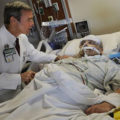
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Why Are ICU Doctors Giving Up on Weaning Mom Off the Ventilator After Multiple Heart Attacks? Help!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ronnie, as part of my 1:1 consulting and advocacy service! Ronnie’s mom is neurologically sound in ICU and wants to continue treatment. He asks how they can remove her DNR (Do Not Resuscitate) status.
My Mom Wishes to Continue Her Treatment in ICU. How Can We Remove Her DNR (Do Not Resuscitate) Status?
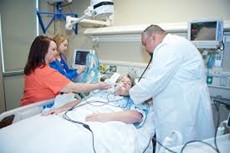
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ronnie here.”
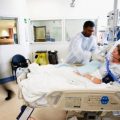
Ted: No. So, in the last picture, she’s asleep. Deep sleep.
Patrik: The volumes there are a little bit lower, and the breathing rate is 23. But still seems to be adequate to me. Do you know what her oxygen saturation is like?
Ted: When I left it was about 27. Is that the one that you’re looking for, the yellow number?
Patrik: No, it would be on the monitor, on the bedside monitor.
Ted: On the bedside monitor. It’s between 95 to 100.
Patrik: That’s pretty good. So therefore, I argue that if they can get her pressure support down to 10 or less, her volumes would stay the same, her breathing rate wouldn’t be any higher and her oxygen saturation wouldn’t be any lower. I would argue she could have time off the ventilator. Do you know if they are still doing arterial blood gases?
Ted: They are doing the blood gases. Yeah. Via the Peripherally Inserted Central Catheter (PICC), they take-
Patrik: Pardon?
Ted: … They take her blood via the PICC line.
Patrik: Ah, okay. Well, that’s kind of an arterial blood gas, it’s venous. Do you know whether she still has an arterial line?
Ted: No, she doesn’t.
Patrik: She doesn’t. That’s okay. So they might be doing venous blood gases but not arterial blood gases. That’s okay. I still argue that even without a blood gas, if they can get the pressure support down to 10 or less, she could have time off the ventilator. Now, what I will also say is that it is very difficult, although not impossible, but it is very difficult to wean someone of a ventilator with lung fibrosis.
And the reason I’m saying that is I don’t know how much you know about lung fibrosis. It is basically a scar tissue in the lungs, and that’s very difficult to reverse. So, from that end, it would be very difficult to reverse that i.e. wean someone off a ventilator as opposed to someone with healthy lung tissue, you have room to move.
Having said all of that, maybe she can have some hours off the ventilator during the day and needs to go back on the ventilator overnight. Now, two questions: (a) you were saying, Ronnie, the other day your mom is fully alert. Is that correct?
RECOMMENDED:
Ted: Yeah, she is fully alert.
Patrik: And are they talking to her about what her wishes are? Or is that just sort of talking to you, and she just gets presented with the facts?
Ronnie: They talk to us. And yesterday in our meeting, we said to the nurse in charge we speak to, who we have a good relationship with, we said, “We’re talking about the Treatment Escalation Plan (TEP), we’re talking about the Do Not Resuscitate (DNR), the consultants don’t want to sit with us.” We said, “Mom’s neurologically sound, nobody’s actually asked her what she wants. And when we’ve asked her, she said she wants continuation of treatment.” And the response to that was, “She might be neurologically sound, but it’s not accurate because we haven’t got a speech valve in so we can’t really make out what she’s saying.”
Ted: So, this week they’re planning on putting the speech valve in and they will ask her-
Ronnie: But then what if somebody’s at that stage where they can’t put the speech valve in? That’s my question. If mom is somebody who, for the next three weeks, can’t have a speech valve in, but there’s a DNR in place and a TEP in place, and she knows that she wants to continue treatment and she needs an escalation of treatment, will they not give it?
That’s unfair when she’s able to say yes to a wish, “I want coconut milk,” she can write. She’s able to express herself very, very clearly. Say yes, no correctly. Psychologically, there, present. Neurologically, very, very sound. It’s unfair to determine, “Oh, yeah, because we can’t hear her voice, she can’t make a decision for herself.”
Ted: … And one time she did actually say that “Well, we can’t fully tell if she’s there because it seems like she might be having bouts of delirium as well.” Now, the thing, she never seems like that to us. She might have when she was originally put on steroids. But recently, her behavior has been related to food where she has been not-
Ronnie: Frustrated at the fact that she can’t eat food.
