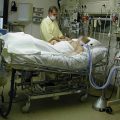
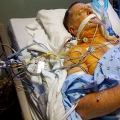
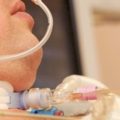
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Mom is Already Awake and Responsive in ICU. Why is the DNR (Do Not Resuscitate) Still in Place?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ronnie, as part of my 1:1 consulting and advocacy service! Ronnie’s mom is in ICU, has lung fibrosis with tracheostomy, and is ventilated. He is asking how his mom can be successfully weaned off the ventilator.
How Can Mom Be Successfully Weaned Off the Ventilator in ICU with Lung Fibrosis and a Tracheostomy?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ronnie here.”
Ronnie: … We actually haven’t. Up until this point, we haven’t sought legal advice. We just are fighting for mom, we’re advocating for mom, and we can see there’s been a clear breach. She’s being palliated, she’s awake, she’s of sound mind. She’s looking at her for a time. And she’s saying to us, “They’re killing me.” She kept saying, “they’re killing me. You need to take me home.”
Patrik: It’s despicable. Look, I do need to get another call now. I want to leave you with all of that. I will send you a recording of this call so it’s a reference point. I hope that was helpful in any way that you can take the next steps. Do not give up. Keep them on their toes.
Go to the hospital CEO and test the waters again with legal advice. You know it’s nonsense when they’re telling you, whatever they’re saying, it’s not in the best interest. It’s nonsense. You know what’s in the best interest for your mom. Only you know that. Nobody else.
Ted: And she knows herself.
Patrik: And she knows, of course. He and you know.
Ted: Yeah, she knows. Because when we said she wants to go home, they were surprised that she actually wants to go home.
Patrik: Well, it’s possible. It’s possible.
Ronnie: Thanks for your time.
Patrik: It’s a great pleasure. I hope it’s all going well. Have a look at WhatsApp as I sent you quite a few things there.
Ted: Yeah. Thank you, Patrik.
Patrik: It’s a pleasure.
Ted: Patrik, if we did want you to be an advocate for us, if for example, in these meetings, if they don’t go according to plan, is that a possibility?
Patrik: Oh, definitely. 100%. They need to hear what we are doing here so they can understand that it’s possible for your mom as well.
Ted: Yeah.
Ronnie: Okay.
Ronnie: Thank you so much, Patrik.
Patrik: Thank you so much. Bye.
RECOMMENDED:
Patrik: Hi Ronnie! How is your mom?
Ronnie: Mom is doing well. So, she’s been stable since we… I can’t remember when we last spoke.
Patrik: I would have to look it up, four weeks ago?
Ronnie: Yeah, so I’d say she’s been stable for the last four weeks. She’s neurologically sound. She’s been a lot more awake, a lot more alert, sitting out in the chair.
Patrik: Great.
Ronnie: Thank God she’s responding. She knows what’s happening, so she’s aware of what’s been happening. She’s responding really, really well to the nurse and the doctors. There’s a level of anxiety there because she keeps, for example, taking a sleeping pill. Then, she thinks they’re using that to sort of put her to sleep and then palliate her, et cetera.
So, the only thing that’s not gone in her favor is the weaning and that’s a little bit about what I wanted to talk about today. So, they spoke with us about the weaning and her respiratory, and the direction they want to take with that. I think they’re saying that they’re referring her to Bay Five, which I’m not sure if-
Patrik: Who’s Bay Five?
Ronnie: Bay Five is part of the District’s Hospital. So, it’s a respiratory unit. There is for long-term patients who need to be weaned off the ventilator. They are saying that they don’t think she will be admitted because they will make a referral, but because she’s also got this heart condition, they say a failing heart (Heart Failure) but thank God her heart has been doing the right thing. So, because of this, they think, and then lots of loss in weight and muscle mass and things like this, that they’re thinking that they’re not necessarily going to accept her.
They did have also this week gone. They had a consultant who works in the general ICU come to see mom and she worked at Bay Five before. So, she tested her muscles, so she asked her to take deep breaths, et cetera. She and another consultant said it is weak but not as weak as they’d assumed. So, that’s where we’re at the moment.
Patrik: Okay. Now, I’ve just looked through my notes from last time. She’s obviously got lung fibrosis from memory. Is that right? That’s in my notes.
Ronnie: Yes.
Patrik: So, when you say weaning, last time they said, from memory, that she wouldn’t come off the ventilator because of lung fibrosis. Has their point of view changed?
