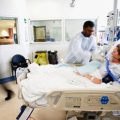
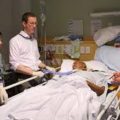
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
The ICU Team is Negative About My Dad’s Condition, But Is There Hope? Live Stream!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ronnie, as part of my 1:1 consulting and advocacy Roman ‘. mom is ventilated and he is asking why they put her on a DNR (Do Not Resuscitate) status despite being awake and alert.
Why Has My Ventilated Mom in ICU Been Placed on a DNR (Do Not Resuscitate) Status Despite Being Awake and Alert? Help!
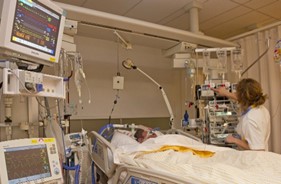
Patrik: Hi Ronnie! How are you?
Ronnie: I’m good. Thank you. Okay, where would you like me to start? So, I’ve given you a bit of background as to what happened on Friday. Mom was palliated. And we had a follow-up meeting where they discussed the Treatment Escalation Plan (TEP). The medical team discussed what happened with the treatment escalation plan. They said that they weren’t going to go beyond where we are now. If she has an infection, the plan is not to even treat her with antibiotics.
Patrik: Wow.
Ronnie: There’s currently a Do Not Resuscitate (DNR) in place and there is a TEP in place.
Patrik: A TEP. What do you mean by TEP?
Ronnie: So it’s a treatment escalation plan, prevention.
Patrik: But it’s almost cynical to say there’s a treatment escalation plan if they’re not even giving her antibiotics.
Ronnie: Yeah, that’s what we’ve been told. They will not give that if she needed it. It felt really rushed, the follow-up meeting that we had. During the course of the week, we kind of noticed that they were a little bit more… What’s the word? When they were focused around that, they ensured they took everything they needed, mom’s numbers. I know they’re doing that anyway. Perhaps we were noticing it more than other days.
But it felt like maybe now they were ensuring they had all their evidences. So, if they tell us again we need to palliate, we will accept it because now they can show. Or if we took it further, perhaps down the legal route, they have all the relevant details to make their side, their decision stronger. Now, when we had this follow-up meeting, we were told-
RECOMMENDED:

Ted: The day was Friday. Sorry, Patrik, just to interrupt my brother. It was on Friday, so yesterday. And it was more focused around mom’s rehabilitation and weaning her off the ventilator. So they use this to tell us where they are currently at. So they brought in the nurse in charge, who they know we have a good relationship with.
Not the nurse in charge who was there in the first meeting. Her way of speaking and all of that wasn’t pleasant at all. In fact, she said, “You have no right,” and brought in that they have years of experience and so on and so forth. Very unprofessional behavior within that session. So they brought in another nurse in charge and they also brought in a physiotherapist and only one of the consultants. Prior to the meeting, as they called us there, we noticed the original consultant who-
Ronnie: … Made the decision.
Ted: .. Yes. They were all huddled together by the doorway just outside the doorway where the meeting was to take place. They had called in for two minutes. They looked at mom’s numbers on the ventilator, at her monitors, they looked at her papers. And I overheard the heart surgeon say, “Oh, but she’s still on the ventilator,” and she went off in a huff.
And then they went and my brother and mom were outside. So they spoke to them and updated them on their thoughts. So it seems like I don’t know what they are doing, although they tell us they’re trying to wean her off. I don’t know. Something doesn’t seem quite right. And then within the meeting, the consultant was there for maybe five minutes or 10 minutes.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Ted: And then he walked out.
Ronnie: The consultant, it was sort of like the current plan. So, we’re discussing the physiotherapy and rehabilitation and weaning mother off the ventilator. After that was shared, he said, “Right, I need to go now.” And he left after about 10 minutes into the meeting, and so there was no opportunity for us to discuss the TEP and have the TEP removed. So we ended up having that chat with the nurse in charge, whom we feel comfortable speaking to.
We ended up saying that the consultant didn’t actually… We waited the whole week for this meeting to have the opportunity to continue to raise our concerns as a family. The whole week mom’s had this treatment escalation plan in place and a DNR in place. Mom’s been awake, she’s been responsive, she’s been alert, she knows what she wants. She’s been craving foods and drinks. The only thing that’s stopping her and us hearing her voice, is obviously she’s got the speech valve in and that’s going to come in time.