Ted: … But that she takes out on the family. And then she speaks to us and we understand what she says. And she’s always asking for food, she wants to eat, she wants to drink.
Ronnie: Just recognizes every nurse and doctor that comes. She recognizes who the consultants are, who the junior doctors are, who the nurses are, who the nurses in charge are. She can read the time, she can read the date, she’s aware of everything, completely neurologically sound. And definitely at a stage where if she needs to be asked, “Would you like treatment to continue?” she can express her wishes.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Ted: My concern is only now that they want to do all of that within this week. So they said by Friday, they will have a better idea regarding the ventilator.
Ronnie: And weaning.
Ted: And weaning. So before, it was just the pressure low, just reducing that. They would give her the entire day to wean. Now they would reduce the pressure, as well as place on a chair. And it’s fine to do that. And then, like today, they reduced the pressure down to 13 while also putting her on the chair. And because she couldn’t do it, so then they put the pressure back up to 14. But that will be noted. But a couple of weeks ago, maybe two months ago when they tried that, they would say, “Yeah, we’re rushing it.”
Ronnie: The point in their argument is that she’s weaker now, but that means she needs to be given that time and not rushed. They didn’t rush her through the process when she was stronger, so it shouldn’t be rushed while she is a little bit weaker due to an aspiration. The same amount of time and due care and diligence needs to be given.
Patrik: Very much so. Here is what hopefully could happen, if they can get the pressure support down to 10 or less, that should enable her to go on the speaking valve.
Ronnie: But they said they will try that tomorrow. She’s currently on 14.
Patrik: And they might have their reasons to do it tomorrow. I don’t think she’s too far away, one way or another. I’m just saying this is what I think needs to happen. If they feel like she’s ready now, they will have more information than I have. I think the sooner, the better. I think it’s very… What’s the word? It’s so disrespectful of talking over your mom and not involving her in the decision-making. It’s despicable, as far as I’m concerned. Your mom needs to have a say. Here is the other.
Ted: Is that an argument then, Patrik? Sorry to interrupt.
Patrik: Oh, 100%. 100%.
Ted: An argument that they give us, from the medical team, that actually, we can’t hear her voice, so it’s not a sound, concrete… Is that an argument that we can-
Patrik: It might be.
Ted: … we should accept?
Patrik: I don’t think you should accept that. I tell you when it might be an argument. Can your mom, for example, point to letters on an alphabet?
Ronnie: Yes.
Patrik: Right. Well, that’s-
Ronnie: Even this week past, she was angry. She said she wants coconut milk and she wants watermelon. And we couldn’t. We said, “Okay, mom, write a shopping list.” And she wrote coconut milk and watermelon and something from the store in the city. So, she’s more than able to express herself, and she’s directing us to the kitchen in the ward, “There, go there, you’ll find apple juice. Go there, you’ll find cheese roll.” She wrote cheese roll. So she’s very much able to write and communicate. And her behavior totally changes when it’s a doctor. She knows it’s a doctor treating her, she’s much more pleasant, polite, looking at them gratefully.
Ted: So she had a few incidents where she refused treatment and they have written those down against her. And that’s what they said to us, that she does not want treatment.
Ronnie: That mom’s not compliant.
Ted: That was one. And then secondly, perhaps the consultant said, “Her refusal of treatment is an indication that she’s not happy where she is.”
Ronnie: Does not want to be treated.
Ted: “She wants the palliative care.” They justified the placement of palliative care through that. Now, when they explore further, and that’s what we keep saying to them, “Ask her why she’s refusing.” For instance, if she does not want to wash, ask her why. So one day the doctor asked. And she said, “Well, they give me cold water one day, and one day they wash me with too hot water.” She goes, “I want to go home and have a shower.” But they aren’t exploring why she doesn’t want the care.
Ronnie: Just to contextualise that, the doctor was sent to obviously ask mom why she’s refusing treatment. And the doctor said to her, “Why do you refuse a wash?” And that’s what mom’s answer was straight away, “They give me a wash with cold water one day and the next day with hot water. “She’s able to express herself. She’s able to express that. The doctor understood totally what she’s saying.
My mom understood they were communicating. So the doctor then asked, “So would you like the nurses to bring you the water, you feel the water, see if you like its temperature and they’ll wash you?” And she said yes. And then within the hour, she was happy to have a wash. But it’s always when she says no, nobody follows up and asks her why. And then they just write down that mom’s not being compliant.
