Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
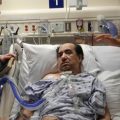
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Ronnie, as part of my 1:1 consulting and advocacy service! Ronnie’s mom had multiple heart attacks and is on a ventilator in ICU. He is asking why the ICU doctors are giving up on weaning his mom off the ventilator.
Why Are ICU Doctors Giving Up on Weaning Mom Off the Ventilator After Multiple Heart Attacks? Help!
Patrik: Have they inserted a permanent pacemaker?
Ronnie: No. Till now, they cannot do that. They keep saying to us, “We can’t do it, we can’t do it. Your mom’s septic, she keeps getting infections.” Till now, they don’t do it. They’ve refused us multiple times.
Patrik: Did they use the temporary pacemaker when it was in?
Ronnie: They did. So, they used the temporary pacemaker initially. Then after a few weeks, I can’t remember exactly how many days they took that out. Then she was stabilized. Again, she got a septic infection, again her heart rate and everything started acting up. She started having arrhythmias, bradycardias. They had to again put in temporary pacemaker. So, she’s had a temporary pacemaker in twice. And then you’ve got the-
Patrik: I see.
Ronnie: … pacemaker that was there from the surgery. So, in total, I’d say about three times.
Patrik: I see. With the arrhythmia-
Ted: Yes. So the last arrhythmia she had recently, followed the Peripherally Inserted Central Catheter (PICC line) that they inserted. So, I don’t know if there’s a connection between all these invasive treatments.
Patrik: … Definitely. When you insert a PICC line, there is definitely the risk of an arrhythmia because you’re basically putting the PICC line right in front of the heart.
Ted: And that’s when she had the bradycardias almost every day, isn’t it?
Ronnie: Not every day. It was every three, four minutes she was having a brady. It took her a while for her heart to get used to it, for her heart to stabilize.
Ted: And then they pulled it back slightly out.
RECOMMENDED:
Ronnie: Yeah, they actually said to us, the consultant actually said to us… I said, “This is what’s causing it. She’s got steroids in her system, and she’s got clonidine in her system. She’s being given oxycodone at the same time. And you’ve put this PICC (peripherally inserted central catheter) line in. For a woman who’s got a frail heart, why would you put the PICC line in?”
And they said it was obviously long-term considerations and things like that. She’s a long-term ICU patient. We understood that, but it instantly made her heart go funny. So, every three minutes her heart was having these bradycardias. It’s stabilized now, thank God. She’s got used to it.
Ted: She still has the PICC (peripherally inserted central catheter) line in though.
Ronnie: She still has it. Yeah, they won’t take that out.
Patrik: A PICC line can stay in for up to six months, potentially 12 months. I’m not too fussed there. But obviously, the risk there is inserting a PICC line for a patient with arrhythmias. That can happen.
Ronnie: Without a pacemaker.
Patrik: Without a pacemaker, that is certainly a risk. Obviously, you would be aware that steroids not only compromise the immune system for a diabetic patient, but they also increase sugar. Are you aware of that?
Ronnie: Yes. Yeah, we are.
Ted: So that’s why we were so shocked when they took the decision to give her. And it begins with an M, the name of the steroid. You’d know. They gave him three-
Patrik: Methylprednisolone?
Ronnie: Yes.
Ted: … That’s the one.
Ronnie: So, they’ve given her three days of that and then they’ve moved to just the P one now. So that stops on Friday.
Patrik: Prednisolone. Yeah. Just a few more questions for me to get the complete picture together. With CAD (Coronary Artery Disease), initially, with the bypass surgery, did she have that as part of a routine consult? Did she have chest pain? What led to it?
Ted: No. So, what had happened on the Saturday before she had gone out with dad and then she ended up having a heart attack in the road I think it was. But she didn’t fall, she just travelled and got herself back home. But she didn’t know she had had a heart attack. She just felt really unwell. So, she was home up until Thursday. She just kept saying, “I don’t feel well, but I’m not ready to go to the hospital.”
So, we know she used up her reserves from that Saturday to Thursday. And then Thursday, obviously, she woke up in the morning and she was just feeling really, really sick. She was vomiting et cetera. And she was just like, “Right, now is the time to go in.” And obviously, as she got into A&E (Accident and Emergency), she walked herself into A&E. When she got there, she was totally breathless et cetera. They knew she wasn’t well. And just after all the checks, rushed her up to the ICU and she’s been there since.