Patrik: Has she had the speech valve at all?
Ted: She has during the journey, yes. But not at this current time. So, during the journey, mom has had the speech valve in. She’s been decannulated, she’s been extubated. Mom had nine days off of the ventilator. And what had happened, her swallow muscles are obviously weak. She aspirated. Now, they were constantly telling her, “You need to eat, you need to eat, you need to eat.” But she kept saying to the nurses, “I feel like I’m choking every time I even take a sip of water.”
They were encouraging us to bring in food and we’d blend the food, make it into liquid so that it was easy for her to swallow. But she kept saying, “Every time that I need to go even slower, I feel like I’m choking.” And what ended up happening, was they called us one morning on a Friday, and said that she’s aspirated really badly. She ended up being intubated again and this is where we are now.
Patrik: Can I just ask a couple of questions there? I do remember, Ronnie, when we spoke, you mentioned about the extubation, and then about the aspiration pneumonia. But are you saying she also had the tracheostomy removed in the meantime?
Ronnie: Yes, of course.
Ted: Yes. For nine days.
Suggested Links:
Patrik: … Okay. So basically, intubation then decannulation. And this is where you’re finding yourself now a month later, pretty much.
Ronnie: So six weeks later, this is where we are right now. On Friday, they moved her into palliative care without… It was such a bad miscommunication. My sister and myself, and the whole family were called in because mom was having bradycardias in the morning. They called us all in. Mom’s carbon dioxide (CO2) levels were really high, pH and CO2 levels or something like that were really high. “Your mom’s not very well. Come in and see her.”
The day before she was on ventilator pressure 14, sitting in the chair, and things like that. The next morning, she’s not in a very good way. We all go in. My sister and I, who are the spokespersons for the family, are called into a meeting. The consultant says he doesn’t want to meet any other family members, just the two of us.
Patrik: What?
Ronnie: Yeah, we’re eight children. So, my father has eight children and my mother. He said he only wants to see me and my sister. In this conversation, we’re told that they won’t escalate his treatment. Mom’s currently got steroids, high doses of steroids in her system. The family was not consulted when they administered the steroids. We discussed it, we discussed the risks. And they said they’re going to continue observation of mom before they administered the steroid and they will let us know what they decide.
They didn’t end up telling us when they did administer it. One day, one of the nurses said, “Oh, she’s been prescribed the steroids.” So we were just in total confusion. And that is our argument that these steroids are administered. Mom’s a diabetic patient as well. Been a diabetes patient for about 15 to 20 years. I’m not sure, between 15 to 20 years. And then obviously, steroids, huge immunosuppressive for somebody who’s been in the ICU for such a long time. This is a huge-
Ted: And she had multiple infections.
Ronnie: … Multiple infections. She can’t leave the ICU and her setbacks are infection related. So taking that was a huge risk. So, saying to us in that meeting, myself and my sister, “We’re not going to treat her with antibiotics because she’s got steroids in her system.” So my sister and I were like, “Okay, that sort of makes sense,” because they said it’s putting another bug into her that she’s going to be resistant to.
So my sister and I, we thought, “Yeah, that makes sense.” We didn’t realize this wasn’t a TEP that’s been placed. Before we know it, in two hours she’s been palliated into palliative care. She had the cannula on her thigh, the monitors are switched off. The only thing remaining was her ventilator. Her feeds was stopped, her insulin was stopped, her medications were not prescribed. Even the blood thinner-
Patrik: I’m sorry to interrupt there. Are you saying that she’s had no feeds since Friday? Is that what you’re saying?
Ted: So what happened, I was with her at that time and they stopped her feeds, because they changed the tube to a smaller one-
Ronnie: From a nasogastric (NG) to a nasojejunal (NJ) tube, they’ve done that when she aspirated.
Suggested Links:
Ted: .. So what happened then is, it got stuck in the afternoon. So, they did not attempt to unblock it as they had been doing so. Then by night, when the nurses changed and I asked, “Are you not going to give her the feeds?” And she just looked at me like, “What do you mean am I not going to give her the feeds? I can’t do anything unless I’ve been given instructions to do that.” I said, “But she will need her feeds.” She said, “Her feed has been stopped since afternoon.”
Ronnie: So we were rushing around trying to get her the feeds for her. Mom is awake by now, by the way. She’s woken up from this little hiccup in the morning.