Ronnie: It hasn’t changed, but they said there’s a small window of opportunity to wean her. So, they’ve started having these meetings with all the consultants that sort of take care of mom. So, weekly meetings about mom and they discuss possible options for her. So, what they did try, in the time we haven’t spoken, is to do a slow wean. So, they just put the pressure down by one. To be honest with you, I’d say the majority of the four weeks she’s stayed under the same pressure. So, it’s on pressure 15 now. Can I share a screenshot of the latest-
Patrik: Oh, please. The more information, the better. Because I’m just about to ask, what is it? What ventilator settings is she on?
Ronnie: Yeah.
Suggested Links:
Patrik: I can tell you what you can do. You can either send it to me on WhatsApp or I can make you host and then you can share the screen if you know how to do that.
Ronnie: Yeah, I’ll just send it via WhatsApp because I think I’ve got one, a later one, I think. I’m just going to go into my deleted box. This was from Thursday.
Patrik: And your mom has every will to live still?
Ronnie: Yes. She just wants to come home. She’s made it clear to the speech therapist to come and see her. So, they did try and get a translator even though she knows how to speak English very well. They did, for impartiality, et cetera, they did try and get a translator to come and talk to her.
So, this is her latest ventilator. So, this was during the night, I would say, on Thursday. So, they up the pressure for the night onto 20, but I would say she’s on this one at the moment.
Patrik: Right. Okay. I’m just waiting until it’s coming through. Okay, it’s coming now. So, is this the first one or the second one?
Ronnie: So, the first one is what they did on Thursday night. So, because she was going to have some tracheostomy changed.
Patrik: 25, 20. Okay. All right.
Ronnie: So, they put the pressure up to 20.
Patrik: Has that tracheostomy changed?
Ronnie: That hasn’t changed, no. That’s where I’m a bit furious with the doctors about that because it was meant to happen yesterday. The nurse got everything ready and then they didn’t do it.
Patrik: Oh, I see.
Ronnie: Yeah. Her tracheostomy has been in since then. So, best practice is 28 days and we’re more than a month now. So, it does need a change.
Patrik: Do you know if your mom has an inner cannula? Do you know what I mean by that?
Ronnie: She does, yeah.
Patrik: She does?
Ronnie: Yeah.
Patrik: Okay, that’s good. That gives me a little bit of relief, sort of where I’m thinking, “Okay, great.” If without an inner cannula, I would be very worried. With an inner cannula, it’s a bit like a safety valve, assuming they’re changing it regularly.
Suggested Links:
Ronnie: Yeah. So, how about the latest pictures of the ventilator settings I sent you?
Patrik: Yeah, so when you look at the top of the picture, it says SPN-CPAP (Spontaneous Continuous Positive Airway Pressure), which stands for Spontaneous CPAP.
Ronnie: Yeah.
Patrik: She’s been in that mode for the last few months?
Ronnie: Yeah.
Patrik: Okay. And she’s not getting exhausted in that mode?
Ronnie: No.
Patrik: Great.
Ronnie: She did have a day of exhaustion, I’d say on a Thursday. And I’d say Wednesday, Thursday. So, Wednesday when it says a slope, they changed back to 30. So, you’ll see in the previous picture, it’s on the 30, and they’ve kept it from Wednesday on the 30.
Patrik: Okay, fair enough.
Ronnie: So, the moment that changed, she started feeling that there was a bit more, she keeps describing it as like a blockage. So, Wednesday, she was really, really struggling with it, but there was no effect on the heart. But by Thursday, she started having these bradycardias. So, for the whole of Thursday, she had bradycardia.
Patrik: Okay. Has she had any time off the ventilator at all since we last spoke?
Ronnie: No.
Patrik: Okay. And I’m not surprised.
Ronnie: Yeah.
Patrik: I’m not too surprised because pressure support of 15, needs to be half of that. So, in order to take her off the ventilator, pressure support needs to be less than 10, ideally 8. And when you look at the last picture that you sent me, you can see the 290 on the right side.
Ronnie: Yeah.
Patrik: That’s the volume she’s taking. So, I can’t remember, I have to look through my notes. Your mom’s weight roughly?
Ronnie: About 52, 53 kg.
Patrik: Well, that’s actually accurate. When I say accurate, appropriate. So that’s good. Does she keep losing weight?
Ronnie: She stayed static, I would say. But she’s lost a lot of weight.
Patrik: Right. Okay. All right. So, have they done blood gases, do you know?
Ronnie: They have, yeah.
Patrik: Do you have a blood gas result?
Ronnie: I can show you a screenshot of her monitors if that’s okay?
Patrik: Yeah, yeah, please.
Ronnie: Just trying to find. Okay. So, this is from the latest one, from the 16th.