Patrik: Did she have an angiogram?
Ted: Yeah, she did. So, she had the angiogram on Friday. So, she went in on Thursday. Friday, she had an angiogram and then they saw the condition of her heart, realized they needed to have her somewhat stable over the weekend and the relevant experienced heart surgeons to work on her.
So, they said that over the weekend they can’t do it. If it gets into an even more critical situation, they’d transfer her to another hospital. But she had stabilized somewhat with all the treatment over the weekend and then they did it on the Monday morning. Monday was a 10-hour surgery.
Patrik: Wow, okay. And what were the complications afterwards?
Ronnie: So, after the heart attack?
Ted: After the operation?
Recommended:
Patrik: After the operation.
Ronnie: So, it was again the week, what I was describing earlier, the cardiac arrests at the end of the week.
Patrik: I see.
Ted: She did not… Did the consultant say she had another heart attack?
Ronnie: Yeah. But they said to us, apparently, that weekend she had another heart attack. But they didn’t tell us that till August, end of August. That’s when we knew my mother had suffered another heart attack in that week.
Ted: This is post-surgery now?
Ronnie: This is post-surgery. Yeah. In the week post-surgery where she was having the cardiac arrest, they mentioned that she had another. In August, they went and informed us, “Oh, yeah. She had another heart attack.”
Patrik: I see. With the lung fibrosis, that sort of resulted out of all of this. Did she have any lung conditions before going into ICU?
Ronnie: Not that we knew of. And they kept asking us, “Did she, did she?” We said, “No, not that we knew of.” We tried to link it. She had one bout of COVID before. We tried to link it to COVID, maybe it’s COVID-related. They said, “No, it doesn’t appear to be so.” But they put it down to the ventilator, that she’s been on the ventilator for a very long time. But she didn’t have any lung conditions. She wasn’t a smoker. No.
Patrik: Couple of more questions, and they might be a little bit more technical, but just it helps me and will help you understand what we can do and where we’re at. Have you heard of the term, ejection fraction?
Ronnie: No.
Patrik: So, because your mom had multiple heart attacks, by the sounds of things, I would think they would’ve done multiple echo or ultrasounds of the heart in order to determine her ejection fraction. Ejection fraction is the medical term for contractility. How strong can the heart pump? Anything above 65% is a reasonably good number. Anything less than 35% is concerning. I would be very curious to find out what that number is. And that number would be present somewhere. They would’ve done that 100%.
Ted: They did say to us post-surgery, till now, mom’s heart is at 40%. That’s what they keep saying to us.
Patrik: That’s probably what they’re referring to then with ejection fraction. That’s good. That was post-surgery though?
Ted: Yeah, post-surgery till even now. It stayed static. Because I asked this in Monday’s conversation, “Has mom’s heart weakened any further?” They couldn’t answer the question, but they did say it’s working at 40%.
Patrik: Do you have access to the medical records?
Ted: Not at the moment, no. But we want advice on that. Can we get access if we just request it?
Patrik: It’s your right. It’s not a privilege. What I will do is I will send you the policy where you can see, because I know what hospitals are like. They will say, “Oh, yeah. You got to wait, and we can’t do it now.” And I will send you the policy that it’s your right. Yes, you have to go through a process, but it’s your right; it’s not a privilege.
Because especially, around the communication, “What are they doing? What are they not doing?” Especially the whole thing with palliative care. And again, when you’re telling me she’s now in palliative care and she’s got DNR (do not resuscitate) in place, it sounds to me like that has been presented to you matter of fact, rather than in consultation with you.
Ted: Yes. So, when we spoke to them in the two meetings, I was present post the DNR and the TEP (Treatment Escalation Plan) being in place. Both meetings-
Ronnie: Were very matter of fact.
Ted: … And they kept saying, “But you cannot-
Ronnie: Dictate to the medical team there. We won’t be dictated by the family.
Ted: … The patient cannot do that nor can the family.”
Ronnie: Can I just clarify? She’s not in palliative care at the moment. She’s on the limited care, should I say, the TEP. So, they’re not going to escalate beyond what they’re on now. So, they removed the palliative care from her, and returned her treatment. But they’re not going to escalate beyond what she is on now.
Ted: And they’ve only returned it because they can see there has been a clear miscommunication. So, we don’t know what they’re planning on doing in the next couple of days. Are they gathering information? We just don’t know. Or are they genuinely trying to get her off the ventilator? Because previously when they tried to get her off the ventilator, every small progress was a big success.
