Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Ronnie, as part of my 1:1 consulting and advocacy service! Ronnie’s mom is in ICU and is difficult to wean off the ventilator. He is asking why would they want to bring her to end-of-life care rather than doing a lung transplant.
Why Would They Prefer to Move My Mom to End-of-Life Care in ICU Instead of Pursuing a Lung Transplant?
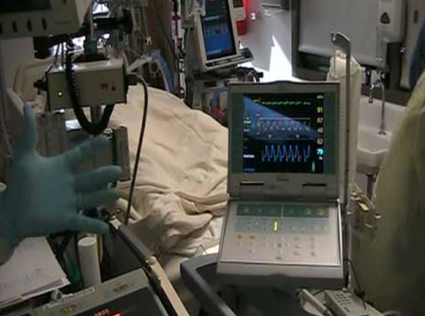
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ronnie here.”
Ronnie: Yeah. I think by then, by the time we spoke, they had palliated mom. So, the week after we spoke, they said, “We’re going to try a week of weaning her,” and they brought her down to pressure 12. And then what happened is, her CO2 just rose, so they stopped, and they said, “Right, we can’t wean her anymore.” And then they put her back up to pressure 17.
Patrik: Right. Right. Okay. Just give me a second. I just need to quickly look through your pictures that were sent last time. So, one is 14 and the other one 14. I don’t see it any lower than 14.
Ted: Yeah, I think by then, by the time we spoke, she was on pressure 14. I think a few days later, they brought her down to 12.
Patrik: Okay. All right.
Ronnie: But then again, her CO2 rose and they just…
Patrik: Sure. This is what I’m predicting, and there could be two outcomes, they might set her up to fail and then they might say, “Well, we’re going to pull out.” Or they might say, “Well, now we know we can’t send her out because if she can’t be weaned, what’s the point of sending her to the respiratory center?” Unless they have something that they’re doing there differently, but I do believe pulmonary fibrosis will be in her way.
Ronnie: Yeah, but what they’ve said is they will trial this week, the aggressive weaning, and then they predict that she won’t cope, they predict the family will be unsettled. They predict other things going wrong, so they’ve given that heads up. And they said, “That in that situation then we have to consider moving her end-of-life,” so that’s either to send her home on a ventilator and this is her life. Will she accept that quality of life?
Patrik: Well, it sounds to me like she will, from what I’m hearing from you.
Ronnie: Yeah. But this is their last sort of opportunity to wean her. They said yesterday they were making the referral to the respiratory center.
Patrik: Now that you mentioned it, as I said, I’m pretty sure that my previous client was talking about the same respiratory center, and they wouldn’t take her mom because she wasn’t the candidate for weaning. But that’s not to say that they won’t look at your mom and they might say, “Hey, maybe we’ve got an idea.” However, I will tell you what I think. So, if your mom would only have pulmonary fibrosis, and she’s around 60?
Ronnie: 63.
RECOMMENDED:
Patrik: 63, okay. Let’s just say your mom would “only have pulmonary fibrosis,” and she would have no other comorbidities, she would be a candidate for a lung transplant.
Ronnie: Yeah.
Patrik: But because she’s got other comorbidities, they probably won’t consider it.
Ronnie: Can I mention it to them?
Patrik: I think you 100% should, you 100% should mention it. If you don’t ask, you don’t get it.
Ronnie: Yeah.
Patrik: When I look through my notes though, from last time, so she’s had number of two cardiac arrests?
Ronnie: Yeah, so she had a bypass operation, so five grafts. Then within the week, one of the leads went and then she had a cardiac arrest after. I overheard that when the doctor came with for the echo this week, I overheard them say that her heart has sort of stayed the same. I even heard them say, “I think the ejection fraction was about 40 to 45 now.” Whereas previously, they’ve said it’s not even 40. But that’s something I’ve overheard. I could totally have gotten it wrong. So, I don’t know if her heart is making some sort of recovery, but they’re not telling us. They’re just saying it’s in failure.
Patrik: Yeah. Look, my notes from last time, you mentioned ejection fraction was 40%. If it’s now 45, that’s pretty good for someone who had bypass grafts times five and two cardiac arrests. That’s pretty good. On my notes, your mom’s diabetic?
Ronnie: Yes.
Patrik: Right. That in and of itself might be a contraindication for a lung transplant. But again, it should not stop you from asking. Have you ever mentioned it?
Ronnie: No, because they’ve mentioned it, they’re like, “Oh, she’ll never be eligible for it.” So, it sorts of like they just shut the door before even looking through it.
Patrik: Is she still on steroids?
Ronnie: She is. I think last Friday is her last dose. So, she is on about 5ml at the moment. 5 mg? 5 mg, yeah.
Patrik: Right. With the goal to wean it off?
Ronnie: So yeah, now it’s just in the process of being weaned off it.
