ventilator, do you know?
Ronnie: Yeah, on the ventilator it was presenting itself 5.6, 5.7. So, they know that on the ventilator, it presents itself differently… Sorry. On the monitor, to the one that had is on the forehead.
Patrik: I wonder why they’re doing it. It doesn’t make sense to me why they would. Did you ask them why they do this?
Ronnie: Yeah. They said it’s like the one that they use to measure oxygen saturation. You know they put the one on the foot?
Patrik: Yeah, yeah.
RECOMMENDED:
Ronnie: And then they said that it’s like that. But because we don’t have an… I asked last night and the nurse said it’s because she hasn’t got the arterial line. So, because of that, they need to measure and watch the trend. When she’s sleeping, is her CO2 rising? Is she retaining more CO2? Yesterday, they mentioned randomly that her kidneys are retaining bicarbonate. I don’t know, I just don’t know where they are. I feel like they’ve given up on her. They have given up and it’s to appease the family, I think more now.
Patrik: Okay. But this is exactly what they’ve done with the other lady. They’ve given up on her dad way back when, and she never gave up. But I also understand that keeping the peace with them is important. I get it. But there may come a point, if they are going to be really hard on your mom and say, “Look, she can’t be weaned off the ventilator, she’s not going to have a lung transplant. We want to move towards palliative care.” That’s probably when keeping the peace may no longer be the right approach, but this is something you need to gauge when it comes to that point.
Ronnie: No, we’ll say, “Then you send her home.” I don’t know if this is the right way. We’ll send her home on a ventilator. Remove the TEP (Treatment Escalation Plan) and DNR (Do Not Resuscitate), so if she gets sick, she gets hospital admission again.
Patrik: Correct. We have clients at home with a ventilator. They’re not on DNR, unless they want to. There are a few clients they want to, but most of our clients are not on DNR. They want to live.
Ronnie: Yeah.
Suggested Links:
Patrik: It sounds like your mom has a lot to live for. She’s got a beautiful family, she’s got a lot to live for.
Ronnie: She knows what her life’s going to be like and she says she just wants to go home. And I keep saying to her, ” Mom, don’t rush yourself home. You still need the treatments,” et cetera. So, they can’t send her home on end-of-life terms. It’s going to be sent her home where if she needs hospital treatment, she gets the hospital treatment. If she needs the treatment at home, she gets the treatment at home. So yeah, you can send her home on a ventilator because you’re not going to do the transplant or whatever it is, but if she needs that extra treatment, she gets it.
Patrik: Absolutely. I will tell you what I’ll do. So, we’ve just hired someone here in the City. We’ve hired an ICU (Intensive Care Unit) nurse. She used to work in a foreign country for 10, 15 years. She also worked in the community, similar to what we do here. And she looked after some ventilated patients at home in some nearby towns and districts. But I know she was mainly in the city and I will find out how those patients were funded. I know that lady got funding through the health service, but I will find out, Maria is her name, is that she only started with us in the last few weeks. She’s been in the city now for a couple of years and she worked in one of the local ICUs here, but she has done similar work in some other countries like what we are doing here. So, there must be other avenues, besides what that lady is sort of prescribing in the interview, and I’ll find out from her.
Ronnie: Thank you, Patrik. I’ll be in contact. Yeah, I will definitely be in contact next week even because they’ve already envisioned that mom’s not going to cope. So, they did say, when they start seeing she’s stressed, they will just stop. So, they made that clear in the meeting. The moment they say she’s stressed out and it’s too much for her , they will stop.
So, we’re just hopeful, and I’ve told mom about this, I said, “Mom, this is their plan. It’s 10-minute bursts.” I don’t know if it’s helpful if we encourage her to do a lot more deep breaths in that 10 minutes. I don’t know, Patrik, you know better. If I said to her, take a bit more deep breaths or don’t breathe so fast, or how can I motivate her to cope with that 10 minutes?
Patrik: Yeah, yeah. Look, there can be a huge psychological component when someone is being weaned off the ventilator in terms of their psychological dependency on the ventilator. That can be a huge part, especially after such a long time on the ventilator. So yes, absolutely. Talking to her, having family there. I would argue the ICU should have a physiotherapist there when they try to do the weaning. Absolutely.
So, an experienced physiotherapist should exactly do what you’ve just said. You can do it yourself, “Calm down, take slow, deep breaths.” All of that is part of it. Do you think your mom is scared about that?