Patrik: Sounds to me like they’re very disrespectful, let’s call it for what it is.
Ted: I visited her after this, couple of days after when they placed her on chair. This is within this week. And she kept showing me. And she was frustrated at every single member of the family because nobody brought her food. She kept sending them out to get her juice and she would see them returning, nothing in the hands and she would be really frustrated.
So she wasn’t with me at that point. So, I was able to speak to her. And she told me, “Tell the nurse to change my bed, the bedding.” She would like her pillow changed, her blanket changed, her mattress cover changed because when she was placed on the chair, she could see there was a small mark on her mattress cover.
So now she wanted… And she just said to me quietly, “I’m going to lift it up and put it back on.” That’s what she said, “I’m not going to change it.” But luckily, another nurse happened to walk in with one of those covers and she changed it. And she watched her take it out. So my point is if she wasn’t neurologically sound-
Ronnie: She wouldn’t be able to express what makes her comfortable and what doesn’t make her comfortable.
Ted: … And the fact she doesn’t like that she’s going to be placed back onto a soiled bedsheet.
Patrik: That sounds horrible. Sounds to me like your mom is very sound in mind and they’re not talking to her.
Ronnie: Sorry, Patrik, just a minute. Sorry. She also said to us this week, she said, “Have you done my accounts? Because I don’t want to get a fine from the accountant. Has the roofing been completed?” Because it’s raining here now, and she knows that there’s been problems with the roofing etcetera. These are conversations she’s having.
Then nurse is saying to her, “Relax my dear.” And she says, “No, I’m the boss of the house. I have to concentrate on these things.” And this is my mom expressing this. Nobody’s encouraging this conversation or starting the conversation. This is her remembering what she needs to do or what she wants to do, and things she used to do before she was hospitalized. So she’s well within, she’s neurologically sound. She can be asked if they needed to. And they know that.
Patrik: And if they wanted to. That’s what it sounds like to me. It’s a matter of wanting to. Well, that’s good information to have that your mom is of very sound of mind and that they simply need to talk to her. It sounds very disrespectful. Your mom sounds to me like she wants to get out of there as quickly as possible. And even though it might mean she will stay on the ventilator for a long time to come, potentially for the rest of her life, we don’t know that at this stage. But going home is, I believe, definitely an option for her with the right support. So, what we’ve done, and unless you want to talk about something else first, I can go into how to really get her home, unless you wanted to talk about something else first?
Ronnie: Just really quickly, the TEP and the DNR, how do we get that removed?
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: The bad news is that in that city and again, I can email all of that to you, the Health Service or the doctors, unfortunately, have the right to make a medical decision there. However, they need to consult with the patient or if the patient is not of sound mind or is in a coma, then obviously, they would have to go to the next of kin. But it sounds to me like your mom can be involved in that decision-making.
And my argument in this situation would be, “Well, you’re completely ignoring the patient and you’re making decisions without talking to her. And it sounds to me like you could talk to her if you make the effort.” And it sounds to me like if that conversation took place, your mom would tell them to go away and not talk about a DNR because she wouldn’t want that. Would that be fair to say?
Ted: Yes, definitely.
Patrik: That is so disrespectful of what they’re doing. I’m appalled. But unfortunately, I’ve seen it so many times. It happens all the time and it’s appalling. If you or I were in a hospital bed or in an ICU bed, you would definitely want to be part of that conversation, especially if you could. And your mom can.
Ted: Yeah, definitely.
Patrik: So that would be how to challenge that. And I tell you what you could do. They are saying she’s neurologically not sound. I tell you how you could assess someone, whether they’re neurologically sound or not, and you can do that even in your mom’s situation. You could ask her simple things like, “Do you know what day of the week it is? Do you know the date? Do you know the month? Do you know the year?”
She can write all of that down. That’s a simple test. And of course, if you’re in ICU for 120 days, you may not necessarily know, “Oh, today is the 30th of October.” You might think it’s the 25th or you might think it’s the 2nd of November. Fair enough, a few days here and there. But I would lose track if I was in ICU for 120 days.
Ronnie: Do you think it would work, Patrik, if we got mom to write down now, for example, if I went in tomorrow, write the date, the time, that she’s been in the ICU for this number of days? Her family have informed her that she’s on a DNR and a TEP and she wants the continuation of care.