Patrik: Okay. Well, it’s good that her heart is getting stronger.
Ronnie: Yeah. The only day that we saw her heart wasn’t stable in a month, was this Thursday where she had continuous bradycardias through the day. And that was, I think, because her breathing wasn’t right, and the doctor says it has something to do with her nerves and long-term ICU patient and this is just normal for her. She’ll have months of stability and months of days of not stability, being stable, et cetera.
But I didn’t understand it because I put it down to the fact that she was really unsettled with her breathing because the tracheostomy needs to be changed. She kept saying, “There’s this blockage,” she feels there’s this blockage. She must be feeling like she’s drowning. Then obviously, that’s affected her heart for the day. But thank God, by night, it had stabilized again.
Patrik: You said your mom was bradycardic with a low heart rate?
Ronnie: Yeah. So, her heart rate would drop.
Patrik: So, in my notes from last time, you mentioned that your mom was on clonidine. Do you know whether she’s still on clonidine?
Ronnie: No, she’s not on any of that anymore.
Patrik: Okay. Because clonidine causes bradycardia.
Ronnie: Okay.
Patrik: But if she’s no longer on clonidine, then it could be what they’re referring to.
Ronnie: Yeah.
Patrik: Talking about tracheostomy and tracheostomy change. And did you say she’s feeling like she’s drowning in secretions? Is that what you said?
Ronnie: Yeah. She feels like she is.
Patrik: How?
Ronnie: So, I’d say on Thursday night, you know that little, it begins with an S on the tracheostomy? The subglottic-
Patrik: Oh, the subglottic port?
Ronnie: Port, yeah. That was blocked with thick secretions.
Patrik: Ah, right. Okay.
Ronnie: So, they couldn’t aspirate anything from there.
Patrik: I see.
Recommended:
Ronnie: And because she’s got thick secretions, she has a lot of secretions sitting on top of her cuffs. So, when they aspirate that, I’d say about a 7 ml at points comes out, about 4 ml comes out of the mucus, but that night they couldn’t. So, she was just really, really unsettled and she just kept saying, “There’s this blockage there.” And hence why they were like, “Right, we need to do a tracheostomy change.” And then overnight they must have unblocked it and then she still hasn’t had her tracheostomy changed.
Patrik: Right, I see. How often do they do subglottic port suction? Do you know?
Ronnie: I’d say every time, because I sort of told her, “Mom, every time you are suctioned, then tell them to just also clean that port so it’ll make you feel better.” Thank God, neurologically sound, she knows when she got a collection there. So, she will also just sort of lift her hand and sort of point to that and say, “Can you aspirate that as well?” So, it happens quite often. Depending on the nurse, it could happen twice a day. It could happen 10 times in day. So, yesterday’s nurse only did so twice in the day, once in the morning and once in the evening. Whereas the day before, it was frequent.
Patrik: Okay. And how often do they suction her, generally speaking? Every two hours?
Ronnie: Yeah. I’d say, dependent on mom, when they can see she’s uncomfortable, they’d suction her.
Patrik: And what comes up?
Ronnie: A lot of mucus comes up. A lot of thick secretions.
Patrik: Thick secretion. White, grey, yellow?
Ronnie: I’d say yellow.
Patrik: Okay. But she’s not on antibiotics at the moment?
Ronnie: She’s not on antibiotics, no.
Patrik: Okay. All right.
Ronnie: Because she’s not clinically presenting herself with an infection.
Patrik: Yeah. Look, the question that I really have with the things that you’re sharing here is, what’s the purpose of the weaning trial? Is it to set her up to fail and then they really want to push for palliative care? If the weaning trial is to determine she can’t be weaned and then they want to help you get her home, fair enough. Right? That is fair enough. But if they want to set her up to fail and then literally kill her, that would be despicable in my eyes.
Ronnie: Will that happen? Do you predict that she could really go… Because how they’ve explained it to me is it’s 10-minute bursts, so it’ll be 10, three times in the day. And overnight, they’ll put high support.
Patrik: Look, I’ve seen all sorts of creative ideas to wean someone off a ventilator. Some of it worked, some of it didn’t work.
Ronnie: Yeah.
Patrik: I’m not saying they shouldn’t try, what I am worried about is, do they want to set her up to fail and then move forward with something that would be cruel in my eyes.
Ronnie: Yeah, of course, that’s where the family’s worry is as well because even the way they’ve sold it to us, its 10-minute bursts. So, three times in the day and the pressure’s up at night. But 10 minutes is a very long time for mom. And then what will be the knock… That’s why I got in contact with you because I’m thinking, what’s the knock and effect? So, in this 10-minute trial, what could happen to mom? Is her CO2 (carbon dioxide) going to rise? Is she going to get drowsy? Are her other organs going to go into failure? They said for mom, it’s going to be like she’s running for 10 minutes.