Ronnie: So, when the slope changed, she definitely wants to come off the ventilator. That’s a fact. She wants to talk, she wants her voice back, she wants to eat and drink, but she knows her lungs can’t sort of cope on their own. And it’s like things like when the slope was changed to 0.30, she felt it instantly. She’s just like, “No, you don’t understand. There’s a blockage there.” When things get blocked or whatever it is, she knows, she can feel the difference. Even though the monitors are showing everything stable, she’s like, “I’m not feeling that it’s stable.” She goes,” It feels different for me.” But yeah, I don’t think she wants to depend on the ventilator, no.
Patrik: Of course not. Is there anyone working with her, whether it’s a doctor, whether it’s a nurse, whether it’s a physiotherapist that you think could be a champion for your mom? In terms of, is there someone within that team that is not scared to speak up, is saying, “Hey look, we’re all wrong here. We need to advocate for this woman.” Is there someone?
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Ronnie: Amongst the nurses, yeah, but they’ve all got a job.
Patrik: They’ve all got a job, but they’re also independent practitioners. They’re registered with the nursing board. And it depends on the level of seniority, it depends on a number of things, whether they’re able to speak up or not. What she needs is a champion within a team, that’s what she needs.
From my experience, it’s often not the team that, especially when the outlook is sort of negative. Your mom needs a champion who says, “Yep, we can do this, and we can do better than this and we need to give this woman a voice and we need to work with her, not against her.” That’s what she needs within the team.
And that could be a doctor, that could be an experienced nurse, it could be a physiotherapist. Yes, they do have a job but one thing that I did when I was still working in ICU, I always and I was very outspoken, which eventually I couldn’t do it anymore because this is why I branched out with doing what I’m doing now. But the way I always position myself as is, well, I’m not reporting to the doctor or to the head nurse. I’m reporting to the registration board.
And as part of your registration with the nursing and midwifery board, there’s a code of conduct, a code of ethics. How that you know that you actually need to advocate for a patient? That is always how I positioned myself to the hospitals whenever I was in conflict saying, “Well, yes, I’ve got a contract here, but first and foremost, I’m reporting to the nursing board, not to my employer.” But (A), it takes gut, and (B), it takes experience. But that’s what I think she needs. But you don’t think there’s anyone at the moment who-
Ronnie: There are loads of people who advocate for her, who really want her to do well. She’s got such a relationship with the nurses. 120 of them, a lot of them adore her, and really, as they’re going past, they motivate her and come over and say hello and things like that. But I think next week, the family will have to be more present as well. We are really worried.
Patrik: Yeah. No, likewise. Knowing what I know about your mom, I’m very concerned there, too.
Ronnie: Patrik, one last question. You know ventilation. So, say she came home on the ventilator, I think she’ll need it 24/7. Right? It won’t be a case of-
Patrik: No, she will need 24/7. So, I don’t think that her condition, it doesn’t sound like her condition will change much in the next few weeks. And imagine, all of a sudden, she wouldn’t have 24/7 with what she’s got at the moment, the risk of something going wrong, especially with now you’re telling me she needs suction every couple hours, they’re fiddling around with the subglottic port. You need to know what you’re doing. She’s got inner cannulas that need to be changed regularly. With diabetes, is she on insulin?
Ronnie: She is on insulin, yeah.
Suggested Links:
Patrik: Right. She’s got a PEG (Percutaneous Endoscopic Gastrostomy) tube or a nasogastric tube?
Ronnie: She’s got an NJ (Nasojejunal) tube.
Patrik: Oh, a jejunostomy?
Ronnie: Yeah.
Patrik: Right. Okay. And with the insulin, she’s getting long-acting insulin?
Ronnie: Yes, she is. One in the morning and one in the afternoon.
Patrik: And they give her boluses here and there?
Ronnie: Yeah.
Patrik: Right. I would think that going home without 24-hour ICU nursing would be futile. And I don’t want to be negative here. I’ll give you some examples, just to illustrate that. We’ve had some clients here at home where we were only funded for the night shift and the funding body said, “Well, during the day this person doesn’t need a nurse, or they need a support worker, or the family can do it.” We were ringing the alarm bell saying, “Well, as soon as we leave here, that patient’s life is hanging by a thread.” And we were right, those patients passed away during the day because families or support workers simply couldn’t manage medical emergencies. It’s a bleak outlook. But you should hold on to the lady’s story and I will ask our staff member here. So, there’s an agency in the city and in the town called JMP. You actually should now reach out to JMP, irrespective.
Ronnie: Okay.
Patrik: Reach out to JMP. I know that some of the things that we are doing here, they’re not at specialized as we are, but this is who our staff member worked for. JMP must have an idea of how those patients get funded. There’s a nursing agency in there and they are doing a little bit of what JMP is doing as well, from what I understand. Reach out to them as well and describe the case to you and let them tell you what they know about how to go about funding and all of that.
