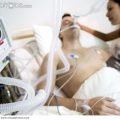
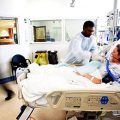
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Can Mom Be Successfully Weaned Off the Ventilator in ICU with Lung Fibrosis and a Tracheostomy?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Ronnie, as part of my 1:1 consulting and advocacy service! Ronnie’s mom in ICU is conscious and coherent. She is consistently saying that she wants to continue her treatment, but the doctors are moving towards end-of-life for her.
My Mom in ICU Wants to Continue Her Treatment But the Doctors are Leaning Towards End-of-Life for Her. Help!
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ronnie here.”
Ronnie: Yeah, they just leave it there and she is saying, “No, it’s affecting… They’re doing something that I’m not content with.” She’s complained of an earache as a result. She’s saying that she’s had this constant headache since, so she doesn’t want that. She refused it last night. Then, we’re just thanking God that she’s neurologically sound, where she can say yes or no to certain things.
The other thing they spoke about with me yesterday, the consultant did, and this meeting was with the lead consultant. He spoke about a CO2 medication, something to help reduce her CO2 levels. Now, something in my gut is telling me I’ve got questions about it because I immediately said that mom did not get the best kidneys since her hospital stay, so I wanted your advice on that. Is there a medication that they give to sort of normalize CO2?
Patrik: Not heard of it. Not heard of it. Look, there could be new developments that I’m unaware of, but I’ve not heard of it. Let’s just say her CO2 was high. They would bring the pressure support up or they would bring up the PEEP (Positive End Expiratory Pressure).
Ronnie: Yeah.
Patrik: That would be the standard course of action for someone that is ventilated. Let me ask you this, is she still on any opiates like morphine, fentanyl, do you know?
Ronnie: No, no, no, no. Not at all.
Patrik: Good. Because that could be the first thing that increases her CO2 (carbon dioxide). Hang on. So yes, if there is a medication, it would be a nebulizer, but they should have introduced that way back when.
Ronnie: Yeah, way back. Yeah. She gets her nebulizer.
Patrik: Right. Let me check, “High CO2, any medication”, the only thing that comes up is Salbutamol or Ventolin. But that’s been around for decades. But maybe there is a new trial drug, I don’t know.
RECOMMENDED:
Ronnie: But I don’t want them to start introducing all these drugs and then it affects my mom. Because she’s neurologically sound and she’s stable at the moment. Then they will say, “Oh, her kidneys weren’t right.” Or her heart wasn’t… it’ll destabilize her, which I don’t want them to do. If they’ve got current data that. I don’t know. I don’t know what they’re thinking. So, I wasn’t too sure about that. I need to check that with you.
Patrik: There’s one drug, yes, that I have come across. That’s Acetazolamide. I can text that to you. Yes, that would’ve been given every now and then for high CO2. I’ll text that to you, but it’s not common. It’s been around.
Ronnie: Do you know if that will affect or destabilize her kidneys or?
Patrik: Not really. Not really. Not that I can think of. But this is something we can definitely find out. With the kidneys, is she on dialysis still?
Ronnie: No, she’s not. And the TEP says that she will never receive dialysis. So, if she does sort of go into failure, she’ll never… Because they’ve still got the TEP, they won’t remove the TEP. They won’t remove the DNAR (do not attempt resuscitation). They just did it to, if anything to… Because I’m continuously speaking with the consultants with that to be removed and to keep mom under constant review. Because that’s what the Health Service website says. That they will keep her under review and decide on the TEP and DNAR. So, they said if anything is reversible, that’s written up in the notes, then they will treat.
Patrik: What do you mean by TEP? What do you mean by that?
Ronnie: TEP is the Treatment Escalation Plan.
Patrik: Does she have a treatment escalation plan?
Ronnie: Apparently, she’s got that at the moment, where they will not, if for example her kidneys needed dialysis, they won’t give her dialysis. If she needed really high doses of medication for her low blood pressures or high blood pressures or whatever to stabilize that, they won’t give it anything that’s not going to reverse her situation because they say she’s currently in a stage of irreversible conditions.
Patrik: I see.
Ronnie: They won’t just use modern medication to keep her artificially alive. That’s the words they use.
Patrik: Right. Have you seen this document?
Ronnie: I’ve not seen it, no. And I’ve asked for a breakdown of everything that what are they going to treat and what are they not going to treat? But I haven’t received that as yet. What we’re currently having are these weekly conversations about mom’s progress or what they’re planning for the following week. Then in those conversations, I raised the DNAR. Even with the DNAR, I said, if mom, for example, has sputum and then she goes into some sort of arrest, her heart stops as a result, and because she is on this tracheostomy, then will somebody just stand and watch her die and allow her to go like that? And then they changed it. I said, “Because if you’re writing things up, the nurses and the doctors will just go on with what’s written. So, they have to actually just treat things which are reversible.” And that’s what they agreed. Not that they removed anything.