Patrik: Probably. Look, there could be strain on the heart, but if they’re doing it for 10 minutes, and with weaning you have to go hard at some point and you have to see what happens, and you really have to, it’s almost like a stress test. But the question in your mom’s situation is, what’s the motive behind it?
With pulmonary fibrosis, I almost feel reluctant to wean. And I’ll tell you why I feel reluctant. The scar tissue is not going away. There’s a lot of resistance in the lungs. The lungs are not very elastic at the moment. With lung fibrosis, the lungs are very stiff and that’s not going to change. If your mom didn’t have fibrosis, but let’s just say your mom came out of a God knows what, brain injury, whatever, she would just wake up after potentially months of ventilation, and she doesn’t have the lung fibrosis, her lungs would be weak, but there would be a real chance for her to wean off with building up her strength. Your mom’s strength might be built up, but the fibrosis is still there.
Ronnie: Yeah.
Patrik: That’s the challenge that I can see here. Which is why fibrotic patients, generally speaking, end up on a lung transplant list.
Ronnie: No, I definitely think I should ask about a lung transplant.
Patrik: You should.
Suggested links:
- Quick tip for families in ICU: Should you stop treatment if your loved one’s in multi organ failure?
Ronnie: Because I know in the U.K. it’s up until 65, and I think that’s what their concern is that we will ask. We haven’t up until this point, but it’s always that’s the card that I want to present to them, stabilize her heart, stabilize her kidneys, which they have been, thank God. And then look, keep her going, put her on the transplant list. But the other option of coming home on a ventilator if that’s possible and that’s what she wants.
She wants to eat. That’s another thing, Patrik, mom wants to eat. She knows she might not have the same quality of life; she might not be moving as a regular and things like that, but she wants to be able to taste food and enjoy juice and things like that. So that’s another question for you, is there, in terms of ventilation at home, that’s going to be out the question then. She won’t be able to eat or drink?
Patrik: Look, I have seen one or two patients over decades that I’ve been doing this that can eat with the tracheostomy and a ventilator. It’s not many. It’s not to say it can’t happen, but there aren’t many. And can they let the cuff down? Have they tried to let the cuff down? Do you know what I mean by that?
Ronnie: No, they don’t take that risk because she aspirated. So, they’re reluctant to do that at the moment, and obviously they have to put the pressure down. But they’re reluctant to do that.
Patrik: Look, have you, because it sounds to me like speech therapy is involved?
Ronnie: Yeah.
Patrik: Have you asked that question to the speech therapist?
Ronnie: I have. And she said the worry is about mom aspirating. The moment, the pressure’s down, the cuffs down, and the air pressure, airway flow, et cetera, and she’s worried that she will aspirate, she will vomit, and then that’s it.
Patrik: That would be my concern, too. The best-case scenario that I can see at the moment is really going home with what’s there on the ventilator, with what she needs in terms of keeping her ventilated. But you will have a better answer after the weaning trial. That’s probably the best-case scenario that I can see at the moment assuming she can’t have a lung transplant. Is a lung specialist involved in all of this?
Ronnie: A lung specialist?
Patrik: Yeah.
Ronnie: Yeah.
Patrik: Is there?
Ronnie: He is one of their own consultants who is a respiratory specialist.
Patrik: Okay. All right. He should be the one, I believe, also advocating for a lung transplant. They should be the one advocating for your mom, but it doesn’t sound to me like that’s what’s happening.
Ronnie: No, because in their minds it’s like, she’s diabetic, she’s a heart patient, she’s got failing heart. They very much want to move her to the end-of-life, hence why the TEP and the DNR aren’t removed because she’s just a burden on the health service now, isn’t she? For them.
Patrik: For them. Yeah.
Ronnie: And I think that’s even in yesterday’s conversation when they said, “We’ll try this aggressive weaning, and then we know there’ll be problems with it. And then if we get to that point, then it’s just moving her to the end-of-life.”
Patrik: It’s just wrong. And especially no one’s asking your mom. So, when they are doing their rounds, is your family there?
Ronnie: They ask us to leave.
Patrik: You should put your foot down there. Have you considered, and maybe you’ve done that already, have you made a complaint to the hospital? CEO?
Ronnie: We haven’t. That’s what I was saying, we’re trying to. We’ve got everything to play.
RECOMMENDED:
Patrik: Want to keep the peace?
Ronnie: Yeah. Collectively, the siblings are doing everything behind the scenes, but we’re trying to vent, we’re keeping things very, very calm and very just so that we can be by mom.
Patrik: Positive.
Ronnie: Yeah. Be positive for mom and be by mom, because at the end of the day, if she presents herself the way she has, there’s not really much that they can do. So, that’s what we’re holding onto, that hope that having the family around stimulates and motivates her, keeps her positive.
Patrik: Right. And she’s positive still?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