Ronnie: Okay.
Patrik: I really don’t want to discourage you, you should keep fighting for your mom, but I do believe that the pulmonary fibrosis will be in the way of weaning her.
Ronnie: I think so.
Patrik: But that shouldn’t stop her from going home. Absolutely not. We have clients at home that have 24-hour nursing care with ICU nurses that can’t be weaned off the ventilator, not because of pulmonary fibrosis, but because of many other things. They live a very good quality of life. They might be a little bit younger, we take them to school, we take them to university, we take them wherever they want to go. A lot is possible at home. You got to think about, at the moment, she’s stuck in this ICU bed. Once she’s at home with the right support, her quality of life will improve.
Ronnie: She can move around, as in move around the house or go around?
Patrik: Absolutely. At the moment, I would imagine she’s not seeing any daylight.
Ronnie: Yeah.
Patrik: It’s terrible. So, I also think that you and your family might just be at the stage where, again, I do believe the pulmonary fibrosis will be in the way of weaning her off. You’ve probably got to come to terms with that and then see what’s possible. That’s a hard pill to swallow, but I think it’s the better pill to swallow compared to them running rampant and really trying to kill her.
Ronnie: Yeah. I think that’s it. It’s the acceptance that she’ll remain on the ventilator and mom to accept that, but then again, quality of life and getting the best quality of life for her.
Patrik: Yeah. And I believe, like most of our clients here too, they will naturally improve just by being at home. That doesn’t mean she can come off the ventilator, but you know what an ICU looks like, it’s terrible. Being in their own home, you can’t beat home.
Ronnie: Yeah. Thank you so much, Patrik. That was really helpful.
Patrik: I’m sorry that I don’t have any better news but work with what’s possible.
Ronnie: Yeah. I will contact you during the week, I think if we need.
Suggested Links:
Patrik: Yeah. Look, we can do another half an hour. You’ve already purchased two hours. I’m very happy to give you another half an hour. There’s no issue there because I really want to help you with this as much as I can because no one should be… It’s frustrated me so greatly when I work in ICU where people are not given a chance.
Ronnie: Yeah.
Patrik: Your mom is still young.
Ronnie: She is. Her birthday is on Tuesday and she just wants to come home.
Patrik: Can’t blame her. And maybe, as I said, I don’t know the dynamics there. See whether, for lack of a better term, you can find a champion. It only takes one.
Ronnie: One consultant did actually say, the consultant who made a few amendments to the DNAR (Do Not Attempt Resuscitation) and the TEP (Treatment Escalation Plan), because I actually said, “Look, I’m really nervous about leaving my mom here,” that there are people that could do it, if something goes wrong, people just stand and watch and let her go, when they could intervene and save her life. That’s really harsh for the family to accept after five months of being in the ICU and seeing mom’s progress and her fight, et cetera. And she said she understood, so she did make a few of the changes. But yeah.
RECOMMENDED:
Patrik: I tell you what the nurses should be doing, and this is something that I’ve always done in ICU when I worked in ICU, tell you what the nurses should be doing, and it’s got nothing to do medical. The fact that they’re not involving your mom in her care, that to me is appalling. That to me is absolutely appalling. The nurse, a senior nurse, should go to the doctors and should say, “Hang on a second. You are not involving your mom in her own care. You’re not talking to her what the plan is, and you’re disrespecting her right to life.” That is something that needs to come from the nurses, I believe. But I think an experienced nurse should be able to do that because a good senior nurse is not afraid to speak up like that. There’s nothing wrong with that. No one will perform and manage a nurse over a comment like that. No one or maybe you can, I don’t know who you can talk to there. See whether they’re senior nurses that might take an interest in your mom’s case.
Ronnie: Yeah.
Patrik: Because talking to her has nothing to do with treatment, that’s got something to do with respect.
Ronnie: Yeah. Exactly. And they do, they’ll prepare her. They’ll say, “We’re going to come and chat to you,” on whatever day it is, and then they don’t, or the translator’s canceled, or whatever it is. And they don’t actually have the discussion with her. Instead, it’s through me or my sister or whatever it is. All right, Patrik.
Patrik: Okay. Reach out to me and we’ll see what we’ll do next.
Ronnie: Okay.
Patrik: Okay.
Ronnie: Thank you so much.
Patrik: It’s a pleasure. All the best.
Ronnie: Thank you.
Patrik:Thank you.
Ronnie: Take care.
Patrik: Thank you. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!