And she does so in the presence of the nurse as the witness as well and the family. And then we can hand that over. When the consultants come on the ward round, her hands that over herself to the consultants. And would that stand in a court of law, for example?
Patrik: I would do that and I would go one step further. I would record a video of that.
Ronnie: Okay.
Ted: Thank you, Patrik.
Patrik: Because I would have as much evidence as possible. It’s despicable what they’re doing. If someone is in a coma, fair enough, you would have to speak up for her. And I know you do that already, and you will need to continue speaking up for her. But she’s very capable of speaking up for herself if they only let her.
Ted: Yes, definitely.
Patrik: They’re completely ignoring her. Have you been there when they’re doing their rounds?
Ronnie: We have. Yeah.
Ted: It was yesterday, where they skip past her.
Ronnie: Yeah. She was really-
Ted: And she was really concerned.
Ronnie: Yeah. This is what’s been happening the last two days. They skip past her. And they’ll talk after they’ve past her bed. So they don’t even acknowledge her and say hello. So we’ll say, “Mom, the doctors are coming around.” And she instantly, it’s like a little child putting herself on her best behavior because she wants the treatment to continue. Yesterday, she was sat in the chair and she was so proud of herself. They just walked right past her without even saying, “Well done, my dear” or “You’re doing well,” or acknowledge her, just acknowledgement.
Ted: And then she said, “Oh, I’m confused.”
Ronnie: She goes, “I’m confused.”
Ted: “I don’t know what’s happened. Where’s the patient here? I want to see her. What did the doctor say?” Instantly, he wants to see all three of us who were present in that meeting. He’s asking for all three of us because he wants to know why the doctors missed her today.
Ronnie: Why did they skip past her and not acknowledge her?
Ted: So perhaps something-
Ronnie: What was said in the meeting?
Ted: … Because the doctor asked me, “Oh, I’ve met her children, and her family.”
Suggested Links:
Ronnie: But it’s the lack of acknowledgement. We noticed, even the nurses on the ward, when they do the handover nurses in charge, they don’t even. They just skip right past her, if we’re sat there as well. You can ask us to leave, no problem. But it’s a simple thing, acknowledge her. She’s been there for a very long time, let her know she’s doing well. And it’s all about motivation and stimulation and things like that, but they just totally ignore her. It’s just a blatant lack of respect.
Patrik: It’s almost like bullying a critically ill patient. It’s despicable.
RECOMMENDED:
Ronnie: “And we’re already sending her to her grave.” It feels like that. “So, let’s just ignore her.”
Patrik: It’s despicable. I tell you what I believe what your next steps are. Definitely what we talked about, get some evidence that she’s of sound mind. Get some evidence of that. I also believe that one of your next steps is to write or contact, I would almost say probably in an email, contact the hospital CEO or hospital general manager. Because I believe, at the moment, you almost need to take this issue out of ICU. And attach, give them as much evidence as possible.
You should definitely keep advocating with the team. But I would take this out of ICU now. I would take this to the hospital CEO as quickly as possible if I was you. Or the hospital general manager, whatever their titles are. In terms of him going home, I really need to give you almost a case study, and I will point you towards an interview that I’ve done a couple of years ago, would’ve just been before COVID.
So there was a reasonably similar case in other countries. Reasonably similar case with a difference that there was an 80-year-old man in ICU for about 12 months at the time. Very similar situation couldn’t be weaned off the ventilator. The man was absolutely desperate to go home. And after much back and forth with the family and with us to them advocating and saying, “Well, there’s no reason why this man can’t go home with the right support.”
And he did in the end, and the health service is paying for it. What I can do, as a first step, I can send you a link to this interview so you can verify what I’m saying here. It’s on our website. I’ll send you a link to that. And it was a long and hard-fought battle, but in the end, this family got there. And it was sort of a similar approach from the ICU, they were dismissing what this man wanted. And the man was of sound mind as well, very sound mind. And bear in mind, that was pre-COVID. Pre-COVID ICU beds were in short supply. So now we’re still reeling from the hangover of COVID.
ICU beds are in even shorter supply now than they were before COVID. They have no interest in keeping your mom for another two months until home care can be organized. They want to get her out as quickly as possible because winter is coming, they need beds and your mom is potentially blocking a bed if they keep her alive. It’s very sad to say it like it is, but that is what it is.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!