Patrik: Right. Okay.
Ronnie: Three days ago. So, it stays roughly around there.
Patrik: Okay. Just give me a second. 5.5 is her PCO2 (Partial Pressure of Carbon Dioxide). I just very quickly need to look 5.5, which is in millimeter per mercury, because I know the blood gas is in millimeter mercury, but that’s in kilopascals. Just give me a second, that is 30. Okay, that’s good. That’s good.
Ronnie: Doesn’t it show something else in the actual blood gases? Isn’t it like ideal?
Patrik: Well, there are two things. Ideally, you have to have 5.5 verified in the blood gas and ideally, you have a PO2 (Partial Pressure of Oxygen) in the blood gas as well. I think in her case it’s more about the PO2. The PO2 means the oxygen level in the blood.
Ronnie: Yeah.
Patrik: Right.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Ronnie: They do the regular blood gases.
Patrik: How often?
Ronnie: I’d say every few hours at the moment. I think every four hours they’re doing the blood gases. And again, it’s from the PICC (Peripherally Inserted Central Catheter) line, it’s not from…
Patrik: Not from the artery because she doesn’t have an arterial line, I can see that.
Ronnie: She doesn’t, no.
Patrik: Which means the blood gas, to a degree, will only give limited information because when they take it from the PICC line, the PICC line sits in the veins. Whereas an arterial blood gas is taken from the artery. So, there’s a difference between veins and arteries. Arteries carry oxygenated blood and veins carry deoxygenated blood. That’s why the result that you get from the venous gas gives you an indication, but it’s nowhere near as accurate as an arterial blood gas. But then after four months in ICU, she doesn’t really need an arterial line, there’s also an infection risk. So, I can understand why she doesn’t have one. Have you listened to the interview that I’ve sent you when we last spoke?
Ronnie: Yeah, with my aunt?
Patrik: Mm-hmm.
Ronnie: I did. Yeah. It sounds really similar to our situation, to be honest.
Patrik: Very similar.
Ronnie:Very, very similar. But we’re trying to keep a really positive relationship with the team because we don’t want it to get to a situation where they move us away from mom because I think that would be so detrimental to her mental health. And that’s where we are trying to maintain some sort of positive relationship with them, keep communicating with them. We just tell them constantly as to what her wishes are, and keep reminding them of this. We did discuss the possibility of her coming home with a portable ventilator as well. She’s happy to do that if need to be. But I think they’re exploring all their angles at the moment. So, what they’re trialing at the moment is the CO2 (Carbon Dioxide) machine. They put a stick on his forehead, and it monitors her CO2 output. She can’t tolerate that. She says it gives her a headache. So, unfortunately, mom can’t tolerate it.
Patrik: Why would they even do that? They can do it with the… So, when you look at the last picture you’ve sent me, I bet they get these… The 5.5 there, that’s the CO2.
Ronnie: That’s the CO2.
Patrik: Right. And they’re getting this from her forehead?
Ronnie: No.
Patrik: There should be a connector in the ventilator circuit.
Ronnie: Yeah. That’s where they’re getting that from. But the last two days, they’ve put this other thing, a sticker on her forehead and she really says it’s giving her an earache and she can’t tolerate the pressure from it or whatever it is, whatever she’s feeling. So, she’s actually refused to keep the sticker in her head. And she is like, “No, I’m not…” And something to do with electrolytes and I’m not too sure.
Patrik: Never heard of it.
Ronnie: A CO2 monitor, yeah.
Patrik: Well, no, of course. A CO2 monitor, I have, but never heard of a CO2 monitor on the forehead.
RECOMMENDED:
Ronnie: Yeah, they just leave it there and she is saying, “No, it’s affecting… They’re doing something that I’m not content with.” She’s complained of an earache as a result. She’s saying that she’s had this constant headache since, so she doesn’t want that. She refused it last night. Then, we’re just thanking God that she’s neurologically sound, where she can say yes or no to certain things.
The other thing they spoke about with me yesterday, the consultant did, and this meeting was with the lead consultant. He spoke about a CO2 medication, something to help reduce her CO2 levels. Now, something in my gut is telling me I’ve got questions about it because I immediately said that mom did not get the best kidneys since her hospital stay, so I wanted your advice on that. Is there a medication that they give to sort of normalize CO2?
Patrik: Not heard of it. Not heard of it. Look, there could be new developments that I’m unaware of, but I’ve not heard of it. Let’s just say her CO2 was high. They would bring the pressure support up or they would bring up the PEEP (Positive End Expiratory Pressure).
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!