Ted: So she was given the feeds because she said she’s going to ask the nurse in charge, who herself, when it was her shift, she walks in and she’s confused as to why mom is in palliative care, yet has the ventilator switched on. That was her exact words. So, because there was a confusion, they decided to give her the feeds. So, the only thing running throughout the night then was her feeds. Her feeds and the ventilator. And then they gave a dose of oxycodone into her thighs.
Ronnie: That was during the day. That was for comfort mainly.
Patrik: Sure, I understand that. And so not giving feeds was a reasonably short period of time though?
Ronnie: Yeah, it was reasonable. Yeah, because we’ve had the-
Patrik: It just sounded to me like when you mentioned that she hasn’t had any feed since before.
Ted: Oh, okay. No.
Ronnie: … No. It was during that day when they palliated her, they stopped the feeds. Her insulin was re-administered the following day on the Saturday. And again, like I was saying, mom’s a diabetes patient, she’s got type 2 diabetes, she needs her insulin, her sugars to be checked etcetera. That wasn’t administered. She had diabetes before she was hospitalized. We were checking her sugars at home, blood pressure medication etcetera. She needs those. None of her medications were given till the following day when we were just constantly on there. As far as I remember, anyway, she wasn’t administered medication.
Ted: No, she wasn’t. So you had to go in.
Ronnie: I had to go in and chase it, and practically plead for her treatment because she needs those.
Patrik: And just for me, just for clarification, just so I remember this correctly for us. When we first spoke, she had open heart surgery about four months ago. She then had complications. She ended up on the ventilator and she’s now stuck with pulmonary fibrosis. Do I remember this correctly?
Ronnie: Yeah. So mom had five Coronary Artery Bypass Grafting (CABG), it’s the bypass.
Patrik: 5 stents. Yeah.
Ronnie: She had to do five. So, she was ventilated before she went into surgery. Yeah, of course. Again, they did the tracheostomy about 21 days later after the surgery date. Sorry, just to give you a bit more context into mom’s condition, the week after her operation, so she went into hospital. I can give you dates if you want. So, she went into hospital months back, straight up to the ICU from Accident & Emergency (A&E).
Then the Monday, was the date of his surgery. By Friday, she had started to have cardiac arrests. So she was quite sick during the week. She started having cardiac arrests on the Friday. Now Saturday, Sunday, again cardiac arrests. Monday, we are told, literally, the consultant said to me, “We’re shocking the life out of your mom constantly.” And then they figured out one of the leads had… You know post-surgery, they put a-
Patrik:ah, sure.
Ronnie: … pacemaker in? So they found out one of the leads had stopped working on those temporary pacemakers. So the whole weekend they’ve been shocking her. Not one bothered to check if it was a lead problem or a lead issue. So, the Monday, I think roughly around that date, they put a temporary pacemaker in, and then that stabilized mom. And obviously, as you can see, we are spotting certain things that are not done correctly.
For example, if she’s having her first cardiac arrest on the Friday post-surgery, check the leads in the pacemaker, and ensure that they’re all working and intact. They waited till the Monday, obviously, perhaps it’s because of weekends and things like that. Waited till the Monday or the Tuesday, said to me, “They’re shocking the life out of her.” She stabilized.
Suggested Links:
Patrik: Have they inserted a permanent pacemaker?
Ronnie: No. Till now, they cannot do that. They keep saying to us, “We can’t do it, we can’t do it. Your mom’s septic she keeps getting infections.” Till now, they don’t do it. They’ve refused us multiple times.
Patrik: Did they use the temporary pacemaker when it was in?
Ronnie: They did. So they used the temporary pacemaker initially. Then after a few weeks, I can’t remember exactly how many days they took that out. Then she was stabilized. Again, she got a septic infection, again her heart rate and everything started acting up. She started having arrhythmias, bradycardias. They had to again put in temporary pacemaker. So she’s had a temporary pacemaker in twice. And then you’ve got the-
Patrik: I see.
RECOMMENDED:
Ronnie: … pacemaker that was there from the surgery. So in total, I’d say about three times.
Patrik: I see. With the arrhythmia-
Ted: Yes. So the last arrhythmia she had recently, followed the Peripherally Inserted Central Catheter (PICC line) that they inserted. So I don’t know if there’s a connection between all these invasive treatments.
Patrik: … Definitely. When you insert a PICC line, there is definitely the risk of an arrhythmia because you’re basically putting the PICC line right in front of the heart.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!