Patrik: Okay. And I do remember last time, they weren’t involving your mom in those discussions. Is that still the case?
Ronnie: So, they’re currently using the speech therapist to talk to her about certain things, but it’s not a formal discussion. They haven’t had any sort of formal discussion or got her views. When she talks to them, she does say, “I want my treatment to continue.” She’ll continuously say this, “I just want my treatment to continue.” So, she says, “Yep, I know what you want.” And there’s witnesses there. “I know what you want.” I don’t know if she takes these back to these meetings that they have weekly.
Patrik: So, no one has the guts from the medical team to talk to her, really?
Ronnie: No.
Patrik: That’s so coward-ish. That’s just appalling, really.
Ted: Yeah, and I think that’s it.
Patrik: The doctors can’t talk to their patients, seriously? It’s just appalling.
Recommended:
- Is it Normal to be Ventilated in ICU After a Heart Attack? Quick Tip for Families in Intensive Care!
Ronnie: Yeah, they haven’t actually sat and spoken to her. Even yesterday, the lead consultant said, “I don’t think she actually knows the true extent of her situation. Would she want to go home on a ventilator?” and things. I said, “She does, she has ideas about what’s happening, and she has a clue, she’s neurologically sound. She knows exactly what’s happening and what’s not.” But they still haven’t had that discussion with her.
And she can sense it. So even yesterday, she’s been prepared for tracheostomy change and then it’s not happening. So, it’s picking and choosing whose priority in the ICU and who’s not. They said that they’ve had more sick patients or whatever it was, but you’re seeing there’s doctors who can do so and didn’t. That’s what’s frustrating, are they waiting for her to have this huge setback and then just say, “Yeah, we are done.”
Patrik: And I think the longer she stays there, I do believe the higher chances she might have a setback.
Ted: Yeah.
Patrik: Would you say your mom is depressed?
Ronnie: She’s strong. She’s not depressed.
Patrik: That’s amazing.
Ronnie: Yeah. Thank God. She does have these down days and that’s usually related to how her breathing is. If she feels like she’s just, “I really can’t do it, the breathing is really unsettling me,” et cetera. Because she got the family around and things like that, it really keeps her motivated.
Patrik: That’s fantastic. That’s fantastic. Do you have access to the medical records now?
Ronnie: No, we haven’t even got access to the medical records.
Patrik: And you’ve requested that?
Ronnie: We’re in the process of requesting it. Once again, it’s about trying to… We’ve got so many thoughts going on in our minds, it’s trying to keep a good relationship with the hospital so that we’re not making it difficult for mom. We’re trying to keep mom at the priority and make sure that we’re around for her.
Patrik: Yes.
Ronnie: At the same time, that she gets all the care that she needs and the treatment that she needs. So, it’s finding that balance. Sorry, Patrik, I just forgot to mention this to you. They also said they’re going to try another weaning plan this coming week. So, what they’ll do, so she’s on pressure 15, in 10-minute bursts, three times in the day, they’re going to lower the pressure to 10. So, from 15 to 10 for 10 minutes.
Patrik: Yep.
Ronnie: And then overnight, give her higher pressures. They say that they think that she’ll have problems with this and that she won’t cope, and it’ll start affecting other organs or other things. They say that the family will also find this difficult. But to be honest with you, I don’t know what the plan is and what are the effects of this.
Patrik: Yeah, yeah, I hear you. It’s almost like they want to set her up to fail.
Ronnie: Yeah.
Patrik: Okay.
Ronnie: So, can you tell me, if she stayed on, for example, 26 for the oxygen, the PEEP (positive end expiratory pressure) is 5, she moves from 15 to 10 and the slope is 30. What could happen for 10-minute bursts?
Patrik: I tell you what I predict. I predict her volumes to go down. So, when you look at the last picture that you sent me, I’ll just explain that to you. Just give me a second. I will tell you what I predict. Her volumes will go down. The last picture, her breathing rate per minute is 18 breaths per minute. So, when you look at this, 18 times 290, gives the minute volume of 10.4 roughly. So, can you see the last picture on the top left, you see RR 18?
Ronnie: Mm-hmm.
Patrik: That’s the respiratory rate breathing rate per minute. Then you see the 290 VTE (End-Tidal Volume). Can you see that?
Ronnie: Yeah.
Patrik: So, 18 breaths per minute times 290 mls per breath is roughly 10.4, probably. That’s the minute volume on the left lower side, can you see that?
Ronnie: Yeah.