It was like, “Oh, her pressure has been on 14 for the last three hours. That’s great. Fantastic. Oh, it’s been on for half a day. That’s really good.” Now, if we say, like a couple of days ago, that she’s been stable, she hasn’t made too much progress because her ventilated pressure has been going down one every day, one every day. And then one day, it went down to 14 for seven hours.
And then on that day, mom got worked up because she could not understand why she was not allowed to drink or eat. So, she was slightly worked up towards my brother. And the nurse had to raise the pressure to 15. Now, in the meeting this is seen as a bad thing.
Suggested Links:
Ronnie: We’re told, “Your mom only lasted seven hours on pressure 14.” That’s the words they used, “She’s only lasted seven hours on pressure 14.”
Ted: So, all of a sudden now, just because they want it done so quickly, she must also make progress quickly. So, I was quick to say, “Well, the healing takes time, and you aren’t giving her enough time to wean off it. You want her to now make progress very quickly, and it seems very, very unfair to expect that of someone who’s been on the ventilator for a very long time.”
Patrik: Do you have a picture of the ventilator that you could share?
Ted: Yeah, I can. I can send that. I’ve got today’s ones.
Patrik: That would be amazing. If you can send it in WhatsApp or if you could email it that would be really good.
Ted: I’ll send you three different ones. So, it’s the progress from today.
Patrik: I just texted you my email address in WhatsApp. Can you see that?
Ted: Yeah, I can. Yeah, I’ve got it. Okay, so I’ll do the progress. We tried to get a few pictures for you today, Patrik. That’s the first one.
Patrik: Yeah, coming.
Ted: Second one.
Ronnie: And you know the second one? Was that while she was on the chair?
Ted: No, I don’t think we got one of her on the chair.
Patrik: Well, the first thing there is pretty good, I’d say. And I’ll talk you through it in detail.
Ronnie: The last one is the latest one. I left her about…
Ted: Three, four hours ago?
Ronnie: Yeah.
Ted: That was the last one you took. Wasn’t it?
Ronnie: No that’s not the last. This is the last one. I’m so sorry, I didn’t actually send you the last one. I’ll do it now.
Patrik: What’s your mom’s weight, roughly?
Ronnie: 58 kg now.
Patrik: 58 kg. The reason I’m asking that is simply because of the volumes. But that’s good. That’s really good because the volumes look reasonably small to me. But given that she’s 50 kgs, that’s-
Ronnie: About 55, 58 now. She went in at 70, and now she’s dropped to 58. So, the last one I sent you, Patrik, is the latest one, which was at eight o’clock.
Patrik: … Right, okay.
Ronnie: This is when she’s deep sleeping, by the way.
Patrik: Sorry, this is when?
Ronnie: This is when she was in deep sleep.
Ted: The last one.
Ronnie: The last one I’ve just sent just to give that as a bit more context.
Patrik: The numbers look good. I can quickly walk you through that. So, when you look at the bottom left, 30% of oxygen is pretty good. Room air, the air that you and I are breathing is 21% oxygen. So, 30% is okay for someone on a ventilator. PEEP (positive end expiratory pressure) of six is pretty minimal. It’s usually not any higher than five anyway, so that’s pretty good. One critical number there is really the pressure support that you can see there, the 14.
That’s sort of a critical number. I argue that anything less than 10 of pressure support with a PEEP of six and 30% of oxygen is a number where you can think about taking someone off a ventilator, assuming that when you go over to the right side, the VTi (inhaled tidal volume) and Vte (exhaled tidal volume), 348 and 317 on the first picture you sent me, that’s basically volume she’s using on inspiration.
So, it’s basically when she’s breathing in, she’s breathing in 348 mls. That’s adequate for her weight, which is why I asked about her weight. So then, when you look at the top, 28 breaths per minute, that’s a little bit on the high side. I would imagine she’s not asleep in that picture, is she?
RECOMMENDED:
Ted: No. So, in the last picture, she’s asleep. Deep sleep.
Patrik: The volumes there are a little bit lower, and the breathing rate is 23. But still seems to be adequate to me. Do you know what her oxygen saturation is like?
Ted: When I left it was about 27. Is that the one that you’re looking for, the yellow number?
Patrik: No, it would be on the monitor, on the bedside monitor.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!