Patrik: So that’s roughly the volume per minute. So, the breathing rate multiplied by the volume, roughly. So, I expect, if they drop the pressure support to 10, that the volume per breath will go down. And in order to compensate for that, the breathing rate will go up. So, in order for her to achieve the 10.4, her breathing rate needs to go up. Let’s just say for simplicity, her volumes dropped to 100 mls, then she would need to compensate with a breathing rate of 30 to make up the minute volume, and that would exhaust her.
Suggested links:
- What are My Mom’s Chances of Survival After Double Heart Attack, Failed Extubation & Kidney Failure?
Ronnie: Will it affect her heart?
Patrik: Maybe not in the short-term, but possibly in the long run because her heart needs to work harder.
Ronnie: And will it up her CO2 (carbon dioxide)?
Patrik: No, it’ll probably lower it.
Ronnie: Okay.
Patrik: Probably lower it.
Ronnie: That’s where my worry is that are they trying to up her CO2? And then she got poisonous gas in her body. So, my brain works in, it’s in overcharge or something here.
Patrik: Look, it might lower her CO2, but then again it really comes back to how she compensates for it. It might actually, but it might not.
Patrik: So yes, so I predict her volumes goes down and her breathing rate goes up. Her CO2 might go up or it might go down. It really depends on how she compensates. If her volumes go down and her breathing rate stays the same, her CO2 will probably go up. If the volume goes down and her breathing rate increases, her CO2 might actually go down. So, it really depends. But I can see that they potentially want to set her up to fail and then make their determinations from there. Now, you mentioned something in the beginning, about a center.
Ronnie: It’s a respiratory center for long-term patients and weaning.
Patrik: Okay. And weaning. Okay, great. No, I tell you why I’m asking. So, I am wondering, let’s just say your mom can’t cope with what they’re predicting. That would probably show that she’s not a candidate for weaning, which I believe will then make a very strong case for her to go home with what she’s got.
So, if you were here in Melbourne and your mom was in a position like she is now and you would come to us, we would probably say to you, “Yep, we can take her home. Here, we know how to go about the funding and all of that. It’s all there. Especially, for someone under the age of 65, but that’s neither here nor there.” And then we would liaise with the ICU and here it’s almost like an accepted model. Your problem in the U.K. is that it’s not an accepted model yet. I do believe that with pulmonary fibrosis, she’ll have a hard time getting off the ventilator. Because what the pulmonary fibrosis means, it’s scar tissue in the lungs, and like we know, scar tissue doesn’t heal.
Ronnie: Do you think there is a chance for her to be weaned, based on her numbers?
Patrik: I really don’t know. Do you know if they tried the 10 before?
Ronnie: Before she aspirated, she was off the ventilator. Yeah. So, she was extubated, she was decannulated, et cetera. So, she was off the ventilator, and she had some level of fibrosis and the aspiration has just made it worse. And obviously now, it’s just… But they’re trialing all of this. So, I don’t know if they’re trialing it. I do feel like it’s a tick box, but I also don’t know if she wasn’t at that stage where they could trial it, they’d just say, “We’re not going to even bother trialing it.”
Patrik: Why do you think they haven’t tried this four weeks ago?
Ronnie: I think she got to pressure 12. I think in our last conversation, she got to pressure 12. So, they did-
Patrik: Oh, I’ll have a quick look. Have a quick look through the pictures there.
Ted: I think she did get to… Yeah.
Patrik: 14, one picture is 14.
Ronnie: Yeah. I think by then, by the time we spoke, they had palliated mom. So, the week after we spoke, they said, “We’re going to try a week of weaning her,” and they brought her down to pressure 12. And then what happened is, her CO2 just rose, so they stopped, and they said, “Right, we can’t wean her anymore.” And then they put her back up to pressure 17.
Patrik: Right. Right. Okay. Just give me a second. I just need to quickly look through your pictures that were sent last time. So, one is 14 and the other one 14. I don’t see it any lower than 14.
Ted: Yeah, I think by then, by the time we spoke, she was on pressure 14. I think a few days later, they brought her down to 12.
Patrik: Okay. All right.
Ronnie: But then again, her CO2 rose and they just…
RECOMMENDED:
Patrik: Sure. This is what I’m predicting, and there could be two outcomes, they might set her up to fail and then they might say, “Well, we’re going to pull out.” Or they might say, “Well, now we know we can’t send her out because if she can’t be weaned, what’s the point of sending her to the respiratory center?” Unless they have something that they’re doing there differently, but I do believe pulmonary fibrosis will be in her way.
Ronnie: Yeah, but what they’ve said is they will trial this week, the aggressive weaning, and then they predict that she won’t cope, they predict the family will be unsettled. They predict other things going wrong, so they’ve given that heads up. And they said, “That in that situation then we have to consider moving her end-of-life,” so that’s either to send her home on a ventilator and this is her life. Will she accept that quality of life?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!